Table of Contents
ToggleIntroduction to Histology: The Study of Tissues
In anatomy, you study the gross (visible) structures of the body. But what happens when you need to look closer? This highly detailed guide introduces you to Histology. By the end of this section, you will master what histology is, why it is an absolutely indispensable tool for health workers, and the precise, step-by-step laboratory journey a piece of tissue takes from the operating table to the microscope slide.
1. What is Histology?
To understand a disease, you must first understand the normal architecture of the body at the microscopic level. Histology is the scientific study of tissues.
- Etymology: The word is derived from the Greek words "histo" (meaning tissue or web) and "logos" (meaning study or science of).
- Definition: Therefore, histology is the science of the microscopic structure of cells, tissues, and organs. Simply put, it is the study of tissues under a microscope.
While Gross Anatomy looks at the heart as a whole pumping organ, Histology looks at the individual cardiac muscle cells, identifying the unique intercalated discs and striations that allow the heart to beat synchronously. It forms the essential bridge between biochemistry (molecules) and gross anatomy (visible organs).
2. Why Health Workers Need to Know Histology
A strong foundation in histology is not just for doctors, pathologists, or laboratory researchers; it is a critical component of a professional nurse's and allied health worker's knowledge base. It elevates practice from basic, task-oriented care to a deeper, more analytical level of patient management.
Understanding the "Why"
Shows how a tissue's microscopic structure dictates its clinical job.
Clinical Example: Why does oxygen therapy work? Because histology teaches us that the lungs are lined with simple squamous epithelium (an incredibly thin, single layer of flat cells). This extreme thinness allows oxygen gas to diffuse instantly into the blood. Knowing this makes administering oxygen far more meaningful.
Recognizing Abnormalities
Knowing normal tissue architecture helps nurses and doctors recognize the microscopic changes that occur in disease (histopathology).
Clinical Example: When performing wound care on a diabetic ulcer, a nurse who understands histology recognizes the specific types of granulation tissue forming, indicating whether the wound is actively healing or becoming necrotic.
Specimen Handling
Improves clinical participation in collecting and preserving laboratory samples.
Clinical Example: When assisting a physician with a punch biopsy of a suspected skin cancer, the nurse knows the tissue must be placed immediately in 10% formalin (a fixative). If it dries out or is placed in water, the cells will burst (lysis) or rot, ruining the histological diagnosis.
Empowering the Patient
Allows nurses to translate complex medical jargon into understandable concepts for patients.
Clinical Example: If a patient receives a pathology report stating "cervical dysplasia" after a Pap smear, a nurse with histological knowledge can calmly explain that the *cells* have changed their normal shape, but they have not yet broken through the basement membrane (meaning it is not invasive cancer yet).
Drug-Cell Interactions
Helps health workers anticipate medication effects and adverse side effects by understanding exactly which cells are being targeted.
Clinical Example: Cancer chemotherapy kills rapidly dividing cells. Histology tells us that hair follicles, stomach lining, and bone marrow possess the fastest dividing cells in the body. Therefore, the nurse anticipates hair loss, severe nausea, and low blood counts.
Speaking the Same Language
Facilitates clear, precise communication with pathologists, surgeons, and other healthcare professionals. Understanding the terminology in a histopathology report directly influences the nursing care plan and post-operative monitoring.
3. Methods of Histology
If you surgically remove a lump of flesh and place it directly under a microscope, you will see absolutely nothing. It is too thick for light to pass through, and the cells are completely transparent. Therefore, Histology employs a strict sequence of techniques to prepare tissues for examination.
The main workflow involves: Tissue Preparation → Staining → Microscopy.
A. Tissue Preparation Techniques
This is the first and most critical step to preserve the tissue, prevent it from rotting, and make it firm enough to cut into transparently thin slices. There are three main methods:
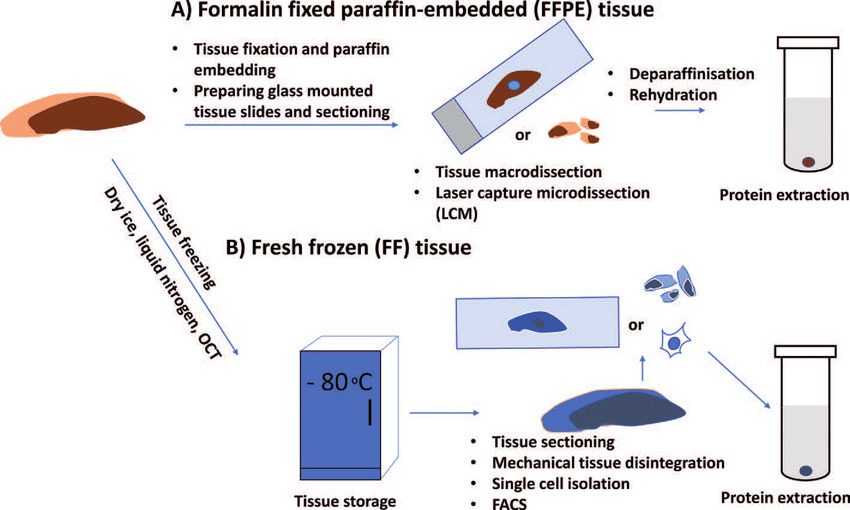
1. The Paraffin Technique (The Gold Standard)
This is the most common, routine method used in hospitals worldwide for histological examination. It uses wax (paraffin) to support the tissue. The process takes roughly 12 to 24 hours and involves 7 exact steps:
- Tissue Sample Collection: Obtaining the live sample (e.g., via needle biopsy or surgical excision).
- Fixation: The most crucial step. The tissue is instantly submerged in a chemical (commonly 4% formaldehyde/formalin). Why? Fixatives instantly kill bacteria, stop cellular enzymes from digesting their own cell (autolysis), and cross-link proteins to lock the cell structure permanently in place.
- Dehydration: We need to put the tissue in wax, but wax and water do not mix! The tissue is passed through increasing concentrations of alcohol (e.g., 70% → 80% → 95% → 100% pure alcohol). This gently pulls all the water out of the cells.
- Clearing: Alcohol does not mix with paraffin wax either. We must replace the alcohol with a clearing agent, usually Xylene. Xylene makes the tissue look highly transparent (clear) and acts as a bridge because it mixes with both alcohol and wax.
- Impregnation (Infiltration): The tissue is placed in a warm oven containing melted, liquid soft paraffin wax. The xylene evaporates, and the liquid wax infiltrates every microscopic empty space inside the cells.
- Embedding: The tissue is placed in a small mold, covered in more melted wax, and allowed to cool. It hardens into a solid "paraffin block." The tissue is now perfectly supported from the inside out.
- Sectioning: The hard wax block is placed in a specialized machine called a Microtome (acting like an extremely precise deli-meat slicer). The microtome cuts the tissue into ultra-thin, transparent ribbons (typically 5-8 micrometers thick—thinner than a human hair!). These ribbons are floated on a warm water bath and scooped up onto a glass microscope slide.
2. The Celloidin Technique
Celloidin is a tough, rubbery nitrocellulose compound. It is used instead of paraffin for specific, difficult tissues.
- Advantages: Provides vastly superior support for incredibly hard tissues (like decalcified bones and teeth) or tissues that easily fall apart (like large whole-brain sections or the delicate layers of the eyeball). It causes minimal shrinkage and distortion, preserving perfect architecture.
- Disadvantages: It is a brutally slow, time-consuming process (taking weeks to months). It is very difficult to cut very thin sections, and requires highly specialized technical skills.
3. The Freezing Technique (Cryostat / Frozen Section)
This is the emergency, "rapid-response" method of histology.
- Advantages: Extremely rapid diagnosis (completed in 15-20 minutes). It avoids the harsh chemicals (alcohol/xylene) used in the paraffin method. Because no heat or harsh chemicals are used, it perfectly preserves sensitive molecules (DNA, RNA, enzymes, and lipids) and preserves antigens for advanced immunostaining.
- Disadvantages: The freezing process causes ice crystals that slightly distort the tissue (poor cellular detail compared to paraffin). The tissue is harder to stain beautifully. Requires an expensive, refrigerated cutting machine called a Cryostat.
Clinical Scenario (Intraoperative Consultation): A patient is on the operating table for breast cancer surgery. The surgeon cuts out the tumor but doesn't know if they left any cancer cells behind at the edges. They send the lump to the lab. The pathologist rapidly freezes the tissue, cuts it, and looks at the edges within 15 minutes. The pathologist calls the surgeon in the OR: "The margins are clear!" The surgeon can safely close the patient up, saving them from a second surgery.
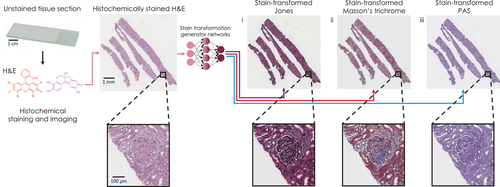
B. Staining Techniques
Because the ultra-thin sections of tissue on the glass slide are completely transparent and colorless, Staining is required. Staining uses colored chemical dyes to highlight and enhance the visibility of different tissue structures, creating a contrast.
| Stain Name | Mechanism / Colors Produced | Primary Clinical Use |
|---|---|---|
| Hematoxylin and Eosin (H&E) | The universal standard. Hematoxylin is a basic dye that binds to acidic structures (like DNA/RNA in the nucleus), turning them Blue/Purple. Eosin is an acidic dye that binds to basic structures (like cytoplasmic proteins), turning them Pink/Red. |
Routine diagnosis. It provides the standard pink-and-blue picture used to diagnose 90% of medical conditions, from inflammation to cancer. |
| PAS (Periodic Acid-Schiff) | Stains complex carbohydrates (polysaccharides) a bright, rich Magenta (Deep Red/Purple). | Used to identify basement membranes (kidney disease), mucus-secreting goblet cells (in the gut/lungs), stored glycogen (in the liver), and the tough walls of fungal infections. |
| Silver Stains (Reticulin stain) | Uses silver nitrate which deposits on specific fibers, staining them Black against a pale background. | Specifically highlights Reticular fibers (Type III Collagen). Crucial for assessing the scaffolding architecture in kidney, liver, and bone marrow biopsies. |
| Trichrome Stains (e.g., Masson's Trichrome) | Uses three different dyes to differentiate tissues. Typically stains Muscle (Red), Collagen/Fibrous tissue (Blue or Green), and nuclei (Black). | The ultimate stain for assessing Fibrosis (scarring). E.g., Diagnosing liver cirrhosis by seeing massive bands of blue scar tissue choking the red liver cells. |
| Immunostains (Immunohistochemistry / IHC) | Does not use chemical dyes. Instead, it uses laboratory-made Antibodies tagged with an enzyme or fluorescent marker. The antibody seeks out and binds strictly to one highly specific target protein (antigen) in the cell. | The ultimate modern tool for highly specific cancer diagnosis and classification. E.g., Testing a breast cancer biopsy to see if it specifically has the "HER2" protein, which dictates exactly which chemotherapy drug the patient must receive. |
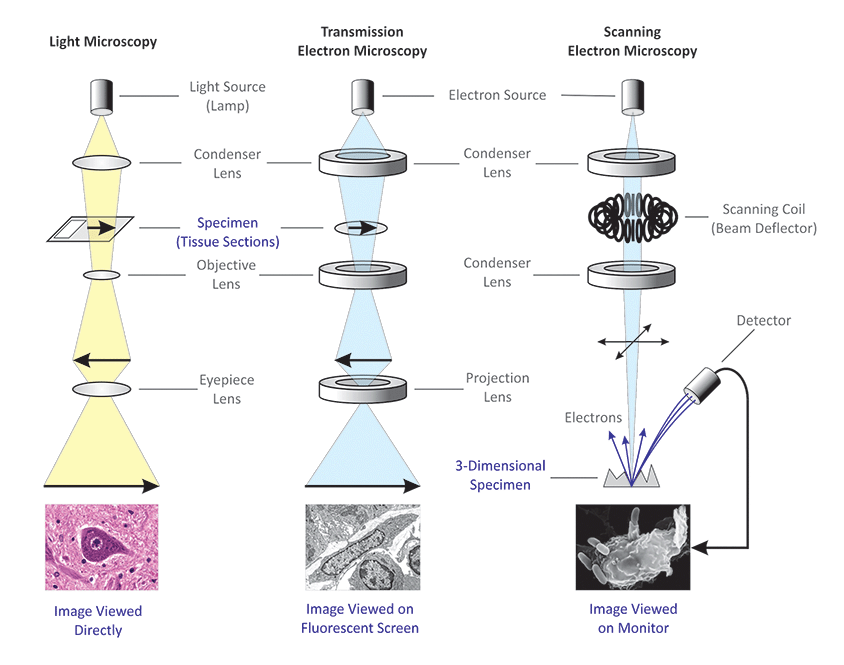
C. Microscopy Techniques
Once the slide is prepared and stained, it must be viewed. Microscopy is the use of microscopes to visualize small structures that are utterly invisible to the naked eye. There are two primary domains of microscopy:
This is the microscope you will see in every hospital and university lab.
- How it works: It uses a beam of visible photons (natural or electric light) passed through glass lenses to magnify the stained tissue section.
- Capability: It provides a 2D image and can typically magnify objects up to 1000x their normal size.
- Usage: Perfect for viewing the overall arrangement of tissues, the shape of cells, and the presence of nuclei (e.g., diagnosing a tumor from an H&E slide).
Used when we need to see the ultra-microscopic details inside the cell.
- How it works: Instead of light, it fires a beam of high-energy electrons through a vacuum, using powerful electromagnets instead of glass lenses to focus the beam.
- Capability: It offers unbelievable magnification (up to 50,000,000x)!
- Sub-Type 1: Transmission Electron Microscope (TEM): The electron beam passes through an ultra-thin slice of tissue. It provides a highly detailed 2D internal view of the cell's "guts" (organelles like mitochondria, ribosomes, and viral particles).
- Sub-Type 2: Scanning Electron Microscope (SEM): The electron beam bounces off the surface of the tissue. It provides breathtaking, highly detailed 3D surface images (e.g., looking at the microscopic hairs/cilia on the outside of a respiratory cell).
Test Your Knowledge
Check your understanding of the concepts covered in this post.
1. Histology is defined as the study of:
- Cells under a light microscope.
- Gross anatomy of organs.
- Tissues under a microscope.
- Chemical composition of biological structures.
2. Why is understanding histology important for nurses regarding medication efficacy?
- It helps them prescribe the correct dosage.
- It allows them to understand how drugs interact with specific cell types and tissues.
- It teaches them how to administer intravenous medications.
- It explains the cost-effectiveness of different drugs.
3. Which tissue preparation technique is most commonly used for routine histological examination due to its preservation and hardening properties?
- Celloidin Technique
- Freezing Technique
- Paraffin Technique
- Vital Staining
4. What is the primary disadvantage of the Celloidin Technique mentioned in the text?
- It causes significant tissue shrinkage and distortion.
- It is a very rapid process.
- It is time-consuming and difficult to cut very thin sections.
- It poorly preserves hard tissues like bone.
5. In the Paraffin Technique, what is the purpose of the 'Clearing' step?
- To replace water with alcohol.
- To harden the tissue by coagulating proteins.
- To replace alcohol with a clearing agent like xylene.
- To embed the tissue in molten paraffin.
6. Which staining technique uses positively charged dyes to stain negatively charged cellular components, such as nuclei?
- Acidic Staining
- Basic Staining
- Neutral Staining
- Metachromatic Staining
7. Which stain is described as the "most routinely used" and provides a basic architectural overview of tissues, staining nuclei blue and cytoplasm pink?
- PAS (Periodic Acid-Schiff)
- Silver Stains
- Trichrome Stains
- Hematoxylin and Eosin (H&E)
8. The Freezing Technique is particularly useful for:
- Ensuring minimal shrinkage over several days.
- Providing rapid diagnosis during surgical procedures.
- Creating very thin sections for routine examination.
- Hardening very delicate tissues like brain.
9. What is a key advantage of the Freezing Technique for molecular studies?
- It causes significant protein denaturation.
- It allows for rapid decomposition of cellular enzymes.
- It preserves biomolecules like DNA, RNA, and enzymes.
- It requires extensive prior chemical fixation.
10. Which type of electron microscope provides high-resolution images of the internal details of a specimen by passing electrons through it?
- Scanning Electron Microscope (SEM)
- Transmission Electron Microscope (TEM)
- Light Microscope
- Cryostat
11. The Greek word "histo" in histology means ________________.
12. In the Paraffin Technique, ________________ is used to remove water from the tissue by immersing it in increasing concentrations of alcohol.
13. The primary fixative commonly used in the Paraffin Technique is ________________.
14. The technique that uses antibodies to show specific molecules or cell types, crucial for cancer diagnosis, is called ________________.
15. A cryostat is used to perform sectioning for the ________________ technique.
Quiz Complete!
Your Score:
0%
0 / 0 correct
