Table of Contents
ToggleConnective Tissue: Structure, Function, and Pathophysiology
Connective Tissue (CT) is a group of tissues that connect, support, protect, and bind other tissues and organs together. Unlike epithelial tissue, which is composed almost entirely of tightly packed cells, connective tissue is defined by its vast non-living extracellular space. All connective tissues are derived from an embryonic tissue called mesenchyme.
1. Key Distinguishing Features of Connective Tissue
To identify any tissue as a "connective tissue," it must possess three overarching, distinguishing hallmarks that separate it from muscle, nervous, or epithelial tissue:
- Origin: All connective tissues—whether they are liquid blood, flexible fat, or solid bone—arise from a common embryonic tissue called mesenchyme (which originates from the embryonic mesoderm layer).
- Degree of Vascularity: Connective tissues have widely varying degrees of blood supply.
- Highly vascularized: Bone, adipose (fat) tissue, and loose areolar tissue have an incredibly rich blood supply.
- Poorly vascularized: Dense regular connective tissue (tendons and ligaments) has very few blood vessels, which is why a torn ligament takes months to heal.
- Avascular (No blood supply): Cartilage contains zero blood vessels. It relies entirely on the slow diffusion of nutrients from surrounding tissues, meaning severe cartilage injuries rarely heal on their own.
- Extracellular Matrix (ECM): This is the defining characteristic of connective tissue. In CT, cells are widely scattered within a massive amount of non-living material that they themselves produce and secrete. The ECM, consisting of ground substance and protein fibers, bears weight, withstands great tension, and absorbs physical abuse. The ECM is completely responsible for the tissue's physical properties.
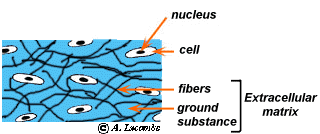
2. The Three Fundamental Components of Connective Tissue
No matter what type of connective tissue you examine, it will always be composed of three basic elements: Ground Substance, Fibers, and Cells. The ground substance and fibers together make up the Extracellular Matrix.
A. Ground Substance
This is an unstructured, amorphous, gel-like material that fills the empty space between the cells and contains the interlacing fibers. It acts as a molecular sieve through which nutrients and dissolved substances can diffuse between blood capillaries and the cells. It is composed of three main elements:
- Interstitial Fluid: A watery, plasma-derived fluid that bathes the cells.
- Adhesion Proteins: (e.g., fibronectin, laminin). These act as the molecular "glue," allowing connective tissue cells to attach securely to the matrix elements around them.
- Proteoglycans: These are massive, starburst-shaped molecules that consist of a protein core with glycosaminoglycans (GAGs) attached (like chondroitin sulfate and hyaluronic acid). These molecules trap massive amounts of water, forming a vicious, slippery gel that allows for the diffusion of nutrients and waste while resisting compressive forces.
B. Fibers
Fibers are the structural proteins secreted into the ground substance. They provide intense support and strength to the connective tissue. There are three types:
The strongest and most abundant type of fiber in the human body. They are constructed of thick, cross-linked, rope-like bundles of the protein collagen. They provide incredibly high tensile strength (the ability to resist pulling or stretching forces). Pound for pound, collagen fibers are stronger than steel fibers of the same size!
Clinical Example: Scurvy. Vitamin C is required for collagen synthesis. Without it, collagen breaks down, leading to teeth falling out and blood vessels bursting.
Long, thin, branching, and stretchy fibers containing a rubber-like protein called elastin. They allow tissues to stretch under tension and instantly recoil back to their original shape. They are heavily found where elasticity is vital: the skin, the lungs, and the walls of large blood vessels (like the aorta).
Clinical Example: Marfan Syndrome is a genetic defect in elastic fibers, leading to a high risk of aortic rupture.
Short, fine, highly branched, and delicate collagenous fibers. They branch extensively to form incredibly delicate, net-like networks (called a stroma) that support the soft tissue of organs, acting like a fuzzy "bed" for free-floating cells. Found abundantly in the spleen, liver, and lymph nodes.
C. Cells of Connective Tissue
Connective tissues contain a variety of resident cells (that live there permanently) and migrating cells (that travel through the blood to get there) with distinct roles. Each major class of connective tissue has a fundamental cell type that exists in immature and mature forms.
Primary Cell Types: "Blast" vs. "Cyte"
- "Blast" Cells (Immature & Active): The suffix -blast means "bud" or "forming." These are the highly active, dividing cells that actively secrete the ground substance and the fibers specific to their tissue matrix.
- Fibroblasts: Found in Connective Tissue Proper.
- Chondroblasts: Found in Cartilage.
- Osteoblasts: Found in Bone.
- Hematopoietic Stem Cells: Found in blood-forming tissue (bone marrow).
- "Cyte" Cells (Mature & Maintaining): Once the "blast" cells synthesize the matrix around themselves, they become trapped inside it. They mature into less active -cyte cells. Their job shifts from building the matrix to simply maintaining its health. However, if the matrix is injured, they can revert back into their active "blast" form to repair the damage.
- Fibrocytes: In Connective Tissue Proper.
- Chondrocytes: In Cartilage.
- Osteocytes: In Bone.
Other Important Cell Types (The Immune and Support Crew):
- Adipocytes (Fat Cells): Specialized cells that store energy as liquid fat (triglycerides), provide thermal insulation, and cushion organs.
- Mast Cells: Sentinel cells that initiate local inflammatory responses against foreign microorganisms they detect. They contain massive secretory granules filled with potent chemicals like histamine (causes blood vessels to leak during allergies) and heparin (an anticoagulant). Found heavily clustered near blood vessels.
- Macrophages: The "big eaters" of the immune system. They are large, irregularly shaped cells that actively engulf (phagocytize) foreign materials, bacteria, dust, and dead tissue cells.
- Plasma Cells: Specialized immune cells that produce and pump out protective antibodies into the blood.
- Leukocytes (White Blood Cells): Tissue defenders (like neutrophils, eosinophils, and lymphocytes) that migrate rapidly from the bloodstream into the connective tissue matrix to fight off acute infections and parasites.
3. Primary Functions & Main Categories of Connective Tissue
The highly diverse composition of connective tissues allows them to perform a vast array of functions in the human body, from binding and structural support to transportation and immune response. Based on their cells, fibers, and ground substance, they are broadly classified into four main categories.
- Connective Tissue Proper: Acts as a binding tissue and a packaging material. Includes Loose CT (e.g., Areolar, Adipose) and Dense CT (e.g., tendons, dermis of the skin).
- Cartilage: A tough, resilient, strong and flexible tissue that provides support and shock absorption. Includes Hyaline, Elastic, and Fibrocartilage.
- Bone Tissue (Osseous): Extremely hard connective tissue that forms the rigid skeleton, uniquely featuring a calcified matrix.
- Blood: The atypical, fluid connective tissue where the extracellular matrix is the liquid plasma, strictly designed for transport rather than physical support.
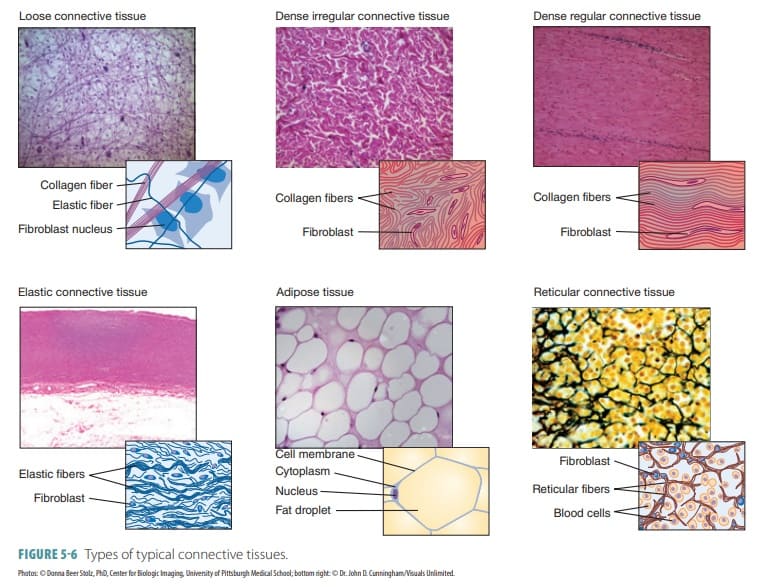
4. Connective Tissue Proper
This is the most diverse group of connective tissues. It encompasses all connective tissues EXCEPT bone, cartilage, and blood. It is divided into two main categories: Loose Connective Tissues (which have more fluid ground substance and fewer fibers) and Dense Connective Tissues (which have heavily packed fibers and very little fluid ground substance).
A. Loose Connective Tissues
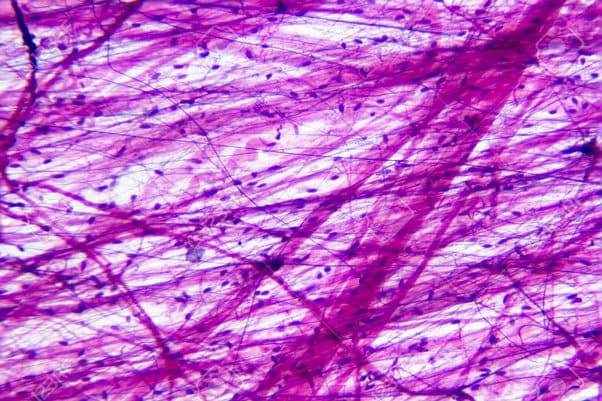 Loose Areolar Connective Tissue
Loose Areolar Connective Tissue
The most widely distributed connective tissue in the body. It serves as the universal "packing material" between other tissues. It features a loose, highly gelatinous matrix containing all three fiber types (collagen, elastic, reticular) and a vast array of cells, including fibroblasts, macrophages, and mast cells.
Histology Hint: Look for a sparse, web-like appearance with randomly arranged thick pink lines (collagen) and very thin, thread-like black/purple lines (elastic fibers), plus many scattered black dots (cell nuclei).
- Function: Wraps and cushions organs, holds massive amounts of tissue fluid (like a biological sponge), and plays a key role in the inflammatory response. (Clinical Note: When a body region is inflamed, the areolar tissue soaks up excess fluid like a sponge, causing the visible swelling known as Edema).
- Location: Widely distributed under epithelia of the body; forms the lamina propria of all mucous membranes; surrounds capillaries.
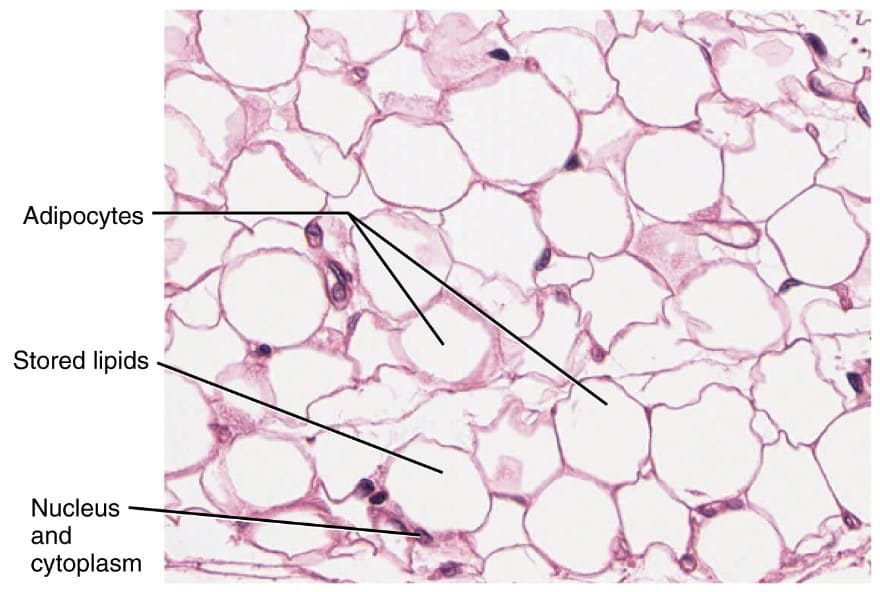 Adipose Tissue (Fat)
Adipose Tissue (Fat)
Similar matrix to areolar, but very sparse. Primarily composed of large, tightly packed adipocytes (fat cells) that account for 90% of the tissue's mass. It is highly vascularized to allow for rapid energy storage and retrieval.
Histology Hint: Characterized by large, empty-looking circular cells (adipocytes) resembling a "chicken-wire" or "signet ring" appearance. They look empty because the giant fat droplet is typically dissolved by chemicals during slide processing. The nucleus is flattened and pushed to the absolute periphery of the cell.
- Function: Massive energy storage, intense thermal insulation to prevent heat loss, and organ protection/cushioning. (Additionally acts as an endocrine organ, secreting the hormone leptin).
- Location: Under the skin (subcutaneous tissue/hypodermis), around delicate organs like kidneys and eyeballs, within the abdomen, and in the breasts.
 Reticular Connective Tissue
Reticular Connective Tissue
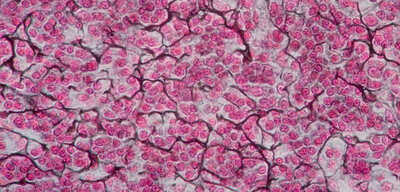
A specialized connective tissue consisting of a delicate network of fine reticular fibers within a loose ground substance. Reticular cells (specialized fibroblasts) lie scattered on the network.
Histology Hint: Look for a fine, branching network of dark-staining reticular fibers (resembling bare tree branches or a cherry blossom tree) forming a delicate internal meshwork (stroma). This meshwork is typically filled with numerous small, round, dark-staining cells (like lymphocytes waiting to attack invaders).
- Function: Forms a soft, internal skeletal framework (stroma) that supports other free-floating cell types (like white blood cells, mast cells, and macrophages) in lymphoid organs.
- Location: Lymphoid organs (lymph nodes, spleen, and bone marrow).
B. Dense (Fibrous) Connective Tissues
In dense connective tissues, fibers are the prominent element, leaving very little room for ground substance or cells.
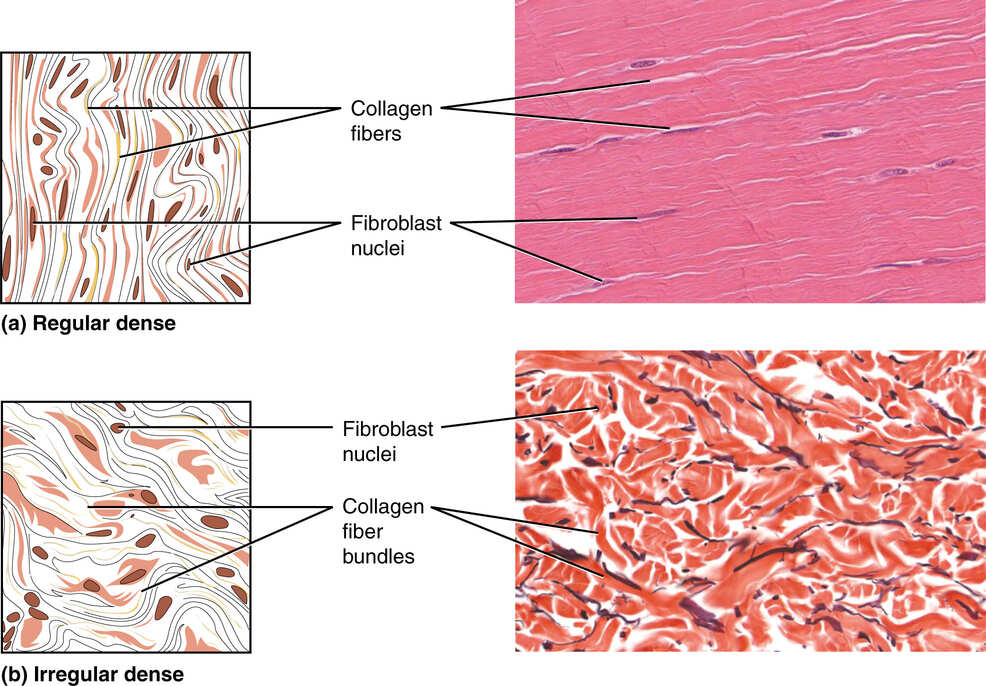
Contains densely packed, strictly parallel bundles of collagen fibers. Fibroblasts, which manufacture the fibers, are the major cell type present. Because the fibers run entirely in one direction, this tissue is incredibly strong when pulled in that specific direction. It is extremely poorly vascularized.
Histology Hint: Characterized by dense, wavy, parallel bundles of pink collagen fibers running uniformly in a single direction, resembling a flowing river or smooth wavy hair. Fibroblast nuclei are squashed, elongated, and flattened strictly between the collagen bundles.
- Function: Attaches muscles to bones (tendons) or bones to bones (ligaments). Provides magnificent tensile strength and resists pulling forces exclusively in one direction. (Example: The Achilles tendon supporting your entire body weight).
- Location: Tendons, most ligaments, and flat, sheet-like tendons called aponeuroses.
Contains the exact same structural elements as dense regular tissue (thick collagen fibers and fibroblasts), but the fibers are arranged irregularly. They interweave and run in all different, seemingly chaotic directions.
Histology Hint: Shows thick bundles of pink collagen fibers running in many different intersecting planes and directions, creating a swirling, marbled, or chaotic appearance.
- Function: Designed to withstand tension exerted from many different directions simultaneously, providing immense multi-directional structural strength.
- Location: The deep dermis of the skin (gives skin its leathery toughness and prevents it from tearing when stretched), fibrous joint capsules, and fibrous coverings of organs like the kidneys and testes.
 Elastic Connective Tissue
Elastic Connective Tissue
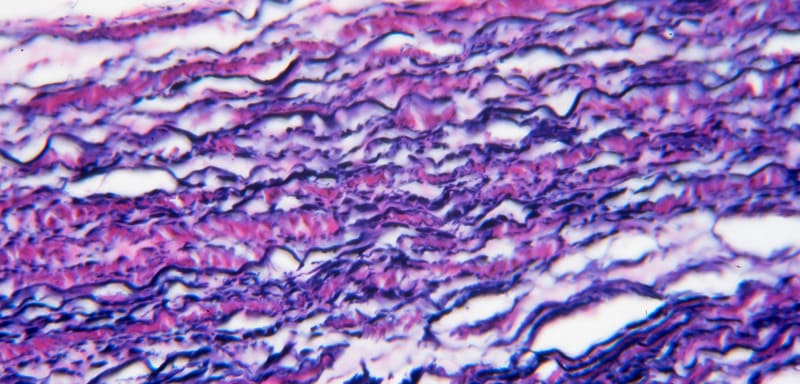
A specialized, rare type of dense regular connective tissue with an extraordinarily high proportion of stretchy elastic fibers interspersed among the collagen.
Histology Hint: Displays prominent, wavy, dark-staining elastic fibers arranged in parallel, often with a background of lighter pink collagen. Looks like densely packed, dark squiggly lines or lasagna noodles.
- Function: Allows tissue to massively stretch and violently recoil back to its original shape. Maintains the pulsatile flow of blood through major arteries and aids in the passive recoil of the lungs during expiration.
- Location: Walls of large, pressure-bearing arteries (like the Aorta), certain ligaments of the vertebral column (ligamenta flava), and walls of the bronchial tubes.
5. Cartilage
Cartilage is a tough, flexible connective tissue that stands intermediate between the rigid support of bone and the pliant nature of dense connective tissue. It consists of a firm, gelatinous matrix in which cartilage cells, or chondrocytes, are embedded within isolated fluid-filled spaces called lacunae.
Clinical Importance of Cartilage Properties:
Cartilage is entirely avascular (lacks blood vessels) and lacks nerve fibers. It relies completely on the slow diffusion of nutrients from the blood vessels located in the surrounding connective tissue membrane, known as the perichondrium. Because of this lack of direct blood supply, injured cartilage heals agonizingly slowly, and severe tears often require surgical intervention to fix.
Key Characteristics:
- Cells: Chondroblasts are the active builders that produce the new matrix until the skeleton stops growing. Once trapped, they mature into chondrocytes that maintain the matrix from within their tiny cave-like lacunae.
- Matrix: A firm, highly resilient, gel-like ground substance rich in water (up to 80% water), proteoglycans (chondroitin sulfate), and thin collagen fibers. This high water content allows cartilage to rebound after being compressed.
- Perichondrium: Most cartilages are completely surrounded by a dense irregular connective tissue membrane (the perichondrium) that physically contains the cartilage and provides its only source of nutrients.
Types of Cartilage
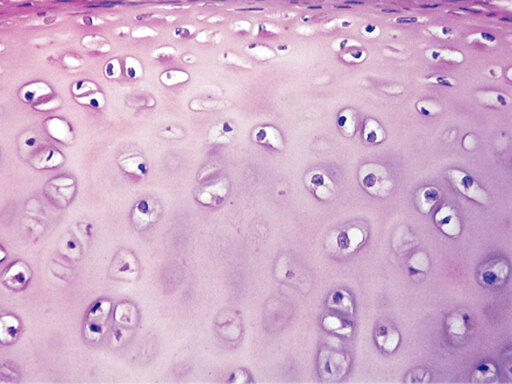
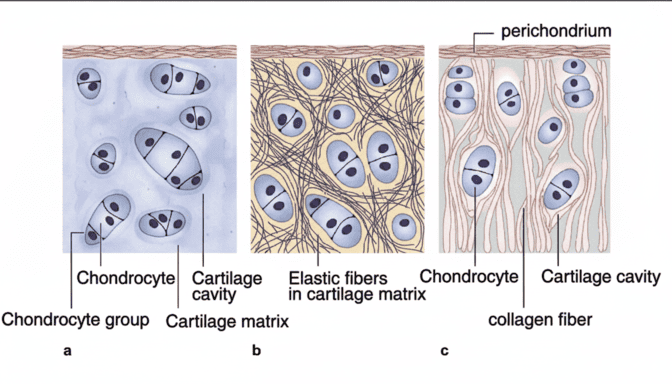
1. Hyaline Cartilage
The most abundant type of cartilage in the body. It appears as a smooth, glassy, bluish-white, semi-transparent mass. It provides a frictionless, protective covering on the ends of long bones, forms the embryonic skeleton before it turns to bone, forms the larynx, connects ribs to the sternum, and supports the air passages.
Histology Details:
- What is in between the lacunae? A firm, smooth, glassy matrix composed of water, proteoglycans, and very fine collagen fibers (the fibers are completely invisible under a light microscope, giving it a flawless "glassy" look).
- How far apart are the lacunae? They are moderately spaced, allowing for an even distribution of chondrocytes (often appearing in small clusters called isogenous groups).
Function: Provides stiff but flexible support and reinforcement, acts as a resilient, frictionless cushion in joints, and resists severe compressive stress. (Clinical Note: When this hyaline cartilage wears down over time, it leads to Osteoarthritis, causing bones to grind painfully against each other).
Location: Articular cartilages of joints, costal cartilages of ribs, cartilages of the nose, trachea, and larynx.
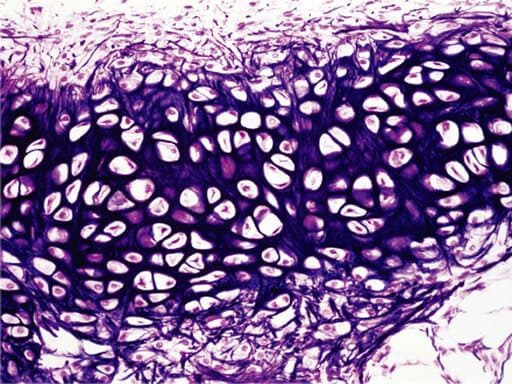
2. Elastic Cartilage
Nearly identical to hyaline cartilage in structure, but it contains a massive abundance of visible elastic fibers. This provides the tissue with exceptional elasticity, stretch, and flexibility without losing its shape.
Histology Details:
- What is in between the lacunae? A matrix containing highly visible, dark-staining, chaotic elastic fibers weaving through the ground substance, in addition to the standard collagen and proteoglycans.
- How far apart are the lacunae? Moderately spaced and very similar to hyaline cartilage, but the lacunae are often larger and more closely packed together, surrounded by the dark, hairy-looking elastic fibers.
Function: Maintains the permanent shape of a structure while allowing for magnificent flexibility and bending. (Example: You can fold your ear in half, and it snaps right back!).
Location: The framework of the external ear (pinna) and the epiglottis (the flap that bends to cover the windpipe so you don't choke when swallowing food).
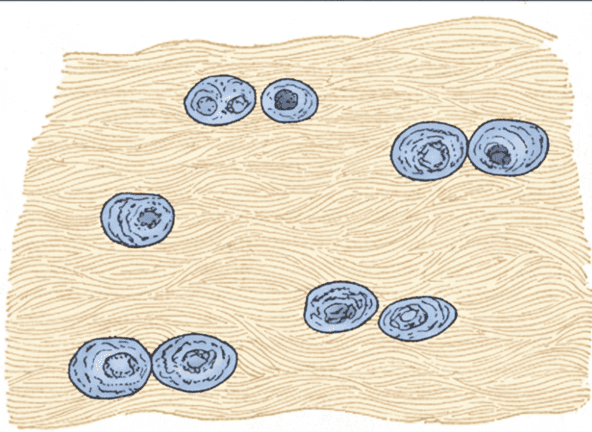
3. Fibrocartilage
The ultimate shock-absorber. It represents a structural intermediate between hyaline cartilage and dense regular connective tissue. The matrix contains extremely thick, heavily packed collagen fibers lying horizontally between short rows of chondrocytes. It is exceptionally tough and compressible.
Histology Details:
- What is in between the lacunae? A matrix completely dominated by thick, parallel, wavy bundles of pink collagen fibers, with significantly less fluid ground substance than hyaline cartilage.
- How far apart are the lacunae? Chondrocytes are often distinctly arranged in long, linear rows or chains directly squeezed between the thick collagen fiber bundles, making them more sparsely distributed than in other cartilage types.
Function: Provides immensely high tensile strength combined with the unique ability to absorb heavy compressive shock and physical pounding.
Location: Intervertebral discs (the pads between spine bones; a "slipped" or "herniated" disc is a rupture of this fibrocartilage), the pubic symphysis (the cartilage connecting the pelvis, which stretches during childbirth), and the menisci of the knee joint.
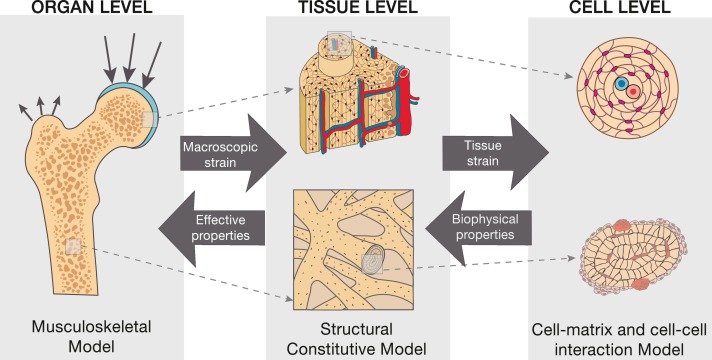
6. Bone (Osseous Tissue)
Of all the supportive connective tissues, bone is the hardest, most rigid, and most protective. This formidable strength results from its unique, highly specialized matrix.
The bone matrix is a composite material composed of two elements:
- Inorganic calcium salts (hydroxyapatite crystals): Packed heavily into the matrix to provide rock-solid hardness and the ability to resist heavy compression.
- Organic collagen fibers: Woven throughout the calcium to provide essential flexibility and extreme tensile strength (preventing the bone from shattering like glass when hit).
Unlike cartilage, bone is highly vascularized (rich with blood vessels, hence why broken bones bleed heavily and heal remarkably fast). It contains specialized cells: osteoblasts (which actively build and form the calcium matrix) and osteocytes (which are mature bone cells that maintain the matrix from within their spider-like lacunae).
Two Forms of Bone Tissue:
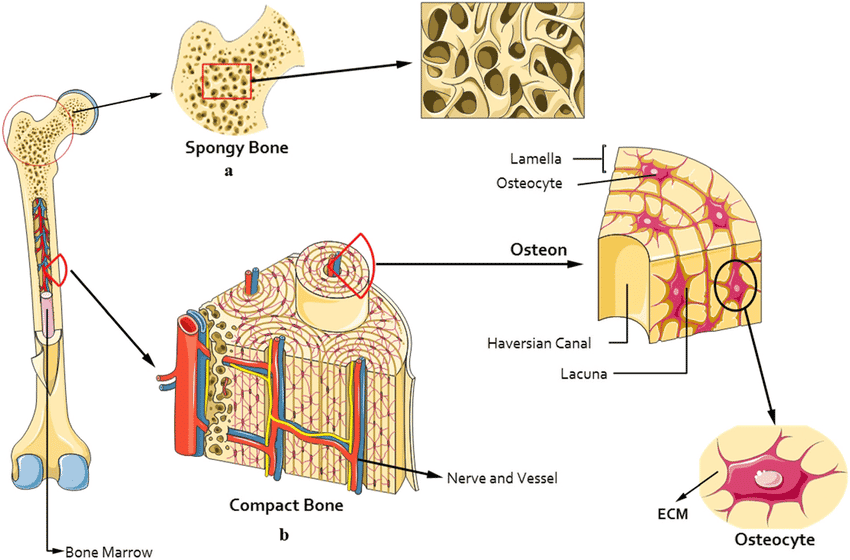
- Compact Bone (The "Hard Outer Shell"):
This is the dense, solid, heavy outer layer of almost all bones, built strictly for unyielding strength and protection against bending forces. It is intricately organized into repeating, perfectly cylindrical weight-bearing structural units called osteons (or Haversian systems). Each osteon features concentric rings of bone matrix (lamellae) surrounding a central canal containing blood vessels and nerves.
Analogy: Think of a bundle of plastic straws packed tightly together with tape. Each straw is an osteon. When packed together, they create a nearly unbreakable pillar of support.
- Spongy Bone (The "Porous Inner Core"):
Also known as cancellous or trabecular bone. This is the lighter, highly porous inner layer found at the ends of long bones and inside flat bones. It consists of a chaotic-looking network of tiny, needle-like bony struts called trabeculae. Despite looking messy, these struts align perfectly along lines of stress to distribute weight. The open spaces between the trabeculae are crucially filled with red bone marrow, the biological factory where all blood cells are produced.
Analogy: Think of a honeycomb or a porous sea sponge. It has thousands of interconnected empty spaces, making the bone light enough for us to move, but structurally sound enough to prevent collapsing.
7. Blood
Blood is the most atypical connective tissue. It does not connect things together physically, nor does it provide structural support. However, it is classified as a connective tissue because it develops from embryonic mesenchyme and consists of cells surrounded by an extracellular matrix.
Blood is the only fluid connective tissue in the human body. It uniquely consists of living blood cells (known as formed elements) suspended in a non-living fluid matrix called plasma. Unlike other connective tissues, the "fibers" in blood are normally dissolved, only becoming visible as fibrin threads during the blood clotting process.
Primary Functions of Blood:
- Transportation: The body's highway system. Delivers vital oxygen, nutrients, and hormones to all cells; picks up and carries away toxic waste products (like carbon dioxide and urea) to the lungs and kidneys for elimination.
- Regulation: Acts as a heat distributor to help maintain normal body temperature, maintains normal tissue pH using blood buffers, and regulates fluid volume in the circulatory system.
- Protection: Prevents fatal blood loss by initiating complex clotting mechanisms, and prevents devastating infections via the action of circulating antibodies, complement proteins, and white blood cells.
1. Plasma (The Extracellular Matrix)
This is the non-living, sticky, straw-colored fluid matrix that makes up about 55% of total blood volume. It is roughly 90% water and acts as the solvent for over 100 different dissolved solutes.
Key Solutes in Plasma:
- Plasma Proteins: These represent 8% by weight of plasma volume.
- Albumins: Produced by the liver, they act as the major contributor to plasma osmotic pressure, holding water inside the blood vessels so it doesn't leak into the tissues (preventing massive edema).
- Globulins: Include vital antibodies (gamma globulins) for immunity, and transport proteins that carry lipids and fat-soluble vitamins.
- Fibrinogen: A soluble protein that converts to insoluble fibrin threads during blood clotting.
- Other Solutes: Nutrients (glucose, amino acids), electrolytes (sodium, potassium, calcium), respiratory gases (oxygen, carbon dioxide), hormones, and metabolic waste products (urea, uric acid).

2. Formed Elements (The Cells)
These are the living cellular components actively suspended in the plasma, making up about 45% of total blood volume. Almost all formed elements originate from hematopoietic stem cells in the red bone marrow, and most survive in the bloodstream for only a few days to a few weeks.
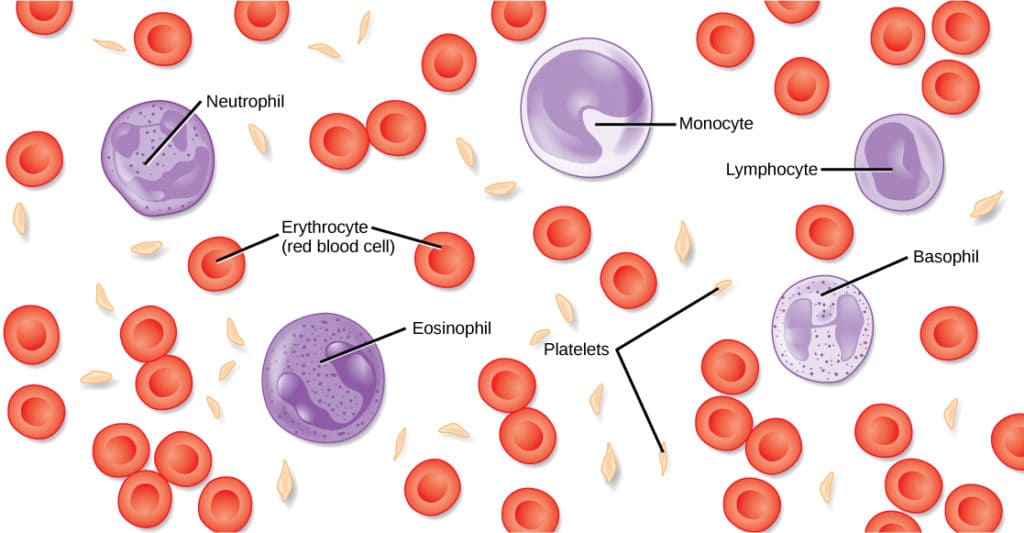
- a. Erythrocytes (Red Blood Cells - RBCs): Massive in number. They are highly specialized, anucleated (lacking a nucleus), biconcave discs essentially acting as "bags" completely filled with the iron-bearing protein hemoglobin. Their sole primary function is the highly efficient transport of oxygen from the lungs to the tissues, and carbon dioxide from the tissues back to the lungs.
- b. Leukocytes (White Blood Cells - WBCs): True, complete cells containing a nucleus and organelles. They are the mobile army of the body, crucial for immunity and defense against bacteria, viruses, parasites, and tumor cells. They are uniquely able to slip out of blood vessels (diapedesis) to mount inflammatory and immune responses in connective tissues. Includes five specific types: Neutrophils, Lymphocytes, Monocytes, Eosinophils, and Basophils.
- c. Thrombocytes (Platelets): These are not actually true cells, but rather tiny, irregular cytoplasmic fragments pinched off from massive bone marrow cells called megakaryocytes. They are absolutely essential for blood clotting (hemostasis)—they physically stick to damaged blood vessel tears to form a temporary plug, halting bleeding until coagulation can occur.
Quick Quiz
Connective Tissue Quiz
Anatomy - mobile-friendly and focused practice.
Privacy: Your details are used only for quiz tracking and certificates.
Connective Tissue Quiz
Anatomy
Preparing questions...
Choose your answer and keep your streak alive.
Great effort.
Here is your quick performance summary.
