Table of Contents
ToggleEpithelium: The Body's Lining & Covering Tissue
What is Epithelium?
Epithelium forms continuous, highly organized sheets of cells that line internal surfaces (like the lumen of the intestines or blood vessels) and cover the external surface of the body (the skin). It acts as a primary selective barrier that protects underlying and overlying tissues, regulates permeability, and is intimately involved in absorption, secretion, excretion, and sensory reception. A specialized, non-cellular layer called the basement membrane separates an epithelium from the underlying connective tissue, providing structural scaffolding and metabolic support.
Key Characteristics of Epithelial Tissue
Epithelial cells exhibit distinct polarity, meaning their top, sides, and bottom have different structures and functions. Cells are securely anchored to a basement membrane.
- Apical Surface: Faces the free space (lumen) or the external environment. This surface is often highly specialized with microvilli or cilia depending on the organ's function.
- Lateral Surface: Faces the adjacent cells. It is packed with cell junctions (tight junctions, desmosomes, and gap junctions) that lock the cells together into an impenetrable sheet and allow for cell-to-cell communication.
- Basal Surface: Attached to the basement membrane via specialized junctions called hemidesmosomes.
Epithelium is designed to be a dense, uninterrupted barrier.
- Avascularity: Epithelium contains absolutely no blood vessels. Because it is avascular, all oxygen, nutrients, and waste removal must occur via passive diffusion from the highly vascularized connective tissue located just beneath the basement membrane.
- Cellularity: Composed almost entirely of tightly packed cells with very little to no extracellular matrix between them. The cells fit together like puzzle pieces.
- High Regeneration Rate: Because epithelium is exposed to constant friction, harsh chemicals, and environmental toxins, it has a remarkable capacity for rapid mitotic division and self-renewal (e.g., you replace your entire epidermis every 28-30 days).
Origin of the Epithelial Tissues
Epithelial tissues are incredibly diverse in function and location, which is directly reflected in their embryological origins. Uniquely, epithelial tissues are derived from all three primary germ layers formed during early embryonic development. These are the primary layers of stem cells from which all tissues and organs of the body are derived.
- Ectoderm (Outermost layer)
Gives rise to structures that interact with the outside world and the nervous system.
Epithelial Derivatives & Extra Examples:
- Epidermis of the skin (and its derivatives like hair and nails).
- Lining of the oral & nasal cavities.
- Lining of the anal canal.
- Glands derived from skin (sweat glands, sebaceous glands, mammary glands).
- The anterior pituitary gland and the enamel of the teeth.
- Mesoderm (Middle layer)
Forms structures related to movement, support, and circulation.
Epithelial Derivatives & Extra Examples:
- Endothelium (the specialized simple squamous epithelium lining all blood and lymphatic vessels).
- Mesothelium (lining serous cavities such as the pleura, pericardium, and peritoneum).
- Epithelium of kidney tubules (both proximal and distal).
- Epithelium of the gonads (ovaries and testes) and the reproductive tracts.
- The adrenal cortex.
- Endoderm (Innermost layer)
Forms the lining of the digestive and respiratory systems and their associated deep internal glands.
Epithelial Derivatives & Extra Examples:
- Lining of the GI tract (from the esophagus to the upper anal canal).
- Lining of the respiratory tract (trachea, bronchi, and alveoli).
- Lining of the urinary bladder and parts of the urethra.
- Epithelium of the thyroid, parathyroid, pancreas, and liver.
- The epithelial lining of the middle ear and auditory (Eustachian) tube.
The Basement Membrane
The basement membrane (BM) is a thin, acellular, extracellular layer that underlies all epithelial tissues, separating them from the adjacent connective tissue. It is not just physical glue; it is a highly complex, chemically active interface that is a critical structural and functional component of tissue survival.
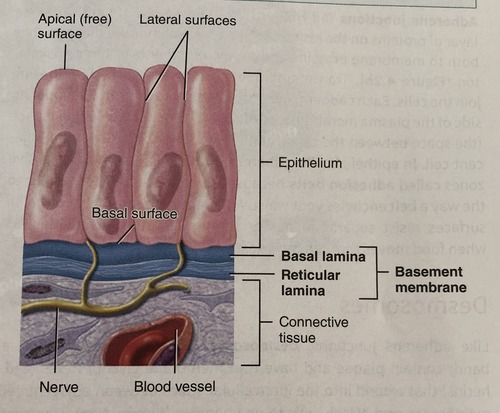
Composition & Structure
The BM is primarily composed of glycoproteins (like laminin, which acts as a sticky bridging molecule), proteoglycans (which hold water and provide cushion), and various types of collagen (especially Type IV collagen, which forms a microscopic "chicken-wire" mesh). Under an electron microscope, it is seen to have two main layers:
- Basal Lamina: Produced and secreted by the epithelial cells themselves. It is further subdivided into a clearer, upper layer (lamina lucida) and a denser, lower layer (lamina densa).
- Reticular Lamina: Produced by the underlying fibroblasts of the connective tissue. It is composed primarily of reticular fibers (Type III collagen) and anchoring fibrils (Type VII collagen) that firmly anchor the basal lamina to the connective tissue bed.
Functions of the Basement Membrane
- Structural Support: Provides a stable, flexible base for epithelial cells to anchor onto, resisting shearing forces.
- Filtration Barrier: Regulates the passage of macromolecules. Extra Example: In the glomerulus of the kidney, the basement membrane acts as a physical and electrical sieve, preventing vital plasma proteins from leaking into the urine.
- Cell Adhesion: Mediates strong attachment of epithelium to the underlying stroma via integrins and hemidesmosomes.
- Maintains Polarity: Contact with the basement membrane biochemically tells the epithelial cell which way is "down," helping define the apical-basal orientation.
- Regulates Cell Behavior: Influences cell growth, differentiation, and metabolism through chemical signals embedded in the matrix.
- Tissue Repair: Acts as a physical scaffold for regeneration. If an epithelium is scraped off but the basement membrane remains intact, new epithelial cells will rapidly glide across it to heal the wound perfectly.
Summary of Key Characteristics
- Anchored to basement membrane.
- Apical and Basal surfaces (Polarity).
- No extracellular matrix (Cellularity).
- Avascular (no blood vessels).
Clinical Correlation: Invasion and Cancer
The basement membrane is a critical, definitive marker in cancer diagnosis and staging. Benign tumors (like polyps or adenomas) respect tissue boundaries and remain confined above the BM. A hallmark of malignant tumors (cancer) is their ability to mutate and produce specialized destructive enzymes called Matrix Metalloproteinases (MMPs). These enzymes degrade the Type IV collagen of the BM, allowing the cancer cells to physically break through, invade the underlying connective tissue, access the blood vessels, and metastasize (spread to distant organs).
Classification of Epithelium
Epithelium is logically classified based on two main morphological features observed under the microscope: the number of cell layers and the shape of the cells specifically at the apical (free) surface.
| Epithelium Type | Primary Function | Key Locations |
|---|---|---|
| Simple Squamous | Ideal for rapid diffusion, osmosis, and filtration. | Alveoli of the lungs, lining of blood vessels (endothelium), lining of serous cavities (mesothelium). |
| Simple Cuboidal | Secretion and absorption. | Kidney tubules, ducts of small glands, surface of the ovary. |
| Simple Columnar | High-capacity absorption and secretion. | Gastrointestinal tract (stomach, intestines), gallbladder. |
| Stratified Squamous | Protection against physical/chemical abrasion. |
Keratinized: Surface cells are dead and filled with keratin. (Location: Epidermis of the skin). Non-keratinized: Surface cells are living. (Location: Esophagus, oral cavity, vagina). |
| Transitional (Urinary) | Allows for massive distension (stretching) and protection from toxicity. | Urinary bladder, ureters, part of the urethra. |
| Pseudostratified Ciliated Columnar | Secretion and mechanical movement of mucus. | Respiratory tract (Trachea, primary bronchi). |
Detailed Analysis of Epithelial Types
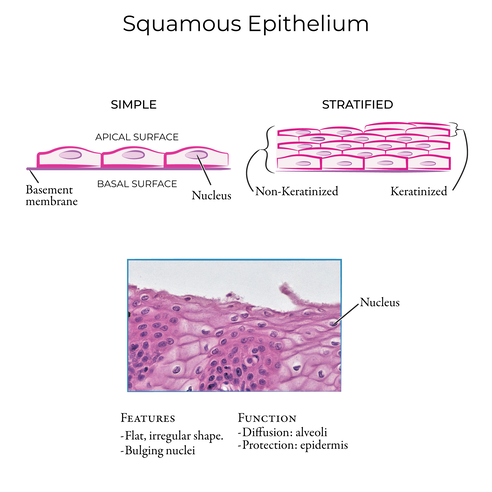
1. Simple Squamous Epithelium
Simple squamous epithelium is a single layer of extremely thin, flattened cells that forms a delicate, glass-like lining in areas where rapid diffusion, filtration, or smooth movement of substances is an absolute necessity. The extreme thinness of the cells provides minimal to no physical protection but heavily conforms to Fick's Law of Diffusion, minimizing the distance molecules must travel to allow for near-instantaneous transport.
- Classification & Defining Characteristics:
- Simple: Consists of a single layer of cells, crucial for rapid transport across the membrane.
- Squamous: Cells are flat, thin, and scale-like ("squashed"), resembling a tiled floor or fried eggs from the surface view.
- Permeable: The extreme thinness makes it highly permeable for quick exchange of gases, fluids, and nutrients.
- Structure & Appearance:
- Cell Shape: Irregularly shaped, flattened cells that interlock tightly like puzzle pieces to prevent leakage.
- Nucleus: Oval or flattened, horizontally oriented, often appearing as a central bulge in the thin cell (like the yolk of a fried egg).
- Cytoplasm: Scanty (very little), reflecting its primary role in passive transport rather than active metabolic synthesis.
- Basement Membrane: Rests on a gossamer-thin basement membrane, separating it from underlying capillary beds.
- Locations and Functions (Expanded):
Simple squamous epithelium is strategically located in areas where rapid diffusion, filtration, or a slick, friction-reducing surface is required.
- Lining of Blood & Lymphatic Vessels (Endothelium): Provides an ultra-smooth, slick, clot-preventing surface for blood flow and facilitates the rapid exchange of gases, nutrients, and waste between the blood and tissues.
- Lining of Serous Cavities (Mesothelium): Lines the pleura (lungs), pericardium (heart), and peritoneum (abdominal organs), actively producing a slippery, water-like serous fluid that lubricates organs and prevents friction as they move and expand against one another.
- Alveoli of the Lungs (Type I Pneumocytes): Forms the extremely thin "air-blood barrier" essential for rapid gas exchange (oxygen rapidly diffusing in, carbon dioxide rapidly diffusing out).
- Glomerular Capsules (Bowman's Capsule) in the Kidneys: Forms the parietal layer and the highly specialized visceral filtration membrane for blood, allowing water and small solutes to pass into the renal tubule while strictly retaining large molecules like red blood cells and albumin.
- Inner lining of the cornea and the thin segment of the Loop of Henle.
Pathology of Simple Squamous Epithelium
- Edema: Fluid accumulation (e.g., in congestive heart failure) physically pushes the basement membrane away from the capillaries, increasing the diffusion distance across the alveolar epithelium, severely impairing gas exchange and causing shortness of breath.
- Inflammation: Inflammation of serous membranes (pleuritis, pericarditis, peritonitis) causes the mesothelium to become roughened and sticky, leading to fluid accumulation (effusions) and extremely painful friction rubs heard via stethoscope.
- Cancer: Malignant mesotheliomas are aggressive, deadly cancers that arise from the mesothelium, almost exclusively linked to asbestos exposure. Additionally, a disrupted or inflamed endothelium is the initiating key factor in vascular diseases, triggering atherosclerosis and life-threatening thrombosis (blood clots).
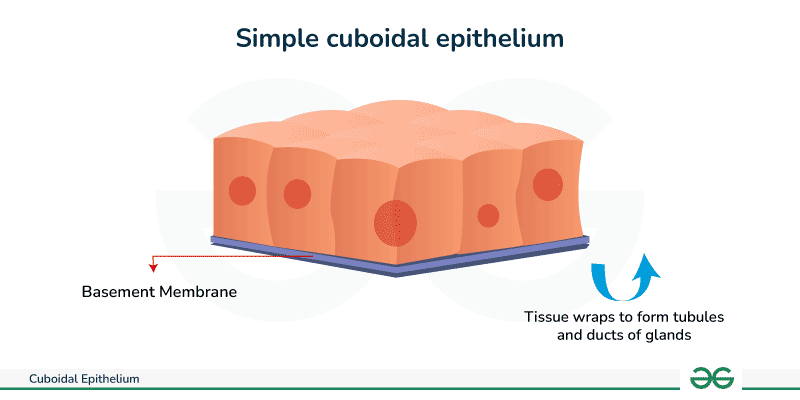
2. Simple Cuboidal Epithelium
Simple cuboidal epithelium is a single layer of cube-shaped cells, often displaying large, round, central nuclei. Unlike the passive squamous cells, cuboidal cells are packed with mitochondria and endoplasmic reticulum, primarily performing active secretion and absorption. It is found lining surfaces like kidney tubules, ducts of glands, and the surface of the ovary, where it plays a vital energy-dependent role in regulating substances and producing glandular secretions.
- Classification & Defining Characteristics:
- Simple: Consists of a single layer of cells, allowing for tightly controlled, active secretion and absorption without the barrier of multiple layers.
- Cuboidal: Cells are cube-like in shape, with a height and width that are approximately equal in cross-section.
- Central Nucleus: The nucleus is spherical, prominent, and centrally located, which is a key identifying diagnostic feature on histological slides.
- Structure & Appearance:
- Overall Shape: Forms a single layer of cells that most frequently line a duct or tubule, seamlessly encircling a central lumen (open space) like a beaded necklace.
- Cytoplasm: Contains significantly more cytoplasm and organelles (like Golgi bodies and mitochondria) than squamous cells, reflecting its highly active metabolic role in pumping ions, absorbing nutrients, and synthesizing secretions.
- Specializations: The apical surface may have microvilli (creating a fuzzy "brush border" under a microscope) to drastically increase surface area, particularly prominent in the proximal convoluted tubules of the kidney.
- Locations and Functions :
- Kidney Tubules (Proximal and Distal): Highly active in the ATP-dependent absorption of water, glucose, and amino acids from the renal filtrate back into the blood, and the active secretion of waste products, drugs, and hydrogen ions into the filtrate to become urine.
- Small Ducts of Glands: Found lining the excretory ducts of salivary glands, the pancreas, and the liver. It also forms the specialized secretory follicles of the thyroid gland, where it dynamically synthesizes, stores, and secretes thyroid hormones (T3 and T4).
- Ovary Surface (Germinal Epithelium): Provides a protective cuboidal covering for the outer surface of the ovary (historically misnamed "germinal" as it does not actually produce ova).
- Choroid Plexus of the Brain: Specialized, highly vascularized cuboidal cells that actively filter blood plasma to produce and secrete cerebrospinal fluid (CSF).
- Anterior surface of the lens of the eye.
Pathology of Simple Cuboidal Epithelium
- Polycystic Kidney Disease (PKD): A devastating genetic disorder where cysts lined by abnormal, hyper-proliferating cuboidal cells form and multiply in the kidneys. These fluid-filled cysts crush surrounding healthy tissue, ultimately leading to total kidney failure.
- Glandular Dysfunction: Thyroid disorders (like Graves' disease or Hashimoto's thyroiditis) often involve altered, hyperactive, or destroyed simple cuboidal cells that form the secretory follicles, disrupting systemic metabolism.
- Carcinomas: Cancers originating from glandular tissue are termed adenocarcinomas. Renal cell carcinoma frequently arises from the simple cuboidal epithelial cells lining the proximal convoluted tubules.
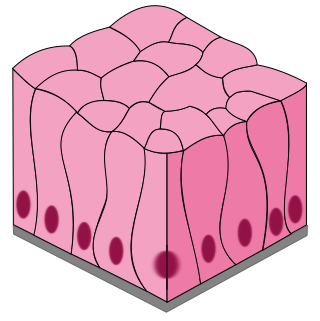
3. Simple Columnar Epithelium
Simple columnar epithelium is a highly robust single layer of tall, column-shaped cells lining the majority of the digestive tract and certain reproductive organs. These cells are highly specialized molecular machines dedicated to intense absorption and heavy secretion. They feature large, oval nuclei located near the basement membrane and often possess distinct apical specializations like microvilli or cilia to execute their specialized tasks.
- Classification & Defining Characteristics:
- Simple: A single layer of cells, maximizing efficiency for the transport of massive amounts of nutrients during absorption and secretion.
- Columnar: The cells are distinctly taller than they are wide (like skyscrapers), providing ample cytoplasmic volume to pack in the massive amounts of metabolic machinery (endoplasmic reticulum, vesicles, mitochondria) needed for their demanding tasks.
- Basal Nucleus: The nucleus is typically oval-shaped, vertically elongated, and located basally (closer to the basement membrane), which is a key diagnostic feature separating it from cuboidal cells.
- Key Specializations:
This is where simple columnar epithelium truly excels, often modifying its apical plasma membrane to adapt to its environment:
- Microvilli (Brush Border): Minute, tightly packed, finger-like projections of the plasma membrane stabilized by actin filaments. They vastly increase the total surface area available for absorption (by up to 20-fold). Found covering the enterocytes of the small intestine.
- Cilia: Longer, highly motile, whip-like projections containing a 9+2 microtubule core. They beat in a coordinated wave to propel substances or fluid along the epithelial surface. Found in the uterine (fallopian) tubes and parts of the respiratory tract.
- Goblet Cells: Highly specialized, flask-shaped unicellular glands interspersed directly among the columnar cells. They rapidly synthesize and secrete mucin (which mixes with water to become mucus) for vital lubrication and chemical protection. Abundantly found throughout the GI and respiratory tracts.
- Locations and Functions :
Simple columnar epithelium is found in areas demanding high-volume absorption, massive enzyme/mucus secretion, and active transport.
- Gastrointestinal Tract (Stomach to Rectum): In the stomach, it secretes a thick blanket of alkaline mucus to protect against harsh stomach acid, as well as digestive enzymes. In the small intestine, it is the primary site for total nutrient absorption, massively enhanced by microvilli. In the large intestine, it primarily absorbs water and contains millions of goblet cells to secrete mucus, allowing smooth passage of feces.
- Gallbladder: Lined purely by tall columnar cells primarily designed for rapid water absorption to concentrate bile. Contains microvilli but notably lacks goblet cells.
- Uterine (Fallopian) Tubes: Contains ciliated columnar cells that create a constant fluid current, helping to propel the unfertilized ovum (and later the embryo) towards the uterus for implantation, while non-ciliated cells provide nourishment.
Pathology of Simple Columnar Epithelium
- Malabsorption Syndromes: In Celiac Disease, an autoimmune reaction to gluten causes massive inflammation that physically flattens and destroys the microvilli of the intestinal columnar epithelium. This drastically reduces the absorptive surface area, leading to severe malnutrition, weight loss, and chronic diarrhea.
- Metaplasia (Barrett's Esophagus): Chronic, severe acid reflux (GERD) continuously burns the normal stratified squamous lining of the lower esophagus. To survive the acid, the tissue adapts and changes (metaplasia) into a simple columnar, mucus-secreting intestinal-type epithelium. This is Barrett's esophagus, a highly dangerous precancerous condition.
- Adenocarcinomas: Because columnar cells are highly active and mitotic, they are prone to mutation. Cancers arising from this glandular tissue, such as colorectal cancer, gastric cancer, and gallbladder cancer, are exceptionally common and originate directly from mutated simple columnar epithelium.
- Cystic Fibrosis: A genetic mutation in the CFTR chloride channel affects the function of mucus-secreting goblet cells and adjacent columnar cells, producing an abnormally thick, dehydrated, glue-like mucus that impairs clearance in the respiratory and digestive tracts, blocking pancreatic ducts and breeding lethal infections.
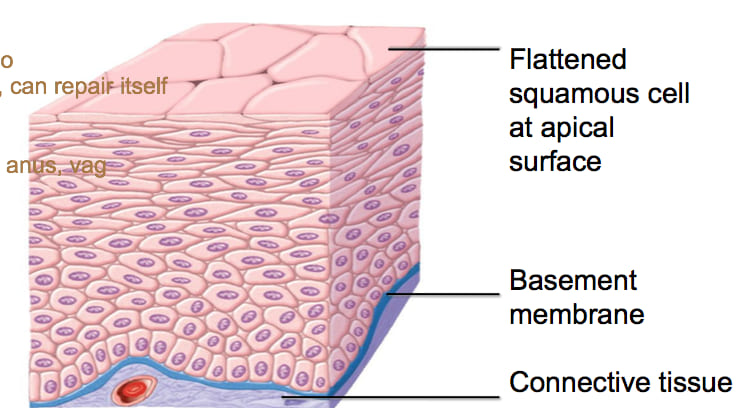
4. Stratified Squamous Epithelium
Stratified squamous epithelium is the body's premier protective tissue. Composed of multiple, stacked layers of cells, with flattened, scale-like cells terminating at the surface. Its primary function is to provide an impenetrable physical barrier against physical abrasion, invading microorganisms, harsh chemicals, and catastrophic water loss. It is the most common type of stratified epithelium in the body.
- Classification & Defining Characteristics:
- Stratified: Consists of multiple layers of cells (ranging from 5 to 50+ layers), providing robust, layered protection. As outer layers are scraped away, deeper layers instantly replace them.
- Squamous: The naming convention of stratified tissue is always based solely on the shape of the cells in the most superficial (apical) layer. In this case, the top cells are flat and scale-like (squamous), even though the deeper cells look totally different.
- Basal Layer: The deepest (basal) layer rests directly on the basement membrane. It consists of cuboidal or columnar stem cells that are actively mitotic (constantly dividing). They produce a continuous stream of new cells that are slowly pushed upward towards the surface, maturing and flattening as they go.
- Layers and Structure:
The tissue is highly organized into distinct layers (strata), tracking the lifecycle of the cell from birth to shedding.
- Basal Layer (Stratum Basale): A single layer of cuboidal/columnar stem cells resting on the basement membrane. The only layer actively undergoing mitosis.
- Intermediate Layers (Stratum Spinosum / Granulosum): Cells become more polyhedral and then progressively flatter as they are pushed upwards and further away from their blood supply. They are strongly connected by thousands of anchoring desmosomes (which look like tiny "spines" under a microscope) to prevent the tissue from tearing apart under mechanical stress.
- Superficial Layer (Stratum Corneum/Apical): Composed of entirely flattened, squamous cells, which eventually undergo apoptosis (programmed cell death) and are shed (desquamated) from the surface.
- The Two Main Subtypes:
Stratified squamous epithelium is clinically further divided based on the presence or absence of a key structural protein—keratin—in its superficial layers.
A. Keratinized Stratified Squamous
The most superficial layers are composed of entirely dead cells completely filled with cross-linked keratin filaments, a tough, fibrous, water-resistant protein. Because the cells are dead, they lack nuclei and all organelles.- Appearance: Forms a dry, tough, flaky surface layer.
- Function: Ultimate waterproofing, preventing total body dehydration, and providing extreme protection from physical abrasion and invading pathogens.
- Location: Forms the epidermis of the skin everywhere on the body (especially thick on the soles of feet and palms of hands).
B. Non-Keratinized Stratified Squamous
The superficial cells do not produce large amounts of keratin. They remain alive, metabolically active, and retain their nuclei all the way to the top layer.- Appearance: Requires a moist, wet environment to survive. Forms a slick, mucosal surface.
- Function: Protection against physical abrasion and sheer stress in internal, moist environments where extreme waterproofing is not required.
- Locations: Lines the oral cavity, pharynx, esophagus, vagina, and the lower anal canal.
Pathology of Stratified Squamous Epithelium
- Psoriasis: A chronic autoimmune condition causing severe hyperproliferation and abnormal, accelerated keratinization of the epidermis. Cells that normally take 28 days to reach the surface do so in 3-5 days, leading to the buildup of thick, itchy, red, scaly plaques.
- Cancer: Because of the constant exposure to environmental mutagens (UV radiation, HPV, chewing tobacco) and high mitotic rate, a massive percentage of human cancers originate from this tissue. Squamous Cell Carcinoma (SCC) of the skin, mouth, esophagus, and cervix are highly prevalent. A routine Pap smear is a cytological test that specifically checks for dysplastic (precancerous) morphological changes in the stratified squamous epithelium of the cervix.
- Leukoplakia: A precancerous condition involving the abnormal thickening and inappropriate hyperkeratinization of normally non-keratinized epithelium (e.g., forming tough white patches in the mouth) primarily due to chronic irritation like tobacco chewing, smoking, or poorly fitting dentures.
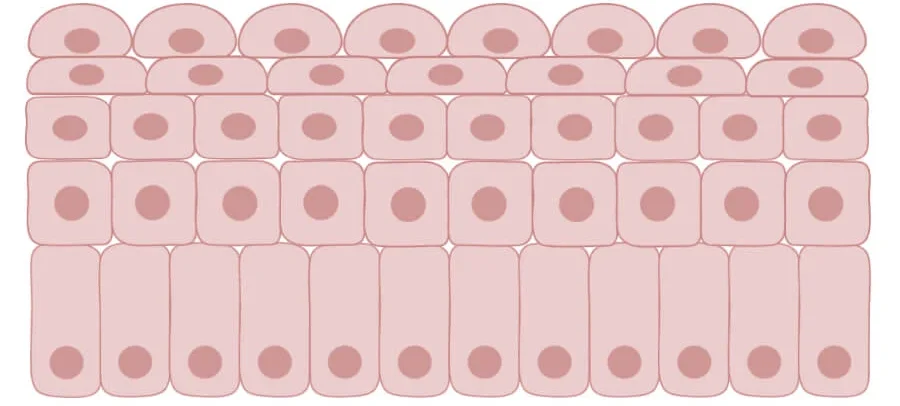
5. Transitional Epithelium (Urothelium)
Transitional epithelium, clinically known as urothelium, is a highly specialized, multi-layered type of stratified epithelium found absolutely exclusively in the urinary system. Its most remarkable, defining feature is its ability to physically stretch and recoil dramatically, allowing organs like the bladder to expand significantly to store large volumes of urine without losing structural integrity or tearing, and simultaneously maintaining a total chemical barrier that prevents the highly toxic, hypertonic components of urine from leaking back into the bloodstream or underlying tissues.
- Classification & Defining Characteristics:
While technically stratified, its key feature is its ability to dynamically change shape, or "transition," based purely on the degree of organ stretch and fluid volume.
- Relaxed / Contracted State (Empty Bladder): The tissue appears thick, having 4-6 or more cell layers. The basal cells are cuboidal, the intermediate cells are polyhedral, and the most superficial (apical) cells are large, plump, and dome-shaped (bulging into the lumen). These specialized apical cells are frequently bi-nucleated (having two nuclei) and are historically known as "umbrella cells."
- Distended / Stretched State (Full Bladder): As urine fills the organ, the epithelium is stretched tight. The entire epithelial layer remarkably thins out to just 2-3 layers. The dome-shaped umbrella cells are pulled and flatten out entirely, becoming more squamous-like (flat) in appearance to instantly accommodate the massively increased volume without tearing.
- Umbrella Cells & Impermeability:
The large, outermost umbrella cells are highly specialized feats of cellular engineering. They possess a dramatically thickened, rigid apical plasma membrane, sometimes called a "crust." This crust is formed by densely packed, crystalline plaques of specialized transmembrane proteins called uroplakins. The membrane between these plaques acts like hinges, allowing the cell membrane to fold and unfold. This unique feature makes the epithelium entirely impermeable to water and salts, forming a crucial barrier that protects the underlying cells from the hypertonic, acidic, and toxic effects of urine.
- Locations and Functions:
Transitional epithelium is strictly and exclusively found lining the hollow, distensible organs of the urinary tract:
- Renal Pelvis and Calyces of the kidney.
- Ureters.
- Urinary Bladder.
- Proximal part of the Urethra.
Pathology of Transitional Epithelium
- Bladder Cancer (Urothelial Carcinoma): The vast majority of cancers of the bladder, ureters, and renal pelvis originate from malignant mutations within this specific tissue. Chemical carcinogens excreted in the urine sit in the bladder and damage the DNA of the urothelium. Cigarette smoking and exposure to industrial aniline dyes are the absolute highest major risk factors for urothelial carcinoma.
- Urinary Tract Infections (UTIs): Despite the uroplakin barrier, specialized pathogenic bacteria (most notably uropathogenic E. coli) have evolved specific fimbriae (pili) that act as grappling hooks to selectively adhere to, invade, and colonize umbrella cells, leading to severe and recurrent infections.
- Cystitis: Severe inflammation of the bladder lining due to infection, radiation, or chemical irritation. The compromised transitional epithelium allows urine to seep into the nerve-rich underlying connective tissue, leading to excruciating symptoms like suprapubic pain, urgency, and extreme frequency of urination.
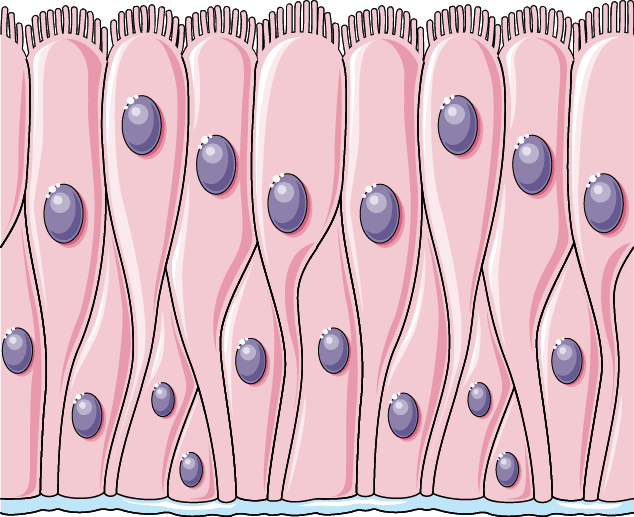
6. Pseudostratified Columnar Epithelium
Pseudostratified columnar epithelium is a tricky, specialized tissue. It is biologically a single layer of cells that deceptively appears multi-layered (stratified) under a microscope because the cell nuclei are located at wildly different heights, and the cells themselves are of different heights. However, every single cell is firmly anchored to the basement membrane. It is famously found in areas like the trachea and upper respiratory tract, where it bears millions of cilia to constantly move and clear mucus.
- Classification & Defining Characteristics:
- Pseudostratified: The defining key feature. "Pseudo" means false. It appears falsely stratified because its nuclei are stacked at different levels, giving the illusion of multiple layers. However, careful electron microscopy confirms it is a simple (single) layer as all cells touch the basement membrane (though not all reach the apical surface).
- Columnar: The functional cells that do reach the apical surface are tall and column-shaped.
- Ciliated: The surface cells almost universally possess numerous motile, hair-like cilia.
- Goblet Cells: The tissue is heavily peppered with numerous interspersed goblet cells that act as individual mucin factories to secrete protective mucus.
- Structure & Cell Types:
This "crowded," densely packed arrangement gives the illusion of stratification and contains three main, distinct cell types working in unison:
- Columnar Ciliated Cells: The tallest cells that reach the luminal surface and bear hundreds of motile cilia.
- Goblet Cells: Mucus-secreting unicellular glands interspersed among the ciliated cells, expanding near the top as they fill with mucin granules.
- Basal Cells: Short, rounded, small stem cells that sit securely on the basement membrane but never reach the surface. Their job is to constantly undergo mitosis to regenerate and replace the taller ciliated and goblet cells as they age and die.
- Locations and Functions (Expanded):
This highly specialized epithelium is almost exclusively found in the respiratory tract, where it serves as the foundation for the critical defense mechanism known as the "mucociliary escalator."
- The Mucociliary Escalator: This is its most famous, life-saving function. The interspersed goblet cells constantly produce a sticky, viscous layer of mucus that floats on top of the cilia. This mucus acts as flypaper, trapping inhaled dust, pollen, bacteria, and viral pathogens. The millions of cilia then beat in a highly coordinated, rhythmic, upward wave (powered by ATP and dynein motor proteins), sweeping the contaminated mucus "escalator" upwards away from the lungs towards the pharynx. Once at the throat, the mucus is unconsciously swallowed and destroyed by stomach acid, or coughed out as sputum. This prevents deadly foreign substances from ever reaching the delicate, sterile alveolar lung tissue.
- Key Locations: Lining the Nasal Cavity, Paranasal Sinuses, Nasopharynx, Trachea, and the large and medium-sized Bronchi.
- Exception Note: In the male reproductive tract (specifically the Epididymis), a variant of this tissue exists that has exceptionally long, immotile microvilli called stereocilia, which function entirely in fluid absorption for sperm maturation, rather than movement.
Pathology of Pseudostratified Columnar Epithelium
- Smoking: Toxic chemicals and immense heat in chronic cigarette smoke physically paralyze and eventually destroy the delicate cilia. This completely compromises the mucociliary escalator. Without the escalator, toxic mucus builds up deeply in the lungs, triggering "smoker's cough" (the body's only remaining way to clear the airway), chronic bronchitis, and massively increased risk of severe bacterial pneumonia.
- Squamous Metaplasia: Due to the constant, chronic severe irritation of smoking or harsh industrial chemicals, this delicate pseudostratified tissue will undergo metaplasia, changing into tough, protective stratified squamous epithelium. While more mechanically protective against the smoke, this new tissue lacks cilia and goblet cells. The vital escalator function is permanently lost, and the metaplastic cells are highly prone to further mutations, drastically increasing the risk of lung cancer (Squamous Cell Carcinoma of the lung).
- Primary Ciliary Dyskinesia (Kartagener Syndrome): A rare, genetic autosomal recessive disorder causing defective, immotile cilia due to mutated dynein arms. Because the cilia cannot beat, the escalator is broken from birth, leading to severe, chronic recurrent respiratory infections, bronchiectasis, and male infertility (sperm flagella use the same dynein mechanisms and cannot swim).
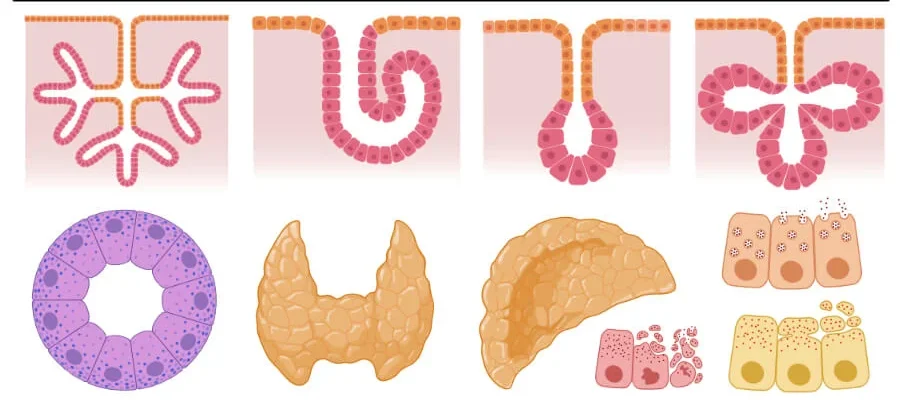
Glandular Epithelium
While lining epithelium forms barriers, Glandular epithelium is a highly specialized variant of epithelial tissue composed of cells whose entire, primary biological function is secretion. These cells are exceptionally rich in rough endoplasmic reticulum and Golgi complexes, highly specialized to synthesize, package, store, and release specific substances such as hormones, mucus, digestive enzymes, sweat, and sebum. Developmentally, all glands in the body originate and develop from localized ingrowths of epithelial sheets that burrow deep into the underlying connective tissue.
Classification of Glands
Glands are primarily classified based on where and how they release their cellular secretions:
A. Exocrine Glands (External Secretion)
These glands retain their connection to the surface epithelium. They secrete their products directly onto an internal or external epithelial surface, either directly (unicellular) or by piping the fluid through a tubular duct system.
- Examples & Locations:
- Sweat glands (eccrine and apocrine) cooling the skin.
- Salivary glands (parotid, submandibular) releasing amylase into the mouth.
- Pancreas (exocrine portion) releasing potent digestive enzymes into the duodenum via the pancreatic duct.
- Mammary glands secreting milk.
- Sebaceous (oil) glands lubricating hair follicles.
- Liver (secreting bile into the biliary ducts).
B. Endocrine Glands (Internal Secretion)
During embryonic development, these glands completely lose their duct connection to the surface epithelium. They are ductless glands. Instead, they secrete their products (powerful chemical messengers called hormones) directly into the interstitial fluid, where they immediately diffuse into the rich, surrounding capillary bloodstream to be carried to distant target organs.
- Examples & Locations:
- Thyroid gland (T3, T4 for metabolism).
- Adrenal glands (cortisol, adrenaline).
- Pituitary gland (the master control gland).
- Pancreas (endocrine islets of Langerhans) secreting insulin and glucagon.
- Ovaries & Testes (estrogen, testosterone).
Modes of Exocrine Secretion
Exocrine glands do not all work the same way. They are further classified by the cellular mechanism they use to physically release their products:
- Merocrine (Eccrine) Secretion:
- Mechanism: The most common method. The secretory products are packaged into intracellular vesicles. These vesicles fuse with the apical plasma membrane and empty their contents via standard exocytosis. The cell remains completely intact with absolute zero loss of cytoplasm or membrane.
- Examples: Salivary glands, the exocrine pancreas, and typical eccrine sweat glands covering the body.
- Apocrine Secretion:
- Mechanism: The secretory product accumulates at the very top (apical) portion of the cell. This entire apical portion of the cell's cytoplasm and cell membrane literally pinches off and is released along with the secretion. The cell survives and rebuilds its top half.
- Examples: The lactating mammary glands (releasing lipid droplets into milk) and specialized, odor-producing apocrine sweat glands in the axillary (armpit) and anogenital regions.
- Holocrine Secretion:
- Mechanism: The most destructive method. The entire cell fills to the brim with secretory products. The cell then intentionally ruptures and undergoes programmed apoptosis, releasing the product mixed with all its dead cellular debris. The gland relies on a high rate of mitosis at its base to constantly replace the exploding cells.
- Examples: Sebaceous (oil) glands of the skin, which produce thick, waxy sebum that causes acne when blocked.
Types of Secretion (Nature of the Product)
Exocrine glands are also classified by what the fluid actually looks and acts like:
- Serous: A thin, watery, protein-rich fluid, often heavily packed with active enzymes (e.g., the parotid salivary gland secreting watery amylase, or the exocrine pancreas).
- Mucous: A thick, viscous, sticky fluid (rich in heavily glycosylated glycoproteins called mucins) designed strictly for heavy lubrication and structural protection (e.g., goblet cells in the colon, or sublingual glands).
- Mixed (Seromucous): Glands that contain both serous-producing and mucous-producing cells, producing a hybrid fluid (e.g., the submandibular salivary gland).
Clinical Significance & Pathological Considerations of Glandular Epithelium
- Glandular Dysfunction (Hypo/Hyper-secretion): Many chronic systemic diseases involve the failure or overactivity of glands. Endocrine examples include Diabetes Mellitus (autoimmune destruction of the pancreatic islet beta cells, halting insulin secretion) and Hypothyroidism. A major Exocrine example includes Sjögren's syndrome (an autoimmune destruction of the lacrimal and salivary glands leading to debilitating dry eyes and dry mouth).
- Tumors/Cancers: Because glandular cells are heavily dedicated to synthesis and division, they are extremely prone to malignant transformation. Benign tumors arising from glandular epithelium are called adenomas (e.g., a benign thyroid adenoma). Malignant, invasive cancers are called adenocarcinomas. The overwhelming majority of breast, colon, pancreatic, and prostate cancers are deadly adenocarcinomas.
- Inflammation (Adenitis): Acute or chronic inflammation of glands, usually due to bacterial or viral infection, or blocked ducts. Examples include sialadenitis (painful swelling of the salivary glands, as seen in the viral Mumps infection) or mastitis (painful bacterial infection of the mammary glands during breastfeeding).
Quick Quiz
Epithelial Tissue Quiz
Anatomy - mobile-friendly and focused practice.
Privacy: Your details are used only for quiz tracking and certificates.
Epithelial Tissue Quiz
Anatomy
Preparing questions...
Choose your answer and keep your streak alive.
Great effort.
Here is your quick performance summary.
