Bipolar Affective Disorder is formerly called manic-depressive illness (MDI). B.A.D is a severe and persistent condition that causes serious lifelong struggle and challenge.
Bipolar affective disorder is a mental health condition characterized by mood swings, from deep and prolonged low mood (profound depression) to extreme euphoria (mania), with intervening normal periods.
Episodes of mood swings may occur rarely or multiple times a year. While some people will experience some emotional symptoms between episodes, some may not experience any.
Differentiating Bipolar Affective Disorder (BPAD) in children and adolescents from other psychiatric conditions is one of the most challenging aspects of pediatric psychopathology. The overlapping symptoms, developmental variability, and comorbidity make accurate diagnosis difficult but crucial for appropriate treatment.
Table of Contents
ToggleDistinguishing Feature of BAD: Episodes of Mania/Hypomania
The defining characteristic of BAD, distinguishing it from unipolar depression, is the presence of at least one manic or hypomanic episode.
- Mania: A distinct period of abnormally and persistently elevated, expansive, or irritable mood and abnormally and persistently increased goal-directed activity or energy, lasting at least one week (or any duration if hospitalization is necessary).
- Hypomania: Similar symptoms to mania but less severe, of shorter duration (at least 4 consecutive days), and not causing marked functional impairment or requiring hospitalization.
Without evidence of these episodic mood elevations, a diagnosis of BAD cannot be made. They are of three kinds i.e.
- Mixed bipolar disorder that is both manic and depressive episodes intermixed.
- Manic bipolar disorder; here there is predominant elation of mood, irritability, excessive motor activity and evident psychotic features.
- Depressed bipolar disorder; symptoms are characteristic of major depression with a history of at least one manic episode.
Differentiation from Major Depressive Disorder (MDD)
This is the most fundamental differentiation.
| Feature | Major Depressive Disorder (MDD) in Youth | Bipolar Affective Disorder (BPAD) in Youth |
|---|---|---|
| Defining Characteristic | Presence of one or more Major Depressive Episodes (MDE) without any manic or hypomanic episodes. | Presence of at least one manic episode (BP-I) or at least one hypomanic episode and one MDE (BP-II). Cyclothymic Disorder involves numerous hypomanic and depressive symptoms over at least one year that don't meet full criteria for hypomanic or MDE. |
| Mood Episodes | Only depressive episodes. | Episodes of depression and mania/hypomania. Mood can be unstable, cycling between states, or present as mixed features (co-occurring manic and depressive symptoms). |
| Irritability | Common, often chronic, and pervasive during a depressive episode. | Can be extreme, explosive, and episodic, particularly during manic/hypomanic phases. Often comes with increased energy and agitation. |
| Energy Levels | Persistently low energy, fatigue, psychomotor retardation. | Fluctuates: Very low during depression, abnormally high during mania/hypomania (restlessness, decreased need for sleep, goal-directed activity). |
| Grandiosity/Euphoria | Absent. | Hallmark of manic/hypomanic episodes. Children might express exaggerated abilities, magical thinking, or an inflated sense of self-importance. |
| Sleep | Increased sleep (hypersomnia) or decreased sleep (insomnia) with difficulty falling/staying asleep. | During mania/hypomania: Decreased need for sleep (e.g., feeling rested after only a few hours), but without feeling tired. During depression: Similar to MDD. |
| Psychosis | Can occur in severe MDD with mood-congruent psychotic features (e.g., delusions of guilt/worthlessness). | More common in BPAD, especially during manic episodes. Can be mood-congruent or mood-incongruent. |
| Family History | Family history of MDD. | Stronger family history of BPAD is a significant risk factor. |
| Treatment Response | Antidepressants are the primary pharmacological treatment. | Mood stabilizers (e.g., lithium, valproate) and atypical antipsychotics are first-line. Antidepressants used alone can sometimes induce mania/hypomania in vulnerable individuals with BPAD, necessitating careful monitoring. |
Differentiation from Attention-Deficit/Hyperactivity Disorder (ADHD)
ADHD is one of the most common comorbidities with BAD, and its symptoms often overlap, making differentiation particularly challenging.
| Feature | Attention-Deficit/Hyperactivity Disorder (ADHD) in Youth | Bipolar Affective Disorder (BPAD) in Youth (Manic/Hypomanic Phase) |
|---|---|---|
| Mood | Chronic irritability, frustration, emotional dysregulation common as a secondary feature due to difficulties with executive function. Mood is generally reactive to external stimuli. | Episodic mood shifts between distinct states (e.g., euphoric, expansive, extremely irritable, agitated) that are out of proportion to external circumstances. These mood states are qualitatively different from typical frustration or reactivity. |
| Energy Level | Chronic hyperactivity, restlessness, difficulty sitting still. Generally present across settings. | Episodic surge of energy, often described as "boundless," "wired," or "driven." Associated with decreased need for sleep. This energy often has a goal-directed (albeit often disorganized) quality that is distinct from ADHD's chronic restlessness. |
| Sleep | Difficulty falling asleep due to an active mind, but generally needs sleep. | Decreased need for sleep is a core manic symptom; the child feels rested after very little sleep. During depressive phases, can have insomnia or hypersomnia. |
| Distractibility | Chronic difficulty sustaining attention, easily diverted by external stimuli. | During mania/hypomania: Severe distractibility, often due to internal flight of ideas and racing thoughts, rather than solely external stimuli. Easily shifts from one activity or topic to another. |
| Impulsivity | Chronic difficulty waiting turn, interrupting, acting without thinking. | During mania/hypomania: Reckless impulsivity with potentially severe consequences (e.g., spending sprees, sexually inappropriate behavior, substance abuse, dangerous stunts) driven by grandiosity or impaired judgment. Differs in severity and consequences. |
| Grandiosity | Absent. | Present during manic/hypomanic episodes (e.g., exaggerated self-importance, belief in special powers/abilities, invincibility). |
| Onset | Typically early childhood (before age 12). Symptoms are usually chronic. | More commonly adolescent-onset, though can occur in childhood. Characterized by discrete episodes with periods of relative remission (though residual symptoms or rapid cycling are common in youth). |
| Family History | Family history of ADHD. | Stronger family history of BPAD. |
| Treatment | Stimulants are first-line. | Mood stabilizers/atypical antipsychotics are first-line. Stimulants can exacerbate manic symptoms or induce mania in children with underlying BPAD, so caution is needed if both are present. |
Differentiation from Disruptive Mood Dysregulation Disorder (DMDD)
DMDD was introduced in DSM-5 to address concerns about overdiagnosis of BPAD in children with severe, chronic irritability.
| Feature | Disruptive Mood Dysregulation Disorder (DMDD) | Bipolar Affective Disorder (BPAD) in Youth |
|---|---|---|
| Key Symptom | Chronic, severe, persistent irritability (mood is irritable or angry most of the day, nearly every day) and frequent, severe temper outbursts (at least 3 times/week) inconsistent with developmental level. | Episodic mood shifts with distinct periods of elevated, expansive, or euphoric mood, or periods of extreme, explosive irritability that are clearly demarcated from baseline. Irritability in BPAD is episodic and distinct, whereas in DMDD, it's chronic. |
| Mood State | Mood is persistently irritable or angry between outbursts. No distinct non-depressed, non-irritable elevated mood periods. | Mood can be irritable during a manic/hypomanic episode, but this is accompanied by other manic symptoms (decreased need for sleep, grandiosity, racing thoughts). There are also periods of distinct elevated/expansive mood, or periods of depression. |
| Episodic Nature | Not episodic. The core feature is chronic irritability. | Characterized by distinct episodes of mania/hypomania and/or depression. Between episodes, mood may return to baseline, although rapid cycling or residual symptoms are common. |
| Age of Onset/Diagnosis | Symptoms must be present before age 10, diagnosis made between ages 6 and 18. Cannot be diagnosed before age 6 or after age 18. | Can be diagnosed at any age, though often presents in adolescence. Onset can be earlier, but manic/hypomanic symptoms must meet criteria. |
| Manic/Hypomanic Episodes | Absence of full manic or hypomanic episodes. If a child meets criteria for a manic/hypomanic episode lasting more than 1 day, then DMDD cannot be diagnosed. | Requires the presence of at least one manic or hypomanic episode. |
| Prognosis | Children with DMDD are more likely to develop unipolar depression or anxiety disorders as adults, not BPAD. | Children with BPAD are at risk for recurrent mood episodes, functional impairment, and a lifelong course of illness if untreated. |
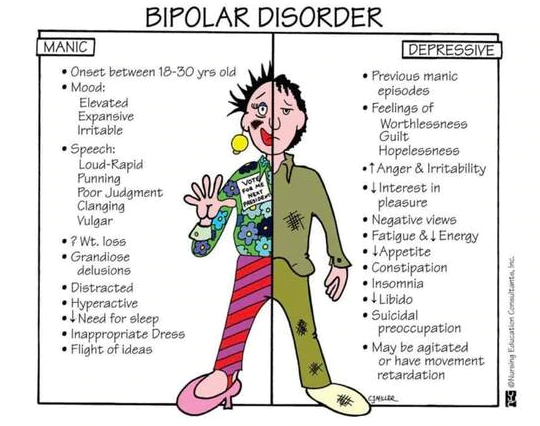
Clinical presentations of Bipolar Affective Disorder in children and adolescents
The clinical presentation of Bipolar Affective Disorder (BAD) in children and adolescents is characterized by variability based on developmental stage, individual differences, and the specific phase of the illness (manic, hypomanic, depressive, or mixed).
I. General Characteristics of Pediatric BPAD
- More Irritability than Euphoria: While adult mania often features classic euphoria, children and adolescents with BPAD frequently present with prominent, explosive, and intense irritability during manic/hypomanic episodes, sometimes without any discernible period of elevated mood. This makes it easily mistaken for ODD or DMDD.
- Rapid Cycling: A significant proportion of youth with BPAD experience rapid cycling (four or more mood episodes within a year). These shifts can be very quick, sometimes within hours or days, rather than weeks or months.
- Mixed Features: Co-occurrence of manic/hypomanic and depressive symptoms within the same episode is very common and can make diagnosis challenging. For example, a child might be extremely agitated and grandiose while simultaneously expressing feelings of worthlessness and suicidal ideation.
- Comorbidity: High rates of co-occurring conditions, especially ADHD, anxiety disorders, oppositional defiant disorder (ODD), conduct disorder (CD), and substance use disorders, complicate the clinical picture and diagnosis.
- Less Discrete Episodes: In younger children, mood states may not be as clearly demarcated as in adults; rather, there can be a chronic, underlying mood dysregulation with superimposed mood swings.
- Psychotic Features: Psychotic symptoms (hallucinations, delusions) are more common in pediatric mania than in adult mania, often manifesting as bizarre or fantastic delusions.
II. Age-Specific Manifestations
A. Preschool/Early Childhood (Ages 3-6):
- Mood: Intense, prolonged temper tantrums (lasting hours), severe irritability, aggression, inconsolable rage. Can appear "wound up" or "out of control."
- Energy/Activity: Increased energy and activity that is qualitatively different from typical childhood play; appears driven, relentless, and non-stop. Decreased need for sleep (e.g., needing only 2-3 hours but still appearing rested).
- Grandiosity: May express grandiose ideas, believe they have special powers, or engage in magical thinking far beyond typical developmental norms (e.g., believing they can fly, superhero fantasies that are acted upon with disregard for safety).
- Impulsivity: Extreme impulsivity and risk-taking behavior (e.g., running into traffic, climbing to dangerous heights without fear).
- Speech: Pressured speech, talking very rapidly, constant chatter.
- Sexualized Behaviors: Inappropriate sexualized language or behavior (rare but can occur).
- Mood: Persistent sadness, apathy, anhedonia (lack of interest in play), social withdrawal.
- Physical: Changes in appetite (overeating or undereating), sleep disturbances (hypersomnia or insomnia), low energy, psychomotor retardation.
- Cognitive: Feelings of worthlessness, guilt (e.g., "I'm a bad kid"), frequent crying spells.
- Developmental Regression: May regress in toilet training or self-care skills.
B. School-Age Children (Ages 7-12):
- Mood: Marked irritability, anger, lability (rapid shifts between euphoria, irritability, and tearfulness). May be verbally aggressive, defiant, or explosive.
- Energy/Activity: Excessive energy, hyperactivity, restlessness, agitation. Decreased need for sleep (feeling rested on minimal sleep).
- Grandiosity: Exaggerated self-esteem, inflated sense of abilities, belief in special talents or invincibility, often leading to arguments with authority figures about rules.
- Impulsivity: Engaging in risky behaviors (e.g., running away, shoplifting, dangerous dares) without considering consequences.
- Speech: Pressured speech, flight of ideas, rapid shifts between topics.
- Distractibility: Easily distracted, difficulty sustaining attention, poor concentration.
- School Impact: Significant academic decline, difficulty following rules, peer conflicts.
- Mood: Persistent sadness, hopelessness, anhedonia, tearfulness, irritability.
- Physical: Changes in appetite/weight, sleep disturbances, fatigue, somatic complaints (headaches, stomachaches).
- Cognitive: Feelings of worthlessness, guilt, self-blame, poor concentration, difficulty making decisions.
- Behavioral: Social withdrawal, decline in school performance, increased defiant behavior, self-injurious behavior.
- Suicidal Ideation: Increased risk of suicidal thoughts or attempts.
C. Adolescents (Ages 13-18):
- Mood: Can present with classic euphoria, expansiveness, or intense, sustained irritability and anger. Mood lability is common.
- Energy/Activity: High energy, restlessness, agitation, decreased need for sleep (often staying up all night for days, but not feeling tired).
- Grandiosity: Inflated self-esteem, unrealistic beliefs about talents, power, or wealth. May believe they don't need to follow rules, engage in delusional thinking.
- Impulsivity/Risk-Taking: Reckless driving, promiscuous sexual behavior, substance abuse (alcohol, illicit drugs), spending sprees, gambling, running away, engaging in illegal activities. This can lead to legal issues.
- Speech: Pressured speech, racing thoughts, flight of ideas, tangentiality.
- Psychotic Features: More common than in adults (e.g., persecutory delusions, grandiose delusions, hallucinations).
- School Impact: Severe academic decline, truancy, expulsion.
- Social: Alienation from peers, family conflict, inappropriate social behaviors.
- Mood: Profound sadness, hopelessness, anhedonia, loss of interest in hobbies/friends, irritability.
- Physical: Significant changes in appetite/weight, chronic fatigue, sleep disturbances (insomnia or hypersomnia).
- Cognitive: Poor concentration, indecisiveness, feelings of worthlessness, guilt, rumination, difficulty with schoolwork.
- Behavioral: Social isolation, withdrawal from family, substance abuse, self-harm (cutting, burning), increased somatic complaints.
- Suicidal Ideation/Attempts: Extremely high risk during depressive episodes.
Etiology Of Bipolar Affective Disorder
Bipolar Affective Disorder (BPAD) is a complex neurodevelopmental illness with a significant biological basis. While psychosocial stressors can trigger episodes, the underlying vulnerability is strongly linked to genetic factors and abnormalities in brain structure, function, and neurochemistry.
I. Genetic Predispositions:
Genetics play a powerful role in the etiology of BPAD, particularly in early-onset cases.
- High Heritability: BPAD is one of the most heritable psychiatric disorders, with heritability estimates ranging from 60-85%. This means that a significant portion of the risk for developing BPAD is passed down through genes.
- Family History: Children and adolescents with a first-degree relative (parent, sibling) who has BPAD are at a significantly higher risk (up to 10-fold) of developing the disorder themselves compared to the general population. The risk increases with the number of affected relatives.
- Polygenic Risk: BPAD is not caused by a single gene but rather by the cumulative effect of multiple genes, each contributing a small amount to the overall risk.
- Overlap with Other Disorders: Genetic research suggests some shared genetic susceptibility between BPAD and other psychiatric conditions, such as schizophrenia, ADHD, and major depressive disorder. This genetic overlap can help explain the high rates of comorbidity seen in pediatric BPAD.
- Specific Genes/Pathways: While no single "bipolar gene" has been identified, research points to genes involved in various neuronal functions, including:
- Neurotransmitter systems: Genes affecting the synthesis, reuptake, and receptor sensitivity of dopamine, serotonin, and norepinephrine.
- Ion channels: Genes regulating calcium and sodium channels, which are crucial for neuronal excitability and mood stabilization (relevant to the mechanism of action of some mood stabilizers).
- Intracellular signaling pathways: Genes involved in pathways like the GSK-3 pathway, which is targeted by lithium.
- Circadian rhythm genes: Genes that regulate the sleep-wake cycle, given the prominent sleep disturbances in BPAD.
II. Brain Structure and Functional Differences:
Neuroimaging studies (MRI, fMRI, PET) have revealed consistent structural and functional abnormalities in the brains of individuals with BAD, even in pediatric populations. These differences are often more pronounced or develop differently in early-onset BPAD compared to adult-onset.
- Structural Differences (Volume and Connectivity):
- Amygdala: Often shows increased volume in youth with BPAD, particularly the left amygdala. The amygdala is a key region involved in processing emotions, fear, and aggression. Dysregulation here can contribute to mood lability and exaggerated emotional responses.
- Hippocampus: Some studies report reduced hippocampal volume, a region critical for memory and emotion regulation, especially in those with more severe illness or repeated episodes.
- Prefrontal Cortex (PFC): The PFC, especially the ventrolateral and orbitofrontal regions, is crucial for executive functions, decision-making, impulse control, and emotional regulation. In pediatric BPAD, reduced gray matter volume or altered cortical thickness in these areas has been observed, potentially explaining difficulties with judgment and impulsivity.
- White Matter Integrity: Alterations in white matter tracts, which connect different brain regions, particularly those connecting the prefrontal cortex with limbic structures, have been found. These altered connections can disrupt efficient communication between emotion-generating and emotion-regulating networks.
- Basal Ganglia: Abnormalities in the basal ganglia, involved in motor control, motivation, and reward processing, have also been reported.
- Functional Differences (Neural Circuitry and Activation Patterns):
- Dysfunctional Emotion Regulation Networks: This is a core finding. During emotional tasks, individuals with BPAD often show:
- Increased Amygdala Activity: Over-activation of the amygdala, suggesting heightened emotional reactivity.
- Decreased Prefrontal Cortex (PFC) Activity: Under-recruitment of the PFC (ventrolateral and dorsolateral PFC), indicating impaired top-down control over emotional responses. This imbalance leads to difficulty modulating strong emotions.
- Reward Circuitry Dysfunction: Alterations in the brain's reward system (e.g., ventral striatum, nucleus accumbens) lead to exaggerated responses to rewards during manic episodes (e.g., heightened pursuit of pleasurable activities) and diminished responses during depressive episodes (anhedonia).
- Default Mode Network (DMN): Abnormalities in the DMN, a network active during resting states and self-referential thought, have been implicated, suggesting altered self-processing and introspection, which could contribute to mood disturbances.
- Abnormal Connectivity: Reduced functional connectivity between the PFC and subcortical limbic regions (amygdala, hippocampus) suggests a "disconnect" in the brain's ability to regulate emotion effectively.
- Dysfunctional Emotion Regulation Networks: This is a core finding. During emotional tasks, individuals with BPAD often show:
III. Neurotransmitter Dysregulation:
Neurotransmitters are chemical messengers that transmit signals across brain cells. Imbalances in these systems are thought to underpin the extreme mood swings in BPAD.
- Dopamine: Often considered a key player in mania.
- Mania: Excessive dopamine activity in reward pathways is hypothesized to drive increased energy, goal-directed behavior, grandiosity, and psychotic symptoms.
- Depression: Reduced dopamine activity might contribute to anhedonia, low motivation, and fatigue.
- Serotonin: Involved in mood, sleep, appetite, and impulse control.
- Mania/Depression: Dysregulation of serotonin (both excess and deficiency) can contribute to mood instability. Reduced serotonin activity is associated with depression and increased impulsivity.
- Norepinephrine (Noradrenaline): Involved in arousal, attention, and the fight-or-flight response.
- Mania: Elevated norepinephrine levels contribute to increased energy, agitation, and racing thoughts.
- Depression: Reduced norepinephrine is associated with low energy and difficulty concentrating.
- Glutamate and GABA: These are the primary excitatory (glutamate) and inhibitory (GABA) neurotransmitters in the brain.
- Imbalance: An imbalance between glutamate and GABA can lead to neuronal hyperexcitability (associated with mania) or hypoexcitability (associated with depression). Mood stabilizers like lithium and valproate are thought to modulate these systems.
- Other Neurotransmitters/Neuropeptides: Research is also exploring the role of acetylcholine, histamine, and various neuropeptides in BPAD.
Comprehensive diagnostic process for Bipolar Affective Disorder
A. Thorough History-Taking (Clinical Interview):
This is the cornerstone of diagnosis and should be conducted with the child/adolescent and primary caregivers separately, then together.
- Presenting Problem: Detailed description of current symptoms, their onset, frequency, intensity, duration, and impact on functioning.
- Past Psychiatric History:
- Previous episodes of depression, mania, hypomania, or mixed symptoms.
- Any prior diagnoses (e.g., ADHD, ODD, anxiety) and response to treatments.
- History of self-harm, suicidal ideation/attempts, aggression, impulsivity.
- Psychiatric hospitalizations or emergency room visits.
- Developmental History:
- Pregnancy and birth complications.
- Developmental milestones (motor, language, social).
- Temperament in infancy/early childhood (e.g., difficult temperament, excessive tantrums).
- Family Psychiatric History: Critically important for BPAD.
- History of BPAD, major depression, anxiety disorders, substance use, suicide in first- and second-degree relatives.
- Early-onset mood disorders in parents.
- Medical History:
- Current and past medical conditions, neurological conditions (e.g., head injury, epilepsy).
- Current medications (prescription, over-the-counter, supplements) and any illicit substance use.
- Sleep patterns, appetite changes.
- Social/Environmental History:
- School performance, academic struggles, disciplinary issues.
- Peer relationships (social isolation, conflicts).
- Family dynamics, significant stressors (e.g., parental divorce, abuse, neglect, trauma).
- Substance use history (including nicotine, alcohol, marijuana, illicit drugs).
- Home environment and safety concerns.
B. Multi-Informant Assessment:
Information from various sources provides a more complete and objective picture of the child's functioning across different settings.
- Child/Adolescent Interview:
- Assess their subjective experience of mood, energy, thoughts, and behaviors.
- Evaluate insight, judgment, and safety (e.g., suicidal/homicidal ideation).
- Use developmentally appropriate language and techniques.
- Parent/Caregiver Interview:
- Crucial for obtaining historical information, developmental context, and observations of symptoms at home.
- May use structured interviews or checklists (e.g., Parent-Rated Young Mania Rating Scale, Child Behavior Checklist).
- Teacher Reports:
- Provide invaluable information on symptoms in the school environment (e.g., attention, hyperactivity, irritability, social difficulties, academic performance).
- May use standardized rating scales (e.g., Conners Rating Scales, Vanderbilt ADHD Diagnostic Parent and Teacher Rating Scales) that can help differentiate ADHD-like symptoms from BPAD.
- Other Informants:
- If applicable, obtain information from other treatment providers (e.g., therapists, previous psychiatrists), coaches, or extended family members.
- Review previous medical/psychiatric records.
C. Application of DSM-5 Criteria:
The Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5) provides the official diagnostic criteria. For pediatric BPAD, particular attention is paid to:
- Manic Episode:
- A distinct period of abnormally and persistently elevated, expansive, or irritable mood and abnormally and persistently increased goal-directed activity or energy, lasting at least 1 week and present most of the day, nearly every day (or any duration if hospitalization is necessary).
- Three (or more) of the following symptoms (four if mood is only irritable) are present to a significant degree and represent a noticeable change from usual behavior:
- Inflated self-esteem or grandiosity.
- Decreased need for sleep (e.g., feels rested after only 3 hours of sleep).
- More talkative than usual or pressure to keep talking.
- Flight of ideas or subjective experience that thoughts are racing.
- Distractibility (i.g., attention too easily drawn to unimportant or irrelevant external stimuli).
- Increase in goal-directed activity (either socially, at school or work, or sexually) or psychomotor agitation.
- Excessive involvement in activities that have a high potential for painful consequences (e.g., engaging in unrestrained buying sprees, sexual indiscretions, foolish business investments).
- The mood disturbance is severe enough to cause marked impairment in social or occupational functioning or to necessitate hospitalization to prevent harm to self or others, or there are psychotic features.
- The episode is not attributable to the physiological effects of a substance or another medical condition.
- Hypomanic Episode: Similar symptoms to a manic episode but lasting at least 4 consecutive days, less severe, and not causing marked functional impairment or necessitating hospitalization.
- Major Depressive Episode: Five (or more) symptoms present during the same 2-week period and represent a change from previous functioning; at least one symptom is either (1) depressed mood or (2) loss of interest or pleasure.
- Bipolar I Disorder: Criteria met for at least one manic episode. Major depressive and hypomanic episodes may precede or follow the manic episode.
- Bipolar II Disorder: Criteria met for at least one hypomanic episode AND at least one major depressive episode. There has NEVER been a manic episode.
- Cyclothymic Disorder: Numerous periods with hypomanic symptoms and numerous periods with depressive symptoms for at least 1 year in children/adolescents (2 years in adults). Symptoms do not meet full criteria for hypomanic or major depressive episodes.
- "With Rapid Cycling": Specifies four or more mood episodes (manic, hypomanic, or major depressive) within 1 year.
- "With Mixed Features": Specifies that full criteria are met for a mood episode (manic, hypomanic, or depressive) AND at least three symptoms of the opposite pole are present.
D. Diagnostic Tools and Rating Scales:
While not diagnostic on their own, these tools can aid in gathering information, tracking symptom severity, and supporting clinical judgment.
- Mood Disorder Questionnaire-Adolescent Version (MDQ-A): A brief screening tool for BPAD symptoms.
- Child Mania Rating Scale (CMRS): Parent- or child-rated scale to assess manic symptoms.
- Young Mania Rating Scale (YMRS): Clinician-rated scale to assess manic symptoms.
- Children's Depression Inventory (CDI) / PHQ-9-Adolescent: To assess depressive symptoms.
- Vanderbilt ADHD Diagnostic Parent and Teacher Rating Scales: To help differentiate from ADHD.
- Semi-structured Diagnostic Interviews: (e.g., Kiddie Schedule for Affective Disorders and Schizophrenia - Present and Lifetime Version (K-SADS-PL)) often used in research and highly specialized clinical settings.
Nursing diagnoses for children and adolescents experiencing Bipolar Affective Disorder
I. Related to Mood Instability:
- Impaired Emotional Regulation related to neurobiological dysregulation and mood lability, as evidenced by rapid, extreme shifts in mood (e.g., euphoria to severe irritability/anger), difficulty modulating emotional responses, and disproportionate reactions to stressors.
Rationale: This diagnosis captures the core mood instability characteristic of BPAD, often manifesting as lability and difficulty controlling emotional expression, particularly during manic, hypomanic, or mixed episodes.
- Disturbed Thought Processes related to racing thoughts, flight of ideas, and distractibility secondary to manic/hypomanic episodes, as evidenced by disorganized speech, difficulty concentrating, impaired judgment, and illogical thinking.
Rationale: During manic phases, cognitive processes are significantly altered, impacting a child's ability to focus, think logically, and communicate coherently.
- Risk for Suicide related to depressed mood, hopelessness, mixed features (agitation with depression), impulsivity, and prior self-harm history, as evidenced by verbalizations of suicidal ideation, past attempts, or engaging in self-injurious behaviors (e.g., cutting, burning).
Rationale: The risk of suicide is significantly elevated in youth with BPAD, particularly during depressive or mixed episodes, and in the presence of impulsivity.
- Ineffective Coping related to immature coping mechanisms, overwhelming mood symptoms, and lack of adaptive problem-solving skills, as evidenced by withdrawal, aggression, self-harm, or substance use in response to emotional distress.
Rationale: Mood instability often overwhelms a child's coping abilities, leading to maladaptive behaviors.
- Disturbed Sleep Pattern related to decreased need for sleep during manic/hypomanic episodes or insomnia/hypersomnia during depressive episodes, as evidenced by reports of feeling rested on minimal sleep, difficulty falling/staying asleep, or excessive sleeping.
Rationale: Sleep disturbance is a hallmark symptom of BPAD, varying across mood states and significantly impacting functioning.
II. Related to Impulsivity and Risk-Taking Behaviors:
- Risk for Injury related to poor judgment, impulsivity, increased psychomotor activity, and disregard for consequences during manic/hypomanic episodes, as evidenced by engaging in dangerous activities (e.g., reckless driving, climbing, running away), aggression, or self-harm.
Rationale: Manic grandiosity, decreased need for sleep, and poor impulse control drastically increase the likelihood of accidents and harm.
- Impaired Social Interaction related to intrusive, irritable, or grandiose behaviors, difficulty with empathy, and rapid mood shifts, as evidenced by peer rejection, conflicts with authority figures, and lack of age-appropriate social skills.
Rationale: Impulsive and grandiose behaviors, coupled with irritability, can severely disrupt social relationships and lead to isolation.
- Ineffective Impulse Control related to neurobiological dysregulation (e.g., prefrontal cortex dysfunction) and manic/hypomanic symptoms, as evidenced by acting without thinking, interrupting others, physical aggression, or engaging in inappropriate sexual behaviors.
Rationale: This is a direct consequence of the neurological changes in BPAD, especially prominent during elevated mood states.
- Risk for Other-Directed Violence related to extreme irritability, low frustration tolerance, impulsivity, and poor anger management, as evidenced by verbal threats, physical aggression towards others, property destruction, or history of outbursts.
Rationale: Severe irritability and agitation during manic or mixed states can lead to violent or aggressive outbursts.
- Risk for Substance Abuse related to impulsivity, desire for mood alteration/self-medication, and peer pressure, as evidenced by reported or observed experimentation with drugs/alcohol, or family history of substance abuse.
Rationale: Adolescents with BPAD are at significantly higher risk for substance use, which can exacerbate mood symptoms and complicate treatment.
III. Related to Family Dynamics:
- Compromised Family Coping related to the chronic, unpredictable nature of BPAD, emotional burden, stigma, and lack of understanding of the illness, as evidenced by family conflict, caregiver exhaustion, social isolation of the family, and difficulty maintaining routines.
Rationale: BPAD profoundly impacts the entire family system, demanding significant adjustments and often leading to stress and dysfunction.
- Impaired Family Processes related to the child's mood instability, challenging behaviors, communication breakdowns, and inconsistent parenting strategies, as evidenced by lack of clear boundaries, ineffective conflict resolution, and parental guilt/blame.
Rationale: The child's symptoms can disrupt family roles, communication patterns, and overall family functioning.
- Deficient Knowledge related to the nature, symptoms, course, and management of pediatric BPAD, as evidenced by verbalized questions, unrealistic expectations for recovery, non-adherence to treatment plan, or inappropriate responses to symptoms.
Rationale: Parents and children often lack accurate information about BPAD, which is crucial for engagement in treatment and effective management.
- Caregiver Role Strain related to the demands of caring for a child with a chronic, complex mental illness, difficulty accessing resources, and managing challenging behaviors, as evidenced by reports of stress, fatigue, anxiety, depression, or feeling overwhelmed.
Rationale: The intense, long-term nature of caring for a child with BPAD places immense strain on caregivers.
Specific nursing care for a child/adolescent with BPAD
It requires a collaborative, interdisciplinary approach, with the nurse playing a central role in coordination, education, and direct care. The plan prioritizes safety, effective symptom management, and fostering resilience and adaptive coping skills.
Goals for the Child/Adolescent with BPAD:
- Achieve and maintain mood stability.
- Ensure safety (self and others) and prevent injury.
- Improve functioning in home, school, and social environments.
- Develop adaptive coping and emotion regulation skills.
- Enhance family understanding and support.
- Promote adherence to treatment.
A. Safety Management (Highest Priority)
| Nursing Diagnosis | Interventions |
|---|---|
| Risk for Suicide; Risk for Injury; Risk for Other-Directed Violence. |
|
B. Pharmacological Interventions & Management
| Nursing Diagnosis | Interventions |
|---|---|
| Impaired Emotional Regulation; Disturbed Thought Processes; Disturbed Sleep Pattern. |
|
C. Psychotherapeutic Interventions (Nurse's Role in Supporting & Facilitating)
| Nursing Diagnosis | Interventions |
|---|---|
| Ineffective Coping; Impaired Emotional Regulation; Impaired Social Interaction; Disturbed Thought Processes. |
|
D. Psychoeducational Interventions
| Nursing Diagnosis | Interventions (for patient and family) |
|---|---|
| Deficient Knowledge; Compromised Family Coping. |
|
E. Family Support and System Interventions
| Nursing Diagnosis | Interventions |
|---|---|
| Compromised Family Coping; Impaired Family Processes; Caregiver Role Strain. |
|
Mania
Mania is a core feature of Bipolar I Disorder, characterized by a distinct period of abnormally and persistently elevated, expansive, or irritable mood and abnormally and persistently increased goal-directed activity or energy.
I. Core Characteristics
- Elevated Mood: Ranges from cheerfulness and euphoria to extreme elation. This can quickly switch to irritability, anger, or hostility, especially when the individual's grandiose plans are thwarted or they are challenged.
- Increased Activity/Energy: A profound and persistent increase in goal-directed activity (socially, at work/school, sexually) or psychomotor agitation.
II. Types of Manic/Hypomanic Episodes
- Hypomania: A milder form of mania. The symptoms are similar but less severe and of shorter duration (at least 4 consecutive days).
- Impact: Does not cause marked impairment in social or occupational functioning and typically does not require hospitalization. Psychotic features are absent. While individuals in a hypomanic state may feel unusually productive or well, they often receive negative feedback from others due to their altered behavior.
- Acute Mania: A severe and full-blown manic episode.
- Impact: Symptoms are intense, causing significant impairment in functioning, and often necessitating hospitalization due to risk of harm to self or others, or severe psychotic features.
- Delirious Mania: An extreme form of mania characterized by profound excitement, severe psychomotor agitation, confusion, disorientation, and often florid psychotic symptoms (e.g., delusions, hallucinations).
- Context: While you mention "mainly found in organic psychoses," it can also occur in severe functional mania, representing a psychiatric emergency.
- Chronic Mania: A manic state that has persisted for an extended period, often years, and has proven resistant to various forms of treatment.
- Demographics: As you note, it is often seen in individuals aged 40 years and above, potentially reflecting a more entrenched or treatment-refractory illness course.
III. Etiology (Causes of Mania)
Mania is understood to arise from a complex interplay of genetic, neurobiological, and psychosocial factors.
- Genetic Factors:
- Heritability: Strong evidence indicates a significant genetic predisposition; mania "runs in families." Individuals with a first-degree relative with BPAD have a substantially higher risk.
- Neurobiological Factors (Neurotransmitter Dysregulation):
- Norepinephrine: Increased levels of norepinephrine metabolites are associated with the heightened energy, arousal, and psychomotor agitation seen in mania.
- Dopamine: Elevated dopamine levels, particularly in reward pathways, are strongly implicated in the euphoric mood, increased goal-directed behavior, grandiosity, and sometimes psychotic symptoms of mania.
- Serotonin: Imbalances in serotonin levels contribute to overall mood dysregulation. While often associated with depression, serotonin plays a complex role in mood stability, and its dysregulation can contribute to both poles of BPAD.
- Cyclothymic Personality:
- Definition: A temperament characterized by chronic, fluctuating mood states that don't meet full criteria for hypomania or depression.
- Role: While not a cause per se, a cyclothymic temperament is considered a significant risk factor or a prodromal state that can predispose an individual to developing full-blown BPAD, including manic episodes.
- Body Physic (Temperament/Constitution): This likely refers to inherent temperamental traits that might interact with other factors, though modern psychiatry focuses more on specific neurobiological and genetic markers.
- Psychosocial Factors:
- Stressors: Significant life stressors (e.g., divorce, bereavement, job loss, interpersonal conflict) can act as triggers for manic episodes, especially in genetically vulnerable individuals. These stressors often interact with biological predispositions (stress-diathesis model).
- Sleep Deprivation: Can be a potent trigger for mania or hypomania in susceptible individuals.
IV. Clinical Features of Mania (Symptoms)
The symptoms of mania are profound and affect mood, cognition, behavior, and physical functioning.
- Mood:
- Elation/Euphoria: Excessive happiness, joy, or high spirits.
- Irritability: Can rapidly shift from euphoria to extreme irritability, anger, or hostility, especially when thwarted.
- Behavioral/Activity:
- Boundless Energy/Restlessness: A significant increase in energy levels, leading to restlessness and incessant activity.
- Increased Goal-Directed Activity: Engaging in multiple activities simultaneously, often with excessive enthusiasm and poor planning (e.g., starting numerous projects, engaging in social events, excessive work).
- Psychomotor Agitation: Non-goal-directed motor activity (e.g., pacing, fidgeting).
- Excessive Involvement in Pleasurable Activities: Engaging in activities with a high potential for painful consequences (e.g., reckless spending, sexual indiscretions, foolish business investments, gambling).
- Increased Urge for Sex (High Libido): Often accompanied by disinhibition.
- Inappropriate Dressing: Selection of bright, clashing colors, excessive makeup, and jewelry, reflecting grandiosity or disinhibition.
- Cognitive/Thought Processes:
- Racing Thoughts: Subjective experience that thoughts are moving too quickly.
- Flight of Ideas: Rapidly shifting from one topic to another, often with discernible connections, but the pace makes it difficult to follow.
- Pressure of Speech/Over-talkativeness: Speaking rapidly, loudly, and often continuously, difficult to interrupt.
- Distractibility: Poor concentration, attention easily drawn to unimportant external stimuli.
- Delusions of Grandeur: Exaggerated beliefs about one's own importance, power, knowledge, or identity (e.g., believing oneself to be a celebrity, deity, or having special abilities). These are more pronounced in severe mania.
- Ideas of Reference: Belief that unrelated events, objects, or people have a particular and unusual significance to oneself.
- Lost Insight: Lack of awareness that one is ill or that one's behavior is problematic.
- Physical:
- Decreased Need for Sleep: Feeling rested after only a few hours of sleep, or experiencing total insomnia, without feeling fatigued.
- High Appetite/Lack of Time to Eat: Despite increased appetite, individuals may neglect eating due to hyperactivity, leading to weight loss and dehydration.
- Perceptual (in severe cases):
- Auditory Hallucinations: Hearing voices or sounds that are not present, common in acute mania with psychotic features.
V. Diagnosis of Mania (DSM-5 Criteria Highlights)
The diagnosis of a manic episode requires the presence of:
- Abnormally and persistently elevated, expansive, or irritable mood.
- Abnormally and persistently increased goal-directed activity or energy.
- Duration: Lasting at least 1 week and present most of the day, nearly every day (or any duration if hospitalization is necessary).
- Significant Impairment: Severe enough to cause marked impairment in social or occupational functioning, or to necessitate hospitalization, or there are psychotic features.
- Three (or more) of the following symptoms (four if mood is only irritable):
- Grandiosity (overrating one's self).
- Decreased need for sleep.
- Over-talkativeness/Pressure of speech.
- Flight of ideas/Racing thoughts.
- Distractibility.
- Increase in goal-directed activity or psychomotor agitation (Boundless energy, over activity).
- Excessive involvement in pleasurable activities with high potential for painful consequences.
VI. Management of Mania
The management of mania is multifaceted, aiming to stabilize the patient, ensure safety, and prevent recurrence.
A. Environmental and Supportive Interventions:
- Hospitalization:
- Indications: Essential for patients who are too excited, pose a risk to self or others, are severely disinhibited, unable to care for themselves (e.g., not eating, drinking, or sleeping), or are experiencing psychotic features.
- Benefits: Provides a safe, structured, and low-stimulus environment, facilitating close observation and medication management.
- Therapeutic Relationship:
- Foundation: Establishing a calm, consistent, and empathetic therapeutic relationship is paramount. It forms the basis for all nursing care and enhances patient cooperation.
- De-escalation and Restraint:
- Initial Approach: For agitated or restless patients, verbal de-escalation with a calm, firm, and direct approach should be attempted.
- Pharmacological Intervention: If verbal de-escalation is ineffective, rapid tranquilization with sedatives/antipsychotics (e.g., chlorpromazine 100-200mg IM, haloperidol 5-10mg IM) may be necessary to ensure safety. Dosages are adjusted as symptoms subside.
- Low Stimulus Environment:
- Rationale: Reducing environmental stimulation (noise, bright lights, excessive activity) helps to decrease agitation, promote calm, and reduce distractibility.
- Implementation: Quiet room, soft lighting, minimal visitors, avoidance of overstimulating activities.
- Safety Precautions:
- Remove Dangerous Objects: Crucial to remove any potential weapons or items for self-harm (e.g., sharp instruments, glass, ligatures, easily portable heavy objects).
- Constant Supervision: Close observation, sometimes 1:1, is essential, especially during acute phases.
- Physical Care:
- Nutrition and Hydration:
- Challenge: Patients are often too busy/hyperactive to eat or drink adequately, risking weight loss and dehydration.
- Intervention: Provide frequent, high-calorie, high-protein, easily portable finger foods and ample fluids. Supervise meals. Supplementation may be necessary.
- Hygiene: Supervise and assist with personal hygiene (bathing, oral care, dressing) as patients may neglect these due to preoccupation or disorganization.
- Sleep: Promote rest by creating a calm environment and administering sedating medications as prescribed.
- Nutrition and Hydration:
- Communication:
- Style: Use short, simple, direct sentences. Avoid complex explanations or arguments.
- Consistency: All staff should approach the patient with a consistent plan.
- Observation: Continuously observe and document patient behavior, mood, sleep patterns, eating habits, and toilet habits, reporting any significant changes.
- Injury Management: Attend to any injuries sustained due to hyperactivity or impulsivity.
B. Drug Treatment (Pharmacotherapy):
Pharmacotherapy is the cornerstone of acute mania management and relapse prevention.
- Antipsychotics (for acute symptom control):
- Mechanism: Used to rapidly control agitation, aggression, psychosis, and severe sleep disturbance.
- Examples:
- Chlorpromazine (CPZ): 100-1200mg in divided doses. Can be sedating.
- Thioridazine: 100-600mg in divided doses. Also noted for potentially lowering libido.
- Haloperidol: 5-15mg nocte (often 5-15mg/day, but can be given acutely as 5-10mg IM). Effective for severe agitation and psychosis.
- Note: Antipsychotics are often used acutely to stabilize the patient, and then mood stabilizers are used for long-term management.
- Mood Stabilizers (for long-term management and prophylaxis):
- Lithium Carbonate:
- First-line: Often considered the drug of choice, especially for classic euphoria-driven mania.
- Dosage: 250-550mg (this is usually a starting dose, titrated based on blood levels and clinical response, typical maintenance levels are 0.6-1.2 mEq/L).
- Monitoring: Requires regular blood level monitoring due to a narrow therapeutic window.
- Anticonvulsants (with mood-stabilizing properties):
- Sodium Valproate (Valproic Acid): 100-1500mg in divided doses (often given as Divalproex Sodium). Highly effective for mixed episodes and rapid cycling.
- Carbamazepine: 100-400mg in divided doses. Used for acute mania and maintenance.
- Other:
- Benzhexol (Artane): An anticholinergic medication, often prescribed to counteract extrapyramidal side effects of antipsychotics, not a primary treatment for mania itself.
- Lithium Carbonate:
C. Electroconvulsive Therapy (ECT):
- Indications: Highly effective for severe manic excitement, especially when rapid response is needed (e.g., severe self-harm risk, catatonia, unresponsiveness to medication) or when medications are contraindicated.
- Protocol: Typically 1-2 shocks per week for 6-9 weeks.
- Combination: Most effective when used in combination with pharmacotherapy.
D. Other Therapies:
- Occupational Therapy:
- Purpose: Helps recovering patients reintegrate into daily routines, develop vocational skills, and engage in meaningful activities.
- Individualized: The type of occupation varies based on the individual's interests and abilities.
- Psychotherapy:
- Family Psychotherapy: Crucial for helping families understand the illness, improve communication, manage stress, and develop coping strategies.
- Individual Therapy: For the patient, focusing on psychoeducation, coping skills, relapse prevention, and addressing underlying psychological issues.
- Resettlement and Follow-up:
- Continuity of Care: Essential for long-term stability. Involves coordinating with community resources, ensuring medication adherence, and facilitating ongoing therapy.
VII. Nursing Care of Manic Patients
This section reiterates and emphasizes the practical aspects of nursing care during a manic episode, integrating the points discussed above.
- Prioritize Safety: Remove dangerous objects, ensure supervision, and manage agitation effectively.
- Maintain Physical Health: Ensure adequate nutrition, hydration, sleep, and hygiene.
- Environmental Management: Create a low-stimulus, structured, and consistent environment.
- Therapeutic Communication: Use calm, direct, and simple language. Assign one nurse for consistency if possible.
- Medication Management: Administer medications, monitor effects and side effects, and provide education.
- Observation and Documentation: Continuously monitor and record changes in behavior, mood, and physical status.
- Address Injuries: Provide care for any physical injuries.
VIII. Prognosis
- Acute Episode Resolution: With appropriate treatment, most manic episodes resolve within three months, rarely lasting beyond six months.
- Risk of Recurrence: There is a significant risk of recurrence, especially if the disorder begins before 30 years of age. BPAD is a chronic, episodic illness.
- Sequential Episodes: Studies indicate that 10-20% of individuals with BPAD may experience multiple depressive episodes before their first manic episode.
- Compared to Schizophrenia: The prognosis for BPAD is generally better than for schizophrenia, particularly concerning functional outcomes.

Good
May the almighty bless the founder of this