Module Unit CN-111: Anatomy and Physiology (I)
Contact Hours: 60
Module Unit Description: Introduces students to the anatomy and physiology of the human body, covering the structure and function of different body parts and systems, specifically skeletal, muscular, circulatory, and digestive systems.
Learning Outcomes for this Unit:
By the end of this unit, the student shall be able to:
- Identify various parts of the human body and their functions.
- Differentiate the normal structure and functioning of various systems from that of abnormal conditions of the skeletal, muscular, cardiovascular and digestive systems.
Topic: Structures and functions of various body systems - Blood

Blood
Blood is a vital connective tissue that circulates throughout the body, acting as a transport system and playing roles in defense and maintaining balance. About 7% of your body weight is blood.
Blood is a fluid connective tissue. It circulates continually around the body, allowing constant communication between tissues distant from each other.
It transports:
- oxygen from the lungs to the tissues, and carbon dioxide from the tissues to the lungs for excretion,
- nutrients from the alimentary tract to the tissues, and cell wastes to the excretory organs, principally the kidneys,
- hormones secreted by endocrine glands to their target glands and tissues,
- heat produced in active tissues to other less active tissues,
- protective substances, e.g. antibodies, to areas of infection
- clotting factors that coagulate blood, minimizing bleeding from ruptured blood vessels
Composition of Blood
Blood is composed of a clear, straw-coloured, watery fluid called plasma in which several different types of blood cell are suspended. Plasma normally constitutes 55% of the volume of blood. The remaining 45% is accounted for by the cellular fraction of blood. The two fractions of blood, blood cells and plasma, can be separated by centrifugation (spinning) or by gravity when blood is allowed to stand (See the picture below). Because the cells are heavier than plasma, they sink to the bottom of any sample.
Blood makes up about 7% of body weight (about 5.6 litres in a 70 kg man). This proportion is less in women and considerably greater in children, gradually decreasing until the adult level is reached.
Blood in the blood vessels is always in motion because of the pumping action of the heart. The continual flow maintains a fairly constant environment for body cells. Blood volume and the concentration of its many constituents are kept within narrow limits by homeostatic mechanisms.
Plasma
The constituents of plasma are water (90 to 92%) and dissolved and suspended substances, including:
- plasma proteins
- inorganic salts
- nutrients, principally from digested foods
- waste materials
- hormones
- gases.
Plasma proteins
Plasma proteins, which make up about 7% of plasma, are normally retained within the blood, because they are too big to escape through the capillary pores into the tissues. They are largely responsible for creating the osmotic pressure of blood, which keeps plasma fluid within the circulation. If plasma protein levels fall, because of either reduced production or loss from the blood vessels, osmotic pressure is also reduced, and fluid moves into the tissues (oedema) and body cavities.
Plasma viscosity (thickness) is due to plasma proteins, mainly albumin and fibrinogen. Plasma proteins, with the exception of immunoglobulins, are formed in the liver.
Albumins
These are the most abundant plasma proteins (about 60% of total) and their main function is to maintain normal plasma osmotic pressure. Albumins also act as carrier molecules for free fatty acids, some drugs and steroid hormones.
Globulins
Their main functions are:
- as antibodies (immunoglobulins), which are complex proteins produced by lymphocytes that play an important part in immunity. They bind to, and neutralize, foreign materials (antigens) such as microorganisms.
- transportation of some hormones and mineral salts, e.g. thyroglobulin carries the hormone thyroxine and transferrin carries the mineral iron.
- inhibition of some proteolytic enzymes, e.g. α2 macroglobulin inhibits trypsin activity.
Clotting factors
These are responsible for coagulation of blood. Serum is plasma from which clotting factors have been removed. The most abundant clotting factor is fibrinogen.
Electrolytes
These have a range of functions, including;
- muscle contraction (e.g. Ca2+),
- transmission of nerve impulses (e.g. Ca2+and Na+),
- maintenance of acid–base balance (e.g. phosphate, ).
The pH of blood is maintained between 7.35 and 7.45 (slightly alkaline) by an ongoing complicated series of chemical activities, involving buffering systems.
Nutrients
The products of digestion, e.g. glucose, amino acids, fatty acids and glycerol, are absorbed from the alimentary tract.
Together with mineral salts and vitamins they are used by body cells for
- energy,
- heat,
- repair and replacement, and for the
- synthesis of other blood components and body secretions.
Waste products
Urea, creatinine and uric acid are the waste products of protein metabolism. They are formed in the liver and carried in blood to the kidneys for excretion.
Hormones
These are chemical messengers synthesized by endocrine glands.
Hormones pass directly from the endocrine cells into the blood, which transports them to their target tissues and organs elsewhere in the body, where they influence cellular activity.
Gases
Oxygen, carbon dioxide and nitrogen are transported round the body dissolved in plasma. Oxygen and carbon dioxide are also transported in combination with haemoglobin in red blood cells.
Most oxygen is carried in combination with haemoglobin and most carbon dioxide as bicarbonate ions dissolved in plasma. Atmospheric nitrogen enters the body in the same way as other gases and is present in plasma but it has no physiological function.
Cellular Contents of Blood
There are three types of blood cell.
- erythrocytes (red blood cells)
- platelets (thrombocytes)
- leukocytes (white blood cells).
Blood cells are synthesized mainly in red bone marrow. Some lymphocytes, additionally, are produced in lymphoid tissue.
In the bone marrow, all blood cells originate from pluripotent stem cells (i.e. capable of developing into one of a number of cell types) and go through several developmental stages before entering the blood. Different types of blood cell follow separate lines of development. The process of blood cell formation is called haemopoiesis.
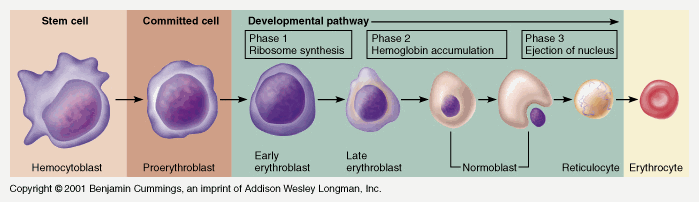 Image Placeholder - Stages in the development of blood cells diagram
Image Placeholder - Stages in the development of blood cells diagramRed Blood Cells
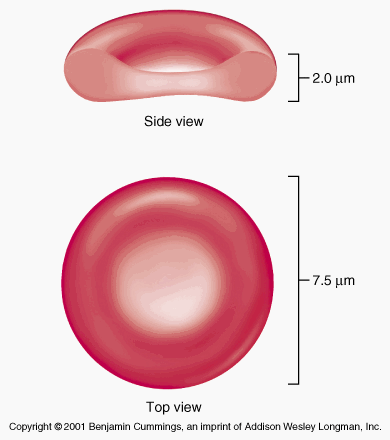
Red blood cells are biconcave discs; they have no nucleus, and their diameter is about 7.5 micrometres.
Their main function is in gas transport, mainly of oxygen, but they also carry some carbon dioxide. Their characteristic shape is suited to their purpose; the biconcavity increases their surface area for gas exchange, and the thinness of the central portion allows fast entry and exit of gases. The cells are flexible so they can squeeze through narrow capillaries, and contain no intracellular organelles, leaving more room for haemoglobin, the large pigmented protein responsible for gas transport.
Life span and function of erythrocytes
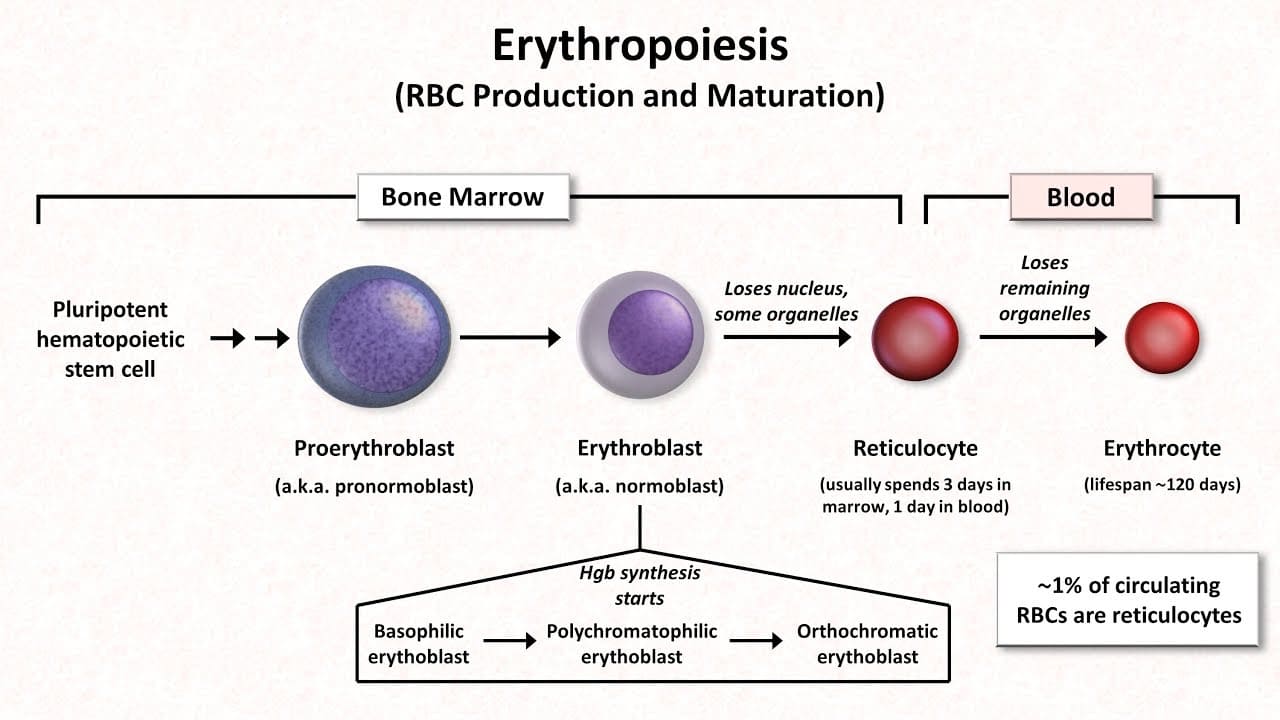
Erythrocytes or red blood cells are produced in red bone marrow, which is present in the ends of long bones and in flat and irregular bones. They pass through several stages of development before entering the blood.
Their life span in the circulation is about 120 days.
The process of development of red blood cells from stem cells takes about 7 days and is called erythropoiesis. The immature cells are released into the bloodstream as reticulocytes, and then mature into erythrocytes over a day or two within the circulation. During this time, they lose their nucleus and therefore become incapable of division.
Both vitamin B12 and folic acid are required for red blood cell synthesis. They are absorbed in the intestines, although vitamin B12 must be bound to intrinsic factor to allow absorption to take place. Both vitamins are present in dairy products, meat and green vegetables. The liver usually contains substantial stores of vitamin B12, several years’ worth, but signs of folic acid deficiency appear within a few months.
Haemoglobin
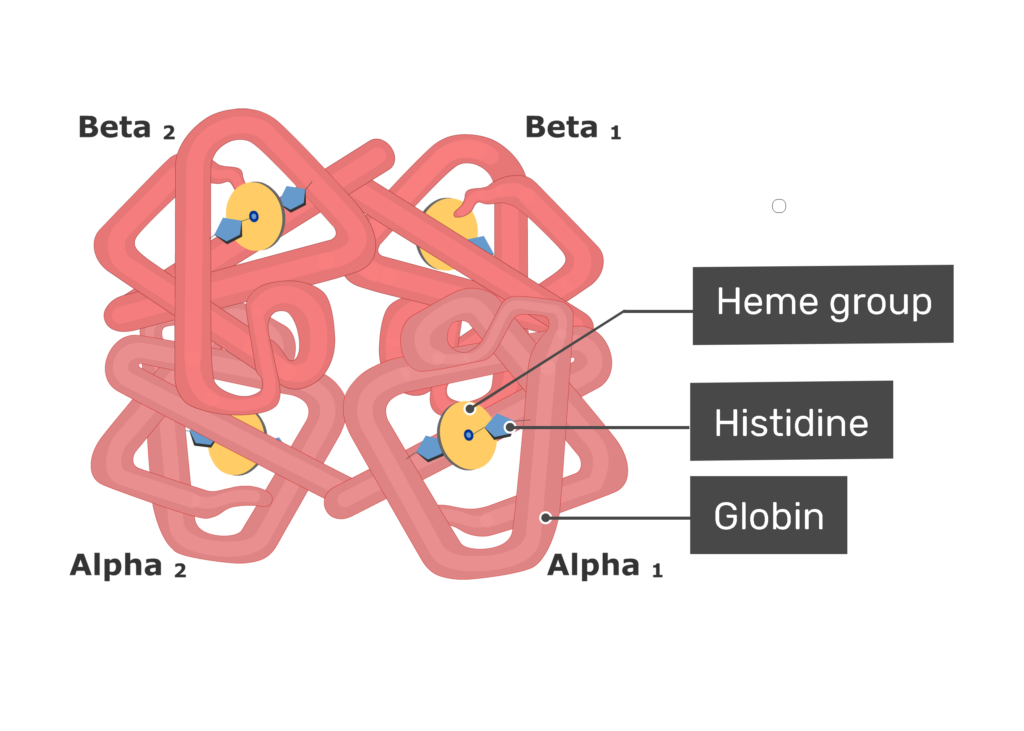
Haemoglobin is a large, complex protein containing a globular protein (globin) and a pigmented iron containing complex called haem.
Each haemoglobin molecule contains four globin chains and four haem units, each with one atom of iron. As each atom of iron can combine with an oxygen molecule, this means that a single haemoglobin molecule can carry up to four molecules of oxygen.
An average red blood cell carries about 280 million haemoglobin molecules, giving each cell a theoretical oxygen-carrying capacity of over a billion oxygen molecules.
Iron is carried in the bloodstream bound to its transport protein, transferrin, and stored in the liver. Normal red cell production requires a steady supply of iron. Iron absorption from the alimentary canal is very slow, even if the diet is rich in iron, meaning that iron deficiency can occur readily if losses exceed intake.
Control of Erythropoiesis
The rate of red blood cell production (erythropoiesis) is controlled by the body's demand for oxygen. The hormone erythropoietin, produced mainly by the kidneys, stimulates the bone marrow to produce more red blood cells when oxygen levels in the blood are low (hypoxia). This is a negative feedback mechanism that helps maintain homeostasis of oxygen carrying capacity in the blood.
Revision Questions for Blood and its Composition:
1. Describe the main functions of blood.
2. What are the two main components of blood by volume, and what percentage does each constitute?
3. List at least three types of substances transported by plasma.
4. Name the three main types of blood cells and briefly state the primary function of each.
5. Where are blood cells mainly synthesized?
6. What is the main function of erythrocytes? How is their shape suited to this function?
7. What is haemoglobin, and what is its key component for oxygen transport?
8. What is erythropoiesis, and what hormone controls this process?
References (from Curriculum for CN-1102):
Below are the core and other references listed in the curriculum for Module CN-1102. Refer to the original document for full details.
- Cohen, JB and Hull, L.K (2016) Memmlers – The Human body in Health and diseases 13th Edition, Wolters, Kluwer. (Core Reference)
- Cohen, J.B and Hull, L.K (2016) Memmler's Structure and Function of the Human Body. 11th Edition. Wolters Kluwer, China
- Kumar, M and Anand, M (2010) Human Anatomy and Physiology for Nursing and Allied Sciences. 2nd Edition. Jaypee Brothers Medical Publishers Ltd.
- Scott, N.W. (2011) Anatomy and Physiology made incredibly easy. 1st Edition. Wolwers Kluwers, Lippincotts Williams and Wilkins.
- Moore, L. K, Agur, M.R.A and Dailey, F.A. (2015) Essential Clinical Anatomy.15th Edition. Wolters Kluwer.
- Snell, S. R. (2012) Clinical Anatomy by Regions. 9th Edition. Wolters Kluwer, Lippincott Williams and Wilkins, China
- Wingerd, B, (2014) The Human Body-Concepts of Anatomy and Physiology. 3rd Edition Lippincott Williams and Wilkins and Wolters Kluwer.
- Rohen, Y.H-Orecoll. (2015) Anatomy.A Photographic Atlas 8th Edition. Lippincott Williams & Wilkins
- Waugh, A., & Grant, A. (2014). Ross and Wilson Anatomy & Physiology in Health and Illness (12th ed.). Churchill Livingstone Elsevier. (Added as per user's reference)


That’s great
Thanks…
Nice notes
Good 👍
Nice notes
Good notes 👍
Very helpful