EMPHYSEMA / PULMONARY EMPHYSEMA
Introduction
Definition: Emphysema is a chronic and progressive lung disease primarily characterized by the destruction and enlargement of the air sacs (alveoli) at the end of the smallest airways (bronchioles) in the lungs. This damage leads to a significant reduction in the surface area available for gas exchange, resulting in chronic and progressively worsening difficulty breathing.
More specifically, emphysema is a pathological diagnosis that affects the air spaces distal to the terminal bronchiole. It is defined by an abnormal, permanent enlargement of the air spaces, accompanied by the destruction of their walls without obvious fibrosis. This destruction of the lung parenchyma leads to a loss of elastic recoil, increased air trapping, thoracic over-distention (hyperinflation), and often, a compromised function of the diaphragm. While sputum accumulation can be present, it is more characteristic of chronic bronchitis, which often coexists with emphysema.
Pulmonary emphysema is a major component and a progressive form of Chronic Obstructive Pulmonary Disease (COPD). The Global Initiative for Chronic Obstructive Lung Disease (GOLD) defines COPD as "a common, preventable, and treatable disease that is characterized by persistent respiratory symptoms and airflow limitation that is due to airway and/or alveolar abnormalities usually caused by significant exposure to noxious particles or gases."
NB: Emphysema, Chronic Bronchitis, and Asthma (when overlapping with persistent airflow limitation) are the primary disease entities that fall under the umbrella term of COPD.
Pathology (Pathophysiology)
The core pathological process in emphysema involves the irreversible breakdown of the elastic fibers and walls of the alveoli, which are the tiny air sacs responsible for gas exchange. This destruction leads to the coalescence of smaller air sacs into larger, irregularly shaped, and less efficient air spaces. The process unfolds as follows:
- Alveolar Destruction and Enlargement: The delicate walls separating individual alveoli are progressively destroyed. This leads to the formation of fewer, but much larger, air-filled spaces. These enlarged spaces, often referred to as bullae if they are greater than 1 cm in diameter, have significantly reduced surface area for the efficient exchange of oxygen into the blood and carbon dioxide out of it.
- Loss of Elastic Recoil: The lung tissue, particularly the elastic fibers that normally allow the lungs to recoil and expel air during exhalation, are damaged or lost. This loss of elasticity means that air becomes trapped within the enlarged air spaces, leading to hyperinflation of the lungs.
- Air Trapping: Due to the loss of elastic recoil and the destruction of alveolar walls, air becomes trapped in the lungs, particularly during exhalation. This increases the residual volume and functional residual capacity, leading to a perpetually overinflated chest.
- Bronchiolar Collapse: The small airways (bronchioles) that lead to the alveoli are also affected. Due to the loss of surrounding parenchymal support and elastic recoil, these airways tend to collapse prematurely during exhalation, further contributing to air trapping.
- Inflammation and Protease-Antiprotease Imbalance: The primary trigger for this destructive process is chronic exposure to irritants, most notably cigarette smoke. These irritants activate an inflammatory response in the lungs. Inflammatory cells (e.g., neutrophils, macrophages) release proteolytic enzymes, particularly neutrophil elastase, which are capable of breaking down elastic fibers and connective tissue in the lung. Normally, the lungs are protected by anti-proteases, such as alpha-1 antitrypsin (AAT). However, in individuals exposed to smoke, the activity of these protective anti-proteases is overwhelmed or directly inhibited by components of cigarette smoke. This imbalance between proteases and anti-proteases leads to the unchecked destruction of the alveolar walls and the breakdown of elastic tissue and collagen.
- Impaired Gas Exchange: The loss of alveolar tissue drastically reduces the surface area available for gas exchange. Additionally, the destruction of the capillary beds surrounding the alveoli (which are part of the alveolar wall) leads to reduced blood flow through the pulmonary capillary system. This combined effect severely impairs the transfer of oxygen into the blood and the removal of carbon dioxide.
- Permanent Damage: The damage to the alveolar structures and elastic tissue is permanent and irreversible. While interventions can manage symptoms and slow progression, the ability to breathe properly cannot be fully restored once this destruction has occurred.

Causes of Emphysema
Emphysema is predominantly caused by long-term exposure to inhaled irritants, with genetic factors playing a significant role in susceptibility for some individuals.
- Occupational Dusts: Such as coal dust (in coal miners), grain dust, cotton dust, and silica.
- Chemical Fumes: Exposure to cadmium, isocyanates, and other industrial chemicals.
- Indoor Air Pollution: Smoke from biomass fuels (e.g., wood, animal dung) used for cooking and heating in poorly ventilated homes, particularly common in developing countries.
- Outdoor Air Pollution: Chronic exposure to high levels of urban air pollution, including particulate matter and ozone.
Contributory Risk Factors (can exacerbate or increase susceptibility)
- Bronchial Asthma: While distinct, severe, chronic, or poorly controlled asthma can lead to airway remodeling and contribute to fixed airflow obstruction, sometimes blurring the lines with COPD, especially "asthma-COPD overlap syndrome."
- Aging: As people age, natural changes occur in the lung structure, including a decrease in elastic recoil, which can make them more susceptible to emphysema.
- Infections: Frequent respiratory infections can accelerate lung damage in susceptible individuals.
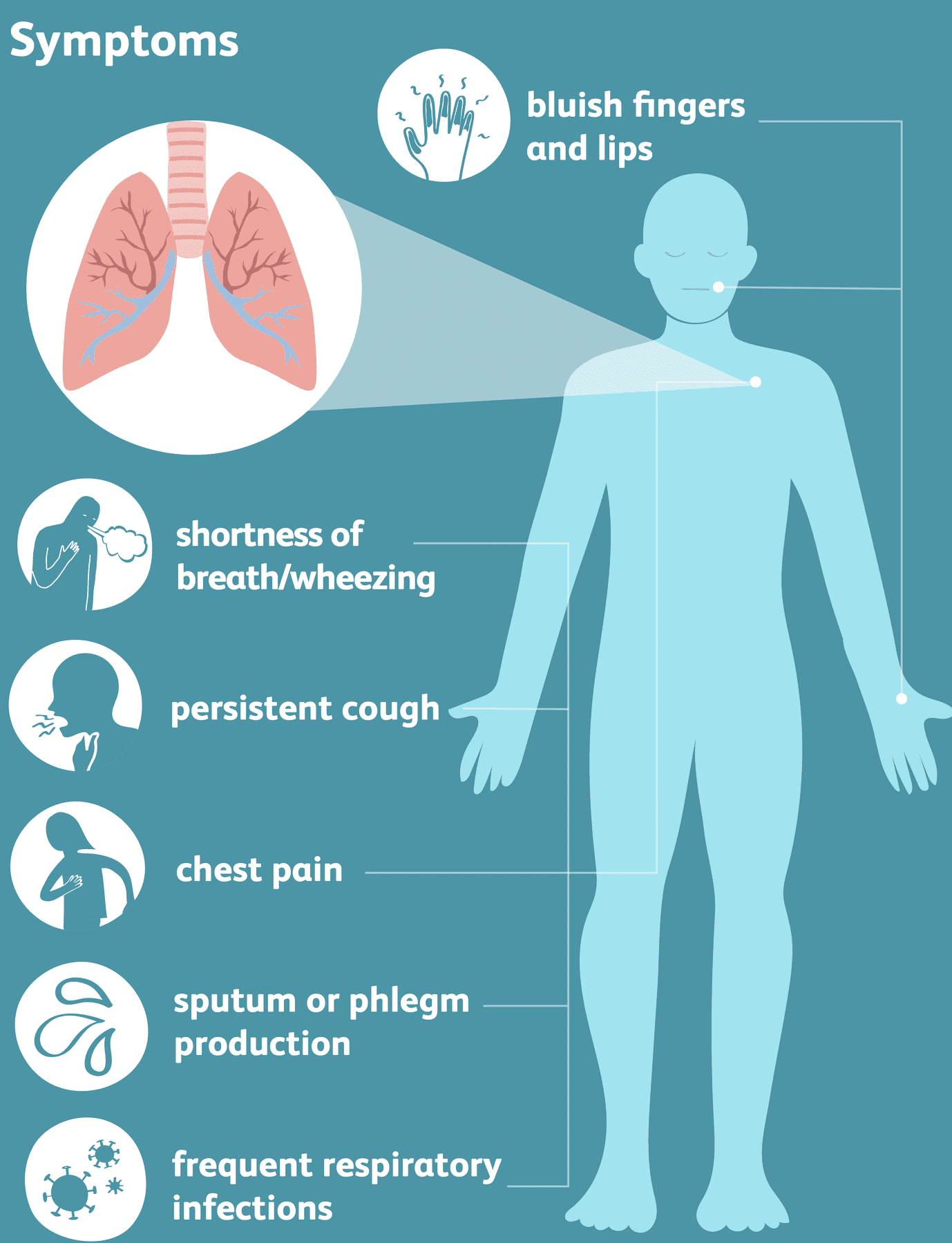
Signs and Symptoms of Emphysema
The symptoms of emphysema typically develop gradually over many years and progressively worsen. They reflect the impaired gas exchange and increased work of breathing.
- Dyspnea (Shortness of Breath): This is the hallmark symptom and is typically progressive. Initially, it may only occur during physical exertion, but as the disease advances, it becomes noticeable even with minimal activity or at rest. Patients often report feeling "air hungry."
- Chronic Cough: While more characteristic of chronic bronchitis, a persistent cough, which may or may not be productive of sputum, can also be present in emphysema, particularly if bronchitis coexists.
- Wheezing: A whistling sound during breathing, caused by narrowed airways.
- Frequent Lung Infections: Due to impaired mucociliary clearance and damaged lung tissue, individuals with emphysema are more susceptible to recurrent respiratory infections (e.g., bronchitis, pneumonia).
- Weight Loss: Significant weight loss can occur due to the increased energy expenditure associated with the constant work of breathing, reduced appetite, and systemic inflammation.
- Fatigue: Chronic dyspnea, increased work of breathing, hypoxemia, and sleep disturbances contribute to profound fatigue.
- Cyanosis: Bluish discoloration of the skin, lips, or nail beds, indicating insufficient oxygen in the blood. This is a sign of advanced disease.
- Anxiety and Depression: The chronic, debilitating nature of the disease, coupled with the constant struggle for breath and fear of suffocation, often leads to significant psychological distress.
- Sleep Problems: Dyspnea, coughing, and hypoxemia can disrupt sleep patterns, leading to insomnia or frequent awakenings.
- Morning Headaches: Can be a sign of hypercapnia (high carbon dioxide levels) during sleep due to hypoventilation.
- Barrel Chest: Due to chronic air trapping and hyperinflation, the chest wall may expand, giving it a rounded, barrel-like appearance.
- Pursed-Lip Breathing: A compensatory breathing technique used to create back pressure in the airways, helping to keep them open during exhalation and reduce air trapping.
- Use of Accessory Muscles of Respiration: As the diaphragm's efficiency decreases, patients may rely on neck and shoulder muscles (e.g., sternocleidomastoid, scalenes) to assist with breathing.
Management of a Patient with Emphysema
The management of emphysema is focused on relieving symptoms, slowing disease progression, preventing and treating complications, and improving the patient's quality of life. As emphysema is irreversible, the goal is not a cure but effective disease management.
Aims of Management
- To optimize respiratory function and restore the best possible breathing pattern.
- To prevent or minimize the frequency and severity of acute exacerbations.
- To alleviate symptoms such as dyspnea and cough.
- To improve exercise tolerance and overall physical functioning.
- To prevent and manage complications, including infections and heart problems.
- To enhance the patient's quality of life and reduce anxiety/depression associated with the disease.
- To provide education and support for self-management.
General Management and Nursing Interventions
A multi-faceted approach involving medical, nursing, and rehabilitative interventions is crucial.
1. Assessment and Monitoring:
- Admission of the patient to a medical ward, ideally quiet and well-ventilated, to promote rest and reduce environmental irritants.
- Thorough initial assessment of respiratory status: rate, rhythm, depth, use of accessory muscles, breath sounds (e.g., diminished, wheezes, rhonchi), and oxygen saturation (SpO2).
- Regular monitoring of vital observations: temperature, pulse, respiration, and blood pressure. These must be meticulously recorded on the patient's file and trended to identify changes or signs of deterioration (e.g., fever indicating infection, increased respiratory rate, tachycardia).
- Assess for signs of hypoxemia (cyanosis, confusion) and hypercapnia (morning headaches, somnolence, confusion).
- Monitor fluid balance, especially if there is increased insensible loss from tachypnea or if diuretics are used for cor pulmonale.
- Assess nutritional status and provide dietary support if needed.
2. Positioning and Comfort:
- Position the patient in a sitting-up position (e.g., High Fowler's, orthopneic position) to maximize lung expansion and aid breathing by reducing pressure on the diaphragm.
- Provide emotional support and reassurance to allay anxiety, which can worsen dyspnea. Teach relaxation techniques.
3. Oxygen Therapy:
- Administration of supplemental oxygen therapy as prescribed, guided by SpO2 levels and arterial blood gases (ABGs). The goal is to maintain adequate oxygenation (e.g., SpO2 > 90%) while carefully monitoring for CO2 retention, especially in advanced stages (start with low flow rates, e.g., 1-2 L/min, and titrate based on patient response and ABGs). Oxygen therapy helps improve oxygen delivery to the lungs and tissues.
4. Pharmacological Management (Drug Therapy):
- Bronchodilators: These medications relax the smooth muscles of the airways, helping to open them up and reduce bronchospasm. They are typically given via inhalers (nebulizers or metered-dose inhalers with spacers).
- Short-acting beta-agonists (SABAs) e.g., Albuterol (Salbutamol): For quick relief of acute dyspnea.
- Long-acting beta-agonists (LABAs) e.g., Salmeterol, Formoterol: For long-term maintenance.
- Short-acting anticholinergics e.g., Ipratropium: For quick relief.
- Long-acting anticholinergics (LAMAs) e.g., Tiotropium: For long-term maintenance.
- Methylxanthines e.g., Theophylline: Less commonly used due to side effects and narrow therapeutic window, but may be used in some cases.
- Corticosteroids:
- Inhaled Corticosteroids (ICS): Often used in combination with LABAs for patients with frequent exacerbations or significant symptoms, particularly if they have an "asthma-like" component. E.g., Fluticasone, Budesonide.
- Oral Corticosteroids: Used for acute exacerbations to reduce inflammation and improve airflow. E.g., Prednisone. Long-term use is generally avoided due to significant side effects.
- Antibiotics: Prescribed for acute exacerbations if there is evidence of bacterial infection (e.g., increased sputum purulence, fever).
- Diuretics: May be used if the patient develops cor pulmonale with peripheral edema.
- Mucolytics: (e.g., acetylcysteine) May be considered in some patients with very thick, tenacious sputum, although their routine use is debated.
- Alpha-1 Antitrypsin Augmentation Therapy: For patients with documented severe AAT deficiency, intravenous infusion of pooled human alpha-1 antitrypsin can help slow the progression of emphysema.
5. Pulmonary Rehabilitation:
- A comprehensive program that includes exercise training, nutritional counseling, education on lung disease, and psychological support. This significantly improves exercise tolerance, reduces symptoms, and enhances quality of life.
- Physical exercises: Encouraged within the patient's tolerance, such as walking, cycling (stationary bikes). These help the body use oxygen more efficiently, improve muscle strength, and reduce breathlessness.
- Breathing Techniques: Teaching pursed-lip breathing and diaphragmatic breathing can help control dyspnea and improve exhalation.
6. Nutritional Support:
- Patients with advanced emphysema often have increased caloric needs due to the work of breathing but may experience reduced appetite. Nutritional counseling and calorie-dense, small, frequent meals can help prevent weight loss and maintain muscle mass.
7. Surgical Interventions (for select cases):
- Lung Volume Reduction Surgery (LVRS): In highly selected patients with upper lobe emphysema and low exercise capacity, surgical removal of the most diseased parts of the lung can reduce hyperinflation and improve lung function.
- Bullectomy: Surgical removal of large bullae that are not contributing to gas exchange and are compressing healthy lung tissue.
- Lung Transplantation: A last-resort option for very severe emphysema in carefully selected candidates.
Health Education on Emphysema
Comprehensive health education is fundamental to empowering patients to manage their condition effectively, prevent complications, and maintain the best possible quality of life.
- Smoking Cessation: This is the single most important intervention. Emphasize that quitting cigarette smoking (and avoiding all other tobacco products) is crucial to slow the progression of the disease and prevent further lung damage. Provide resources for smoking cessation programs, nicotine replacement therapy, or medications.
- Vaccination: Highly recommended to prevent respiratory infections that can trigger acute exacerbations.
- Annual influenza (flu) immunization.
- Pneumococcal vaccination: Typically, a series of two vaccinations (PCV13 and PPSV23) for adults with chronic lung disease, with specific intervals. (Note: "5 yearly one against pneumonia" is a simplified guideline, and current recommendations for pneumococcal vaccines should be followed).
- COVID-19 vaccination and boosters.
- Pertussis (whooping cough) vaccine.
- Nutritional Guidance: A healthful diet with plenty of fresh fruits, vegetables, whole grains, lean proteins, and a low intake of processed foods, unhealthy fats, and added sugars is necessary. Advise on strategies to manage appetite and maintain weight, such as smaller, more frequent meals.
- Physical Activity and Exercise: Encourage regular, gentle physical exercises within the patient's tolerance (e.g., walking, using stationary bikes, light resistance training). Explain that these help the body use oxygen more efficiently, improve muscle strength, and hence improve breathing and overall well-being. Emphasize the importance of pulmonary rehabilitation.
- Breathing Techniques: Teach and reinforce effective breathing techniques such as pursed-lip breathing (to control breathlessness and prevent airway collapse) and diaphragmatic (abdominal) breathing (to maximize diaphragm efficiency).
- Medication Adherence: Educate on the purpose, correct administration (especially for inhalers), dosage, and potential side effects of all prescribed medications. Emphasize the importance of consistent use of maintenance medications.
- Symptom Recognition and Action Plan: Teach patients to recognize early signs of worsening symptoms or acute exacerbations (e.g., increased dyspnea, increased cough, change in sputum color/volume, fever) and provide a clear action plan on when to contact their healthcare provider or seek emergency care.
- Avoidance of Irritants: Advise avoiding exposure to environmental lung irritants such as secondhand smoke, air pollution, chemical fumes, and strong odors.
- Infection Control: Practice good hand hygiene, avoid crowds during flu season, and manage underlying conditions that increase infection risk.
- Psychological Support: Address anxiety and depression. Encourage open communication, support groups, and professional counseling if needed.
- Follow-up Care: Emphasize that regular follow-up visits with healthcare providers are crucial for ongoing assessment, adjustment of treatment plans, and early detection of complications.
- Energy Conservation Techniques: Advise on strategies to conserve energy and manage daily activities, such as pacing oneself, taking breaks, and using assistive devices if necessary.
Complications of Emphysema
The complications of emphysema range from direct respiratory issues to systemic effects, often progressing in severity as the disease advances.
- Acute Exacerbations of COPD (AECOPD): Emphysema patients are highly susceptible to acute worsening of their symptoms, often triggered by respiratory infections (viral or bacterial) or increased exposure to irritants. These exacerbations can be severe, requiring hospitalization and significantly impacting lung function and quality of life.
- Pneumonia: Due to impaired lung defenses and altered lung architecture, individuals with emphysema are at increased risk of developing bacterial or viral pneumonia, which can be life-threatening.
- Pneumothorax (Collapsed Lung): The destruction of alveolar walls can lead to the formation of large air-filled sacs (bullae). These bullae can sometimes rupture, allowing air to escape into the space between the lung and the chest wall (pleural space), leading to a collapsed lung (spontaneous pneumothorax). This is a medical emergency.
- Bullae: While bullae themselves are part of the emphysematous process, very large bullae can compress healthy lung tissue, further impairing function. They also carry the risk of rupture.
- Pulmonary Hypertension: The chronic hypoxemia (low blood oxygen) in emphysema causes the blood vessels in the lungs to constrict (pulmonary vasoconstriction). This leads to increased pressure in the arteries of the lungs, a condition known as pulmonary hypertension.
- Cor Pulmonale (Right-Sided Heart Failure): Persistent pulmonary hypertension places increased strain on the right side of the heart, which is responsible for pumping blood to the lungs. Over time, this increased workload can cause the right ventricle to enlarge and weaken, leading to right-sided heart failure (cor pulmonale). Symptoms include swelling in the ankles and legs (peripheral edema), jugular venous distension, and liver enlargement.
- Respiratory Failure: In advanced stages or during severe exacerbations, the lungs' ability to adequately oxygenate the blood and remove carbon dioxide becomes severely compromised, leading to acute or chronic respiratory failure. This may necessitate mechanical ventilation or long-term oxygen therapy.
- Polycythemia: Chronic hypoxemia can stimulate the bone marrow to produce more red blood cells (erythrocytosis or polycythemia) as the body attempts to compensate for low oxygen levels. This increases the viscosity (thickness) of the blood, raising the risk of blood clots (e.g., deep vein thrombosis, pulmonary embolism).
- Weight Loss and Malnutrition: The increased metabolic demands from the work of breathing, reduced appetite, and systemic inflammation often lead to unintentional weight loss and muscle wasting.
- Osteoporosis: Patients with emphysema are at higher risk of developing osteoporosis due to chronic inflammation, corticosteroid use, and reduced physical activity.
- Muscle Weakness and Dysfunction: Systemic inflammation and deconditioning contribute to weakness and atrophy of skeletal muscles, further impacting exercise capacity and quality of life.
- Depression and Anxiety: The chronic and debilitating nature of emphysema significantly impacts mental health, often leading to depression and anxiety.

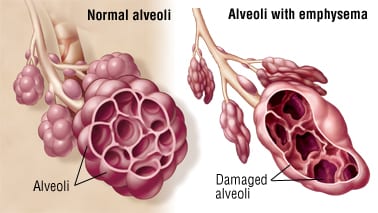
this is really educative