Learning Outcomes
By the end of this section, the learner shall be able to:
- Explain the major physiological changes a newborn undergoes at birth.
- Describe the transition from fetal to pulmonary respiration.
- Detail the changes in the cardiovascular system, including the closure of fetal shunts.
- Discuss the immaturities of the newborn's digestive, hepatic, and renal systems.
- Explain the mechanism of temperature regulation in a neonate.
- Describe the status of the newborn's immune and haematopoietic systems at birth.
Introduction to Newborn Physiology
The moment of birth marks the most dramatic physiological transition in a person's life. The newborn must rapidly adapt from a dependent, fluid-filled intrauterine environment, where the placenta performed all vital functions, to an independent, air-breathing existence. This transition involves profound and immediate changes in nearly every organ system, most critically the respiratory and cardiovascular systems.
Changes in the Newborn at Birth
Changes in the newborn at birth are a number of changes that an infant’s body undergoes to allow it to survive outside the womb and adapt to life in a new environment.
During intrauterine life, the fetus receives oxygen and nutrients by absorption through the placenta. It does not use its lungs or the digestive organs. Similarly, it excretes carbon dioxide and other waste products through placental structures into the mother’s blood.
It is protected from many harmful factors/organisms by the placenta, and it is kept in a warm environment.
Size and Growth:
- The term infant weighs about 3000g. Boys weigh approximately 250g more than girls.
- Infants of less than 2500g are classified as ‘low birth.’
- During the first 3–5 days, up to 10% of birth weight is lost. This is regained by 7–10 days.
- In the first month, average weight gain per week is 200g.
Skin:
- The newborn skin is immature, with a thin epithelial layer and incompletely developed sweat and sebaceous glands.
- Combined with the high surface area to body mass ratio, this renders the baby prone to heat and water losses.
- Numerous benign skin lesions occur, e.g. a greasy protective layer, the vernix caseosa.
Temperature Regulation:
- The neonate has a low metabolic activity resulting in a poor ability to produce heat.
- The infant enters a much cooler environment than to which it is used. Its body is wet and thus liable to lose heat through evaporation.
- Receptors on the baby’s skin send messages to the brain that the baby’s body is cold.
- The baby’s body then creates heat by shivering and by burning stores of brown fat, a type of fat found only in fetuses and newborns.
Head:
- The average occipito-frontal head circumference is 35 cm.
- Two soft spots or fontanels are present.
- The anterior fontanel closes at 18 months of age, and the posterior closes by 6–8 weeks.
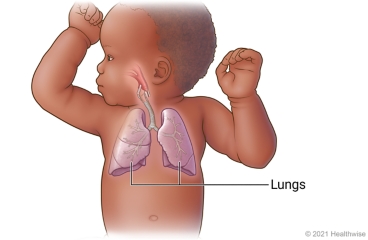
Respiratory System:
The initiation of respiration is the most crucial event in the newborn's adaptation. In the womb, the lungs are filled with fluid and are not used for gas exchange.
- Changes that occur at birth allow the newborn to convert from dependence on the placenta to breathing air for the exchange of respiratory gases.
- In utero, the airways and lungs are filled with fluid that contains surfactant.
- The lung fluid is removed by the squeezing of the thorax during vaginal delivery and by reduced secretion and increased absorption mediated by fetal catecholamine during labor and after birth.
- Surfactant lines the air–fluid interface of the alveoli and reduces the surface tension, thereby facilitating lung expansion. This is associated with a fall in pulmonary vascular resistance.
- The rate is variable and normally ranges between 30 and 60 breaths/min. Brief self-limiting apnoeic spells might occur during sleep.
Factors That Stimulate the First Breath
The first breath is not a single event but a response to a combination of powerful stimuli:
- Chemical Stimuli: During labor, placental blood flow is temporarily reduced, causing a slight decrease in oxygen (hypoxia) and an increase in carbon dioxide (hypercapnia) in the baby's blood. This change in blood chemistry directly stimulates the respiratory center in the brain.
- Mechanical Stimuli: The passage through the birth canal squeezes the baby's chest (thoracic squeeze), forcing approximately one-third of the fluid out of the lungs. As the chest recoils after birth, air is drawn in for the first time. Crying also helps to expand the lungs.
- Thermal Stimuli: The sudden change from the warm intrauterine environment (approx. 37°C) to the cooler delivery room stimulates sensory receptors in the skin, which in turn stimulate the respiratory center.
- Sensory Stimuli: The new experiences of being touched, dried, and exposed to light and sound all provide stimulation that encourages breathing.
Normal Breathing Patterns
A newborn's respiratory rate is 30-60 breaths per minute. Their breathing is often irregular, with short pauses of 5-15 seconds (periodic breathing), which is normal. They are also obligatory nose breathers and use their abdominal muscles to breathe.
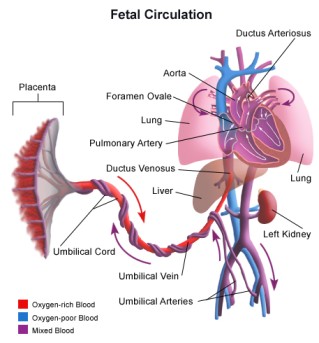
Cardiovascular System
With the first breath and the clamping of the umbilical cord, the entire circulatory system must reroute itself. Fetal circulation, which bypasses the lungs, must switch to newborn circulation, where blood is sent to the lungs for oxygenation.
- Major changes in the lungs and circulation allow adaptation to extra-uterine life.
- In the fetal circulation, the right-sided (pulmonary) pressure exceeds the left-sided (systemic) pressure. Blood flows from right to left through the foramen ovale and ductus arteriosus.
- At birth, these relationships reverse: Left-sided (systemic) pressure rises with clamping of umbilical vessels. Right-sided (pulmonary) pressure falls as the lungs expand, and the rising pressure triggers a prostaglandin-mediated vasodilatation.
- The foramen ovale and ductus arteriosus close functionally shortly after birth. The ductus closes due to muscular contraction in response to rising oxygen tension.
Closure of Fetal Shunts
This rerouting is accomplished by the closure of three fetal shunts:
- Foramen Ovale: A flap-like opening between the right and left atria. Increased blood flow from the newly functioning lungs raises the pressure in the left atrium, pushing this flap closed.
- Ductus Arteriosus: A blood vessel connecting the pulmonary artery to the aorta, which shunted blood away from the fetal lungs. It constricts and closes in response to higher oxygen levels in the blood and other hormonal changes.
- Ductus Venosus: A vessel that shunted oxygenated blood from the placenta away from the liver and directly to the heart. When the umbilical cord is clamped, blood flow ceases, and this shunt closes.
A newborn's heart rate is typically 110-160 beats per minute and can fluctuate with activity and sleep.
Thermoregulation
Newborns are at a high risk for heat loss (hypothermia) due to several factors: a large body surface area to mass ratio, thin skin with less subcutaneous fat, and an inability to shiver effectively.
How Newborns Lose Heat
- Evaporation: Loss of heat as amniotic fluid dries from the skin after birth. (Action: Dry the baby thoroughly).
- Conduction: Loss of heat through direct contact with a cooler surface, like a cold scale or stethoscope. (Action: Place the baby on warm surfaces; use skin-to-skin contact).
- Convection: Loss of heat to cooler air currents, like drafts from windows or air conditioners. (Action: Keep the baby wrapped and away from drafts).
- Radiation: Loss of heat to a nearby cooler object without direct contact, like a cold windowpane. (Action: Keep cribs away from cold outer walls).
How Newborns Produce Heat
The primary method of heat production in newborns is non-shivering thermogenesis. This is the metabolism of a special type of fat called brown adipose tissue (BAT), or "brown fat," which is uniquely located around the newborn's neck, back, and major organs. Burning this fat produces heat and warms the blood passing through it.
Haematopoietic and Immune Systems
Haematopoietic System (Blood)
- Hemoglobin: Newborns have a high concentration of red blood cells and hemoglobin, specifically fetal hemoglobin (HbF), which is very efficient at carrying oxygen.
- Physiological Jaundice: After birth, the excess red blood cells are broken down. This process releases bilirubin. The newborn's immature liver cannot process this bilirubin quickly, causing it to build up in the blood and lead to a temporary yellowing of the skin and eyes (physiological jaundice), typically appearing on the 2nd or 3rd day of life.
- Vitamin K: The newborn's gut is sterile and cannot yet produce Vitamin K, which is essential for blood clotting. To prevent hemorrhagic disease of the newborn, all babies are given a prophylactic injection of Vitamin K at birth.
Immune System
The newborn's immune system is immature and inexperienced, making them vulnerable to infections. They receive temporary protection through passive immunity:
- IgG: These antibodies cross the placenta from the mother during the third trimester, providing protection against diseases to which the mother is immune.
- IgA: These antibodies are found in high concentrations in colostrum and breast milk, providing protection to the gastrointestinal and respiratory tracts.
- The neonatal immune system is incomplete compared to older children and adults:
- Impaired neutrophil reserves.
- Diminished phagocytosis and intracellular killing capacity.
- Decreased complement components.
- Low IgG2, leading to infections with organisms.
- The presence of maternal antibody in babies born greater than 30 weeks’ gestational age provides some protection against infection.
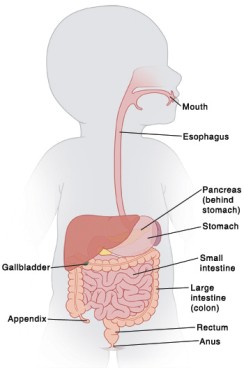
Gastrointestinal and Renal Systems
- At term, the secretory and absorbing surfaces are well developed, as are digestive enzymes, with the exception of pancreatic amylase.
- Meconium is usually passed within 6 hrs, and delay beyond 24 hrs is considered abnormal.
- Normally, meconium is replaced by yellow stool by day 3-4.
Gastrointestinal (Digestive) System
- Meconium: The first stool, passed within 24-48 hours. It is sticky, thick, dark green/black, and odorless.
- Transitional Stool: Appears by day 3-4. It is thin, slimy, and greenish-brown to yellowish-brown.
- Milk Stool: By day 4-5. If breastfed, the stool is loose, seedy, and mustard-yellow. If formula-fed, it is paler, firmer, and has a more noticeable odor.
Liver:
- In the fetus, the liver acts as a storage site for sugar (glycogen) and iron.
- When the baby is born, the liver has various functions: It produces substances that help the blood to clot. It begins breaking down waste products such as excess red blood cells. It produces a protein that helps break down bilirubin.
- Immaturity of the liver enzymes responsible for conjugation of bilirubin is responsible for the ‘physiological jaundice’ which can occur from the second day of life.
Genitourinary System:
- The infant should void within the first 24 hours of life.
The kidneys are able to produce urine, but their ability to concentrate it is limited. This makes newborns susceptible to dehydration if fluid intake is insufficient. A newborn should pass their first urine within 24 hours of birth, though it can take up to 48 hours.
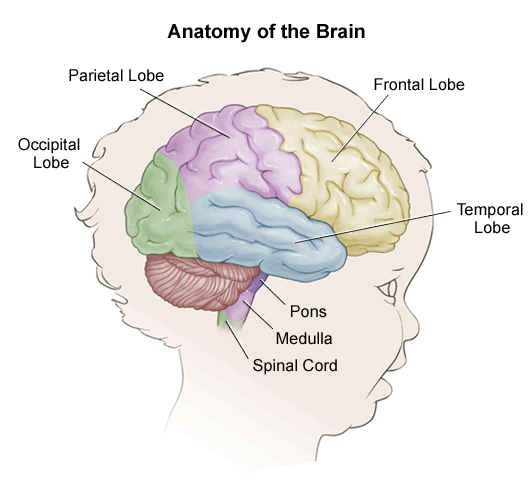
Central Nervous System:
- The central nervous system (CNS) is relatively immature at birth.
- Newborn infants sleep for a total of 16–20 hours each day.
- The touch of a nipple on the baby’s face initiates the sequence of rooting and the complex coordination of lip, tongue, palate, and pharynx required for sucking and swallowing.
- Crying (without tears) is the main means of communication.
Revision Questions
- What are the four main stimuli that trigger the first breath in a newborn?
- Explain the function of the ductus arteriosus in the fetus and describe what causes it to close after birth.
- A newborn is placed on a cold weighing scale. Which mechanism of heat loss is this, and what is one nursing action to prevent it?
- What is physiological jaundice, and what two factors in the newborn's liver and blood system contribute to its development?
- Describe the normal progression of a newborn's stools, from meconium to milk stool. Why do these changes occur?
- Why is Vitamin K administered to all newborns at birth?

