SECTION A: Objective Questions (20 marks)
💡 Exam Strategy: Read each question carefully! Pay special attention to "NOT" and "exclude" questions. Use the process of elimination to narrow down your choices.
1 Which of the following biological factors predisposes to suicide?
a) Genetics and decreased levels of serotonin
b) Heredity and increased levels of nor-epinephrine
c) Structural alterations of the brain
d) Temporal lobe atrophy
(a) Genetics and decreased levels of serotonin
Research strongly suggests a link between neurobiology and suicidal behavior. Decreased levels of serotonin (5-HT), a neurotransmitter involved in mood regulation, impulse control, and aggression, have been consistently found in individuals who have died by suicide or attempted suicide. Studies often show lower concentrations of serotonin metabolites (like 5-HIAA) in the cerebrospinal fluid (CSF) of suicidal individuals. Furthermore, genetics play a role; family history of suicide is a known risk factor, suggesting a heritable component to this predisposition, which may involve genes related to serotonin function or other neurobiological pathways.
(b) Heredity and increased levels of nor-epinephrine: While heredity (genetics) is a factor, increased levels of norepinephrine are more commonly associated with anxiety, stress responses, and mania, rather than being a primary predisposing factor for suicide directly. Some studies suggest dysregulation of the noradrenegic system in depression, but the link to suicide is less direct and consistent than that of serotonin.
(c) Structural alterations of the brain: While certain mental illnesses associated with suicide risk (like depression or schizophrenia) can involve structural brain alterations, this option is too general. Specific alterations in areas like the prefrontal cortex or hippocampus have been noted in some studies of suicidal individuals, often related to mood disorders, but "structural alterations" alone isn't as precise as the serotonin link.
(d) Temporal lobe atrophy: Temporal lobe atrophy is more characteristic of conditions like Alzheimer's disease or certain types of dementia or epilepsy. While individuals with these conditions might experience depression or hopelessness that increases suicide risk, temporal lobe atrophy itself is not a primary or direct biological factor predisposing to suicide across the broader population at risk.
SUICIDE RISK FACTORS: "SAD HOPELESS" - Substance abuse, Age (elderly/adolescent), Depression, Hopelessness, Previous attempt, Occupation (access to means), Psychosis, Ethnicity, Sex (male), Social isolation, Stress
2 Priorities for nurses caring for patients with suicidal ideations exclude
a) Ruling out substance abuse
b) Establishing a therapeutic relationship
c) Implementing safety measures immediately
d) Providing education and support
(a) Ruling out substance abuse
While assessing for and addressing substance abuse is a very important part of comprehensive care for a patient with suicidal ideations (as substance abuse is a major risk factor), it is not the immediate priority compared to the other options. The question asks what is "excluded" from priorities. The other three options are all core, immediate priorities in the acute management of suicidal patients.
(b) Establishing a therapeutic relationship: This is a fundamental and immediate priority. A trusting relationship is essential for effective assessment, communication of distress by the patient, and their willingness to engage in safety planning and treatment.
(c) Implementing safety measures immediately: This is the absolute top priority. Actions include ensuring a safe environment (removing potential ligatures, sharp objects, medications), one-to-one observation if indicated, and constant reassessment of risk.
(d) Providing education and support: This is a crucial ongoing priority. Education may involve understanding their feelings, coping mechanisms, available resources, and safety plans. Support involves empathy, validation, and fostering hope.
🚨 IMMEDIATE PRIORITIES IN SUICIDAL PATIENTS: Safety → Relationship → Assessment → Intervention. Substance abuse assessment is part of comprehensive assessment but not the immediate priority.
3 An appropriate expected outcome for a patient being nursed with schizophrenia is client will
a) Spend 2 hours session sharing environmental observations with the nurse
b) Listen attentively and communicate clearly in 48 hours
c) Maintain reality based thoughts in 24 hours
d) Develop trust in at least 1 staff within 7 days of admission
(d) Develop trust in at least 1 staff within 7 days of admission
Developing trust is a foundational step in the care of a patient with schizophrenia, especially given that symptoms like paranoia and suspiciousness can make forming relationships difficult. An expected outcome that is realistic, measurable, and patient-centered would be for the client to develop trust in at least one staff member within a reasonable timeframe (e.g., 7 days of admission). This trust is essential for engagement in therapy, medication adherence, and overall treatment progress.
(a) Spend 2 hours session sharing environmental observations: While interacting with the nurse is positive, a 2-hour session focused on environmental observations might not be the most therapeutic or realistic initial outcome. It's also very specific and lengthy. The focus should be on building rapport and addressing core symptoms or needs.
(b) Listen attentively and communicate clearly in 48 hours: While improved communication is a desirable long-term goal, expecting a patient with schizophrenia (who may have thought disorder, alogia, or negative symptoms affecting communication) to achieve this within 48 hours is unrealistic, especially during an acute phase.
(c) Maintain reality based thoughts in 24 hours: Schizophrenia is characterized by disturbances in thought processes, including delusions and hallucinations. Expecting a patient to maintain "reality-based thoughts" completely within 24 hours of admission is highly unrealistic. Reduction in psychotic symptoms and improved reality testing is a longer-term goal achieved through medication and therapy.
⏰ SMART Goals: Specific, Measurable, Achievable, Relevant, Time-bound. Trust-building is a realistic early goal in schizophrenia care.
4 Which of the following points to a good prognosis for schizophrenia?
a) Gradual onset
b) Good social network
c) Early onset
d) Absence of passivity phenomenon
(b) Good social network
A good social network (strong family support, friendships, community connections) is consistently associated with a better prognosis in schizophrenia. Social support can help with treatment adherence, reduce stress, provide practical assistance, improve coping skills, and reduce social isolation, all of which contribute to better outcomes, including fewer relapses and improved quality of life.
(a) Gradual onset: A gradual, insidious onset of schizophrenia is generally associated with a poorer prognosis compared to an acute or sudden onset. Gradual onset often means a longer period of untreated psychosis and more prominent negative symptoms, which are harder to treat.
(c) Early onset: Early onset of schizophrenia (e.g., in childhood or early adolescence) is typically associated with a poorer prognosis, including more severe symptoms, greater cognitive impairment, and a more chronic course. Later onset (e.g., late 20s or 30s) often has a better prognosis.
(d) Absence of passivity phenomenon: Passivity phenomena (e.g., thought insertion, withdrawal, broadcast; delusions of control) are specific types of psychotic symptoms. While the presence of severe positive symptoms can indicate an acute phase, their specific absence isn't as strong a prognostic indicator as factors like good premorbid functioning, acute onset, good social support, or predominantly positive (as opposed to negative) symptoms.
GOOD PROGNOSIS FACTORS: "SAVE" - Sudden onset, Acute presentation, good Vocational history, good support network, Early treatment, no family history
5 Families support binge eating amidst their children when they
a) Practice mindful eating
b) Identify triggers to this habit
c) Become active in exercises as a family
d) Encourage the children to skip meals
(d) Encourage the children to skip meals
Encouraging children to skip meals is a practice that can inadvertently support or trigger binge eating. When meals are skipped, especially breakfast or lunch, it can lead to extreme hunger later in the day. This intense hunger can make it difficult to control eating behaviors, potentially leading to overeating or bingeing when food does become available. Restrictive eating patterns, including meal skipping, are known risk factors for the development and maintenance of binge eating disorder.
(a) Practice mindful eating: Practicing mindful eating (paying attention to hunger and fullness cues, savoring food, eating without distractions) is a strategy that helps to prevent or manage binge eating, not support it. It encourages a healthier relationship with food.
(b) Identify triggers to this habit: Helping children identify triggers for binge eating (e.g., stress, boredom, certain emotions, specific situations) is a constructive step in addressing and managing the behavior. This awareness is part of therapeutic interventions.
(c) Become active in exercises as a family: Engaging in regular physical activity as a family promotes overall health, can improve mood, and can be a positive coping mechanism. It is generally seen as beneficial and does not support binge eating; in fact, it can be part of a healthy lifestyle that counteracts disordered eating.
🍽️ BINGE EATING CYCLE: Restriction → Hunger → Binge → Guilt → Restriction. Breaking the cycle requires regular, balanced meals, not meal skipping.
6 Which of the following is the most common cause of childhood epilepsy?
a) Genetics
b) Alcohol in pregnancy
c) Birth injuries
d) Infections
(a) Genetics
While the causes of childhood epilepsy are diverse and often unknown (idiopathic), genetics play a significant role and are considered a very common underlying factor for many types of childhood epilepsy. Many specific epilepsy syndromes in children have a known or suspected genetic basis, involving mutations in single genes or complex polygenic inheritance. Some genetic epilepsies are benign and resolve with age, while others are more severe and persistent.
(b) Alcohol in pregnancy: Maternal alcohol consumption during pregnancy can lead to Fetal Alcohol Spectrum Disorders (FASD), which can include neurological problems and an increased risk of seizures. However, it is not considered the most common cause of childhood epilepsy overall compared to genetic factors.
(c) Birth injuries: Birth injuries, such as hypoxic-ischemic encephalopathy (brain damage due to lack of oxygen or blood flow during birth), can lead to epilepsy. These are significant causes, but genetic predispositions account for a larger proportion of cases when all childhood epilepsies are considered.
(d) Infections: CNS infections, such as meningitis or encephalitis, can cause seizures and lead to epilepsy as a long-term sequela due to brain scarring. Infections are a major cause of epilepsy worldwide, especially in resource-limited settings, but again, "genetics" as a broad category encompassing many syndromes is often cited as most common overall.
🧬 GENETIC EPILEPSIES: Many childhood epilepsy syndromes like Dravet syndrome, West syndrome, and Lennox-Gastaut syndrome have strong genetic components. Genetic testing is increasingly available.
7 The initial nursing intervention for a patient who is aggressive and violent is to
a) Tactfully escape
b) Call for help
c) Restrain the patient
d) Seclude the patient
(b) Call for help
When a patient becomes aggressive and violent, the nurse's immediate safety and the safety of others are paramount. The initial nursing intervention should be to call for help. Attempting to manage a violent patient alone can put the nurse and the patient at increased risk of injury. Calling for help ensures that adequate staff (e.g., other nurses, security personnel, medical staff) are available to manage the situation safely and effectively, using de-escalation techniques or, if necessary, physical restraint or seclusion according to established protocols.
(a) Tactfully escape: While ensuring one's own safety is crucial, and removing oneself from immediate danger if alone and overwhelmed is important, simply escaping without summoning assistance does not address the patient's behavior or the safety of others who may be present or unaware. "Calling for help" is a more comprehensive initial action.
(c) Restrain the patient: Attempting to restrain a violent patient single-handedly is dangerous and generally contraindicated. Physical restraint should only be implemented by a trained team with sufficient numbers to ensure safety for both the patient and staff, and only as a last resort when de-escalation has failed.
(d) Seclude the patient: Seclusion, like restraint, is a restrictive intervention used as a last resort when less restrictive measures are ineffective and the patient poses an ongoing danger to self or others. It requires a team approach and is not the initial action a nurse takes immediately upon encountering aggression.
AGGRESSION RESPONSE: "CALL" - Call for help, Assess situation, Limit danger, Leave if unsafe alone
8 Which of the following approaches is most effective for controlling alcohol abuse in Uganda?
a) Reviewing and implementation of policies
b) Intensifying health education talks
c) Hiking alcohol prices
d) Regulating drinking hours
(a) Reviewing and implementation of policies
While all listed approaches can contribute, a comprehensive strategy involving the reviewing and implementation of policies is generally considered the most effective framework. Effective policies can encompass and enforce many specific measures: taxation/pricing, availability regulation, marketing restrictions, drink-driving countermeasures, and support for treatment/prevention. A multi-pronged approach guided by strong, well-enforced national and local alcohol control policies has the broadest and most sustainable impact. The WHO Global Strategy to Reduce the Harmful Use of Alcohol emphasizes comprehensive policies.
(b) Intensifying health education talks: Health education is important for raising awareness, but on its own, it often has limited impact on changing widespread substance abuse behaviors without being part of a broader strategy that includes policy and environmental changes.
(c) Hiking alcohol prices: Increasing alcohol prices through taxation is recognized as one of the most effective individual measures (a "best buy" intervention according to WHO). However, this is usually implemented as part of a broader policy framework, not as a standalone approach.
(d) Regulating drinking hours: Restricting the hours during which alcohol can be sold is another specific policy measure that can help reduce alcohol-related harm. Again, this is a component that would fall under a comprehensive policy approach.
🌍 WHO BEST BUYS: 1) Increase alcohol prices, 2) Restrict availability, 3) Enforce drink-driving laws, 4) Ban alcohol advertising. All require strong policy implementation.
9 Which of the following orders facilitates quick removal of a mentally ill patient from the community to the hospital?
a) Temporary detention order
b) Order of commitment on detention
c) Urgency order
d) Warrant order
(c) Urgency order
In the context of mental health legislation in many jurisdictions, including Uganda's Mental Health Act, an Urgency Order is specifically designed for situations where a person is believed to be mentally ill and is behaving in a manner that indicates they are a danger to themselves or others, requiring immediate apprehension and removal to a hospital or mental health unit for assessment and treatment. This order allows for swift action when the delay in obtaining other types of orders could pose a significant risk. It's an emergency measure.
(a) Temporary detention order: While this also involves detention, an "Urgency Order" is typically the specific legal instrument for immediate, emergency removal. A temporary detention order might be part of the process following an urgency order, allowing for a short period of assessment.
(b) Order of commitment on detention: This sounds more like a formal, longer-term commitment order made by a court or tribunal after a period of assessment. It's not typically the order for quick initial removal from the community in an emergency.
(d) Warrant order: A warrant is a general legal document authorizing police to make an arrest or search. While a warrant might be used in some circumstances, an "Urgency Order" under mental health law is more specific for the immediate needs of a mentally ill person posing a danger.
⚡ URGENCY ORDER: Allows for immediate action without court delay. Must be followed by proper assessment and formal admission procedures within specified timeframes (e.g., 72 hours).
10 Which of the following types of hallucinations is characteristic of schizophrenia?
a) Single person
b) Gustatory
c) Third party
d) Tactile
(c) Third party
Auditory hallucinations are the most common type in schizophrenia. Among these, third-person hallucinations ("Third party") are particularly characteristic. This involves voices talking about the patient in the third person (e.g., "He is a bad person," "She is going to fail"). Other characteristic auditory hallucinations include voices commenting on the patient's actions (running commentary), thought echo (hearing one's own thoughts spoken aloud), and voices arguing or discussing the patient. These are considered Schneiderian first-rank symptoms, highly suggestive of schizophrenia.
(a) Single person: This is too vague. Auditory hallucinations can involve one voice or multiple voices. If it refers to hearing a familiar single person, that's possible in many conditions. The content and nature of the hallucination (like third-person commentary) are more characteristic than just the number of perceived speakers.
(b) Gustatory: These are hallucinations of taste. While they can occur in schizophrenia, they are less common than auditory hallucinations and can also be seen in medical or neurological disorders, not as specifically characteristic as certain types of auditory hallucinations.
(d) Tactile: These are hallucinations of touch (e.g., feeling insects crawling). Tactile hallucinations can occur in schizophrenia but are also commonly associated with substance withdrawal (e.g., alcohol or cocaine withdrawal), delirium, or neurological conditions. They are not as classic for schizophrenia as third-party auditory hallucinations.
FIRST-RANK SYMPTOMS: "VAN" - Voices commenting, Audible thoughts, Thought broadcasting, Voices arguing, Thought insertion/withdrawal
11 Which of the following is NOT an anxiety disorder?
a) Generalised anxiety
b) Panic disorder
c) Agora phobia
d) Conversion state
(d) Conversion state
Conversion state (also known as Conversion Disorder or Functional Neurological Symptom Disorder in DSM-5) is classified as a Somatic Symptom and Related Disorder (or previously as a Somatoform Disorder). It is characterized by one or more symptoms of altered voluntary motor or sensory function that are incompatible with recognized neurological or medical conditions. While anxiety can be a significant co-occurring issue or a precipitating factor, the disorder itself is not primarily classified as an anxiety disorder. Its core feature is the unexplained neurological symptom(s).
(a) Generalised anxiety (Generalized Anxiety Disorder - GAD): GAD is a common anxiety disorder characterized by excessive, uncontrollable, and often irrational worry about everyday things, persisting for at least six months.
(b) Panic disorder: This is an anxiety disorder characterized by recurrent, unexpected panic attacks – sudden periods of intense fear or discomfort that reach a peak within minutes.
(c) Agoraphobia: This is an anxiety disorder characterized by intense fear or anxiety about being in situations from which escape might be difficult or help might not be available, such as public transportation, open spaces, or crowds.
🧠 CONVERSION DISORDER: "La belle indifference" (lack of concern about symptoms) is a classic but not universal feature. Symptoms are real to the patient, not faked.
12 Which of the following conditions presents with survival guiltiness?
a) Generalised anxiety disorder
b) Post-traumatic stress disorder
c) Schizophrenia
d) Grandmal epilepsy
(b) Post-traumatic stress disorder
Survivor guilt (or survival guiltiness) is a common symptom experienced by individuals who have survived a traumatic event in which others died or suffered greatly. It involves persistent and distressing feelings of guilt about having survived when others did not, or about things they did or did not do during the event. This is a well-recognized feature associated with Post-Traumatic Stress Disorder (PTSD), which can develop after exposure to actual or threatened death, serious injury, or sexual violence.
(a) Generalised anxiety disorder (GAD): GAD is characterized by excessive and pervasive worry about various aspects of life, but survivor guilt is not a core diagnostic feature of GAD.
(c) Schizophrenia: Schizophrenia is characterized by psychosis (delusions, hallucinations), disorganized thought and speech, and negative symptoms. While individuals with schizophrenia may experience guilt related to their illness, "survivor guilt" as a specific phenomenon linked to surviving a traumatic event is not a characteristic feature of schizophrenia itself.
(d) Grandmal epilepsy (Tonic-clonic seizure): This is a type of seizure characterized by loss of consciousness and violent muscle contractions. While experiencing seizures can be traumatic, survivor guilt related to others not surviving is not a direct presentation of epilepsy.
PTSD SYMPTOMS: "REAP" - Re-experiencing, Emotional numbing, Avoidance, Physiological hyperarousal
13 Which of the following is an anxiety disorder?
a) Depression
b) Mania
c) Bipolar
d) Phobia
(d) Phobia
A Phobia (or Specific Phobia) is a type of anxiety disorder characterized by an intense, persistent, and irrational fear of a specific object, situation, or activity (the phobic stimulus). Exposure to the phobic stimulus almost invariably provokes an immediate anxiety response, which may take the form of a panic attack. The fear is out of proportion to the actual danger posed, and the individual often recognizes this but cannot control their reaction, leading to avoidance of the feared stimulus.
(a) Depression (Major Depressive Disorder): This is primarily a mood disorder characterized by persistent sadness, loss of interest or pleasure (anhedonia), and other emotional and physical problems. While anxiety symptoms are common in depression (comorbid anxiety), depression itself is classified as a mood disorder, not an anxiety disorder.
(b) Mania: Mania is a state of abnormally elevated arousal, affect, and energy level, or "a state of heightened overall activation with enhanced affective expression together with lability of affect." It is a key feature of Bipolar I Disorder and is classified as a mood state, not an anxiety disorder.
(c) Bipolar (Bipolar Disorder): This is a mood disorder characterized by shifts in mood, energy, activity levels, and concentration, ranging from periods of intense excitement and energy (manic or hypomanic episodes) to periods of depression.
📊 ANXIETY DISORDERS: GAD, Panic Disorder, Phobias, Agoraphobia, Social Anxiety, Separation Anxiety, Selective Mutism
14 Which of the following is NOT associated with suicide?
a) Mental retardation
b) Schizophrenia
c) Major depression
d) Substance abuse
(a) Mental retardation (Intellectual Disability)
While individuals with Mental Retardation (now more commonly termed Intellectual Disability - ID) can experience co-occurring mental health conditions like depression or anxiety, which are risk factors for suicide, ID itself is generally considered to have a lower direct association with suicide compared to severe mental illnesses like major depression, schizophrenia, or substance use disorders. Some studies suggest that suicide rates might be lower in individuals with ID, possibly due to factors like different cognitive understanding of death, closer supervision, or different stressor profiles. However, they are NOT immune to suicidal thoughts or behaviors.
(b) Schizophrenia: Schizophrenia is a severe mental illness that significantly increases the risk of suicide. Individuals with schizophrenia have a lifetime suicide risk estimated to be around 5-10%. Factors include command hallucinations, depression, hopelessness, substance abuse, and impact of illness on functioning.
(c) Major depression (Major Depressive Disorder - MDD): MDD is one of the most significant risk factors for suicide. A large percentage of individuals who die by suicide have a diagnosable mood disorder at the time of their death. Symptoms like hopelessness, worthlessness, anhedonia, and suicidal ideation are core features.
(d) Substance abuse (Substance Use Disorders - SUDs): SUDs are strongly associated with increased risk of suicidal ideation, attempts, and completion. Substance use can lower inhibitions, impair judgment, increase impulsivity, worsen underlying mental health conditions, and lead to social/occupational problems that contribute to hopelessness.
HIGH-RISK CONDITIONS: "SMD" - Schizophrenia, Mood Disorders, Drug/Alcohol abuse
15 Which of the following is the drug of choice for status epilepticus?
a) Diazepam injection
b) Chlor-diazepovide
c) Phenytoin
d) Carbamazepine
(a) Diazepam injection
For the immediate management of status epilepticus (a neurological emergency defined as a continuous seizure lasting more than 5 minutes, or two or more seizures without full recovery of consciousness in between), intravenous (IV) or rectal benzodiazepines are the first-line drugs of choice due to their rapid onset of action. Diazepam injection (IV or rectal gel) is a commonly used benzodiazepine for this purpose. Lorazepam (IV) is another preferred benzodiazepine, often considered superior due to a longer duration of action, but diazepam is widely available and effective. Midazolam (intramuscular, intranasal, or buccal) is also an option, especially in pre-hospital settings.
(b) Chlor-diazepovide (Chlordiazepoxide): This is a benzodiazepine primarily used for anxiety disorders and alcohol withdrawal symptoms. It has a slower onset of action compared to diazepam or lorazepam and is not typically used for the acute treatment of status epilepticus.
(c) Phenytoin: Phenytoin is an anti-epileptic drug often used as a second-line agent if seizures do not stop after initial benzodiazepine administration. It has a slower onset and requires careful administration (slow IV infusion to avoid cardiac side effects), making it unsuitable as the initial drug of choice.
(d) Carbamazepine: Carbamazepine is an anti-epileptic drug used for long-term management of certain seizure types (focal seizures) and also for bipolar disorder. It is an oral medication and is not used for the acute emergency treatment of status epilepticus.
⚡ STATUS EPILEPTICUS PROTOCOL: "D-50" - Diazepam (or Lorazepam) → 50% Dextrose (if hypoglycemia) → Phenytoin (or Fosphenytoin) → Phenobarbital → Midazolam infusion → General anesthesia
16 Which of the following is the commonest side effect of oral combined contraceptive pills?
a) Breakthrough bleeding
b) Cervicitis
c) Fibrocystic disease
d) Ovarian cyst
(a) Breakthrough bleeding
Breakthrough bleeding (BTB) or intermenstrual spotting (bleeding or spotting between expected periods) is one of the most common side effects experienced by women when starting or using combined oral contraceptive pills (COCs), especially with low-dose formulations or during the first few cycles of use. This occurs as the endometrium (uterine lining) adjusts to the new hormonal levels. It usually subsides over time (within the first 3 months for many women).
(b) Cervicitis: Cervicitis is inflammation of the cervix, more commonly caused by infections (like STIs) rather than being a direct side effect of COCs. COCs might even offer some protection against pelvic inflammatory disease (PID).
(c) Fibrocystic disease (Fibrocystic breast changes): Combined oral contraceptives have actually been shown to decrease the incidence and symptoms of benign fibrocystic breast changes, not cause them.
(d) Ovarian cyst: COCs work by suppressing ovulation. By preventing ovulation, they can actually reduce the risk of developing functional ovarian cysts (like follicular cysts or corpus luteum cysts), which form as part of the normal ovulatory cycle.
COC SIDE EFFECTS: "BANANA" - Breakthrough bleeding, Amenorrhea, Nausea, Acne, Mood changes, Weight gain
17 Which of the following is the mode of action of diazepam in patients with persistent tonic clonic convulsions?
a) Slows down cardiac contractions
b) Relaxes peripheral muscles
c) Dilates the bronchial structures
d) Provides amnesia for the convulsive episode
(b) Relaxes peripheral muscles
Diazepam is a benzodiazepine that primarily exerts its anticonvulsant effect by enhancing the activity of gamma-aminobutyric acid (GABA), the main inhibitory neurotransmitter in the central nervous system. By potentiating GABA's effects, diazepam increases neuronal inhibition, which helps to suppress excessive neuronal firing and terminate seizure activity. This central nervous system depression leads to several effects, including muscle relaxation. In tonic-clonic convulsions, the relaxation of peripheral muscles is a direct and observable effect that addresses the tonic (muscle stiffening) and clonic (rhythmic jerking) phases.
(a) Slows down cardiac contractions: While high doses or rapid IV administration of diazepam can cause cardiovascular side effects like hypotension or bradycardia, slowing cardiac contractions is not its primary mode of action or therapeutic goal for treating convulsions.
(c) Dilates the bronchial structures: Diazepam is not a bronchodilator. Drugs that dilate bronchial structures are typically used for respiratory conditions like asthma. Benzodiazepines can, in fact, cause respiratory depression as a side effect.
(d) Provides amnesia for the convulsive episode: While diazepam is known to cause anterograde amnesia, this is a side effect, not its primary mode of action for stopping the convulsion itself. The question asks for the mode of action, which refers to how it therapeutically stops the seizure.
🔬 GABA MECHANISM: Benzodiazepines bind to GABA-A receptors, increasing chloride influx, causing neuronal hyperpolarization and inhibition. This stops seizure spread.
18 Which of the following drug combinations is used for pain management in advanced cancer of the cervix?
a) Furosemide and oral pethidine
b) Paracetamol and oral diclofenac
c) Bisacodyl and oral morphine
d) IM pethidine and oral morphine
(d) IM pethidine and oral morphine
Advanced cancer pain is often severe and requires strong opioids. Option (d) lists two strong opioids. Pethidine is a strong opioid, often used for acute, short-term pain. Morphine is the gold standard strong opioid for chronic cancer pain, typically administered orally for sustained relief. While using two strong opioids concurrently needs careful management, it is a combination of drugs used for severe pain. Intramuscular (IM) pethidine might be used for breakthrough pain or if oral routes are compromised, while oral morphine provides baseline analgesia.
(a) Furosemide and oral pethidine: Furosemide is a loop diuretic used to treat fluid overload; it has no analgesic properties. Pethidine is an analgesic. This combination doesn't make sense for pain management itself.
(b) Paracetamol and oral diclofenac: This combination can be used for mild to moderate pain, or as an adjunct to opioids. However, for advanced cancer pain, which is often severe, this combination alone might not be sufficient and strong opioids are usually required.
(c) Bisacodyl and oral morphine: Bisacodyl is a stimulant laxative used to treat constipation - a common side effect of opioids. While bisacodyl would be appropriately prescribed alongside morphine to manage this side effect, bisacodyl itself is not for pain management.
💊 WHO ANALGESIC LADDER: Step 1: Non-opioids → Step 2: Weak opioids → Step 3: Strong opioids ± adjuvants. Advanced cancer requires Step 3.
19 Which of the following drugs is used to inhibit lactation?
a) Salbutamol
b) Furosemide
c) Bromocriptine
d) Aspirin
(c) Bromocriptine
Bromocriptine is a dopamine D2 receptor agonist. Prolactin, the hormone primarily responsible for milk production (lactation), is under inhibitory control by dopamine released from the hypothalamus. By stimulating dopamine receptors in the pituitary gland, bromocriptine mimics the action of dopamine and thereby inhibits the secretion of prolactin from the anterior pituitary. Reduced prolactin levels lead to the suppression or inhibition of lactation.
(a) Salbutamol: Salbutamol (albuterol) is a short-acting beta2-adrenergic receptor agonist used as a bronchodilator to treat asthma and COPD. It has no role in inhibiting lactation.
(b) Furosemide: Furosemide is a potent loop diuretic used to treat edema and hypertension. It acts on the kidneys to increase urine output and has no direct effect on inhibiting lactation.
(d) Aspirin: Aspirin (acetylsalicylic acid) is a non-steroidal anti-inflammatory drug (NSAID) with analgesic, antipyretic, and antiplatelet properties. It is used for pain relief and to prevent blood clots. It does not inhibit lactation.
LACTATION SUPPRESSION: "BROMO" - Bromocriptine, cabergoline (both dopamine agonists that inhibit prolactin)
20 Which of the following is the most commonly abused drug in Uganda?
a) Nicotine
b) Cannabis
c) Cocaine
d) Alcohol
(d) Alcohol
Globally, and specifically in many parts of Africa including Uganda, alcohol is the most widely used and abused psychoactive substance. Its legal status, cultural acceptance in many contexts, widespread availability (including locally brewed forms), and relatively low cost contribute to its high prevalence of use and abuse. Alcohol abuse leads to significant health problems (liver disease, cardiovascular issues, mental health disorders), social problems (violence, family disruption), and economic burdens. Numerous reports and surveys from Uganda consistently highlight alcohol as the most commonly abused substance.
(a) Nicotine (primarily from tobacco): Nicotine is highly addictive, and tobacco use is a major public health concern. While nicotine dependence is very common, alcohol consumption and its associated harms often surpass it in terms of overall prevalence of "abuse" when considering impairment and broader societal impact.
(b) Cannabis (Marijuana): Cannabis is the most commonly used illicit drug in many parts of the world, including Uganda. Its use is significant, but generally, the overall prevalence of alcohol abuse tends to be higher than that of cannabis abuse when population-level data is considered.
(c) Cocaine: Cocaine is a powerful stimulant drug. While its use occurs in Uganda, particularly in certain urban populations, it is generally far less common and less widely abused compared to alcohol or even cannabis, partly due to its higher cost and more limited availability.
🌍 WHO DATA: Alcohol causes 3 million deaths annually worldwide. In Uganda, alcohol-related harm is a leading public health concern.
















![[Full anterior and posterior views of the human skeleton with major bones and key joints labeled.]](https://nursesrevisionuganda.com/wp-content/uploads/2025/07/Full-anterior-and-posterior-views-of-the-human-skeleton-with-major-bones-and-key-joints-labeled.jpg)
![[Diagram showing the human skeleton with the axial skeleton highlighted or color-coded differently from the appendicular skeleton.]](https://nursesrevisionuganda.com/wp-content/uploads/2025/07/axial-skeleton-highlighted-or-color-coded-differently-from-the-appendicular-skeleton.jpg)
![[Cross-section diagram of a bone showing the outer layer of compact bone surrounding the inner network of spongy bone. Maybe show a flat bone cross-section (diploe) as well.]](https://nursesrevisionuganda.com/wp-content/uploads/2025/07/ClassificationofBonesontheBasisofShape-e1751439762811.jpg)
![[Detailed, labeled diagram of a long bone showing all key anatomical features: diaphysis, epiphysis, metaphysis, epiphyseal line/plate, articular cartilage, periosteum, endosteum, medullary cavity, compact bone, spongy bone.]](https://nursesrevisionuganda.com/wp-content/uploads/2025/07/603_Anatomy_of_Long_Bone-1.jpg)
![[Cross-section diagram of a bone showing the outer layer of compact bone surrounding the inner network of spongy bone. Maybe show a flat bone cross-section (diploe) as well.]](https://nursesrevisionuganda.com/wp-content/uploads/2025/07/Cross-section-diagram-of-a-bone-showing-the-outer-layer-of-compact-bone.jpg)
![[Diagram showing the different types of bone cells (osteogenic cell, osteoblast, osteocyte, osteoclast) and their location/role in bone tissue.]](https://nursesrevisionuganda.com/wp-content/uploads/2025/07/types-of-bone-cells-osteogenic-cell-osteoblast-osteocyte-osteoclast.jpg)
![[Diagram illustrating the process of endochondral ossification, showing the hyaline cartilage model being progressively replaced by bone tissue from primary and secondary ossification centers.]](https://nursesrevisionuganda.com/wp-content/uploads/2025/07/endochondral-ossification.jpg)
![[Diagram illustrating both longitudinal growth at the epiphyseal plate and appositional growth (growth in width) occurring simultaneously in a long bone.]](https://nursesrevisionuganda.com/wp-content/uploads/2025/07/longitudinal-growth-at-the-epiphyseal-plate-and-appositional-growth-1.jpg)
![[Diagram or table illustrating common types of fractures (e.g., transverse, oblique, spiral, comminuted, compression, greenstick, open/closed).]](https://nursesrevisionuganda.com/wp-content/uploads/2023/05/ezgif.com-webp-to-jpg-11-1.jpg)
![[Diagram illustrating the four stages of fracture healing: 1. Hematoma formation, 2. Fibrocartilaginous callus formation, 3. Bony callus formation, 4. Bone remodeling.]](https://nursesrevisionuganda.com/wp-content/uploads/2023/03/Illustration-of-stages-in-bone-healing-after-a-fracture.jpg)
![[Diagram illustrating the three main structural classifications of joints: Fibrous joint (suture), Cartilaginous joint (symphysis or synchondrosis), and Synovial joint. Clearly label the components of a synovial joint (articular cartilage, joint capsule, synovial membrane, synovial fluid, joint cavity, ligaments).]](https://nursesrevisionuganda.com/wp-content/uploads/2025/07/Classification-of-Joints.png)
![[Diagrams illustrating the six different types of synovial joints (Plane, Hinge, Pivot, Condyloid, Saddle, Ball-and-Socket) with a small illustration of the bone shapes and arrows indicating the types of movement allowed for each, and examples of where they are found in the body.]](https://nursesrevisionuganda.com/wp-content/uploads/2025/07/cartilagenous-joints.jpg)
![[Diagram illustrating the three main structural classifications of joints: Fibrous joint (suture), Cartilaginous joint (symphysis or synchondrosis), and Synovial joint. Clearly label the components of a synovial joint (articular cartilage, joint capsule, synovial membrane, synovial fluid, joint cavity, ligaments).]](https://nursesrevisionuganda.com/wp-content/uploads/2025/07/types-of-synovial-joints-1.jpg)
![[Images illustrating common joint disorders: Osteoarthritis (showing cartilage erosion), Rheumatoid Arthritis (showing joint deformity), Gout (inflamed joint), diagram of a sprained ankle, diagram of a joint dislocation.]](https://nursesrevisionuganda.com/wp-content/uploads/2025/07/common-joint-disorders.webp)
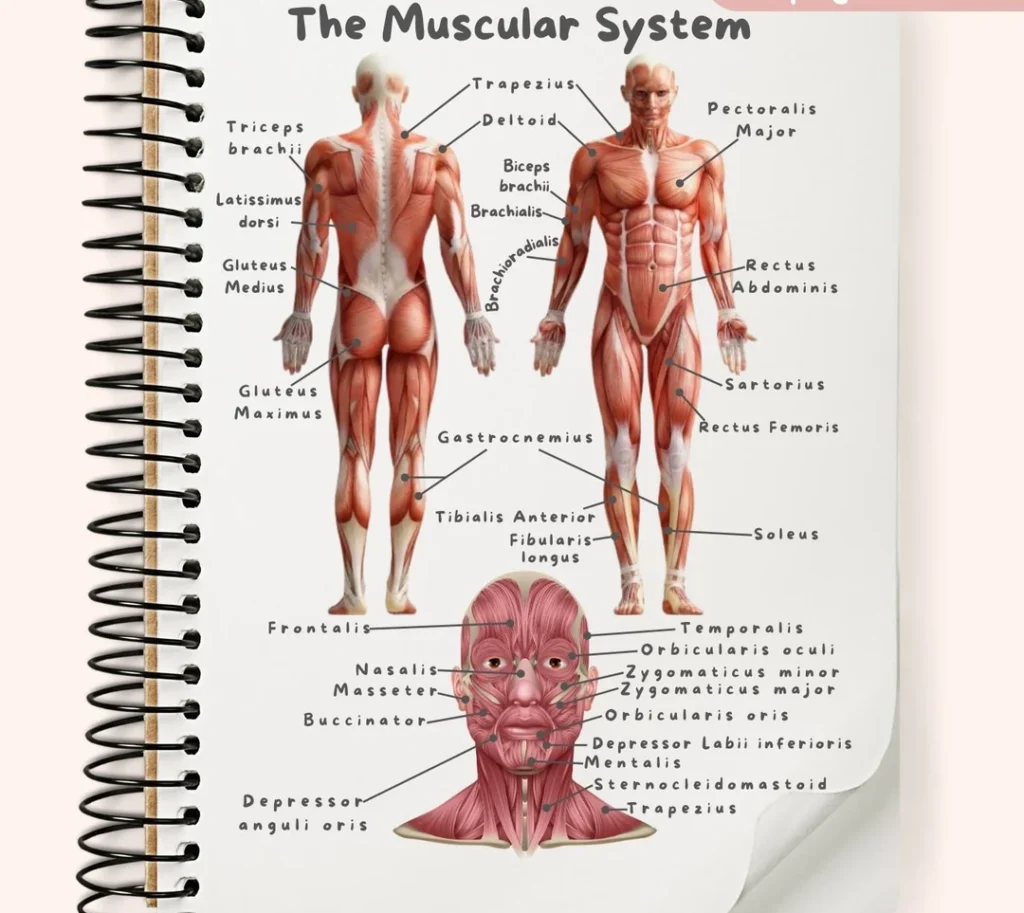
![[An overview diagram showing the major muscles of the human body, anterior and posterior views. Label main muscle groups.]](https://nursesrevisionuganda.com/wp-content/uploads/2025/07/1105_Anterior_and_Posterior_Views_of_Muscles2-1024x631-1.jpg)
![[Microscopic view of skeletal muscle tissue, showing its long, cylindrical fibers, striations, and multiple nuclei located peripherally.]](https://nursesrevisionuganda.com/wp-content/uploads/2025/07/microscopic-skeletal-muscle-e1751345586323.webp) Smooth Muscle:
Smooth Muscle:
![[Microscopic view of smooth muscle tissue, highlighting its spindle shape, single central nucleus, and lack of striations.]](https://nursesrevisionuganda.com/wp-content/uploads/2025/07/Smooth-musclet-tissue-1-1-e1751389483746.png) Cardiac Muscle:
Cardiac Muscle:
![[Microscopic view of cardiac muscle tissue, showing striations, branching cells, central nuclei, and prominent intercalated discs connecting the cells.]](https://nursesrevisionuganda.com/wp-content/uploads/2025/07/Microscopic-view-of-cardiac-muscle-tissue.jpg)
![[Diagram showing the hierarchical structure of a skeletal muscle, starting from the entire muscle organ, down to a fascicle, a single muscle fiber (cell), and finally a myofibril, illustrating the connective tissue coverings at each level.]](https://nursesrevisionuganda.com/wp-content/uploads/2025/07/Diagram-showing-the-hierarchical-structure-of-a-skeletal-muscle.jpg)
![[Detailed diagram illustrating the structure of thick (myosin) and thin (actin, tropomyosin, troponin, elastic/titin) filaments and showing their arrangement within a sarcomere.]](https://nursesrevisionuganda.com/wp-content/uploads/2025/07/Structure-of-Sarcomere.webp)
![[Diagram of a motor unit, showing a motor neuron originating from the spinal cord, its axon branching out, and each axon branch forming a neuromuscular junction with a different skeletal muscle fiber within the muscle.]](https://nursesrevisionuganda.com/wp-content/uploads/2025/07/Diagram-of-a-motor-unit.jpg)
![[Diagram of a motor unit, showing a motor neuron originating from the spinal cord, its axon branching out, and each axon branch forming a neuromuscular junction with a different skeletal muscle fiber within the muscle.]](https://nursesrevisionuganda.com/wp-content/uploads/2025/07/nueromuscular-junction.png)
![[Detailed diagram of the neuromuscular junction, clearly labeling the presynaptic axon terminal, synaptic vesicles containing ACh, the synaptic cleft, the motor end-plate with junctional folds, and acetylcholine receptors on the muscle fiber membrane.]](https://nursesrevisionuganda.com/wp-content/uploads/2025/07/Detailed-diagram-of-the-neuromuscular-junction-clearly-labeling-the-presynaptic-axon-terminal.jpg)
![[Series of detailed diagrams illustrating the step-by-step process of neuromuscular transmission at the NMJ, from arrival of action potential to ACh release, binding, EPP generation, and initiation of muscle action potential.]](https://nursesrevisionuganda.com/wp-content/uploads/2025/07/Step-by-step-process-of-neuromuscular-transmission-at-the-NMJ-1.jpg)
![[Diagram clearly illustrating the difference between a relaxed sarcomere and a contracted sarcomere, showing how the thin filaments move inwards and the Z-discs get closer while the thick and thin filaments retain their original length.]](https://nursesrevisionuganda.com/wp-content/uploads/2025/07/Diagram-clearly-illustrating-the-difference-between-a-relaxed-sarcomere-and-a-contracted-sarcomere.jpg)
![[Series of detailed diagrams illustrating the steps of the sliding filament theory and cross-bridge cycling: 1. Calcium binding to troponin/tropomyosin movement, 2. Cross-bridge formation, 3. Power stroke, 4. ATP binding and detachment, 5. ATP hydrolysis and re-cocking of myosin head.]](https://nursesrevisionuganda.com/wp-content/uploads/2025/07/steps-of-the-sliding-filament-theory-and-cross-bridge-cycling.jpg)
![[Flowchart or diagram comparing the three main metabolic pathways for ATP production in muscle cells: Creatine Phosphate System (Direct Phosphorylation), Anaerobic Glycolysis, and Aerobic Respiration. Show inputs, outputs, speed, duration supported, and location.]](https://nursesrevisionuganda.com/wp-content/uploads/2025/07/Flowchart-or-diagram-comparing-the-three-main-metabolic-pathways-for-ATP-production-in-muscle-cells-1.jpg)
![[Diagram clearly illustrating the concepts of muscle origin and insertion using a specific muscle (e.g., Biceps Brachii or Gastrocnemius) and showing how contraction pulls the insertion towards the origin.]](https://nursesrevisionuganda.com/wp-content/uploads/2025/07/concepts-of-muscle-origin-and-insertion-using-a-specific-muscle.jpg)
![[Diagram illustrating the roles of different muscles (agonist, antagonist, synergist, fixator) during a specific movement, such as elbow flexion or forearm pronation/supination.]](https://nursesrevisionuganda.com/wp-content/uploads/2025/07/roles-of-different-muscles-agonist-antagonist-synergist-fixator.jpg)
![[Diagram illustrating isotonic (concentric and eccentric) and isometric contractions with simple examples like lifting and holding a weight.]](https://nursesrevisionuganda.com/wp-content/uploads/2025/07/isotonic-concentric-and-eccentric-and-isometric-contractions.jpg)
![[Illustrations showing various common body movements (flexion, extension, abduction, adduction, rotation, circumduction) at different joints.]](https://nursesrevisionuganda.com/wp-content/uploads/2025/07/common-body-movements-flexion-extension-abduction.webp)
![[Illustrations showing movements of the ankle and foot (dorsiflexion, plantar flexion, inversion, eversion) and movements of the forearm/wrist (supination, pronation, opposition of the thumb).]](https://nursesrevisionuganda.com/wp-content/uploads/2025/07/common-body-movements-flexion-extension-abduction-adduction-rotation-circumduction-at-different-joints.jpg)
![[Diagrams illustrating the concept of muscle origin and insertion, and showing how muscles act on joints as levers (maybe show a simple example like the elbow joint).]](https://nursesrevisionuganda.com/wp-content/uploads/2025/07/concept-of-muscle-origin-and-insertion-and-showing-how-muscles-act-on-joints-as-levers-1.png)
![[Images illustrating common muscular disorders: muscle strain, tendinitis, muscular dystrophy (showing muscle wasting), myasthenia gravis (e.g., drooping eyelid), diagram of compartment syndrome, image of an inguinal hernia.]](https://nursesrevisionuganda.com/wp-content/uploads/2025/07/common-muscular-disorders.jpg)



