STRABISMUS
Strabismus, also known as “crossed eyes” or “squint,” is a condition characterized by an eye misalignment.
In individuals with strabismus, the eyes do not properly align with each other, meaning they point in different directions. One eye may look straight ahead, while the other eye may turn inward, outward, upward, or downward. This misalignment can be constant or intermittent. often referred to as: cross-eyed, crossed eyes, cockeye, weak eye, wall-eyed, wandering eyes, and/or eye turn.
Strabismus can affect people of all ages, but it commonly develops in early childhood. It is estimated to affect approximately 4% of children. If left untreated, strabismus can cause several issues, including decreased depth perception, double vision (diplopia), and amblyopia (lazy eye), where the brain favors one eye over the other.

Causes of Strabismus
Childhood strabismus often has no known cause, but it tends to run in families.
A. Muscular Factors:
- Imbalance in the extraocular muscles: Strabismus can occur due to a weakness or imbalance in the muscles responsible for eye movement, leading to misalignment.
- Restrictive eye muscle disorders: Certain conditions, such as thyroid eye disease or orbital fractures, can restrict the movement of the eye muscles and cause strabismus.
B. Nervous System Factors:
- Nerve dysfunction: Strabismus may result from abnormalities in the nerves that control eye movements, disrupting the coordination between the eyes.
- Neurological disorders: Some neurological conditions, including cerebral palsy, stroke, or brain tumors, can affect the control of eye movements and lead to strabismus.
- Stroke: Stroke is a leading cause of strabismus in adults
C. Refractive Errors:
- Nearsightedness (myopia): Severe nearsightedness can contribute to the development of strabismus.
- Farsightedness (hyperopia): Strabismus may occur in individuals with uncorrected or significantly imbalanced farsightedness.
D. Other Factors:
- Congenital factors: Some individuals are born with strabismus, which may be related to genetic or developmental factors.
- Eye injuries or trauma: Trauma to the eye or eye muscles can lead to strabismus.
- Graves’ disease: Overproduction of thyroid hormone in Graves’ disease can cause strabismus.
Risk/Predisposing Factors for Strabismus:
Family History:
- Genetic predisposition: Strabismus can run in families, suggesting a genetic component to the condition.
Age and Development:
- Early childhood: Strabismus often develops during infancy or early childhood when the visual system is still developing.
Medical Conditions:
- Neurological disorders: Conditions such as cerebral palsy, Down syndrome, or hydrocephalus increase the risk of strabismus.
- Premature birth: Premature infants are at a higher risk of developing strabismus compared to full-term infants.
Refractive Errors:
- Nearsightedness or farsightedness: Significant refractive errors can contribute to the development of strabismus.
Other Factors:
- Eye muscle imbalance: An imbalance in the strength or coordination of the eye muscles can increase the likelihood of strabismus.
- Visual stress: Prolonged or intense visual activities, such as excessive screen time or reading, may contribute to strabismus development in susceptible individuals.
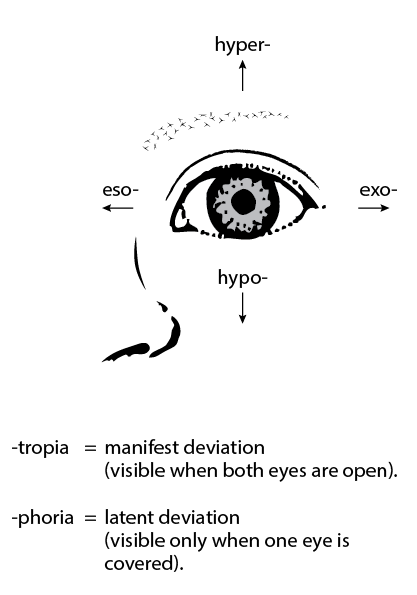
Pathophysiology of Strabismus
The pathophysiology of strabismus involves the extraocular muscles, cranial nerves, and the visual cortex.
- Extraocular Muscles: The extraocular muscles control the movement and position of the eyes. Any problem with these muscles or the nerves that control them can lead to strabismus.
- Cranial Nerves: The extraocular muscles are controlled by cranial nerves III, IV, and VI. If there is an impairment of cranial nerve III, it can cause the associated eye to deviate down and out. Impairment of cranial nerve IV can cause the eye to drift up and slightly inward. Sixth nerve palsy, which affects cranial nerve VI, causes the eyes to deviate inward.
- Causes of Nerve Impairment: There can be various causes of nerve impairment leading to strabismus. Increased cranial pressure can compress the nerve as it runs between the clivus and brain stem. In some cases, twisting of the baby’s neck during forceps delivery can damage cranial nerve VI.
- Visual Cortex: Evidence suggests that the input provided to the visual cortex may play a role in the development of strabismus. This means that strabismus can occur without direct impairment of cranial nerves or extraocular muscles.
- Amblyopia: Strabismus can cause amblyopia, also known as lazy eye. Amblyopia occurs when the brain ignores the signals from one eye, leading to reduced visual acuity. During the early years of life, the brain learns how to interpret the signals from both eyes, and this process, called visual development, can be impaired in strabismus.
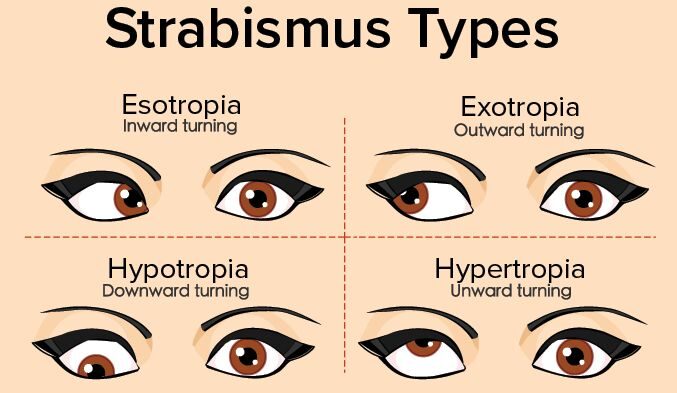
Types of Strabismus
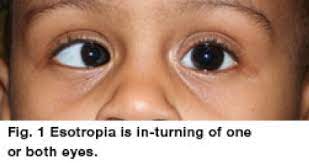
Esotropia:
- Esotropia is a type of strabismus characterized by the inward turn of one or both eyes.
- It can be classified into different subtypes based on the age of onset and underlying causes.
- Infantile esotropia: This type of esotropia appears within the first six months of life and is often constant.
- Accommodative esotropia: It occurs due to farsightedness (hyperopia) and can be corrected with glasses.
- Sixth nerve palsy: Damage to the sixth cranial nerve can cause one eye to turn inward.

Exotropia:
- Exotropia is a type of strabismus characterized by the outward deviation of one or both eyes.
- It can be intermittent or constant and may be more noticeable when the person is tired or daydreaming.
- Exotropia can be classified into different subtypes, including intermittent exotropia, sensory exotropia, and divergence excess exotropia.

Hypertropia:
- Hypertropia is a type of strabismus characterized by one eye deviating upward while the other eye maintains a straight position.
- It can be classified as unilateral (affecting one eye) or bilateral (affecting both eyes).
- Hypertropia can be caused by various factors, including muscle imbalance, thyroid eye disease,trochlear nerve palsy, nerve palsy, or mechanical restrictions.
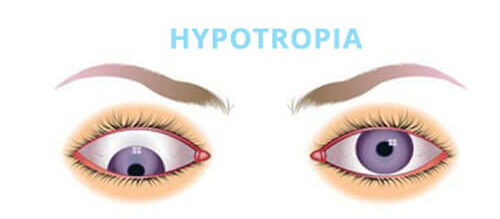
Hypotropia:
- Hypotropia is a type of strabismus characterized by one eye deviating downward while the other eye maintains a straight position.
- It can be classified as unilateral or bilateral, similar to hypertropia.
- Hypotropia can be caused by muscle imbalance, nerve palsy, or mechanical restrictions.
Note; They can also be classified by whether the problem is present in all directions a person looks (comitant) or varies by direction (incomitant).
Clinical Features of Strabismus:
Misalignment of the Eyes:
- The primary clinical feature of strabismus is the misalignment of the eyes, where one eye deviates from its normal position.
- The misalignment can be inward (esotropia), outward (exotropia), upward (hypertropia), or downward (hypotropia).
Double Vision:
- Strabismus can cause double vision, also known as diplopia.
- Double vision occurs when the brain receives conflicting visual information from the misaligned eyes.
Head Tilting or Turning:
- Individuals with strabismus may tilt or turn their head to compensate for the misalignment of their eyes.
- This head posture helps to align the eyes and reduce the diplopia.
Eye Fatigue and Strain:
- Strabismus can lead to eye fatigue and strain due to the constant effort required to align the eyes.
- The misalignment can cause the eye muscles to work harder, leading to discomfort and fatigue.
Reduced Depth Perception:
- Strabismus can affect depth perception, making it difficult to accurately judge distances.
- The misalignment of the eyes can disrupt binocular vision, which is essential for depth perception.
Amblyopia (Lazy Eye):
- Strabismus can result in amblyopia, also known as a lazy eye.
- Amblyopia occurs when the brain suppresses the visual input from the misaligned eye to avoid double vision.
- This can lead to reduced visual acuity and poor development of the affected eye.
Eye Fatigue and Strain:
- Strabismus can lead to eye fatigue and strain due to the constant effort required to align the eyes.
- The misalignment can cause the eye muscles to work harder, leading to discomfort and fatigue.
Headaches:
- Some individuals with strabismus may experience headaches, particularly after prolonged visual tasks.
- The strain on the eye muscles and the disruption of binocular vision can contribute to headaches.
Difficulty Reading:
- Strabismus can affect reading ability, as the misalignment of the eyes can make it challenging to track lines of text smoothly.
- This can result in skipping lines, losing place, or experiencing visual disturbances while reading.
Self-esteem Issues:
- Strabismus can have a psychological impact, leading to self-esteem issues and social difficulties.
- The visible misalignment of the eyes may cause embarrassment or self-consciousness, particularly in children.

Challenges faced by people with strabismus.
- Emotional Distress: Strabismic children commonly exhibit behaviors marked by higher degrees of inhibition, anxiety, and emotional distress. The negative perception of the child by peers can lead to feelings of embarrassment, anger, and a sense of awkwardness, thereby affecting social communication in a fundamental way.
- Negative Effect on Self-esteem: Strabismus can have a negative impact on self-esteem, as individuals may feel self-conscious about their appearance and worry about how others perceive them.
- Limited Opportunities: Strabismus can affect employment opportunities, as individuals may face misconceptions about their ability to work hard. This can lead to career difficulties and limitations in professional growth.
- Social Stigma: The cosmetic aspect of strabismus can result in social stigma, with individuals facing negative attitudes and misconceptions about their intelligence, trustworthiness, and attractiveness. This can lead to feelings of isolation and discrimination.
- Vision Difficulties: Strabismus can cause vision problems such as double vision, difficulty reading, eye strain, and headaches. The misalignment of the eyes can affect depth perception and visual coordination, making it challenging to focus on objects.
COPING MECHANISM TO STRESS FROM HAVING STRABISMUS.
One study categorized coping methods into three subcategories:
- Avoidance: Some individuals may cope with the stress of having strabismus by refraining from participating in activities that they feel may draw attention to their condition.
- Distraction: Deflecting attention from the condition can be a coping mechanism for individuals with strabismus. This may involve focusing on other aspects of their life or engaging in activities that help take their mind off their condition.
- Adjustment: Approaching activities differently can be a coping mechanism for individuals with strabismus. This may involve finding alternative ways to accomplish tasks or adapting to situations to minimize the impact of their condition.
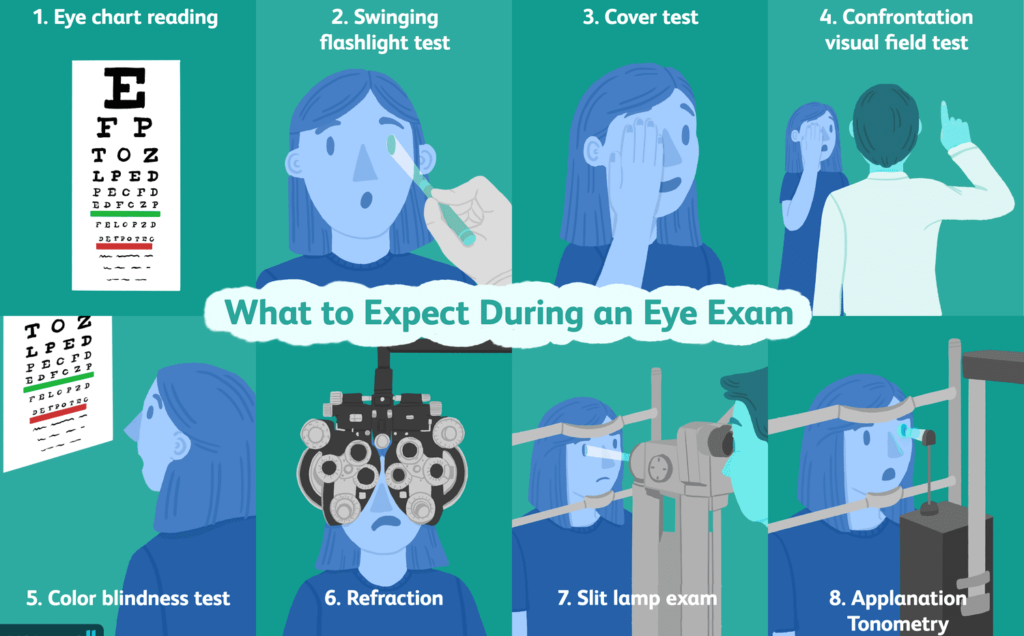
Diagnosis of Strabismus
Diagnosing strabismus involves a combination of medical history, symptom evaluation, and specific eye examinations.
- Medical History: Gather information about the patient’s medical history, including any symptoms related to strabismus, family history of eye conditions, and any underlying health conditions that may be associated with strabismus.
- Symptom Evaluation: Assess the patient’s symptoms, which may include crossed eyes, double vision, decreased depth perception, and misaligned eyes with uncoordinated movements.
- Visual Acuity Test: This test measures the clarity of vision at different distances using an eye chart. It helps determine any changes in vision caused by strabismus.
- Cover-Uncover Test: This test involves covering one eye at a time to observe the movement and alignment of the eyes when the cover is removed. It helps detect any deviation or misalignment of the eyes.
- Ocular Alignment and Focus Test: This test evaluates the movement, focus, and coordination of the eyes. It may involve using a synoptophore, a specialized device that assesses binocular vision and eye alignment.
- Refraction Test: This test measures the refractive error of the eyes using a phoropter and retinoscope. It helps determine if any corrective lenses are needed to compensate for vision changes associated with strabismus.
- Retinal Examination: This examination involves observing the physical structure of the eye, including the retina, to check for any other eye diseases or conditions that may be causing the strabismus symptoms.
- Additional Testing: In some cases, additional tests may be required to evaluate the involvement of other related health conditions. For example, a neurological exam may be conducted to check for conditions such as cerebral palsy or Guillain-Barre syndrome.
Management of strabismus
Management of strabismus involves various treatment options depending on the severity and underlying cause of the condition.
Aims of Management.
- To improve eye alignment and coordination.
- To prevent complications.
- To optimize visual development.
- Eyeglasses: In some cases, strabismus can be corrected or improved with the use of eyeglasses. If a child has blurry vision due to nearsightedness or farsightedness, wearing glasses can help reduce the strain on the eyes and improve alignment.
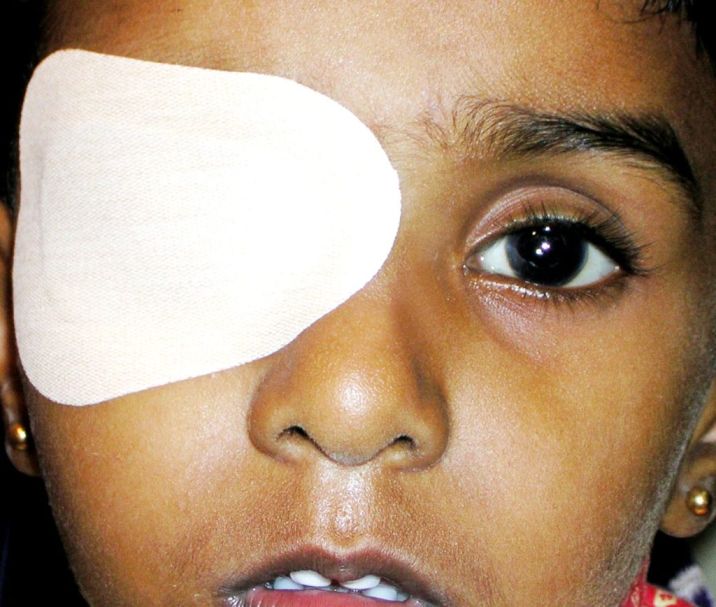
- Patching or eye drops: Patching or using eye drops may be recommended by an ophthalmologist to strengthen the weaker eye. This technique, known as occlusion therapy, helps to encourage the use of the weaker eye and improve its visual development.
- Vision therapy: Vision therapy involves a series of exercises and activities designed to improve eye coordination and strengthen the eye muscles. It is often used in conjunction with other treatments and can be particularly beneficial for individuals with certain types of strabismus.
- Prisms: Prisms are special lenses that can be prescribed to help align the eyes and reduce double vision. They work by bending light and redirecting it to the correct position on the retina, improving visual alignment.
- Botulinum toxin injections: In some cases, botulinum toxin injections may be used to temporarily weaken specific eye muscles, allowing for better alignment of the eyes. The toxin is injected in the stronger muscle, causing temporary and partial paralysis. The treatment may need to be repeated three to four months later once the paralysis wears off. This treatment is reserved for certain types of strabismus or as a temporary measure before considering surgery.
- Eye muscle surgery: Eye muscle surgery is often recommended for individuals with persistent or severe strabismus. During the surgery, the ophthalmologist adjusts the tension or position of the eye muscles to improve eye alignment. This procedure is usually performed under general anesthesia and may require multiple surgeries depending on the individual case.
Nursing Diagnosis.
- Risk for Injury related to impaired sensory function.
The lack of coordination between the muscles around the eyes in strabismus can result in double vision, blurry vision, and poor depth perception, increasing the risk of injury.
- Disturbed Sensory Perception related to structural damage.
Evidence: Strabismus causes a lack of coordination between the muscles around the eyes, leading to double vision, blurry vision, and poor depth perception, which can result in a disturbed sensory perception.
- Knowledge Deficit related to impaired vision.
Evidence: Children with strabismus may have limited understanding of their condition, treatment options, and the need for early intervention. This lack of knowledge can contribute to a knowledge deficit.
- Social Isolation related to limited ability to participate in activities and impaired vision
Evidence: Strabismus can affect a child’s ability to interact socially due to the limited ability to participate in activities and impaired vision, which may lead to social isolation.
- Impaired Parent-Child Interaction related to the child’s visual impairment
Evidence: Strabismus can affect the parent-child interaction due to the child’s visual impairment, which may require additional support and education for parents to effectively communicate and engage with their child.


Always greatful for your work
May God make your dreams true