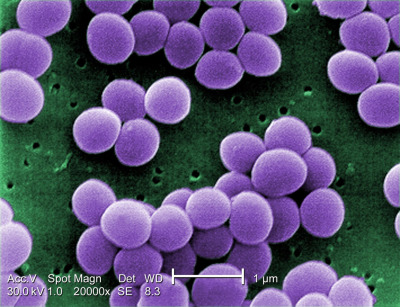
Nocardia Species
Nocardia Species
By the conclusion of this exhaustive master guide, you will be deeply conversant with:
- The comprehensive microbiological profile, biochemical characteristics, and unique staining properties of Nocardia species.
- The critical, high-yield distinctions between Nocardia and Actinomyces in clinical presentations.
- The complex pathogenesis and virulence factors that allow this environmental saprophyte to evade the human immune system.
- The massive spectrum of clinical disease, specifically focusing on Pulmonary, Central Nervous System (CNS), and Cutaneous Nocardiosis.
- The strict, specialized laboratory diagnostic protocols required to successfully isolate and identify the pathogen.
- The exhaustive pharmacological management strategies, including combination therapies, duration of treatment, and surgical interventions.
I. Introduction & General Characteristics
Nocardia species are notorious, life-threatening opportunistic pathogens. While they commonly reside harmlessly in the environment, they can cause devastating, highly destructive, and disseminated infections with a highly specific, dangerous predilection for the brain and lungs in immunocompromised patients.
Microbiological Profile & Morphology:
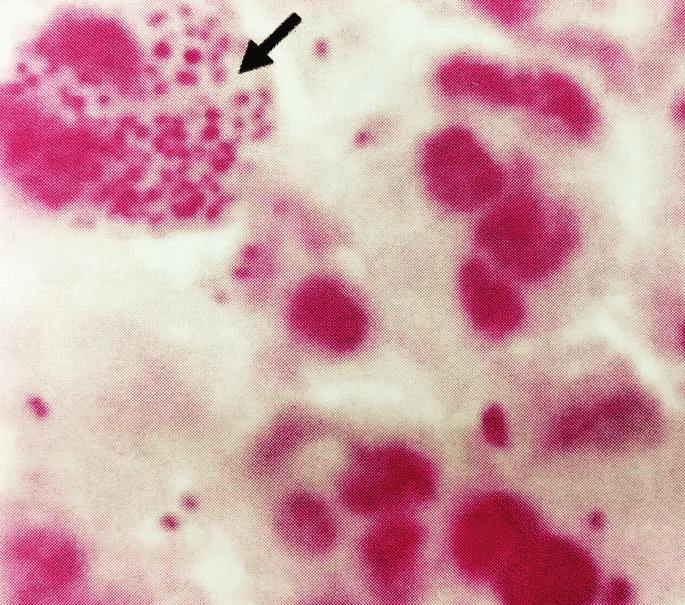
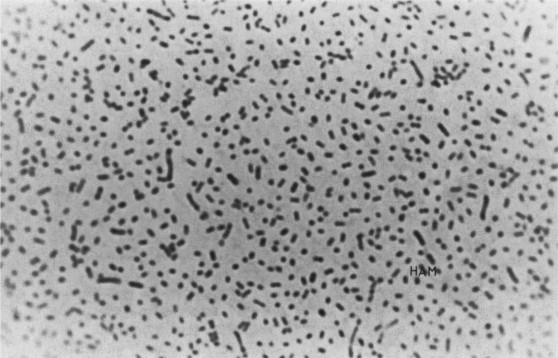
- Gram Stain: They are Gram-positive bacilli, but they are uniquely filamentous and branching. Under the microscope, they appear as a tangled web of delicate, beaded threads that frequently fragment into smaller rod-like (bacillary) and coccoid elements. They often stain irregularly, giving them a "beaded" appearance.
- Oxygen Requirement: They are strictly, obligately aerobic (they absolutely require oxygen to survive and multiply, which explains their overwhelming preference for the highly oxygenated environment of the lungs).
- Ubiquity (Habitat): They are ubiquitous environmental saprophytes (organisms that live on dead or decaying organic matter). They are universally found worldwide in soil, decaying vegetation, fresh water, salt water, and animal feces. Crucial Epidemiological Note: Nocardiosis is strictly an exogenous infection; there is ZERO evidence of person-to-person (human-to-human) transmission.
- Biochemical Tests: They are strongly Catalase-positive, urease variable, and possess the ability to utilize complex carbohydrates.
The "Partially Acid-Fast" Distinction
The cell wall architecture of Nocardia is highly unique and heavily tested. Like Mycobacterium tuberculosis (TB), Nocardia has mycolic acid in its cell wall, providing a waxy, hydrophobic exterior. However, the lipid chains in Nocardia are much shorter (approximately 50-62 carbon atoms) compared to the exceptionally long chains in TB (70-90 carbon atoms).
Because of these shorter chains, Nocardia is only partially acid-fast (also known as weakly acid-fast). It resists decolorization by weak acids (using 1% sulfuric acid) but will be rapidly stripped of its color by strong acids (like the 3% hydrochloric acid used in standard Ziehl-Neelsen TB stains).
To successfully visualize Nocardia, microbiologists MUST use the modified Ziehl-Neelsen, Fite-Faraco, or modified Kinyoun staining methods.
Growth & Culture Characteristics:
- Growth Rate: They are notoriously, excruciatingly slow-growing. Visible macroscopic colonies may take 3 to 5 days to appear, and some fastidious species take up to 2 to 3 weeks to emerge.
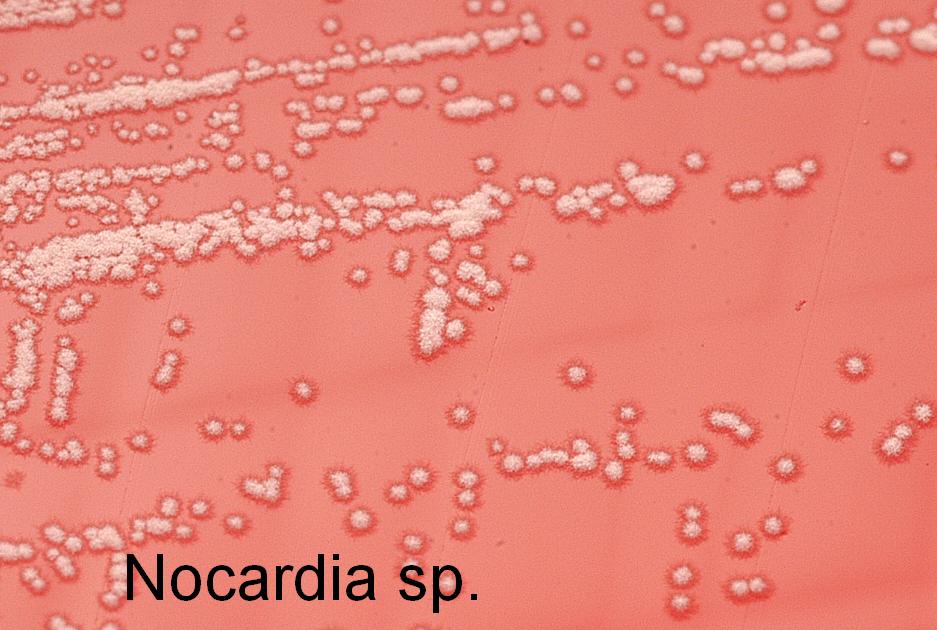
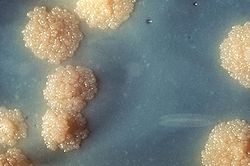
- Colony Morphology: Highly variable. Colonies range from glabrous (smooth) to heavily wrinkled, producing a chalky, waxy, or velvety aerial mycelium. Pigmentation can be strikingly diverse, ranging from chalky white, to cream, to brilliant orange, pink, or red.
- Odor: When cultured, they emit a highly characteristic earthy, musty odor (resembling wet dirt after a fresh rainstorm, caused by the production of the volatile organic compound geosmin).
💡 High-Yield Distinction: Nocardia vs. Actinomyces
These two branching, Gram-positive, filamentous bacteria are constantly tested against each other on clinical board exams. How do you definitively tell them apart clinically and microbiologically?
- Nocardia: Strictly Aerobic (loves the oxygen-rich lungs), found purely in the environment (acquired via inhalation or penetrating soil trauma), and is partially Acid-Fast. It frequently disseminates to the brain.
- Actinomyces: Strictly Anaerobic (loves deep, oxygen-deprived tissue crevices), is part of the normal human oral/cervicovaginal flora (acquired via dental trauma, jaw fractures, or prolonged IUD use), and is absolutely NOT Acid-Fast. It characteristically produces hard, yellow "sulfur granules" in the pus of deep "lumpy jaw" abscesses.
II. Clinically Important Species
There is no single "Nocardia" pathogen. The genus has been extensively reclassified over the last two decades using advanced molecular techniques (like 16S rRNA sequencing) into over 100 distinct species. Understanding the specific species is vital because each exhibits wildly unique clinical behaviors, geographic distributions, and, most importantly, antibiotic resistance profiles.
Historically recognized as the single most common cause of human disease (accounting for over 70% of systemic and pulmonary nocardiosis cases). It has now been genetically dismantled and reclassified into multiple distinct sub-species, including N. cyriacigeorgica, N. farcinica, and N. abscessus.
The undisputed, most common worldwide cause of primary cutaneous (skin) and subcutaneous nocardiosis. It is heavily endemic to tropical and subtropical regions (particularly Mexico, Central America, and the southern United States). It is the classic culprit behind "Madura foot" or Actinomycotic mycetoma following a thorn prick or walking barefoot in contaminated soil.
Highly dangerous and clinically terrifying. It exhibits significantly higher virulence than other species, possesses a massive tropism for causing multiple, overwhelming brain abscesses, and is notoriously multidrug-resistant (frequently resistant to third-generation cephalosporins and occasionally TMP-SMX, often requiring aggressive salvage drugs like Linezolid or Amikacin).
N. otitidiscaviarum: Generally considered less virulent; sporadically causes pulmonary and cutaneous infections, frequently linked to traumatic gardening injuries.
N. nova: Presents with a highly variable clinical picture, often causing disseminated disease in profoundly immunocompromised hosts, but is generally more susceptible to antibiotics (like erythromycin and clarithromycin) than N. farcinica.
III. Virulence and Pathogenesis
How does a simple, environmental soil bacterium survive the hostile, highly regulated interior of the human body and destroy tissue so effectively? It relies on a lethal, sophisticated biochemical toolkit designed specifically to bypass and neutralize our immune system's primary defenders: neutrophils and alveolar macrophages.
Entry Mechanisms:
- Inhalation: Aerosolized soil dust is inhaled deep into the lower respiratory tract, bypassing mucociliary clearance (leading to pulmonary disease). Example: Exposure during massive dust storms, farming, or landscaping.
- Percutaneous Inoculation: Physically introduced through skin trauma (leading to cutaneous disease). Example: Motor vehicle accidents, traumatic thorn pricks, or agricultural injuries.
1. Cord Factor (Trehalose 6,6'-Dimycolate):
A powerful, highly toxic lipid molecule embedded in the bacterial cell wall (a virulence factor famously shared with M. tuberculosis).
- Function: It actively inhibits neutrophil chemotaxis (preventing the immune system from calling for backup) and, most dangerously, prevents the fusion of the phagosome with the lysosome inside human macrophages. By physically blocking this fusion, the bacteria successfully avoid being bathed in deadly lysosomal acid hydrolases, allowing them to survive, germinate, and multiply wildly inside the very immune cells meant to kill them.
2. Oxidative Shielding (Superoxide Dismutase & Catalase):
When macrophages swallow bacteria, they unleash a lethal, rapid "oxidative burst" of toxic free radicals (like superoxide anions and hydrogen peroxide) to burn the bacteria alive at a molecular level.
- Function: Nocardia secretes massive, overwhelming amounts of the enzymes Superoxide Dismutase (SOD) and Catalase. SOD neutralizes the deadly superoxide anion into hydrogen peroxide, and Catalase instantly breaks the hydrogen peroxide down into harmless water and oxygen. This provides an impenetrable molecular shield, completely protecting the bacteria from oxidative killing.
3. Evasion of Phagocytosis & Secretion of Hemolysins:
As the bacteria grow into long, branching filaments, they become physically too large for a single macrophage or neutrophil to engulf. Additionally, some virulent strains secrete hemolysins and cytotoxins that directly puncture and destroy host cell membranes, causing the massive tissue necrosis characteristic of Nocardial abscesses.
4. Central Nervous System (CNS) Tropism:
Nocardia has a highly unique, poorly understood molecular affinity (tropism) for adhering to cerebral capillary endothelium, efficiently crossing the blood-brain barrier, and setting up destructive, multi-loculated (multi-chambered) abscesses directly in deep brain tissue, often without provoking significant meningeal inflammation until the abscess ruptures.
IV. Clinical Manifestations
Nocardiosis is heavily, undeniably associated with profound immunosuppression. It relies on a defect in T-cell-mediated immunity. It almost never affects a completely healthy, immunocompetent host. The disease presents in multiple anatomical forms.
Major Risk Factors for Nocardiosis:
- Immunosuppression: Chronic high-dose corticosteroid therapy (the single highest risk factor), solid organ transplant recipients (kidney, heart, lung) taking anti-rejection drugs like tacrolimus or mycophenolate, hematopoietic stem cell transplants, and advanced HIV/AIDS (CD4 count typically < 100 cells/µL).
- Biologic Therapies: Patients on TNF-alpha inhibitors (e.g., Infliximab, Adalimumab) for autoimmune diseases.
- Structural Lung Disease: Pre-existing architectural damage such as COPD, bronchiectasis, cystic fibrosis, or cavities from previous TB infections.
- Pulmonary Alveolar Proteinosis (PAP): A rare autoimmune/genetic disease where the lung alveoli fill with surfactant-like lipoproteins, providing a perfect, rich, unprotected growth medium for Nocardia.
A. Pulmonary Nocardiosis (Accounts for 50% to 70% of all cases)
Presentation: It acts as a severe, subacute-to-chronic necrotizing pneumonia with rampant abscess formation and massive cavitation.
- Symptoms: Non-specific and insidious. Low-grade but progressive fever, severe productive cough (often with thick, purulent sputum), dyspnea (shortness of breath), pleuritic chest pain, profound weight loss, night sweats, and hemoptysis (coughing up blood).
- Radiology: Chest X-rays and high-resolution CT scans show a highly variable picture: irregular, dense infiltrates, large singular or multiple nodules, and thick-walled cavities. It frequently invades the pleural space causing empyema (pus in the pleural cavity). Diagnostic Trap: It perfectly and flawlessly mimics Pulmonary Tuberculosis, invasive fungal infections (like Aspergillosis or Histoplasmosis), or primary lung malignancy (cancer).
B. Extrapulmonary and Disseminated Nocardiosis
In up to 50% of pulmonary cases, the bacteria break into the bloodstream (hematogenous dissemination) and travel to distant organs.
- CNS Involvement (Brain Abscesses): The brain is the most common site of dissemination. It presents subacutely (slowly worsening over weeks to months) with severe, unrelenting headaches, focal neurological deficits (e.g., unilateral weakness/hemiparesis, cranial nerve palsies, speech difficulty), lethargy, and seizures. Unlike typical bacterial meningitis, the CSF profile may be entirely normal if the abscess has not leaked into the ventricles. It carries an extremely high mortality rate (often >40% even with treatment).
- Cutaneous (Skin) Involvement: Caused by direct inoculation (trauma) or secondary dissemination. Presents in three distinct clinical forms:
- Primary superficial cutaneous: Pustules, severe localized cellulitis, or localized skin abscesses following a scratch.
- Lymphocutaneous (Sporotrichoid) spread: Nodules developing linearly up the arm or leg, perfectly following the anatomical lymphatic drainage tract (mimicking Sporothrix schenckii).
- Actinomycotic Mycetoma (Madura Foot): A chronic, painless, massively swollen, woody, and severely disfiguring deep tissue/bone infection of the foot or hand. It discharges thick pus containing bacterial granules through multiple, chronic, draining sinus tracts to the skin surface.
- Ocular & Other Organs: Can cause destructive, sight-threatening keratitis or endophthalmitis of the eye following direct agricultural trauma (e.g., being struck in the eye with a soil-covered branch). In severely immunocompromised patients, it can disseminate to the kidneys, joints, bone (osteomyelitis), and heart valves.
❓ Applied Clinical Case Study: The Diagnostic Trap
Case: A 55-year-old male kidney transplant recipient currently taking daily prednisone and tacrolimus presents with a 4-week history of a productive, blood-streaked cough, drenching night sweats, and a new-onset, severe, right-sided headache accompanied by left arm weakness. A chest X-ray reveals a massive, thick-walled upper-lobe cavity. The provider aggressively isolates the patient for suspected Tuberculosis. However, three consecutive standard Acid-Fast Bacillus (AFB) stains come back negative. A brain MRI with contrast reveals a 3 cm multi-loculated, ring-enhancing lesion (abscess) in the right frontal lobe. What is the likely pathogen?
Answer: Nocardia species (likely N. farcinica or N. asteroides complex). The patient's profound immunosuppressed status (transplant medications), lung cavities mimicking TB, and the subsequent pathognomonic hematogenous spread to the brain (CNS tropism causing the headache and weakness) are classic, textbook hallmarks for Nocardiosis. The standard TB acid-fast stain (using 3% HCl) was negative because Nocardia is only partially acid-fast; its shorter mycolic acid chains were stripped of dye by the harsh acid. The lab requires a modified weak-acid stain (Fite-Faraco or modified Kinyoun) to accurately visualize the branching filaments.
V. Laboratory Diagnosis
Nocardia is notorious for causing false-negative lab results because it grows so excruciatingly slowly and is easily overgrown by normal respiratory flora. Close, explicit communication between the clinical nurse, the infectious disease physician, and the microbiology lab is absolutely vital to secure a diagnosis.
1. Specimen Collection:
Generous amounts of clinical material must be obtained. This includes deep expectorated sputum, Bronchoalveolar lavage (BAL) fluid via bronchoscopy, open lung biopsy, stereotactic aspirated brain abscess material, or Cerebrospinal fluid (CSF).
2. Microscopy & Staining:
- Gram Stain: Will reliably show delicate, thin, branching Gram-positive filaments, often beaded in appearance.
- Modified Acid-Fast Stain: (Modified Kinyoun or Fite-Faraco using 1% sulfuric acid) will be positive, highlighting the bacteria in bright red/pink against a blue background.
- Gomori Methenamine Silver (GMS) Stain: Frequently used in tissue pathology to stain the filaments black, easily distinguishing them from surrounding necrotic human tissue.
3. Culture Protocol:
- Requires strictly aerobic incubation at 35-37°C, often enhanced by 5-10% CO2.
- The Crucial Clinical Step: The laboratory must be explicitly instructed on the requisition form to "Hold cultures for suspected Nocardia." Standard bacterial cultures are routinely thrown away after 48-72 hours by automated lab systems, which will miss Nocardia completely. Cultures must be held for 14 to 21 days.
- Selective Media: Thrives on Buffered Charcoal-Yeast Extract (BCYE) agar, Sabouraud dextrose agar (often used for fungi but supports Nocardia), or Thayer-Martin agar supplemented with broad-spectrum antibiotics to kill off faster-growing competing bacteria (like Pseudomonas or Streptococcus) that would otherwise drown out the slow-growing Nocardia.
4. Advanced Identification & Susceptibility:
Because the numerous species vary wildly and unpredictably in their antibiotic resistance profiles, basic biochemical testing is no longer sufficient. Modern clinical labs must utilize high-end molecular methods for exact species identification, such as:
- 16S rRNA gene sequencing.
- MALDI-TOF Mass Spectrometry (Matrix-Assisted Laser Desorption/Ionization Time-of-Flight), which matches the unique protein fingerprint of the bacteria against a massive global database.
VI. Pharmacological Treatment & Management
Eradicating Nocardia is exceptionally difficult, frustrating, and prolonged. The bacteria hide intracellularly inside host macrophages, and they aggressively wall themselves off in thick, fibrous, necrotic abscesses that intravenous drugs struggle to physically penetrate.
Sulfonamides
The undisputed drug of choice for almost all Nocardia infections is High-Dose TMP-SMX (Trimethoprim-Sulfamethoxazole / Cotrimoxazole).
- Mechanism: TMP-SMX synergistically blocks two consecutive steps in the bacterial synthesis of essential folate, starving the bacteria of the nucleotides required to build DNA.
- Duration: Treatment is a marathon, not a sprint. It must be maintained for a minimum of 6 to 12 months to completely prevent devastating relapses. For CNS disease (brain abscesses) or severe immunocompromise (like HIV), treatment is often strictly extended to 12 months or longer (sometimes lifelong suppressive therapy).
Severe or Refractory Disease
For patients with sulfa allergies, severe disseminated disease, or brain involvement, monotherapy is guaranteed to fail. Aggressive, multi-drug Induction Therapy is mandatory upfront.
- Alternative Agents: Imipenem, Meropenem, Amikacin, Linezolid, Minocycline, Ceftriaxone, and Cefotaxime.
- Standard Severe Regimen: Often begins empirically with a 2- or 3-drug cocktail (e.g., Intravenous TMP-SMX + Amikacin + Imipenem, or Linezolid) for the first 3 to 6 weeks, stepping down to oral monotherapy (Consolidation Phase) once the patient stabilizes and lab sensitivities return.
- Drug Resistance Alert: Nocardia farcinica is globally recognized as highly resistant to multiple agents (including third-generation cephalosporins) and may specifically require the immediate use of Linezolid to save the patient's life.
Surgical Management:
Antibiotics alone physically cannot clear a heavily walled-off pocket of dead tissue. Surgical intervention is absolutely critical. Surgical drainage, aspiration, or complete resection of large pulmonary cavities, soft tissue abscesses, and particularly brain abscesses (especially those larger than 2.5 cm) is frequently required for survival and to obtain definitive diagnostic tissue.
Susceptibility Testing:
Due to wildly unpredictable resistance patterns among the different reclassified species, formalized antimicrobial susceptibility testing (using broth microdilution) is strictly recommended by the Clinical and Laboratory Standards Institute (CLSI) for all clinically significant isolates. (Note: Due to the pathogen's slow growth, doctors must wait 3 to 5 extra days just for the resistance panel results, making strong empiric combination therapy crucial initially).
🧠 Pharmacological Mnemonic: SNAP
To effortlessly remember the primary, first-line treatments for the two distinct but frequently confused branching, Gram-positive bacteria on exams, remember the word SNAP:
- Sulfonamides (TMP-SMX) are for Nocardia.
- Actinomyces gets Penicillin.
List of References
- Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases. 9th Edition. (Provides the gold standard for clinical manifestations, species classification, and multi-drug treatment regimens for Nocardiosis).
- Murray, P. R., Rosenthal, K. S., & Pfaller, M. A. (2020). Medical Microbiology. 9th Edition. Elsevier. (Details the cellular morphology, trehalose 6,6'-dimycolate virulence factors, and laboratory diagnostic staining procedures).
- Harrison's Principles of Internal Medicine. 21st Edition. McGraw Hill. (Exhaustive overview of clinical pathophysiology, CNS tropism, and the specific impacts of immunosuppression).
- Centers for Disease Control and Prevention (CDC). Guidelines on opportunistic infections in severely immunocompromised populations and transplant recipients.
- Clinical and Laboratory Standards Institute (CLSI). Susceptibility testing protocols for aerobic actinomycetes, detailing the mandatory broth microdilution techniques and required incubation periods.
Quick Quiz
Bacteriology Intro Quiz
Microbiology - mobile-friendly and focused practice.
Privacy: Your details are used only for quiz tracking and certificates.
Bacteriology Intro Quiz
Microbiology
Preparing questions...
Choose your answer and keep your streak alive.
Great effort.
Here is your quick performance summary.