IMNCI Cumulative Exam
IMNCI Cumulative Exam Read More »

Test your knowledge with these 50 questions.
Question 1/50
Here are your results, .
Your Score
27/30
90%
IMNCI Cumulative Exam Read More »

Test your knowledge with these 25 questions.
Question 1/25
Here are your results, .
Your Score
27/30
90%
IMNCI Session 3 Identify Treatment Quiz Read More »

Test your knowledge with these 30 questions.
Question 1/30
Here are your results, .
Your Score
27/30
90%
IMNCI Session One Continuation QUIZ Read More »

Test your knowledge with these 30 questions.
Question 1/30
Here are your results, .
Your Score
27/30
90%
IMNCI Session One Asess and cLASSIFY QUIZ Read More »
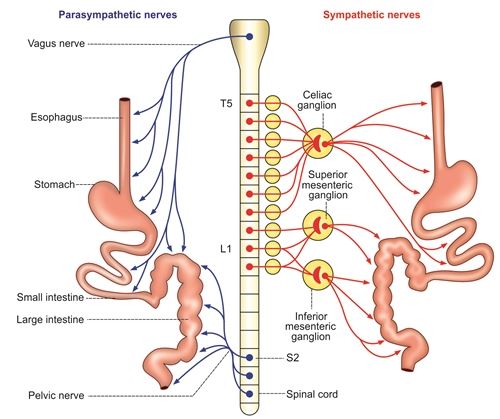
The gastrointestinal (GI) tract is a continuous, hollow, muscular tube that serves as the primary pathway for digestion and absorption. It is approximately 23 to 26 feet (7 to 8 meters) long and extends from the mouth to the anus, passing through the thoracic and abdominopelvic cavities.

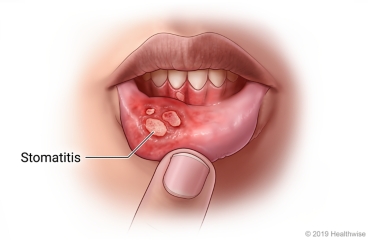
Stomatitis refers to a broad range of inflammatory conditions affecting the epithelial lining of the oral mucosa, which is the moist membrane that lines the inside of the mouth. This inflammation can manifest in various ways, from mild redness and discomfort to severe ulceration and pain, significantly impacting a person's ability to eat, speak, and maintain oral hygiene. Stomatitis is not a single disease but rather a symptom or a group of symptoms that can arise from a diverse array of local (within the mouth) and systemic (affecting the entire body) factors.
The etiology of stomatitis is multifaceted, often involving an interplay of various predisposing and precipitating factors. Understanding the underlying cause is crucial for effective diagnosis and management.
Trauma:The signs and symptoms of stomatitis vary depending on the cause, location, and severity of the inflammation, but commonly include:
Diagnosing stomatitis involves a thorough clinical examination and, often, specific laboratory tests to identify the underlying cause.
Mouth Swab: A sample taken from the affected area for:Effective management of stomatitis is multimodal, focusing on treating the underlying cause, alleviating symptoms, and preventing recurrence.
Treat the Underlying Cause: This is the cornerstone of effective therapy. Antimicrobial Therapy:If left untreated or improperly managed, stomatitis can lead to a range of complications that can significantly impact a patient's health and quality of life. These complications can be localized to the oral cavity or have systemic repercussions.
Preventing stomatitis involves addressing the predisposing factors and maintaining optimal oral and general health. A proactive approach is key.
Stomatitis lecture notes Read More »
Malnutrition is a pathological state resulting from a relative or absolute deficiency or excess of one or more essential nutrients. It refers to any condition in which the body does not receive enough nutrients for proper function, encompassing both undernutrition and overnutrition.
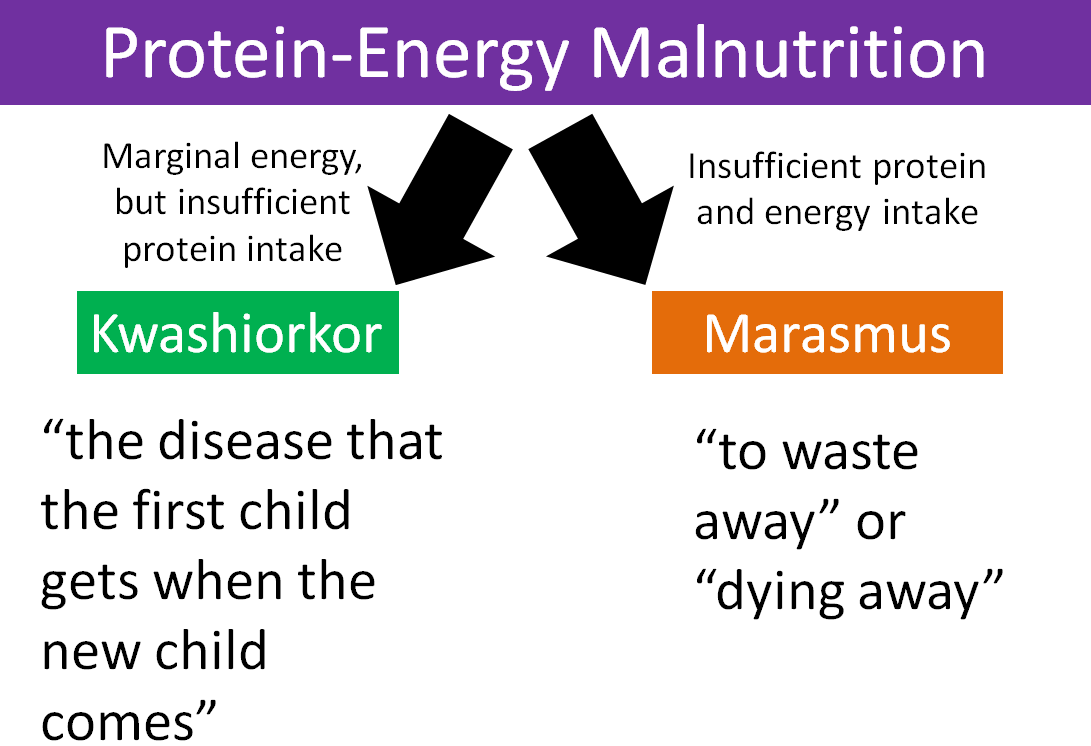
Protein-Energy Malnutrition (PEM), also known as Protein-Calorie Malnutrition (PCM), is a group of clinical conditions resulting from varying degrees of protein and/or energy (calorie) deficiency. It is primarily caused by an inadequate intake of food in both quantity and quality.
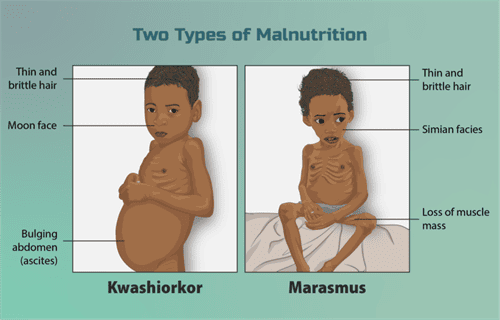
This condition is mainly found in preschool children (typically 1-3 years) after being weaned from breast milk onto a diet high in carbohydrates but low in protein. The name is said to mean "the sickness the older child gets when the new baby comes."
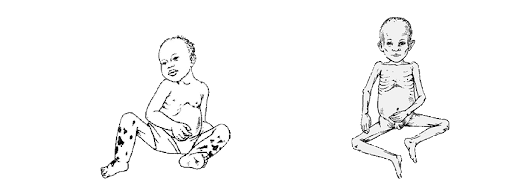
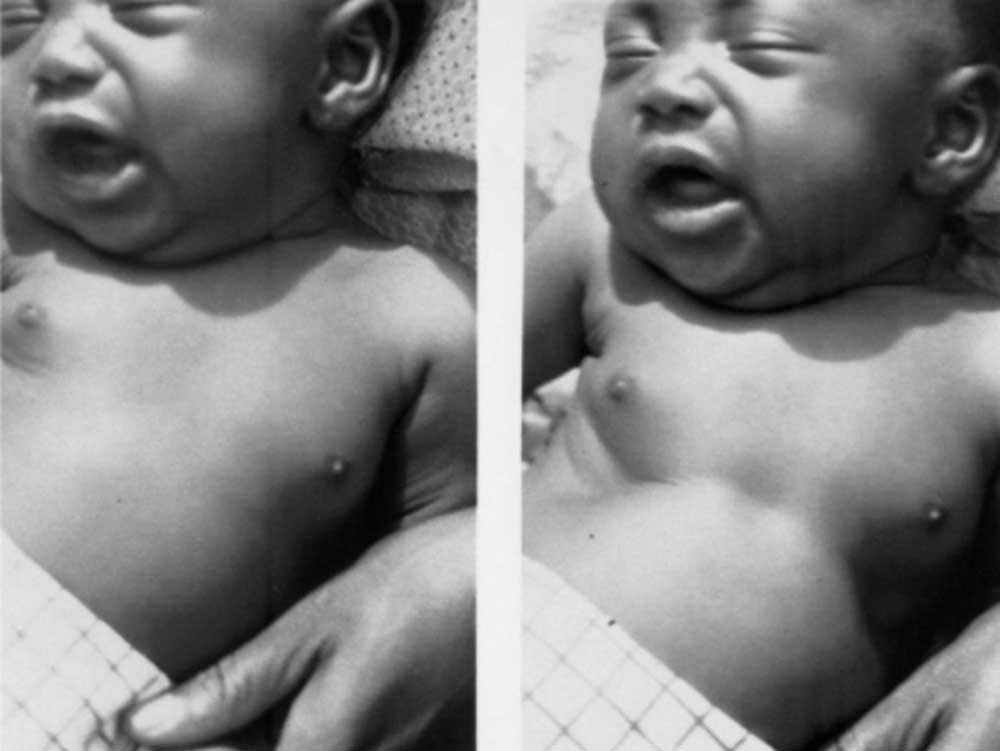
This condition results from a severe, prolonged deficiency of all nutrients, especially energy (calories) and protein. It is common in infants and toddlers. It is also known as infantile atrophy.
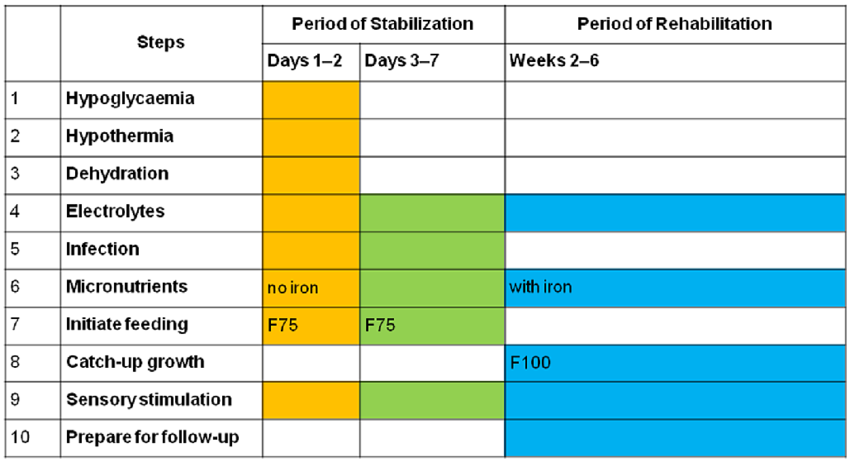
Management depends on the severity of the condition and the presence of complications. It can take place at home, in a nutritional rehabilitation center, or in a hospital.
This is essential for children with severe PEM who have complications like severe edema, infections, dehydration, shock, or persistent loss of appetite. The WHO outlines a 10-step plan for inpatient management.
Vitamins and minerals are essential for bodily functions. Deficiencies can lead to specific disorders.
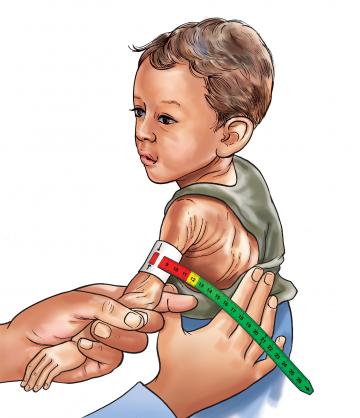
This is the science of body measurements to assess nutritional status.
These are used to identify complications and associated conditions:
MALNUTRITION IN CHILDREN Read More »
Growth monitoring involves regularly weighing a child, plotting the weight on a child health card (also known as a growth chart), interpreting the results, and counseling parents or caregivers. It's a proactive and preventative health measure to track a child's developmental progress over time and identify potential issues early.
Monitoring includes a range of anthropometric measurements to provide a holistic view of the child's physical development. These parameters are compared against standardized growth charts, which show the typical growth patterns of healthy children.
To effectively combat growth problems and ensure optimal child development, a comprehensive approach to growth promotion is essential. This involves a continuum of care starting from the antenatal period and continuing through various stages of childhood, integrating health, nutrition, and social support.
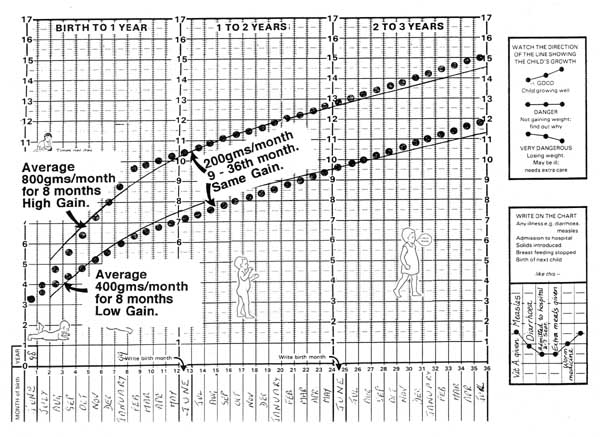
The Child Health Card is a vital clinical tool designed for the comprehensive monitoring of children's health from birth up to 5 years of age. While specifically mentioned as a tool used by the Ministry of Health (MoH) Uganda, similar child health records or growth charts are employed globally to track growth, immunizations, and overall well-being. It serves as a continuous record of a child's health journey, facilitating informed decision-making by healthcare providers and empowering parents in their child's care.
A well-designed Child Health Card typically includes several key sections to capture essential information:
Child demographics specifically include: Child’s name, birth weight, sex, date of birth, birth order, mother’s occupation, father’s name and occupation, and where the child lives.
Effective counseling is a critical component of growth monitoring, empowering mothers with knowledge and practical advice tailored to their child's growth status. The approach differs based on whether the child has gained adequate weight or not.
When a baby in this age group shows healthy weight gain, the counseling focuses on reinforcement and positive affirmation, while also subtly assessing for any underlying issues or misconceptions.
If the baby has not gained weight as expected, the counseling approach shifts to a more investigative and supportive dialogue to identify potential causes and provide targeted solutions.
Counseling continues to build upon previous advice, now incorporating the introduction of complementary foods.
For this age group, inadequate weight gain often points to issues with complementary feeding or ongoing illness.
Growth Monitoring and Promotion Read More »
Young infants have special characteristics which must be considered when classifying their illness. They can become sick and die very quickly from serious bacterial infection but which may manifest themselves through general signs e.g. reduced movements, fever or even hypothermia, failure to breastfeed etc.
ASK: Child’s age ASK : What are the infant’s problems? | ASK: Initial or follow-up visit for problems? MEASURE: Weight and temperature |
All with severe disease require URGENT referral |
MAIN SYMPTOMS
|
URGENT REFERRAL REQUIRED • IDENTIFY and give pre-referral treatment • URGENTLY REFER | TREAT IN CLINIC • IDENTIFY TREATMENT • TREAT • COUNSEL caretaker • FOLLOW-UP CARE | TREAT AT HOME • IDENTIFY TREATMENT • COUNSEL caretaker on home treatment • FOLLOW-UP CARE |
Not feeding.
Severe chest indrawing or Fast breathing.
Convulsions.
No movement/Lethargy.
Temperature too high or too low.
DO QUICK ASSESSMENT OF ALL SICK YOUNG INFANTS BIRTH UP TO 2 MONTHS*
ASK THE MOTHER WHAT THE YOUNG INFANT’S PROBLEMS ARE
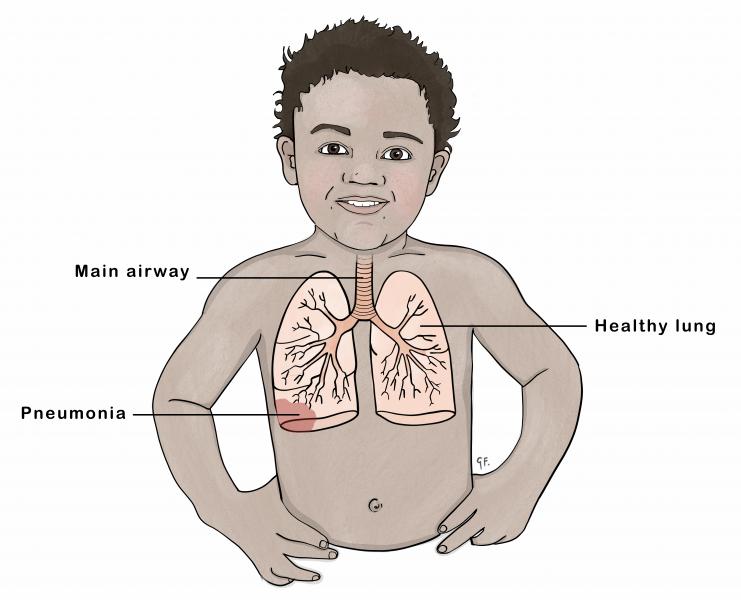
ASSESS:
ASK | LOOK, LISTEN AND FEEL |
ASK and LOOK:
|
(Young infant must be Calm) |
CLASSIFY AND IDENTIFY TREATMENT
SIGNS | CLASSIFY AS | IDENTIFY TREATMENT |
Any of the following signs:
| POSSIBLE SERIOUS BACTERIAL INFECTION OR VERY SEVERE DISEASE | • Immediately resuscitate using a bag and mask if the baby: – Is gasping or not breathing – Has a respiratory rate less than 20 breaths per minute • If convulsing now, give Phenobarbitone • Give the first dose of Benzylpenicillin & Gentamicin. • Treat to prevent low blood sugar • Admit or refer URGENTLY to hospital** • Advise mother how to keep the infant warm on the way to the hospital. • Screen for possible TB disease and check for HIV • If oxygen saturation is less than 90%, start oxygen therapy and refer or admit • IF REFERRAL NOT POSSIBLE (see pg 37) |
| LOCAL BACTERIAL INFECTION | • Give Flucloxacillin Syrup • Teach the mother to treat local infections at home. • Advise mother to give home care for the young infant. • Follow-up in 2 days • Screen for possible TB disease and check for HIV. • Advise mother when to return immediately |
| PNEUMONIA | • Give amoxicillin for 7 days • Advise mother to give home care for the young infant • Follow up on day 4 of treatment |
| LOW BODY TEMPERATURE | • Re-warm the young infant and reassess after 1 hour. (kangaroo warming) • Treat to prevent low blood sugar • Advise mother to give home care for the young infant • Advise mother when to return immediately |
None of the signs of Very Severe Disease or Local Bacterial Infection | INFECTION UNLIKELY | • Advise mother to give home care for the young infant • Screen for possible TB disease and check for HIV. • Advise mother when to return immediately. |
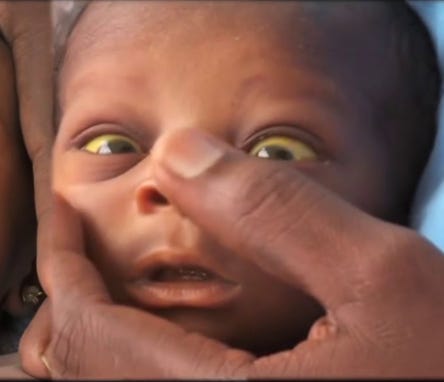
Physiological Jaundice:
Pathological Jaundice:
ASK | LOOK |
|
|
Classify Jaundice
SIGNS | CLASSIFY AS | IDENTIFY TREATMENT |
|
SEVERE JAUNDICE | • Treat to prevent low blood sugar: • Refer URGENTLY to the hospital. • Advise mother how to keep the infant warm on the way or the Hospital. • Screen for possible TB disease |
| JAUNDICE | • Advise the mother to give home care for the young infant. • Advise mother to return immediately if eyes, palms and soles appear yellow • If young infant older than 14 days refer to hospital for assessment. • Follow up in 1 day |
| JAUNDICE | Advise mother to give home care for the young infant |
ASK | LOOK |
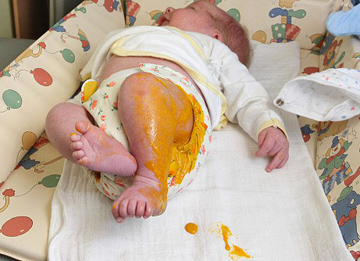
DOES THE YOUNG INFANT HAVE DIARRHOEA OR SIGNS OF DEHYDRATION? IF YES ASK:
* What is diarrhoea in a young infant? A young infant has diarrhoea if the stools have changed from usual pattern and are many and watery (more water than faecal matter). The normally frequent or semi-solid stools of a breastfed baby are not diarrhoea. | Infants Movements • Does the infant move on his/her own? • Does the infant move even when stimulated but then stops? • Does the infant not move at all? • Is the infant restless and irritable? • Look for sunken eyes. Pinch the skin of the abdomen. Does it go back: • Very slowly (longer than 2 seconds)? • Slowly? • Immediately? • Assess the young infant’s ability to feed • Assess the young infant’s urine output |
Classify for DEHYDRATION
SIGNS | CLASSIFY AS | IDENTIFY TREATMENT |
Two of the following signs:
| SEVERE DEHYDRATION | If infant has no other severe classification: • Give fluid for severe dehydration (Plan C) OR If infant also has another severe classification: • Admit/Refer URGENTLY to hospital with mother or caregiver giving frequent sips of ORS on the way • Advise mother to continue breast feeding. • If child is not passing urine admit/refer urgently to hospital. • If child is not able to feed, admit/refer urgently to hospital. |
Two of the following signs:
| SOME DEHYDRATION | • Give fluid and breast milk for some dehydration (Plan B) • Advise mother when to return immediately • Follow-up in 2 days if not improving • If infant also has VERY SEVERE CLASSIFICATION • Admit/Refer URGENTLY to hospital** with the mother giving frequent sips of ORS on the way if child has diarrhoea. • Advise mother to continue breast feeding • Follow-up in 3 days if not improving |
Not enough signs to classify as some or severe dehydration. | NO DEHYDRATION | • Give fluids to treat diarrhoea at home and continue breast feeding at home (Plan A) • Give ORS and Zinc sulphate if child has diarrhoea • Advise mother when to return immediately • Follow-up in 2 days if not improving. |
ASK |
• Has the mother and/or young infant had an HIV test? IF YES: • What is the mother’s HIV status?:
If mother is HIV positive and NO positive DNA PCR test in child ASK: Is the mother on ART and young infant on ARV prophylaxis? IF NO TEST: Mother and young infant status unknown Perform HIV test for the mother: If positive, perform DNA PCR test for the young infant IF the mother is NOT available, do an antibody test on the child. If positive, do a DNA PCR test. |
CLASSIFY HIV STATUS
SIGNS | CLASSIFY AS | IDENTIFY TREATMENT |
| CONFIRMED HIV INFECTION | • Initiate ART, counsel and follow up existing infections • Initiate Cotrimoxazole prophylaxis • Assess child’s feeding and provide appropriate counseling to the mother/ caregiver • Advise the mother on home care • Offer routine follow up for growth, nutrition and development • Educate caregivers on adherence and its importance • Screen for possible TB disease at every visit. • For those who do not have TB disease, start Isoniazid prophylactic therapy (IPT). Screen for possible TB disease throughout IPT • Immunize as per schedule • Follow up monthly as per the national ART guidelines and offer comprehensive management of HIV. Refer to appropriate national ART guidelines for comprehensive HIV care of the child. |
OR
OR
| HIV EXPOSED | • Treat, counsel and follow up existing infections • Initiate Cotrimoxazole prophylaxis • Start or continue PMTCT* prophylaxis as per the national recommendations • Assess child’s feeding and provide appropriate counseling to the mother/caregiver • Advise the mother on home care • Offer routine follow up for growth, nutrition and development • Screen for possible TB disease at every visit • Immunize as per schedule • Follow up monthly as per the national ART guidelines and offer comprehensive management of HIV. Refer to appropriate national ART guidelines for comprehensive care of the child. |
Mother’s antibody test is NEGATIVE | HIV NEGATIVE | • Manage presenting conditions according to IMNCI and other recommended national guidelines • Advise the mother about feeding and about her own health. |
ASK | LOOK AND FEEL |
For symptoms suggestive of TB • Has the young infant had contact with a person with Pulmonary Tuberculosis or chronic cough? • Has the young infant had persistent fevers for 14 days or more? • Does the young infant have pneumonia which is not responding to standard therapy? • Has the young infant been coughing for 14 days or more? | Look or feel for physical signs of TB • Determine weight for age – Weight less than 1.5kg? – Weight for age less than -3 Z score? |
SIGNS | CLASSIFY AS | IDENTIFY TREATMENT |
Presence of ANY of the symptoms and signs suggestive of TB OR weight less than 1.5kg or 3Z score with any symptom. | PRESUMPTIVE TB | • Refer to hospital for further assessment and management • Ask about the caregiver’s health and treat as necessary |
A sick young infant with no TB symptoms or signs | NO PRESUMPTIVE TB | • Treat, counsel, and follow up existing infections • Ask about the caregiver’s health and treat as necessary |

ASK | LOOK AND FEEL | |
Is the infant breastfed? If yes, how many times in 24 hours?
Does the infant usually receive any other foods or drinks?
If yes, how often? If yes, what do you use to feed the infant? | Determine weight for age. – Weight less than 1.5 kg? – Weight for age less than -3 Z score?
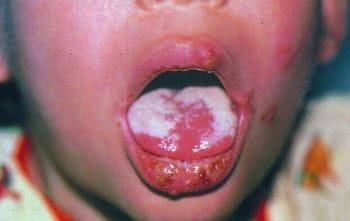
Look for ulcers or white patches in the mouth (thrush). | |
ASSESS BREASTFEEDING: | ||
• Has the infant breast-fed in the previous hour? | • If the infant has not fed in the previous hour, ask the mother to put her infant to the breast. Observe the breastfeed for 4 minutes. • (If the infant was fed during the last hour, ask the mother if she can wait and tell you when the infant is willing to feed again.)
• Is the infant well attached? -not well attached? -good attachment?
• Is the infant suckling effectively (that is, slow deep sucks, sometimes pausing)? -not suckling effectively? -suckling effectively? • Clear a blocked nose if it interferes with breastfeeding. | |
Classify all FEEDING
SIGNS | CLASSIFY AS | IDENTIFY TREATMENT |
• Weight < 1.5 kg, or • Weight < -3 Z score | VERY LOW WEIGHT | • Treat to prevent low blood sugar. • Refer URGENTLY to hospital. • Teach the mother to keep the young infant warm on the way to hospital • Check for HIV |
• Not well attached to breast or • Not suckling eectively, or • Less than 8 breastfeeds in 24 hours, or • Receives other foods or drinks, or • Low weight for age, or • Thrush (ulcers or white patches in mouth) | FEEDING PROBLEM and/or LOW WEIGHT FOR AGE | • If not well attached or not suckling effectively, teach correct positioning and attachment. – If not able to attach well immediately, teach the mother to express breastmilk and feed by a cup • If breastfeeding less than 8 times in 24 hours, advise to increase frequency of feeding. Advise the mother to breastfeed as often and for as long as the infant wants, day and night. • If receiving other foods or drinks, counsel mother about breastfeeding more, reducing other foods or drinks, and using a cup. • If not breastfeeding at all: – Refer for breastfeeding counselling and possible relactation. – Advise about correctly preparing breastmilk substitutes and using a cup. • Check for TB • Advise the mother how to feed and keep the low weight infant warm at home • If thrush, teach the mother how to treat thrush at home. • Advise mother to give home care for the young infant. • Follow up FEEDING PROBLEM or thrush on day 3. • Follow up LOW WEIGHT FOR AGE on day 14. |
• Not low weight for age and no other signs of inadequate feeding | NO FEEDING PROBLEM | • Advise mother to give home care for the young infant. • Praise the mother for feeding the infant well. |
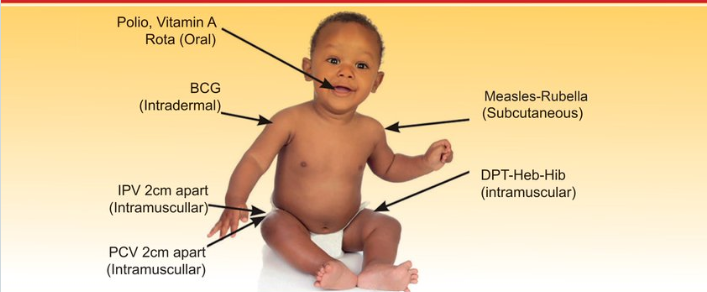
THEN CHECK THE YOUNG INFANT‘S IMMUNIZATION STATUS
Age | Vaccine |
Birth* | BCG |
bOPV-0 | |
6 Weeks | bOPV-1 |
DPT / HepB / Hib -1 | |
PCV 10-1 | |
ROTA 1 |
Assess the child’s growth and development milestones • Plot the child’s weight on his/her growth card (child health card or mother baby passport) • Ask mother about what the child is now able to do in terms of physical movement, communication and interaction. | Assess the Child for ECD / other problems including Congenital Malformations Ask mother for any other problem or identified external malformations • Check child for any external malformations and abnormal signs • Refer infant to hospital, if they have any external malformations ECD-Early Childhood Development | Assess the Mother’s Health Needs • Check if had full course of tetanus toxoid, if not, give an appointment. • Ask if pregnant , if so give an antenatal appointment. If not, ask if interested to talk about family planning. • Ask if RCT has been done and the results. • If mother is an adolescent, link to appropriate clinic or service provider for support. |
1. Give First Doses of Intramuscular Gentamicin and Intramuscular Ampicillin |
– Gentamicin: Give 5 mg/kg/day in once daily injection. In low birthweight (<2.5kg) infants, give 4 mg/kg/day in once daily injection. To prepare the injection: From a 2 ml vial containing 40 mg/ml, remove 1 ml gentamicin from the vial and add 1 ml distilled water to make the required strength of 20 mg/ml. – Ampicillin: Give 50mg/kg IM * If referral is not possible, continue treatment for seven days |
2. Prevent Low Blood Sugar |
– If the young infant is able to breastfeed: Ask the mother to breastfeed the young infant. – If the young infant is not able to breastfeed but is able to swallow: Give 20–50 ml (10 ml/kg) expressed breastmilk before departure. If not possible to give expressed breastmilk, give 20–50 ml (10 ml/kg) sugar water. (To make sugar water: Dissolve 4 level teaspoons of sugar (20 grams) in a 200-ml cup of clean water.) – If the young infant is not able to swallow: Give 20–50 ml (10 ml/kg) of expressed breastmilk or sugar water by nasogastric tube. |
3. Keep the Young Infant Warm on the Way to the Hospital |
– Provide skin-to-skin contact, OR – Keep the young infant clothed or covered as much as possible all the time, especially in a cold environment. Dress the young infant with extra clothing, including a hat, gloves, and socks. Wrap the infant in a soft dry cloth and cover with a blanket. |
4. Refer Urgently |
– Write a referral note for the mother to take to the hospital. – If the infant also has SOME DEHYDRATION OR SEVERE DEHYDRATION and is able to drink: Give the mother some prepared ORS and ask her to give frequent sips of ORS on the way. Advise the mother to continue breastfeeding. – Use the appropriate plan, A, B or C. |
5. How to Give Oral Medicines at Home |
– Follow the instructions below to teach the mother about each oral medicine to be given at home. Also, follow the instructions listed with each medicine’s dosage table. – Determine the appropriate medicines and dosage for the infant’s age or weight. – Tell the mother the reason for giving the medicine to the infant. – Demonstrate how to measure a dose. – Watch the mother practice measuring a dose by herself. – Ask the mother to give the dose to her infant. – Explain carefully how to give the medicine, then label and package the medicine. – If more than one medicine will be given, collect, count, and package each medicine separately. – Explain that all the tablets or syrups must be used for the course of treatment, even if the infant gets better. – Check the mother’s understanding before she leaves the clinic. |
6. Give Oral Amoxicillin |
* Local Infection: Give oral amoxicillin twice daily for 5 days * Pneumonia (fast breathing alone) in infant 7–59 days old: Give oral amoxicillin twice daily for 7 days |
AMOXICILLIN Desired range is 75 to 100 mg/kg/day divided into 2 daily oral doses. Give twice daily
WEIGHT(kg) | Dispersible Tablet (250 mg) Per Dose | Dispersible Tablet (125 mg) Per Dose | Syrup (125 mg in 5 ml) Per dose |
1.5 to 2.4 | 1/2 tablet | 1 tablet | 5 ml |
2.5 to 3.9 | 1/2 tablet | 1 tablet | 5 ml |
4.0 to 5.9 | 1 tablet | 2 tablets | 10 ml |
TEACH THE CAREGIVER TO TREAT LOCAL INFECTIONS AT HOME
Follow the instructions below for every oral drug to be given at home. Also, follow the instructions listed with each drug’s dosage table.
TO TREAT SKIN PUSTULES OR UMBILICAL INFECTION
Apply Gentian Violet twice daily for 5 days.
The mother should:
TO TREAT THRUSH (WHITE PATCHES IN MOUTH) OR MOUTH ULCERS
The mother should:
If breastfed, advise the mother to wash her breast after feeds and apply the same medicine on the areola.
TREAT EYE INFECTION WITH TETRACYCLINE EYE OINTMENT
TEACH THE MOTHER/CAREGIVER TO GIVE ORAL DRUGS AT HOME
Follow the instructions below for every oral drug to be given at home. Also, follow the instructions listed with each drug’s dosage table.

TEACH CORRECT POSITIONING AND ATTACHMENT FOR BREASTFEEDING
Demonstrate how to hold the infant:
Show how to help the infant attach:
TEACH THE MOTHER TO TREAT BREAST OR NIPPLE PROBLEMS

TEACH THE MOTHER HOW TO KEEP THE YOUNG INFANT WITH LOW WEIGHT OR LOW BODY TEMPERATURE WARM AT HOME:
Periodically feel the feet of the baby—baby’s feet should always be warm to touch.
1. Correct Positioning and Attachment for Breastfeeding
Show the mother how to hold her infant:
Show her how to help the infant attach:
2. How to Feed by a Cup
3. How to Express Breastmilk
Ask the mother to:
4. How to Keep the Low Weight Infant Warm at Home
When not in skin-to-skin contact, keep the young infant clothed or covered as much as possible at all times. Dress the young infant with extra clothing, including a hat and socks, loosely wrap the young infant in a soft dry cloth, and cover with a blanket.
Check frequently if the hands and feet are warm. If cold, re-warm the baby using skin-to-skin contact.
Breastfeed the infant frequently (or give expressed breastmilk by cup).
5. How to Give Home Care for the Young Infant
EXCLUSIVELY BREASTFEED THE YOUNG INFANT (for breastfeeding mothers)
MAKE SURE THAT THE YOUNG INFANT IS KEPT WARM AT ALL TIMES
WHEN TO RETURN (Follow-up visit)
Infant’s Condition | Follow-up Day |
JAUNDICE | Day 2 |
DIARRHOEA | Day 3 |
FEEDING PROBLEM | Day 3 |
THRUSH | Day 3 |
LOCAL INFECTION | Day 3 |
PNEUMONIA | Day 4 |
SEVERE PNEUMONIA (referral refused or not possible) | Day 4 |
LOW WEIGHT FOR AGE (in infant receiving no breast milk) | Day 7 |
LOW WEIGHT FOR AGE (in breastfed infant) | Day 14 |
CONFIRMED HIV INFECTION or HIV EXPOSED: POSSIBLE HIV INFECTION | Per national guidelines |
Advise the caretaker to return immediately if the young infant has any of these signs:
Clinical Severe Infection:
If using a 2-day gentamicin regimen:
If using a 7-day gentamicin regimen:
Local Bacterial Infection:
After 2 days:
Treatment:
Jaundice:
After 1 day:
Eye Infection:
After 2 days:
Treatment:
Diarrhoea (Some Dehydration):
After 2 days:
Treatment:
Advise the caretaker to return immediately if the young infant has any of these signs:
Feeding Problem:
After 2 days, reassess feeding.
Exception:
Low Weight or Low Birth Weight:
After 2 days, weigh the young infant and assess if still low weight for age.
Exception:
If feeding is not expected to improve or if the infant has lost weight, refer to the hospital.
Thrush or Mouth Ulcers:
ASSESS AND CLASSIFY A SICK YOUNG INFANT 0-2 MONTHS Read More »
All children found to have pneumonia, persistent diarrhea, ear discharge or very low weight for age (any of these features) and have no urgent need or indication for referral, should be assessed for symptomatic HIV infection.
ASK | LOOK, FEEL AND DIAGNOSE | |
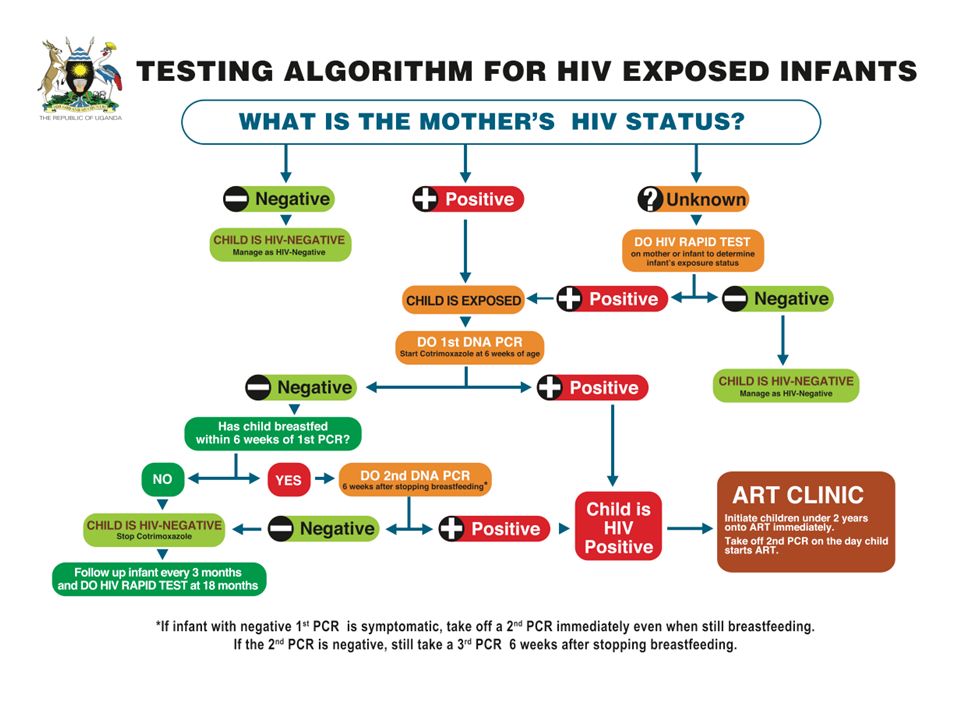
• Ask for mother’s HIV status to establish child’s HIV exposure* Is it: Positive, Negative or Unknown (to establish child’s HIV exposure)
• Ask if child has had any TB Contact | Child <18 months • If mother is HIV positive**, conduct DNA PCR for the baby at 6 weeks or at first contact with the child • If the mother’s HIV status is unknown, conduct an antibody test (rapid test) on the mother to determine HIV exposure. PRESUMPTIVE SYMPTOMATIC DIAGNOSIS OF HIV INFECTION IN CHILDREN <18 MONTHS • Pneumonia *** • Oral Candidiasis /thrush • Severe sepsis • Other AIDS defining conditions**
Child ≥18 months • If the mother’s antibody test is POSITIVE, the child is exposed. Conduct an antibody test on the child.
Child whose mother is NOT available: • Child < 18 months Do an antibody test on the child. If positive, do a DNA PCR test. • Child ≥ 18 months Do an antibody test to determine the HIV status of the child | |
SIGNS | CLASSIFY AS | TREATMENT |
• Child < 18 months and DNA PCR test POSITIVE
• Child ≥ 18 months and Antibody test POSITIVE | CONFIRMED HIV INFECTION | • Initiate ART, counsel and follow up existing infections • Initiate or continue cotrimoxazole prophylaxis • Assess child’s feeding and provide appropriate counseling to the mother/caregiver • Offer routine follow up for growth, nutrition and development and HIV services • Educate caregivers on adherence and its importance • Screen for possible TB disease at every visit. • For those who do not have TB disease, start Isoniazid prophylactic therapy (IPT). Screen for possible TB throughout IPT • Immunize for measles at 6 months and 9 months and boost at 18 months • Follow up monthly as per the national ART guidelines and offer comprehensive management of HIV. Refer to appropriate national ART guidelines for comprehensive HIV care of the child. |
Child<18 months • If mother test is positive and child’s DNA PCR is negative OR • If mother is unavailable; child’s antibody test is positive and DNA PCR is negative | HIV EXPOSED | • Treat, counsel and follow up existing infections • Initiate or continue Cotrimoxazole prophylaxis • Give Zidovudine and Nevirapine prophylaxis as per the national PMTCT guidelines • Assess child’s feeding and provide appropriate counseling to the mother/caregiver • Offer routine follow up for growth, nutrition and development • Repeat DNA PCR test at 6 months. If negative, repeat DNA PCR test again at 12 months. If negative, repeat antibody test at 18 months • Continue with routine care for under 5 clinics • Screen for possible TB at every visit • Immunize for measles at 6 months and 9 months and boost at 18 months • Follow up monthly as per the national ART guidelines and offer comprehensive management of HIV. Refer to appropriate national ART guidelines for comprehensive care of the child. |
• No test results for child or mother • 2 or more of the following conditions: • Severe pneumonia • Oral candidiasis/thrush • Severe Sepsis OR • An AIDS defining condition | SUSPECTED SYMPTOMATIC HIV INFECTION | • Treat, counsel and follow-up existing infections • Give cotrimoxazole prophylaxis • Give vitamin A supplements from 6 months of age every 6 months • Assess the child’s feeding and provide appropriate counseling to the mother • Test to confirm HIV infection • Refer for further assessment including HIV care/ ART • Follow-up in 14 days, then monthly for 3 months and then every 3 months or as per immunization schedule |
Mother’s HIV status is NEGATIVE OR Mother’s HIV status is POSITIVE and child is ≥ 18 months with antibody test NEGATIVE 6 weeks after completion of breastfeeding | HIV NEGATIVE | • Manage presenting conditions according to IMNCI and other recommended national guidelines • Advise the mother about feeding and about her own health |
ASK | LOOK AND FEEL | |
For symptoms suggestive of TB
History of contact
| Look or feel for physical signs of TB
brochodilaters. Collect sample for GeneXpert or smear microscopy
If available, send the child for laboratory tests (GeneXpert or smear microscopy) and/ or Chest X-Ray. | |
SIGNS | CLASSIFY AS | TREATMENT |
Two or more of the following in HIV Negative child AND one or more of the following in HIV Positive child:
OR
| TB | • Initiate TB treatment • Treat, counsel, and follow up any co- infections • Ask about the caregiver’s health and treat as necessary • Link the child to the nearest TB clinic for further assessment and ongoing follow-up • If GeneXpert or smear microscopy test is not available or negative, refer for further assessment |
Positive history of contact with a TB case and NO other TB symptoms or signs listed above | TB EXPOSURE | • Start Isoniazid at 10mg/kg for 6 months • Treat, counsel, and follow up existing infections • Ask about the caregiver’s health and treat as necessary • Link child to the nearest TB clinic |
NO TB symptoms or signs | NO TB | • Treat, counsel, and follow up existing infections • Start Isoniazid in HIV positive child above 1 year at 10mg/kg for 6 months |
Immunization Schedule
Age | Vaccine |
Birth | BCG* |
OPV-0 | |
6 weeks | DPT+HepB+HIB |
OPV-1 | |
RTV1 | |
PCV1 | |
10 weeks | DPT+HepB+HIB |
OPV-2 | |
RTV2 | |
PCV2 | |
14 weeks | DPT+HepB+HIB |
OPV-3 | |
IPV | |
RTV3 | |
PCV3 | |
9 months | Measles |
| VITAMIN A SUPPLEMENTATION Give every child a dose of Vitamin A every six months from the age of 6 months. Record the dose on the child’s chart. ROUTINE DEWORMING TREATMENT Give every child mebendazole every six months from the age of 1 year. Record the dose on the child’s chart. |
Child is under 18 months:
Child is over 18 months:
If results are discordant, refer
If HIV infection is confirmed, and child is in stable condition, GO TO STEP 2
Check that the caregiver is willing and able to give ART. The caregiver should ideally have disclosed the child’s HIV Status to another adult who can assist with providing ART, or be part of a support group.
but NOT ON ART. Counsel and support the caregiver. Follow-up regularly. Move to STEP 3 once the caregiver is willing and able to give ART.
Record the following information:
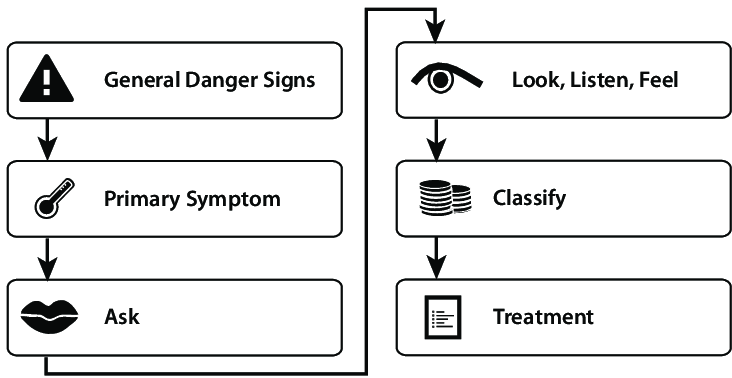
Overview: The IMNCI guidelines provide a structured approach to managing HIV in children through systematic assessment, classification, treatment, and counseling. This follows the standard IMNCI process flow: Assess → Classify → Treat → Counsel → Follow-up.
Refer to: Page 9 (Child 2 months–5 years) and Page 37 (Young Infant 0–2 months)
Before managing HIV, you must determine the status for every child not already enrolled in HIV care.
Based on assessment, the child is classified into one of three categories. The management depends entirely on this classification.
| Classification | Criteria | Color Code | Management Level |
|---|---|---|---|
| CONFIRMED HIV INFECTION |
|
PINK - URGENT | Immediate treatment & ART linkage |
| HIV EXPOSED |
|
YELLOW - CLINIC | Prophylaxis & frequent monitoring |
| HIV INFECTION UNLIKELY |
|
GREEN - HOME | Routine care & prevention counseling |
| Age/Weight | Formulation | Dose |
|---|---|---|
| < 6 months | 5 ml syrup (40/200 mg per 5ml) | 2.5 ml once daily |
| 6 months – 5 years | 5 ml syrup OR ½ adult tablet (80/400 mg) | 5 ml or ½ tablet once daily |
Correct feeding is critical to reduce HIV transmission and ensure child survival.
Advise stopping breastfeeding ONLY if ALL these criteria are met:
| AFASS | Requirements |
|---|---|
| Acceptable | Socially and culturally acceptable to mother and family |
| Feasible | Mother has time, knowledge, skills, and support to prepare formula 8-12 times daily |
| Affordable | Mother/family can afford continuous formula supply for 1 year without harming family nutrition |
| Sustainable | Continuous supply of formula and clean water is assured |
| Safe | Clean water, hygienic preparation, and feeding with cup (not bottle) can be ensured |
Check that the caregiver is willing and able to give ART. The caregiver should ideally have:
Caregiver able to give ART: GO TO STEP 3
Caregiver not able: Classify as CONFIRMED HIV INFECTION but NOT ON ART. Counsel and support the caregiver. Follow-up regularly. Move to STEP 3 once the caregiver is willing and able to give ART.
Record the following information:
Patient Category | Indication | ARV Regimen |
Adults and Adolescents (aged 10 and above) | Initiating ART | TDF+3TC+DTG |
Alternative Regimens | ||
TDF+3TC+DTG (Contraindications for EFV) | ||
ABC+3TC+DTG (Contraindications for TDF) | ||
Pregnant or Breastfeeding Women | Initiating ART | TDF+3TC+DTG |
Alternative Regimen | ||
ABC+3TC+ATV/r (Contraindications for TDF or EFV) | ||
Children (3 to <10 years) | Initiating ART | ABC+3TC+DTG |
Alternative Regimen | ||
ABC+3TC+NVP (Contraindications for EFV) | ||
Children Under 3 Years | Initiating ART | ABC+3TC+LPV/r |
Alternative Regimen | ||
AZT+3TC+LPV/r (Hypersensitivity reaction to ABC) | ||
Population | Patients Failing First-Line Regimens | Second-Line Regimens | Third-Line Regimens |
Adults, Pregnant and Breastfeeding Women, Adolescents | TDF + 3TC + DTG | AZT+3TC+ATV/r (recommended) or AZT+3TC+LPV/r (alternative) | All 3rd line regimens guided by resistance testing |
If not exposed to INSTIs: DRV/r + DTG ± 1-2 NRTIs | |||
If exposed to INSTIs: DRV/r + ETV±1-2 NRTIs | |||
TDF + 3TC + DTG | |||
ABC+ 3TC+ DTG | |||
ABC+ 3TC+ EFV | |||
ABC/3TC/NVP | |||
TDF/3TC/NVP | |||
AZT/3TC/NVP | |||
TDF+3TC+ATV/r (recommended) or TDF+3TC+LPV/r | AZT/3TC/EFV | ||
Children (3–<10 years) | ABC + 3TC + DTG | AZT+3TC+LPV/r | For children above 6 years, and prior exposure to INSTIs, DRV/r±1-2 NRTIs |
ABC+ 3TC + NVP | |||
AZT+3TC+NVP | |||
ABC+3TC+LPV/r | |||
For children below 6 years, AZT/3TC/EFV | |||
DRV/r+ RAL+ 2 NRTIs | |||
AZT+3TC+LPV/r | |||
Children Under 3 Years | ABC+3TC+LPV/r pellets | AZT+3TC+RAL | Optimize regimen using genotype profile |
AZT+3TC+LPV/r pellets | |||
ABC+3TC+RAL | |||
AZT+3TC+NVP | |||
ABC+3TC+LPV/r | |||
ABC: Abacavir AZT: Zidovudine 3TC: Lamivudine LPV/r: Lopinavir/Ritonavir RTV: Ritonavir NVP: Nevirapine | EFV: Efavirenz DTG: Dolutegravir TDF: Tenofovir Disoproxil Fumarate RAL: Raltegravir ATV/r: Atazanavir/Ritonavir |
AGE/WEIGHT | FIRST LINE TB/HIV CO-INFECTION |
< 2 Weeks | Start TB treatment immediately, start ART (Usually after 2 weeks of age) once tolerating TB drugs |
> 2 Weeks and <35 kgs | ABC/3TC/LPVr/RTV If not able to tolerate super boosted LPVr/RTV then use ABC/3TC + RAL for duration of TB treatment. After completion of TB treatment revert back to the recommended 1st line regimen ABC/3TC +LPVr. If on ABC/3TC/DTG regimen – continue If on NVP based regimen, change to EFV. |
>35 kgs body weight and < 15 years age | ABC/3TC/DTG continue with the regimen AND double the dose for DTG If on PI based regimen switch the patients to DTG, hence doubling the dose |
WEIGHT (KG) | SUSPENSION 240MG PER 5ML | SINGLE STRENGTH TABLET 480MG (SS) | DOUBLE STRENGTH TABLET 960MG (DS) |
1-4 | 2.5ml | 1/4 SS tab | – |
5-8 | 5ml | 1/2 SS tab | 1/4 DS tab |
9-16 | 10ml | 1 SS tab | 1/2 DS tab |
17-30 | 15ml | 2 SS tab | 1 DS |
>30(Adults and adolescents) | – | 2 SS | 1 DS |
Dose by body weight is 24-30 mg/kg once daily of the trimethoprim-sulphamethaxazole – combination drug.
• Oral thrush management– use miconazole gel
• Cotrimoxazole use is still recommended
• Most infants and children initiated on treatment take time before immune recovery occurs
• Children on LPV/r – continue with boosted ritonavir
• RAL – for those unable to tolerate super boosted LPV/r
WEIGHT RANGE (KG) | ABACAVIR + LAMIVUDINE 120 mg ABC + 60 mg 3TC | ZIDOVUDINE + LAMIVUDINE 60 mg ZDV + 30 mg 3TC | EFAVIRENCE (EFV) Once Daily 200mg tabs | LAMIVUDINE + ZIDOVUDINE Twice Daily 200mg tabs |
3 – 5.9 | 0.5 tab | 1 tab | – | |
6 – 9.9 | 1 tab | 1.5 tabs | – | |
10 – 13.9 | 1 tab | 2 tabs | 1 tab | 1.5 tabs |
14 – 19.9 | 1.5 tabs | 2.5 tabs | 1.5 tabs | + 1 tab in AM & 0.5 tab in PM |
20 – 24.9 | 2 tabs | 3 tabs | 1.5 tabs | 1 tab in AM & 0.5 tab in PM |
25 – 34.9 | 300 mg ABC + 150 mg 3TC | 300 mg ZDV + 150 mg 3TC | 2 tabs | 1 tab in AM & 0.5 tab in PM |
SIGNS or SYMPTOMS | APPROPRIATE CARE RESPONSE |
Yellow eyes (jaundice) or abdominal pain | Stop drugs and REFER URGENTLY |
Rash | If on abacavir, assess carefully. Call for advice. If severe, generalized, or associated with fever or vomiting: stop drugs and REFER URGENTLY |
Nausea | Advise drug administration with food. If it persists for more than 2 weeks or worsens, call for advice or refer. |
Vomiting | If medication is seen in vomitus, repeat the dose. If vomiting persists, bring the child to the clinic. REFER URGENTLY if vomiting everything or associated with severe symptoms. |
Diarrhoea | Assess, classify, and treat using diarrhoea charts. Reassure that it may improve in a few weeks. Follow up as per chart booklet. Call for advice or refer if not improved after two weeks. |
Fever | Assess, classify, and treat using fever chart. |
Headache | Give paracetamol. If on efavirenz, reassure that it is common and usually self-limiting. Call for advice or refer if it persists for more than 2 weeks or worsens. |
Sleep disturbances, nightmares, anxiety | Due to efavirenz. Administer at night on an empty stomach with low-fat foods. Call for advice or refer if it persists for more than 2 weeks or worsens. |
Tingling, numb, or painful feet or legs | If new or worse on treatment, call for advice or refer. |
Changes in fat distribution | Consider switching from stavudine to abacavir, consider viral load. Refer if needed. |
Care for the child who returns for follow-up using all the boxes that match the child’s previous classifications.
If the child has any new problem, assess, classify fully and treat as on the ASSESS AND CLASSIFY chart.
PNEUMONIA After 2 days Check the child for general danger signs. Assess the child for cough or difficult breathing. Ask:
Treatment:
|
WHEEZINGAfter 2 days Check the child for general danger signs or chest indrawing. Assess the child for cough or difficult breathing. Ask:
For Children under 1 year:
General danger sign or stridor in a calm child or chest indrawing, fast breathing, poor feeding;
For Children over 1 year:
General danger sign or stridor in a calm child or chest indrawing, fast breathing, poor feeding;
|
PERSISTENT DIARRHOEAAfter 5 days Ask:
Treatment:
|
DYSENTERYAfter 2 days Assess the child for diarrhea. > See ASSESS & CLASSIFY chart Ask:
Treatment:
If the condition is the same: add Metronidazole to the treatment. Give it for 5 days. Advise the mother to continue ciprofloxacin and zinc and to return in 2 days.
|
UNCOMPLICATED MALARIAIf fever persists after 3 days, or recurs within 14 days: Do a full reassessment of the child. >See ASSESS & CLASSIFY chart. Assess for other causes of fever. Treatment:
|
FEVER – NO MALARIAIf fever persists after 3 days: Do a full reassessment of the child. > See ASSESS & CLASSIFY chart (see pg 6) Assess for other causes of fever. Treatment:
|
EYE OR MOUTH COMPLICATIONS OF MEASLESAfter 2 days: Look for red eyes and pus draining from the eyes. Look at mouth ulcers. Smell the mouth. Treatment for Eye Infection:
Treatment for Mouth Ulcers:
Treatment for thrush:
|
EAR INFECTIONAfter 5 days: Reassess for ear problem. > See ASSESS & CLASSIFY chart Measure the child’s temperature. Treatment:
|
FEEDING PROBLEMAfter 5 days: Reassess feeding. See questions at the top of the COUNSEL THE MOTHER. Ask about any feeding problems found on the initial visit.
|
PALLORAfter 14 days:
|
MALNUTRITIONAfter 14 days: If the child is gaining weight, encourage the mother to continue with feeding. Counsel the mother about any feeding problem. SEVERE MALNUTRITION WITHOUT COMPLICATIONS After 7 days or during regular follow-up:
Treatment:
MODERATE ACUTE MALNUTRITION After 14 days:
Treatment:
|
| HIV EXPOSED & INFECTED CHILDREN HIV INFECTED CHILD After 1 month:
HIV EXPOSED CHILD (<18 months): For children tested DNA PCR Negative After 1 month:
|
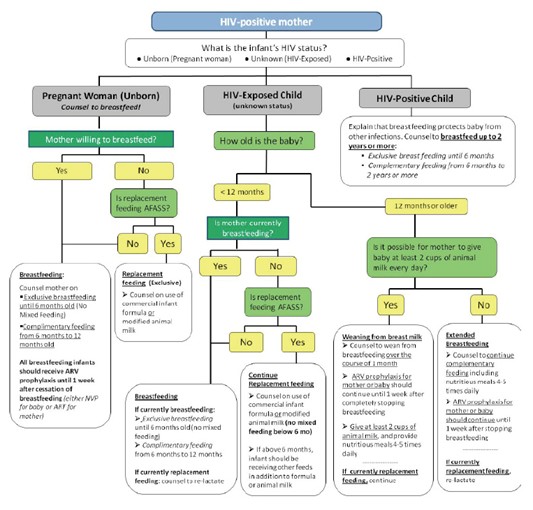
For Mothers and caregivers of infants under 18 months.
Goals:
Just after giving birth, the mother should be counseled on:
Overview of Infant Feeding Guidelines for Exposed Infants
Manage HIV/AIDS using IMCI approach Read More »
Follow the instructions below for every oral drug to be given at home
Also, follow the instructions listed with each drug’s dose
Give an appropriate oral antibiotic**

FIRST-LINE ANTIBIOTIC: Oral Amoxicillin
Age or Weight | Amoxicillin(Give two times daily for 5 days) |
2 months up to 12 months (4 – <10 kg) | 1 tablet (250 mg) or 5 ml syrup |
12 months up to 3 years (10 – <14 kg) | 2 tablets (250 mg) or 10 ml syrup |
3 years up to 5 years (14-19 kg) | 3 tablets (250 mg) or 15 ml syrup |
ANTIBIOTIC FOR PROPHYLAXIS: Oral Cotrimoxazole
Age | Cotrimoxazole(Give once a day starting at 4-6 weeks of age) |
Less than 6 months | 2.5 ml syrup |
6 months up to 5 years | 5 ml syrup or 2 tablets (20/100 mg) |

FIRST-LINE ANTIBIOTIC: Oral Ciprofloxacin
Age | Ciprofloxacin(Give 15 mg/kg two times daily for 3 days) |
Less than 6 months | 1/2 tablet (250 mg) |
6 months up to 5 years | 1 tablet (250 mg) or 1/2 tablet (500 mg) |
FIRST-LINE ANTIBIOTIC FOR CHOLERA: Erythromycin
SECOND-LINE ANTIBIOTIC FOR CHOLERA: Tetracycline
Age or Weight | Erythromycin | Tetracycline |
2 years up to 5 years (10 – 19 kg) | 1 tablet (250 mg) | 1 tablet (250 mg) |
Give four times daily for 3 days
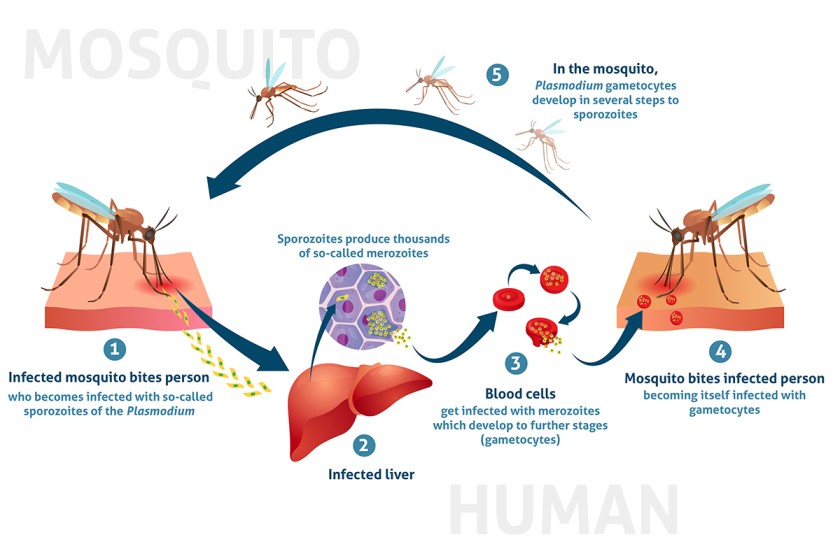
FIRST-LINE ANTIMALARIAL: ARTEMETHER + LUMEFANTRINE (AL)
SECOND-LINE ANTIMALARIAL: DIHYDROARTEMISININ-PIPERAQUINE (DHA-PPQ)
Artemether + Lumefantrine Tablets Dosage
Weight (kg) | Age (Years) | AL Dosage |
Below 15 | Below 3 | 20mg Artemether and 120mg Lumefantrine |
15 – 24 | 3 – 7 | 40mg Artemether and 240mg Lumefantrine |
Counsel the Mother or Caregiver on Malaria Management for a Sick Child:
SECOND LINE: DIHYDROARTEMISININ 20MG + PIPERAQUINE 160MG
Dihydroartemisinin + Piperaquine Dosage
Body Weight (kg) | Dose (mg) |
5 to < 8 | 20 + 160 |
8 to <11 | 30 + 240 |
11 to < 17 | 40 + 320 |
FIRST-LINE TREATMENT FOR SEVERE MALARIA: ARTESUNATE
Artesunate is provided as a powder accompanied by a 1ml vial of 5% bicarbonate. The preparation involves further dilution with either normal saline or 5% dextrose, with the specific amounts varying for intravenous (IV) or intramuscular (IM) administration (refer to the table below).
Preparing IV/IM Artesunate
Component | IV | IM |
Artesunate Powder (mg) | 60mg | 60mg |
Sodium Bicarbonate (mls, 5%) | 1ml | 1ml |
Normal Saline or 5% Dextrose (mls) | 5mls | 2mls |
Artesunate Concentration (mg/ml) | 10mg/ml | 20mg/ml |
Note:
After 24 hours of artesunate administration, if the child can eat and drink, transition to a full course of artemisinin combination therapy (ACT), typically the first-line oral anti-malarial, Artemether Lumefantrine.
Quinine for Severe Malaria
For Intravenous (IV) Infusion:
For Intramuscular (IM) Quinine:
Artemether for Severe Malaria
Admit or refer patients with:
Treatment for Severe Malaria in Children with Very Severe Febrile Disease:
For Pre-referral Treatment:
Check available pre-referral treatment options (rectal artesunate suppositories, artesunate injection, or quinine).
If rectal artesunate suppository is available: Insert the first dose and urgently refer the child.
If intramuscular artesunate or quinine is available: Administer the first dose and urgently refer the child to the hospital.
If Referral is Not Possible:
For Artesunate Injection:
For Artesunate Suppository:
For Quinine:
Age or Weight | Rectal Artesunate Suppository (50 mg suppositories, Dosage 10 mg/kg) | Rectal Artesunate Suppository(200 mg suppositories, Dosage 10 mg/kg) | Intramuscular Artesunate(60 mg vial, 20mg/ml, 2.4 mg/kg) | Intramuscular Quinine (150 mg/ml, in 2 ml ampoules)* | Intramuscular Quinine (300 mg/ml, in 2 ml ampoules)* |
2 – 4 months (4 – <6 kg) | 1 | 1/2 ml | 0.4 ml | 0.2 ml | |
4 – 12 months (6 – <10 kg) | 2 | 1 ml | 0.6 ml | 0.3 ml | |
12 months – 2 years (10 – <12 kg) | 2 | 1.5 ml | 0.8 ml | 0.4 ml | |
2 – 3 years (12 – <14 kg) | 3 | 1 | 1.5 ml | 1.0 ml | 0.5 ml |
3 – 5 years (14 – 19 kg) | 3 | 1 | 2 ml | 1.2 ml | 0.6 ml |
*Note: Dosages are given in milliliters (ml) and milligrams per kilogram (mg/kg) based on the child’s weight or age.
GIVE PARACETAMOL FOR HIGH FEVER >38.5°c OR EAR PAIN
Paracetamol for Fever or Ear Pain:
AGE or WEIGHT | Paracetamol Tablet (100 mg) | Paracetamol Tablet (500 mg) |
2 months up to 3 years (4 – <14 kg) | 1/4 tablet every 6 hours | Not applicable |
3 years up to 5 years (14 – <19 kg) | 1/2 tablet every 6 hours | 1/2 tablet every 6 hours |
Give Diazepam to Stop Convulsions
If convulsions have not stopped after 10 minutes, repeat diazepam dose.
Diazepam Dosage
Age or Weight | Diazepam 10mg/2mls Dosage |
2 months – 6 months (5 – 7 kg) | 0.5 ml |
6 months – 12 months (7 – <10 kg) | 1.0 ml |
12 months – 3 years (10 – <14 kg) | 1.5 ml |
3 years – 5 years (14-19 kg) | 2.0 ml |
Note: Dosages are given in milliliters (ml) based on the child’s weight or age.
**For measles, persistent diarrhea, severe malnutrition ****
Age Range | 200,000 IU Capsule | 100,000 IU Capsule | 50,000 IU Capsule |
Up to 6 months | Not applicable | 1/2 capsule | 1 capsule |
6 months up to 12 months | 1/2 capsule | 1 capsule | 2 capsules |
12 months up to 5 years | 1 capsule | 2 capsules | 4 capsules |
For anemia***
Iron and Folate Administration Guidelines
Iron/Folate Tablet Dosage Based on Age or Weight
Age or Weight | Ferrous Sulfate 200 mg + 250 mcg Folate | Iron Tablet (200 mg) | Folic Acid Tablet (5 mg) |
2 up to 4 months (4 – 6 kg) | – | 1/4 | 1/2 |
4 up to 12 months (6 – 10 kg) | – | 1/4 | 1 |
12 months up to 3 years(10 – 14 kg) | 1/2 tablet | 1/2 | 1 |
3 years up to 5 years(14 – 19 kg) | 1/2 tablet | 1/2 | 1 |
**Zinc Sulphate Administration for Diarrhea:
Age | Zinc Sulphate Dispersible Tablet (20 mg) |
0 months up to 6 months | 1/2* |
6 months up to 5 years | 1 |
*Dispose the other half tablet of Zinc Sulphate 20mg
Deworm**
Give mebendazole if:
Treat the Child to Prevent Low Blood Sugar
If the child is able to breastfeed:
If the child is not able to breastfeed but is able to swallow:
If neither of these is available, give sugar water*.
If the child is not able to swallow:
If no nasogastric tube is available, give 1 teaspoon of sugar moistened with 1-2 drops of water sublingually and repeat doses every 20 minutes to prevent relapse.
* To make sugar water: Dissolve 4 level teaspoons of sugar (20 grams) in a 200-ml cup of clean water.
Clean both eyes 3 times daily:
Wash hands.
Apply tetracycline eye ointment in both eyes 4 times daily:
* Quinolone ear drops may include ciprofloxacin, norfloxacin, or ofloxacin.
Soothe the throat, relieve the cough with a safe remedy.
Safe remedies to recommend:
Give these treatments only in the clinic.

GIVE EXTRA FLUID FOR DIARRHOEA AND CONTINUE FEEDING
Counsel the mother on the 4 Rules of Home Treatment:
1. Give Extra Fluid (Give ORS and other Fluids- as much as the child will take)
ADVISE THE MOTHER
Age Group | Fluid Amount after Each Loose Stool |
Up to 2 years | 50 to 100 ml |
2 years or more | 100 to 200 ml |
Advise the mother/caregiver to:
2. Give Zinc (age 2 months up to 5 years)
Tell the mother how much zinc to give (20 mg tab):
Age Group | Zinc Dosage |
2 months up to 6 months | 1/2 tablet daily for 14 days |
6 months or more | 1 tablet daily for 14 days |
Show the mother how to give zinc supplements:
3. Continue Feeding
4. When to Return
Give in the clinic recommended amount of ORS over 4-hr period:
1. DETERMINE THE AMOUNT OF ORS TO GIVE DURING THE FIRST 4 HRS:
WEIGHT | AGE (Use when weight is unknown) | Amount of ORS (in ml) |
< 6 kg | Up to 4 months | 200 – 450 |
6 – <10 kg | 4 months up to 12 months | 450 – 800 |
10 – <12 kg | 12 months up to 2 years | 800 – 960 |
12 – 19 kg | 2 years up to 5 years | 960 – 1600 |
Use the child’s age only when you do not know the weight. The approximate amount of ORS required (in ml) can also be calculated by multiplying the child’s weight (in kg) times 75.
2. SHOW THE MOTHER HOW TO GIVE ORS SOLUTION.
3. AFTER 4 HOURS:
4. IF THE MOTHER MUST LEAVE BEFORE COMPLETING TREATMENT:
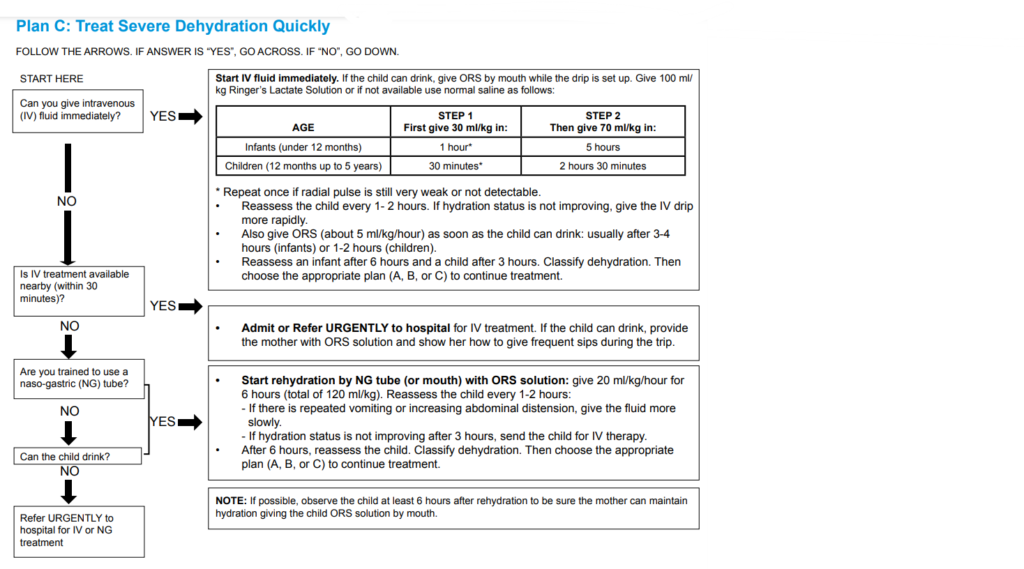
Can you give IV fluids?
Start IV fluid immediately. If the child can drink, give ORS by mouth while the drip is set up. Give 100 ml/kg Ringer’s Lactate Solution or, if not available, use normal saline as follows:
AGE | STEP 1 (First give 30 ml/kg in:) | STEP 2 (Then give 70 ml/kg in:) |
Infants (under 12 months) | 1 hour* | 5 hours |
Children (12 months up to 5 years) | 30 minutes* | 2 hours 30 minutes |
*Repeat once if the radial pulse is still very weak or not detectable.
If NO
Is IV treatment available nearby (within 30 minutes)?
Admit or Refer URGENTLY to hospital for IV treatment. If the child can drink, provide the mother with ORS solution and show her how to give frequent sips during the trip.
Are you trained to use a naso-gastric (NG) tube?
Start rehydration by NG tube (or mouth) with ORS solution: give 20 ml/kg/hour for 6 hours (total of 120 ml/kg). Reassess the child every 1-2 hours:
Can the child drink?
Start rehydration by NG tube (or mouth) with ORS solution:
Then refer URGENTLY to the hospital for IV or NGT rehydration.
Treating Shock
If PNEUMONIA
Follow up after 2 days.
In case of any problem, classify & treat or refer URGENTLY.
If PERSISTENT DIARRHEA
Follow up after 5 days.
In case of any problem, classify, treat & or refer URGENTLY.
If DYSENTERY
Follow up after 2 days.
Assess for persistence of the problem, establish any new problem, classify, treat or refer URGENTLY.
If MALARIA
If fever persists after 2 days or returns after 14 days, then follow up is necessary.
If MEASLES
Follow up after 2 days.
If EAR INFECTION
Follow up after 5 days.
If FEEDING PROBLEM
Follow up after 5 days.
If PALLOR
Follow up after 14 days.
If VERY LOW WEIGHT
Follow up after 30 days.
IF ANY MORE FOLLOW VISITS ARE NEEDED BASED ON THE INITIAL VISIT OR CURRENT VISIT, ADVISE THE MOTHER OF THE NEXT FOLLOW UP VISIT. ALSO, ADVISE THE MOTHER WHEN TO RETURN IMMEDIATELY.
FOOD
Ask!
Does the child take any other foods or fluids?
During the illness has the child’s feeding changed? If yes. How?
FEEDING RECOMMENDATIONS DURING SICKNESS AND HEALTH FOR CHILDREN UP TO 6 MONTHS OF AGE
6-12 MONTHS OF AGE
12 MONTHS – 2 YEARS OF AGE
2 YEARS OF AGE AND OLDER
COUNSEL THE MOTHER ABOUT FEEDING PROBLEMS
If the child is less than 6 months of age and is taking other milk or foods:
Follow up : If the child has
Condition | Follow-up |
Pneumonia, dysentery, malaria, measles | 2 days |
Persistent diarrhea, acute/chronic ear infection, feeding problem, any other not improving | 5 days |
Pallor | 14 days |
Very low weight for age | 30 days |
Advise on when to return immediately
Any sick child | -not able to drink or breastfeed -becomes sicker -develops a fever |
If child has no pneumonia: cough or cold, return if | -fast breathing -difficult breathing |
If child has diarrhea: return if | -blood in stool Drinks or breastfeeds poorly |
Counsel the mother about her own health
TREAT THE CHILD in IMCI Read More »
Javascript not detected. Javascript required for this site to function. Please enable it in your browser settings and refresh this page.