Injuries and Trauma
FRACTURE
A fracture is a break in the continuity of a bone. Any injury involving a bone should be considered a fracture until proved otherwise.
CAUSES OF FRACTURE
- A fracture can be caused by direct force. This is when the injury occurs at the site where the forces have been applied e.g. blow, accident
- Indirect force. For this case, the bone breaks a distance from where the force is applied. This means that the force is transmitted an example is fall from a tree.
- Strong muscular action, this is common with the patella bone.
- Stress i.e. repetitive force
- Fracture may also be caused by bone diseases ( pathological) responsible diseases e.g.
- Osteomyelitis
- Tuberculosis of bones
- Cancer
- Old age
- Bone tumors.
Classification by Fracture Location
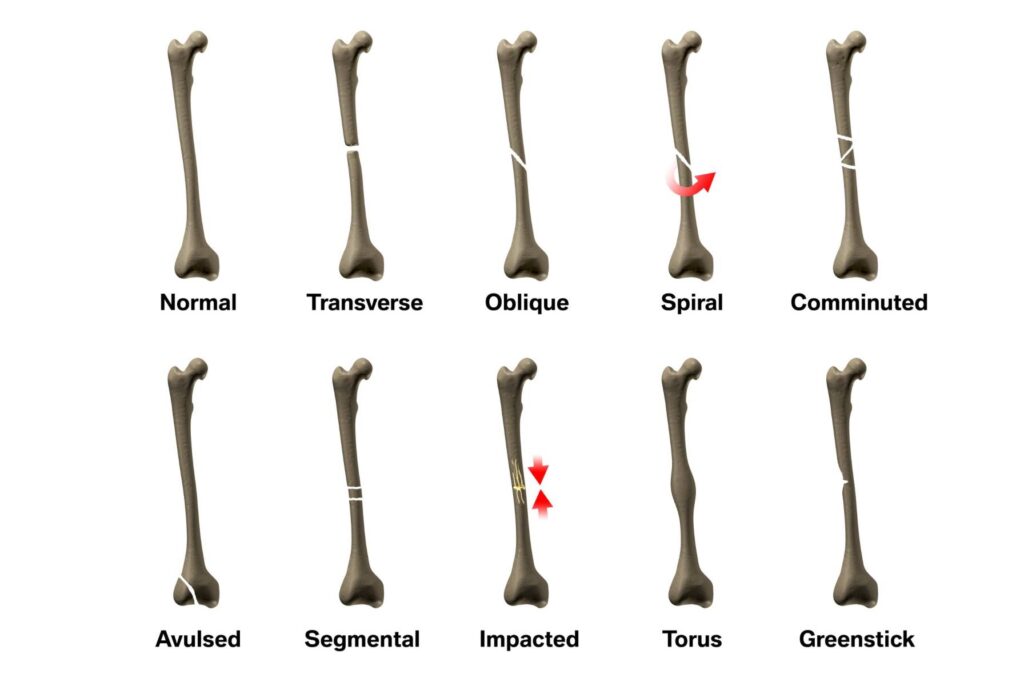
TYPES OF FRACTURES
- SIMPLE OR CLOSED FRACTURE : This is fracture in which the bone is broken but the skin remains intact. A simple fracture can become complicated if not handled properly.
- COMPOUND OR OPEN FRACTURE : This is when there is a wound associated with the fracture sometimes the wound is caused by a protruding piece of broken bone. This may be associated with extensive blood loss.
- COMPLICATED FRACTURES: This may be open or closed but there may be injury to internal or surrounding structures. It could be the lungs incase of fracture of the ribs etc.
- COMMUNITED FRACTURES: In this type of fracture, the bone is broken into several pieces.
- IMPACTED FRACTURES: Here the broken bone enters into each other.
- DEPRESSED FRACTURE: The broken parts are pushed in wards.
- GREENSTICK FRACTURE: Is where the bone is cracked or bent. It’s common in children because their bones are still soft.
GENERAL SIGNS
- There is pain and tenderness at the site.
- There is difficulty in movement.
- There is swelling and oedema
- Deformity.
- Discoloration
- Loss of function
- There may be unnatural or abnormal movement of the affected part.
- Crepitating (grating sound) if limb is moved gently.
- The patient may also go into shock.
- Warmth due to increased blood supply
AIMS OF FIRST AID
- To prevent further damage of the fracture.
- To prevent pain or reduce.
- To make the patient as comfortable as possible as you wait for expertise.
- To prevent shock.
RULES FOR TREATMENT OF FRACTURES
- Do not remove the affected part if not in danger.
- Steady and support the injured part at once and prevent movement.
- Reassure your casualty and send for medical aid
- Stop bleeding if any.
- Cover any wound with a sterile dressing.
- Do not remove the casualty’s clothes unnecessarily.
- Try to prevent/ counter act shock. This is by handling the casualty gently, keeping him warm, and give sweeter fluids incase if there is no possibility of anaesthia.
GENERAL MANAGEMENT OF A CASUALTY WHO HAS SUSTAINED A FRACTURE.
- Prevent rubbing of the broken bones by immobilization and keeping the pieces of broken bones together.
- Re – assure the patient.
- Ensure the clear air way.
- Stop hemorrhage if any.
- Treat shock
- Relieve pain
- Immobilize the fracture using splints and apply a sling.
- Do not move the injured part unnecessarily.
FRACTURE HEALING
FACTORS THAT IMPEDE BONE HEALING
- Excessive motion of fracture fragments
- Poor approximation of fracture fragments-inaccurate reduction-excessive bone loss during fracture.
- Compromised blood supply-damage to blood vessel-muscular injury-
- Excessive edema at fracture
- Infection at fracture site.
- Metabolic disorders or diseases (cancer, diabetes, malnutrition)-they retard osteogenesis.
- Soft tissue injury-disrupts blood supply.
- Medication use e.g. steroids, anticoagulants. Steroids can cause osteoporosis and long term use of heparin also causes the same.
COMPLICATION OF FRACTURES
- General-blood loss, deep vein thrombosis, pulmonary embolism, respiratory distress
- Early complication- infection, septicemia, plaster sores.
- Late complication-joint instability, osteoarthritis, mal union, delayed union, non union.
MANAGEMENT OF SPECIFIC FRACTURES
- FRACTURE OF THE SKULL.
This fracture may be associated with injuries to the spinal cord and to the brain. Fracture may also be associated with condition like concussion.
Concussion is the shaking of the brain leading loss of consciousness. It may also be due to compression and hence also leading to the (compression/pressure) on brain. Patient may bleed from the nose or ears and the casualty may be unconscious.
SIGNS AND SYMPTOMS
- There may be history of an accident
- Bleeding from the skull.
- Pupils may be unequal, dilated.
- Partial unconsciousness
- Vomiting may be there
- Pulse rate is slow.
- There might be paralysis of the limb.
- Eye movements may also be disturbed
- Speech disorders.
MANAGEMENT
- A person who has sustained a head injury should be carefully watched and arranged to send to the doctor as soon as possible.
- Patient should be nursed in a spine position with head turned to one side and shoulders slightly elevated if conscious
- If there is bleeding as discharge from ear then the head should be turned to the side of the bleeding ear. But do not plug the ear.
- Patient should be kept quite. Nurse him/her in a quite environment.
- In case of any wound, dress it
- If unconscious, change to recovery position check breathing, pulse, level of response and record.
FRACTURE OF THE SPINE
- The danger of this type of fracture is injury with the spinal cord.
- You treat shock as you make arrangements to transport the patient.
- You tie the legs together
- You put padding between the knees and thighs so that they are not touching directly
- You need four people to lift this patient
- You should avoid bending or twisting of the spine.
- The best position for transporting this person is recumbent position.
- The patient is transported by stretcher with hard surface.
FRACTURE OF THE RIBS
The broken ribs may be pushed inwards making the fracture to be complicated.
- The patient will complain of local pain.
- It is worsened by breathing, severing.
- The fractured end may manage the underlying part which may lead to blood stained sputum.
- If the rib has pieced the lungs, the patient may have shallow respiration.
- Patient may have signs of internal bleeding
- Air may escape to the plural cavity or escape to tissues and may lead to lung collapse.
If the air finds its ways to the tissues, we talk of a condition known as Emphysema.
IF THE PATIENT PRESENT WITH THIS;
- Make the patient sit.
- Restrict chest movement by applying broad bandages and fix on the opposite side.
- Support the arm using a sling.
- If there is an open wound, cover it, immediately to keep out air.
- You can lay, lean patient on the affected side
- Support the patient using pillows.
- Transfer the patient to hospital.
FRACTURE OF THE CLAVICLE
This usually occurs due to indirect pressure like falling on an out stretched arm.
TREATMENT
- Support the arm of the injured.
- Put padding in the axilla.
- Tie the arm to the chest using abroad bandage.
- Alternatively support with a sling.
FRACTURE OF THE UPPER ARM
- The humerus may be fractured at a part close to the shoulder.
- The fracture may be at the shaft or it may be towards the elbow.
- Sometimes the lower end of the radius may be broken.
- Sometimes the person sustains the fracture of metacarpal bones. This may be associated with bleeding into the palms of the hand.
MANAGEMENT
- The limb must be immobilized
- If the elbow can comfortably bend without increasing the pain, flex the arm against the chest with the fingers touching the opposite shoulder.
- Put padding between the limb and chest and fix it with a collar sling.
- Bind the arm firmly to chest.
- If the elbow can’t be bent without causing pain, tie the limb to the trunk. And again fix with broad bandages.
- Alternatively, a splint may be used to fix the limb. Transport the patient in any position that he/she is comfortable in.
FRACTURE OF THE FORE ARM (ULNA, RADIUS)
- For this, you ask the casualty to sit. Place the arm on the/ across the chest with the thumbs upper most.
- Use a padded splint which is applied to the front from the elbow up to the fingers.
- Fix it with bandages.
- Support the arm with a sling with fingers upper most.
- Watch the fingers for signs of interference with circulation.
FRACTURE OF THE PELVIS
These usually occur due to indirect force. It may be a car accident, falling from height.
A fracture pelvis may be complicated due to injury of the urinary bladder system.
SIGNS AND SYMPTOMS
History of injury
- Patient unable to stand
- Pain may be in hips, back.
- Pain increase with movement
- Difficulty and pain in passing urine.
- Sometimes the urine is stained.
- May have desire of passing urine but he finds it difficult. And the patient may present shock signs.
MANAGEMENT
- Help the patient lie down with the head lower than the rest of the body
- Keep the legs straight or the patient can bent the knees slightly and they should be supported in the position.
- Abroad bandage can be applied around the pelvis
- But you still put pads between legs and ankles and tie legs safely.
- The patient is lifted onto the stretcher with the pelvis supported.
FRACTURE OF THE FEMUR
The femur is the longest bone in the body. And it has every rich blood supply. A fracture of the neck of the femur is common in the elderly but it can affect any part of the femur.
SIGNS AND SYMPTOMS
- Severe pain
- Shortening of the bone
- And the foot may be turned out upwards.
- Patient may go into shock because of pain.
- The broken bone ends may piece blood vessels leading to blood loss.
TREATMENT
- Help the casualty to lie down as you support the injured limb.
- Treat shock if any.
- Immobilize the limb as follows,
- Tie together the knees, the hips and above and below the site of the fracture.
- Re-assure the casualty.
- Arrange for transport to hospital.
If the distance to the hospital is long, do the following.
- Apply a padded splint from the axilla down to the foot on the outside and put a short splint that starts from the groin (between the legs) up to the foot so that you maintain the injured part.
- Tie with a number of bandages.
- First bandage across the chest.
- Second bandage a cross the pelvis
- Third above the fracture
- Fourth under the fracture
- Fifth fix the knees.
- Sixth bandage fixes the ankles.
In some cases there is a splint known as THOMAS SPLINT
Then after, you can transport the patient.
DISLOCATION
Is a displacement of the bones which form a joint. The most commonly affected joints are the shoulder joints, elbow joints, lower jaw.
SIGNS AND SYMPTOMS
- Severe pain at the sight of the injury.
- Movement is restricted at the joint.
- Deformity of the limb.
- Swelling may set in especially if there is collection of blood.
TREATMENT
- Support the limb in the most comfortable position.
- Relieve pain and refer the patient to hospital.
A SPRAIN
This is an injury to the joint associated with tearing of the ligament. It is sometimes associated with injury to the soft tissues which surround the joints. And this could be a tendon.
SIGNS AND SYMPTOMS
- Severe pains at first but reduce slowly.
- Swelling
- Bruising which is due to collection of blood at the site.
- Loss of movement.
TREATMENT
- You can place the limb in a comfortable position.
- Apply a firm bandages.
- Apply cold compress to reduce on swelling.
- Gently massage the muscle above the sprain.
- Encourage the patient to try to move the joint
- Then advise him to go to hospital to rule other injuries.
STRAIN
This is an injury to a muscle or tendon when it’s forcefully stretched beyond its proper length. It is sometimes associated with tearing of muscle fibers.
SIGNS AND SYMPTOMS
- The patient will complain of sudden sharp pain at the site of pain.
- The pain is worsened by movement
- Swelling
- Loss of power.
TREATMENT
- Place the patient in a comfortable position
- Apply bandage or plaster to the affected part.
- In case of a fracture, you immobilize.
STITCH
It is a painful spasm of diaphragm. It usually occurs during games or running.
Treatment
- Rest
- If not relieved by rest, give sips of hot water and rub the affected area.
BITES AND STINGS
Many insect stings cause irritation, swelling, pain and some are poisonous. Bites from sharp pointed teeth cause deep puncture wounds which can damage tissues and introduce germs. Some of them might crash the tissues. Any bite that breaks the skin needs prompt first aid because it increases the risk of infection.
SNAKE BITES
These can cause punctured wounds. The wound may not be serious but it’s important to determine whether it’s poisonous or not.
SIGNS AND SYMPTOMS
- The wound may be visible.
- The patient may show signs of poisoning like bleeding, paralysis of affected limb.
- Signs of shock may be present.
- Pulse may be weak and rapid.
- Visual disturbance.
- They may have nausea and vomiting
- Small punctures may appear at the sight which is painful.
- Swelling.
- Breathing may become difficult or may completely fail.
- Patient may start sweating.
- He/she may become unconscious.
TREATMENT FOR SNAKE BITES.
- Tie a piece of cloth or tourniquet.
- It’s tied above the site to prevent venous blood return
- It should be tight enough so that blood can’t flow through vein but not too tight to obstruct arterial flow.
- This tourniquet should be loosen every after 10- 20 minutes
- Keep the bitten limbs hanging.
- Re – assure the patient.
- Keep the patient warm
- Ensure rest.
- Examine the wounds for any marks.
- If there are marks, people think it is not poisonous and if no marks, it is poisonous.
- Try to get to hospital immediately.
- And this patient should be given an anti – venom injection.
- If you are not able to get the patient to hospital immediately, you can do the following:
- Wash the wound with lukewarm water.
- You can add potassium permanganate if it is available.
- Get sterilized knife or a new razor blade, make a cut across the site about 1cm, put a cloth and suck out the poison and spit it out.
- Apply a clean dressing.
- Treat shock
- Refer to the nearest hospital.
- If breathing fails, start artificial respiration continue monitoring vital signs as you wait for transport.
SCORPION BITE
Scorpion bites or stings or bites from other insects like spiders, mosquitoes etc. can cause serious illness and may be fatal if not treated promptly. A scorpion sting is poisonous so if it bites a person who is weak, it may produce serious results.
SIGNS AND SYMPTOMS
- Severe pain at the site.
- Sweating
- Swelling
- In case of children, the children may get convulsion.
TREATMENT
- Reassure the casualty.
- If the sting is visible, scrap it or brush it a way.
- Raise the broken part if applicable.
- Apply a cold compress.
- Treat for shock.
- Give a hot drink and keep the patient warm.
- If the pain and swelling persist and the patient shows signs of shock, advise him to seek medical advice
- Keep monitoring the vital signs.
- Check out for allergic reactions like wheezing.
STINGS FOR BEES AND WASPS.
- These stings occur quite often in rural areas especially if their nests are disturbed.
- These are very painful but not that dangerous. However, if bitten by many insects (bees).
- They have a sting which is left at the site and it should be removed.
- If the person bitten is prone to allergies, then it may cause serious effect or condition because he/she may go into shock.
- A sting in the mouth or throat is dangerous because the swelling can obstruct the air way.
- Multiple insect bites cause/ produce serious reaction.
SIGNS AND SYMPTOMS
- Pain at the site.
- Swelling
- Discoloration of the skin.
FIRST AID TREATMENT
- Remove the sting using your finger, brush, or pair of forceps.
- Re – assure the casualty.
- Elevate the affected part if possible.
- Apply a cold compress and keep it in position for at least 10 minutes.
- Monitor the vital signs.
- Treat shock.
- Watch out for signs of allergic reaction.
- Advise the patient or casualty to seek medical advice.
- If the pain persists.
WOUNDS
A wound is a break or tears in the continuity of the skin.
Wounds can be classified into different types depending on the cause and appearance. And each type has specific risks associated with the surrounding tissue damage.
TYPES OF WOUNDS
- AN INCISED WOUND: Its clean cut wound. It’s usually caused by a sharp object like a razor blade, knife. It has straight edges. And it’s usually accompanied by profuse bleeding because blood vessels are cut across. Surrounding structures like the tendons and nerves may be injured.
- LACERATED WOUNDS (TORN WOUND): They are caused by blunt instruments. These wounds do not bleed much but more tissues may be damaged and this type of wound is more prone to infection.
- CONTUSED (BRUISED) WOUND: This can be caused by falling down on something that is blunt leaving bruises on the surrounding tissue. The capillaries beneath the skin may rapture and blood may leak into the tissues. And this will result into color change. If the injury is severe, there may be damage to the underlying structure.
This patient may present with the following:
- Pain and swelling.
- There are may be discoloration at the site of injury.
The aim of treatment is to reduce blood flow by cooling and gentle compression.
MANAGEMENT
- Raise and support the injured part in the most comfortable position for the patients.
- Then apply a cold compress to restrict the bleeding
- If you are in doubt about the severity of the injury, refer for medical aid.
- PUNCTURED (STAB) WOUNDS: These are caused by sharp pointed instrument e.g. knife, needle, bullet or anything that penetrates into tissues. They tend to cause internal bleed which is dangerous. It can also introduce germs into the bottom of the wound. There is a danger of injury to the internal organs (structure).
The patient may present with following (signs and symptoms)
- T here might be a wound.
- There is some bleeding which may not be much.
- Shock may be there or not.
FIRST AID
- Handle the injured patient gently as possible.
- Seat/ lay the patient and raise the injured part.
- Stop bleeding.
- Do not disturb any formed clot.
- If the wound is too big, it requires suturing, just apply a dressing and transfer to hospital.
- If it’s a limb, immobilize to prevent unnecessary movements.
- All punctured wounds of the chest and abdomen must be referred to hospital for the doctor to see.
In case of a small wound
- Seat or lay the patient down handle the injured part with water and soap.
- Clean the injured part with water and soap.
- Stop bleeding using direct pressure.
- If it is small wound, apply an antibiotic ointment and cover with a clean dressing.
- GUNSHOT WOUNDS: These tend to have a small entry and a big exit. As the missile passes through the body, it may damage internal organs tissues and even some blood vessels. In addition to the external bleeding, there is also internal bleeding the deeper the wound, the more are the chances of becoming infected. Aim of treatment is to stop bleeding and to prevent infection.
6. PENETRATING CHEST WOUNDS: The rib cage protects not only the lungs, the heart and blood vessels above the diaphragm but it also protects the liver and the spleen below the diaphragm in the upper abdominal cavity. A wound to the front or back of the chest penetrating into the chest allows air to enter the space occupied by the lungs and this will interfere with bleeding and the lungs on the affected side collapses.
Air in the chest cavity interferes with functions of the sound lung and sometimes the function of the heart is affected. If the wound is not the left lower part of the chest, it may penetrate into the abdominal cavity causing severe hemorrhage.
SIGNS AND SYMPTOMS
- The casualty may complaint of chest pain.
- Difficulty in breathing
- Breathing is narrow.
- Cyanosis may be present indicating lack of oxygen.
- A patient may cough up bright red frothy blood
- Funny noise may be heard as the patient breathes in.
- The patient may have signs and symptoms of shock.
AIM OF TREATMENT
To ease breathing by sealing off the wound immediately.
- Arrange agent transfer to hospital.
- Place the patient in a half sitting position with the head and shoulder supported.
- Turn the body to the injured or affected side.
- Gently cover the wound with a sterile dressing as soon as possible.
- Form an air tight seal. It can be plastic cover.
- Support the arm with a sling and make the patient as comfortable as possible.
- Watch out for signs of internal bleeding.
- If the casualty becomes unconscious, ensure a clear airway, place in a recovery position with the injured part. Upper most and keep checking breathing.
- Arrange for urgent remove to hospital.
- BED SORE WOUND: Caused by being confined in bed with poor nursing care. It results from bed sore to bed sore wound. When micro organisms invade any of the above wounds, sepsis (pus formation) will occur, and the wound will be dirty and when these micro organisms are destroyed by the use of antiseptics or disinfectants e.g. hibitane, hydrogen peroxide then the wound will be clean.
- ABRASSION: Is caused by tying round a string in a part of the body and it causes a peel of tissues.
Signs and symptoms
- Is easily seen
- Bleeding- external or internal
- Pain.
- Swelling can occur.
- There can be sweating.
- Hot and tender.
- Increased blood supply to the site.
Many wounds do not bleed very much and this slight bleeding may soon stop on its own as clot forms. The process of arresting hemorrhage can be helped by giving the following management.
- It is better to wash your hands before dealing with the wound. If the wound is dirty, wash it under running water.
- Protect the wound with sterile swab and carefully clean the surrounding area with soap and water.
- Gently wipe away from the wound. Do not take off any clot which is forming. You should use each swab once only if the bleeding continues.
- Apply direct pressure on the wound using the sterile swab.
- Dress small wounds with adhesive dressing while larger ones with addressing pad and bandage.
- Raise and support the bleeding part unless you suspect a fracture.
- If you do not achieve the objective or you have doubts about the injury seek medical help.
- Eye wounds: All eye injuries can be serious, even the smallest injury on the eye can affect the cornea. It can also lead to infection with deterioration of the eye sight and even permanent blindness. The cut may be bruised or cut by direct broken fragments, metallic materials, pieces of stone or broken glasses.
Signs and symptoms
- Patient may complaint of partial or total loss of vision of the affected eye.
- The eye might appear red; there may be a visible wound.
- Blood may be seen or a clear wound on the eye.
- The shape of eye ball may have become flat.
The aim of treatment is to protect the eye by preventing the movement and seeking medical aid.
Management
- Let the casualty lie on the back and keep it as still as possible.
- Do not attempt to remove any foreign body which is embedded.
- Ask the casualty to close the injured eye and cover it with an eye pad or clean dressing then secure the dressing with a bandage or plaster.
- Advise the casualty not to move the good eye.
- It may be necessary to cover both eyes and re-assure the patient.
- Arrange to transfer the casualty to hospital maintaining the treatment position.
10.Wounds which occur in the hand palms: These wounds can occur when a person handles or touches broken pieces of glass, broken objects and cut. Or: If a person falls putting hands on something sharp. These wounds tend to bleed profusely. It can be associated to a fracture. If the wound is deep, some nerves tendons might be affected.
Signs and symptoms
- Pain at the sight of the wound
- Bleeding which is sometimes profuse.
- Loss of sensation, this is because nerves have been injured
Management
Aim
- To control bleeding
- Make arrangement to transfer the patient without disturbing any foreign body.
- To control bleeding, you place a sterile dressing over the wound and apply pressure.
- Elevate the injured part; put it above the level of the heart.
- Encourage the patient to maintain the pressure if the casualty can do it him or himself.
- You can also use bandage to support the casualty.
- Support the arm with sling as the casualty is being transferred to hospital
- ABDOMINAL WOUNDS: These usually occur due to sharp, instruments, gunshots, or anything that penetrates the abdominal wall. A deep wound is serious because it causes internal or external bleeding. But also it might have caused injury to the internal structures. If it has caused internal damage, this may cause severe internal bleeding.
Signs and symptoms
- Patient may complaint of general abdominal pain.
- Bleeding might be there.
- There might be a wound which may appear small.
- Sometimes part of the intestine is visible.
- The casualty may be vomiting.
- He/she may have signs of shock
AIM:
- To protect the wound so that chances of infection are decreased.
- Make arrangements to send the casualty to hospital as quickly as possible.
Management
- Patient lies at the back with knees upwards. This helps in gaping of the wound.
- This position helps to decrease strain on the injured part.
- Knees should be supported in the position.
- Apply a sterile dressing and secure it with a bandage or plaster.
- Prevent or treat shock.
- Do not remove any protruding object in the wound.
- Do not give anything by mouth.
- Check the breathing and pulse every 10 minutes.
- Watch out for any signs of internal bleeding.
- If the casualty coughs or vomits, support the abdomen gently so that the wound is not strained. It also helps to prevent protrusion of the intestines.
- If the casualty becomes unconscious, open airway, check breathing and place her in a recovery position while supporting the abdomen.
- Quickly transfer the patient to hospital maintaining the treatment position.
- Do not touch protruding intestines because you may cause infection. You continue supporting the abdomen during coughing and vomiting.
FACTORS AFFECTING WOUND HEALING
- Type and severity of the wound: The type and extent of the wound play a significant role in the healing process. Different wounds, such as surgical incisions, lacerations, or burns, may have different healing needs.
- Infections: Bacterial or fungal infections can significantly affect the healing process and may require medical intervention, such as antibiotics or antifungal medications.
- Blood supply: An adequate blood supply is essential for wound healing. Blood carries oxygen and nutrients to the wound, promoting cell growth and tissue repair. Poor blood circulation, often associated with conditions like diabetes or peripheral artery disease, can delay healing.
- Chronic conditions: Chronic health conditions like diabetes, autoimmune disorders, and cardiovascular disease can affect wound healing. These conditions can impair the body\’s ability to deliver necessary nutrients and oxygen to the wound site and weaken the immune response.
- Age: Advanced age can slow down the wound healing process. Older individuals may have reduced collagen production, decreased immune function, and other age-related factors that affect wound healing.
- Nutrition: Adequate nutrition is crucial for proper wound healing. A balanced diet rich in protein, vitamins (mainly vitamin C and A), and minerals (such as zinc) supports the body\’s healing processes. Malnutrition or deficiencies in these essential nutrients can impair wound healing.
- Medications: Certain medications, such as corticosteroids or immunosuppressants, can hinder with wound healing. Also, treatments like radiation therapy or chemotherapy may negatively affect the healing process.
- Lifestyle factors: Lifestyle choices, such as smoking or excessive alcohol consumption, can impair wound healing. Smoking, in mainly, reduces blood flow and oxygen delivery to the wound site, hindering the healing process.
- Psychological factors: Psychological stress, anxiety, and depression can influence wound healing. High-stress levels may negatively affect the immune system and slow down the healing process.
- Wound care: Proper wound care is crucial for maximum healing. Factors such as keeping the wound clean, moist, and protected can affect the healing process. Neglecting wound care or using inappropriate wound dressings can affect healing.