Sexually Transmitted Diseases (STDs)/HIV/AIDS
Sexually Transmitted Diseases (STDs)/HIV/AIDS
Sexually Transmitted Diseases are infections which are generally acquired through unprotected sexual intercourse with another person who is infected with particular diseases.
The organisms that cause STDs may pass from person to person in blood, semen, vaginal fluids and other body fluids.
STIs are a collection of disorders, several of which are better regarded as syndromes for more effective management using a syndromic approach. Some infections can also be transmitted from mother to child during pregnancy, childbirth and or lactation, blood transfusion or shared sharps.
Reproductive tract infections (RTIs) are infections of the genital tract. There are three types of RTIs:
- Sexually transmitted infections (STIs): Infections caused by organisms that are passed through sexual activity with an infected partner. More than 40 have been identified, including Chlamydia, gonorrhoea, hepatitis B and C, herpes, HPV, syphilis, trichomoniasis, and HIV.
- Endogenous infections: Infections that result from an overgrowth of organisms normally present in the vagina. These infections are not usually sexually transmitted, and include bacterial vaginosis and candidiasis.
- Iatrogenic infections: Infections introduced into the reproductive tract by a medical procedure such as menstrual regulation, induced abortion, IUD insertion, or childbirth. This can happen if surgical instruments used in the procedure are not properly sterilized, or if an infection is already present in the lower tract.
Classification of Sexually Transmitted Diseases.
S/N | CLASS | CAUSATIVE ORGANISM | DISEASE |
1 | BACTERIAL | Neisseria gonorrhoeae | Gonorrhea |
Chlamydia trachomatis | Chlamydial Infections (trachoma) | ||
Treponema pallidum | Syphilis | ||
Haemophilus ducreyi | Chancroid | ||
2 | VIRAL | HIV | AIDS |
Herpes Simplex | Genital herpes | ||
HPV(Human Papillomavirus) | Genital Warts/Ca. Cx | ||
HBV(Hepatitis B virus) | Hepatitis B | ||
CMV(Cytomegalovirus) | Blindness | ||
Condylomata Acuminata | Genital Warts | ||
3 | FUNGAL | Candida albicans | Vaginal Candidiasis |
Dermatophytes | (Tinea corporis) | ||
4 | PROTOZOAL | Trichomonas vaginalis | Trichomoniasis |
5 | PARASITIC | Pediculosis Pubis | Lice infestation |
Sarcoptes scabiei | Scabies |
Prognostic classification of STDs
S/N | CLASSIFICATION | DISEASE | INFECTIOUS AGENT |
1 | CURABLE(Mostly Bacterial) | Gonorrhea | Neisseria gonorrhoeae |
Syphilis | Treponema pallidum | ||
Chlamydia | Chlamydia trachomatis | ||
Trichomoniasis | Trichomonas vaginalis | ||
2 | INCURABLE(Virus) | HIV/AIDS | Human Immunodeficiency Virus (HIV) |
Hepatitis | Hepatitis viruses | ||
Herpes | Herpes Simplex Virus | ||
Human Papilloma Virus (HPV) | Human Papilloma Virus |
General Pathology
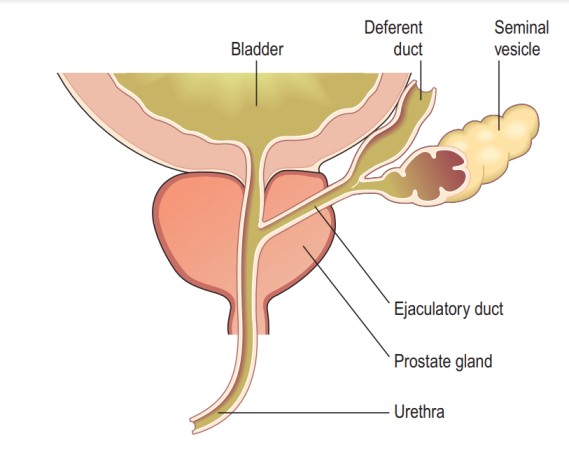
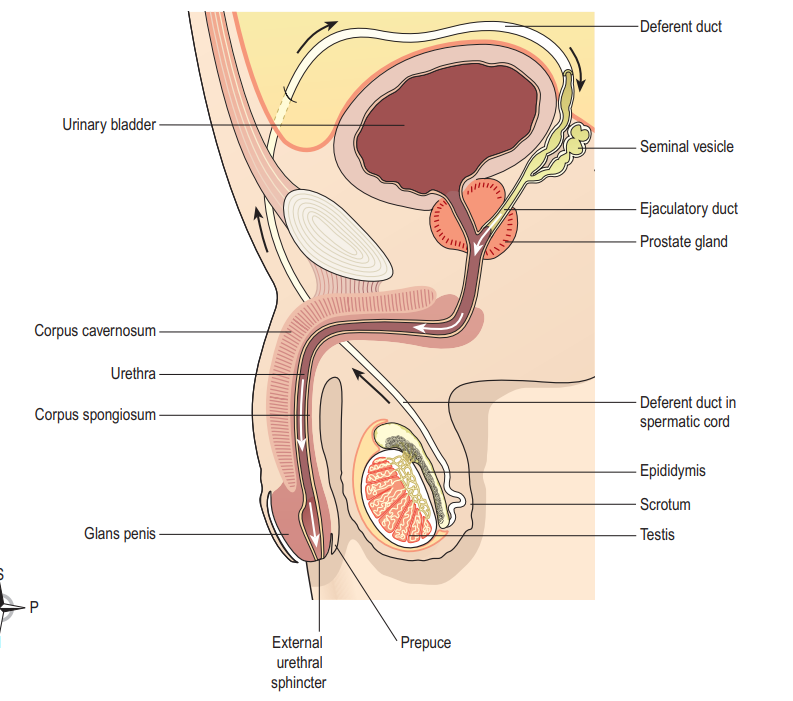
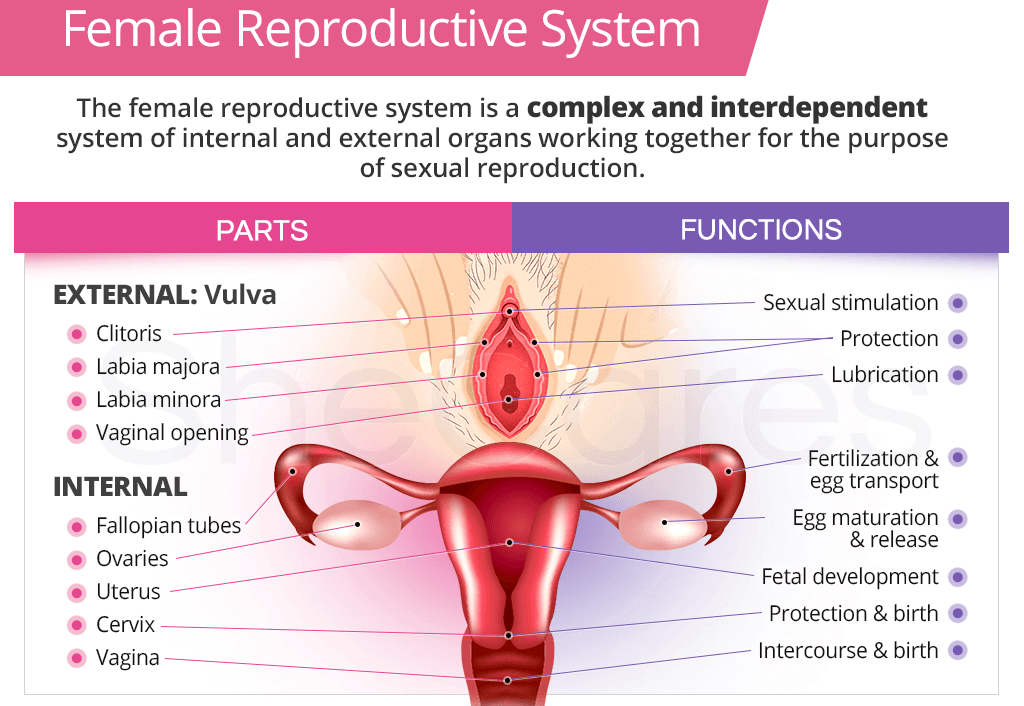
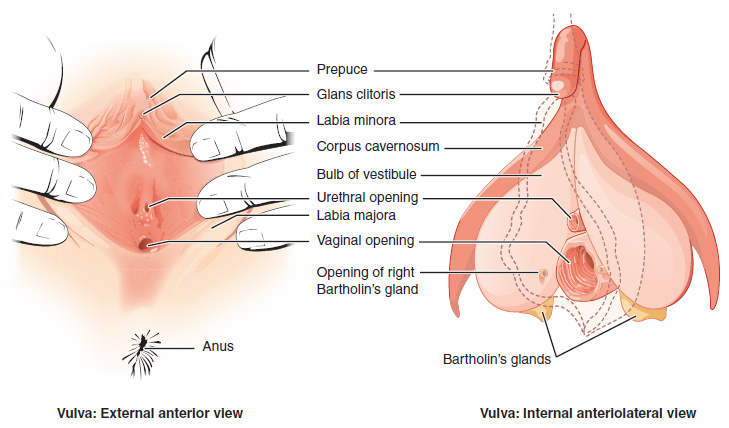
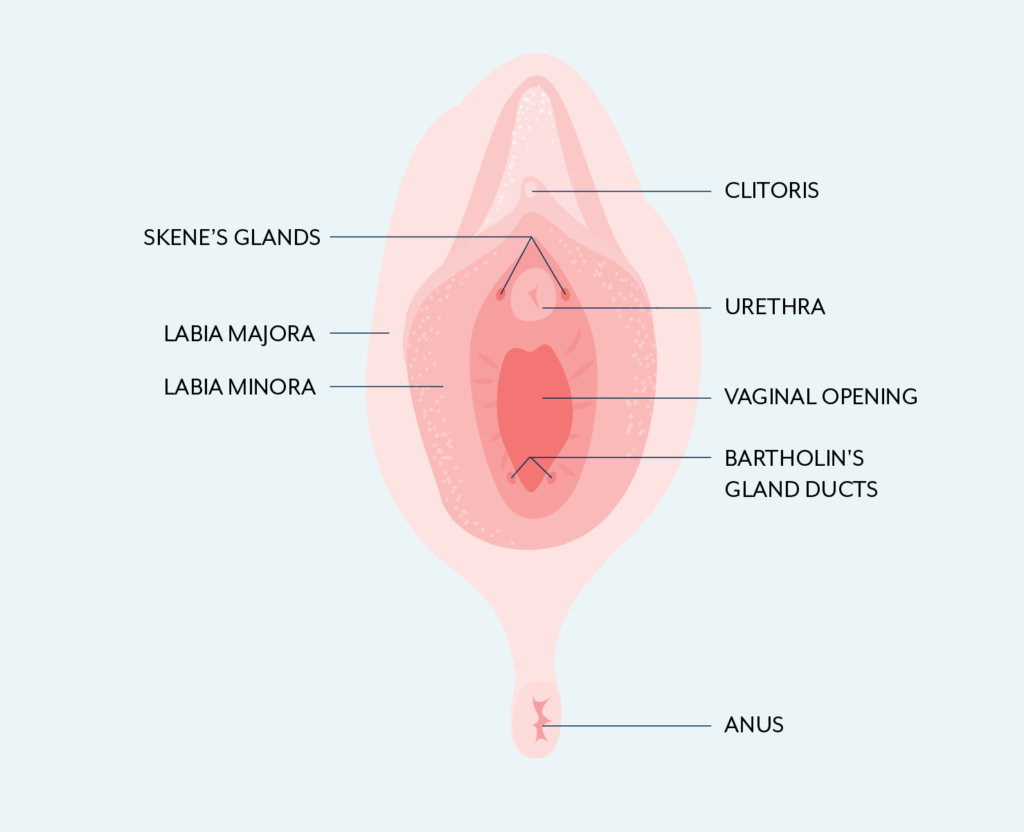
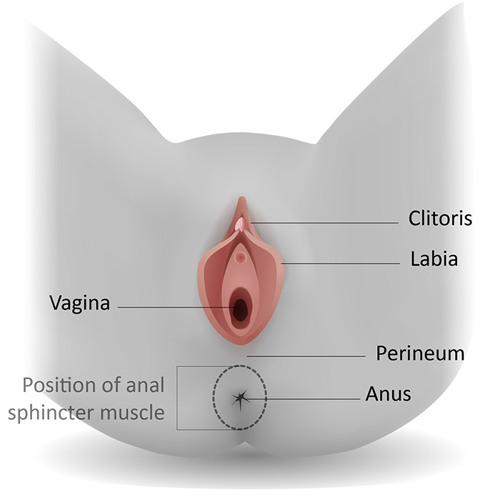
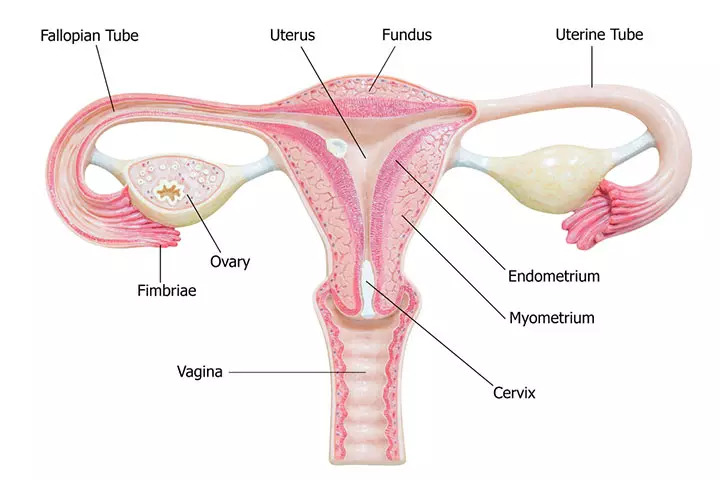
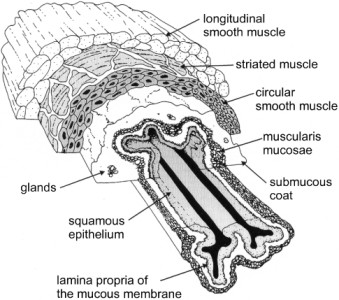
Many sexually transmitted infections (STIs) are more easily transmitted through the mucous membranes found in the penis, vulva, rectum, urinary tract, and, depending on the type of infection, the mouth, throat, respiratory tract, and eyes, though less frequently.
Mucous membranes differ from the skin as they allow certain pathogens into the body, and pathogens can also pass through breaks or abrasions in the skin, even minute ones. The shaft of the penis is particularly susceptible due to the friction caused during penetrative sex.
The primary sources of infection, in ascending order, are venereal fluids, saliva, mucosal or skin (particularly the penis); infections may also be transmitted from faeces, urine, and sweat.
Some infections labelled as STIs can be transmitted by direct skin contact; examples include herpes simplex, pubic lice, and HPV.
Risk Factors for Acquiring STDs
- Unprotected Sexual Intercourse: Engaging in genital or oral penetration without proper condom use significantly increases the risk of acquiring STDs.
- Multiple Sexual Partners: Having sexual contact with multiple partners elevates the risk of contracting sexually transmitted infections (STIs).
- Existing STDs: Being infected with one STI increases vulnerability to others; for example, having herpes, syphilis, gonorrhoea, or chlamydia exposes an individual to a higher risk of contracting HIV.
- Unlawful Sexual Intercourse or Sexual Assault: Forceful acts such as rape or sexual assault expose victims to trauma, making them more susceptible to bacterial and viral infections from penetration.
- Alcohol Abuse: Substance abuse, particularly alcohol, impairs judgement, making individuals more willing to engage in risky sexual behaviours.
- Drug Abuse and Needle Sharing: Needle sharing, associated with drug abuse, spreads serious infections, including HIV, Hepatitis B, and Hepatitis C. Although primarily acquired through injection, these infections can also be transmitted sexually.
- Adolescence: The transitional phase from childhood to adulthood is marked by experimentation and risk-taking behaviours, increasing susceptibility to risky sexual practices and STDs.
- Political Instability: Environments marked by political instability, where rape and forced relationships are common, contribute to a higher risk of acquiring STDs.
- Vertical Transmission: STDs can be transmitted from mother to child during pregnancy or childbirth, for example, HIV, gonorrhoea, chlamydia, and syphilis.
General Control and Prevention of STIs
- Abstinence: The most effective method of avoiding STIs is abstaining from sexual activity.
- Correct and Consistent Condom Use: Proper and consistent use of condoms during sexual activity provides effective protection against STIs.
- Avoidance of Excessive Alcohol and Drug Use: Limiting alcohol consumption and avoiding drug abuse reduces the likelihood of engaging in risky behaviours.
- Vaccination: Early vaccination before sexual exposure is effective in preventing certain STIs, such as HPV and Hepatitis B.
- Mutual Communication and Fidelity: Open communication between partners and mutual faithfulness contribute to safer sexual practices.
- Life Skills Education: Providing education on life skills to young adolescents and those becoming sexually active helps them understand the consequences of early sexual debut.
- Safe Male Circumcision: Male circumcision is associated with a reduced risk of acquiring HIV from infected women and helps prevent the transmission of genital HPV and genital herpes.
Complications of STIs
- Abortion
- Premature labour
- Intrauterine death
- Stillbirth
- Congenital syphilis
- Recurrent genital sores
- Scrotal pain, redness, and swelling
- Infertility
- Pelvic pain
- Hair loss
- Eye infection
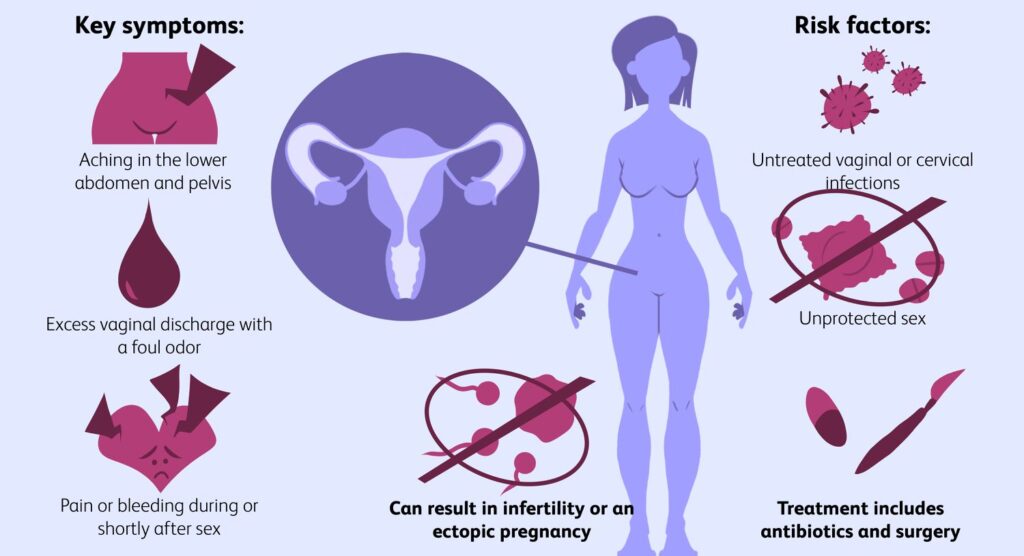
- Pelvic Inflammatory Disease (PID)
- Arthritis
- Divorce
STIs and Pregnancy
STIs can increase maternal risk of:
- Ectopic pregnancy
- Premature delivery
- Miscarriage
- Premature rupture of membranes
- Puerperal sepsis
- Postpartum infection
And risks to the infant of:
- Stillbirth
- Low birth weight
- Conjunctivitis
- Blindness
- Congenital infection
- Pneumonia
- Neonatal sepsis
- Congenital abnormalities
Prevention Strategy
- Advocacy.
- Abstinence, Behavior Change Communication (BCC).
- Safe sex – condom use.
- Counselling, active & prompt treatment of sexual partners.
- Health Education on STI.
- Vaccines against some viral STIs, such as Hepatitis B and some types of HPV.
- Prudent antimicrobial use.
- Hygiene (genitals, hands).
Take Home Question
What will I do to help stop STIs?
In daily practice:
- Ask about risk factors.
- Encourage abstinence, especially in the young.
- Promote safer sex practices.
- Support behaviours to decrease risk.
- Screen asymptomatic people based on the epidemiology of the area and your patient population.
- Give all available vaccines.
In the community:
- Participate in disease reporting.
- Support evidence-based decisions.
- Teach young people to practice safe behaviours.
Sexually Transmitted Diseases (STDs)/HIV/AIDS Read More »