Medicine Day 3 Quiz
Medicine Day 3 Quiz Read More »
This quiz is for logged in users only.

Time's up
Medicine Day 3 Quiz Read More »
Money matters involve issues related to finances, particularly personal and business finances.
Money Matters For Small Businesses means that financial management is important for the success and survival of small businesses.
It acts as the lifeblood of any business, enabling it to meet its operational expenses and sustain activities.
A small business is an enterprise that operates with limited capital, usually owned by one person or a few individuals.
These owners contribute the capital and often make key decisions. Small businesses usually employ a limited number of staff.


Business Exit Strategy
A business exit strategy is an entrepreneur’s strategic plan to sell his or her ownership in a company to investors or another company.
It outlines the plan for how the owner will eventually sell or transfer ownership of their company, allowing them to realize the value they have built.
An exit strategy gives a business owner a way to reduce or liquidate his stake in a business and, if the business is successful, make a substantial profit. If the business is not successful, an exit strategy (or “exit plan”) enables the entrepreneur to limit losses. An exit strategy may also be used by an investor such as a venture capitalist in order to plan for a cash-out of an investment.
1. Merger and Acquisition (M&A): This involves selling your company to another company, either through a merger or acquisition. This can be a lucrative option.
2. Selling Stake to Partner/Investor: You can sell your ownership stake to an existing partner or investor. This can provide immediate liquidity while retaining some control over the company.
3. Family Succession: This involves transferring ownership to a family member, ensuring the business stays within the family.
4. Acquihires: Acqui-hiring or Acq-hiring refers to the process of acquiring a company primarily to recruit its employees, rather than to gain control of its products or services. This can be a good option for startups with a strong team and innovative technology. Google acquihired Superpod. Google acquired Superpod to improve Google Assistant’s ability to answer questions.
5. Management and Employee Buyouts (MBO): This involves selling your company to your management team or employees. This can incentivize employees and ensure continuity of leadership.
6. Initial Public Offering (IPO): This involves selling shares of your company to the public on a stock exchange. This can raise significant capital for growth but comes with increased scrutiny and regulatory requirements.
7. Liquidation: This involves selling off the company’s assets and distributing the proceeds to shareholders. This is usually a last resort option, often used when the business is no longer viable.
8. Bankruptcy: This is a legal process that allows a company to restructure its debts and potentially continue operating. It should be considered only as a last resort due to its significant financial and legal implications.
Buying an existing business can be a great opportunity, giving you an established brand, customers, and immediate income. But finding the right business to buy isn’t easy—it’s a time-consuming, costly, and sometimes frustrating process.
Evaluating a business means assessing and analyzing various areas of a business to determine its value, potential risks, and viability. It involves thoroughly examining factors such as financial performance, market position, operations, assets, liabilities, reputation, and legal compliance.
The purpose of evaluating a business is to gain a clear understanding of its strengths, weaknesses, opportunities, and threats before making a decision to buy or invest in it.
Personal Assessment and Criteria: First, consider if the business aligns with your interests, resources, and skills. Evaluate if it’s the right fit for you in terms of cash, credibility, skills, and contacts.
Perform due diligence: This involves researching and confirming the details of the business to ensure you are buying what you expect and to assess its value. Create a team of experts including a banker, industry-specific accountant, attorney, and possibly a small business consultant to perform due diligence. During due diligence, focus on five critical areas:
Ask for the Business Plan: Does the seller have a business plan? This document (or lack thereof) can reveal a lot about the business’s history, future plans, and the owner’s commitment to selling.
Assess the Seller: Your relationship with the seller is important, as you’ll depend on them for information. Pay attention to your interactions during the initial investigation—signs of difficulty now could mean trouble later.
Get a picture of operations: Understand how the business operates by assessing its working capital, manufacturing and operations processes, supply chain, and capital expenditures. Ensure that the business is running smoothly and efficiently.
Evaluate the assets involved: Determine what assets are included in the transaction and their value. This includes intellectual property, brand names, trademarks, patents, and other important assets. Assess how these assets are protected and their significance to the business.
Consider the firm’s reputation: Research the company’s reputation by checking review sites, media outlets, and any past incidents that may have affected its reputation. A strong reputation can positively impact the business’s value.
Verify business licenses and permits: Ensure that the business has all the necessary licenses and permits to operate legally. Check if the required permissions are up-to-date to avoid any potential interruptions or fines after the acquisition.
Confirm the business’ entity status: If the business is a partnership, corporation or limited liability company (LLC) or joint stock company, review entity documents and related records to ensure the business is registered and in good standing. Verify that the owner has the legal rights to sell the business.
The strategies are important for building a solid foundation of the business.
Planning: Creating a roadmap for your business, outlining goals, strategies, and action steps. A business plan helps the business owner to think through issues and understand problems. It’s the shorter-term plan — 12 months — as compared to the longer-term strategy plan.
Funding a Successful Business: Securing the necessary financial resources to launch and operate your business. Adequate and appropriate funding is an ongoing necessity for a healthy business, he advises business owners to develop a relationship with their bank before the need for a loan arises.
Branding, Marketing & Image: Establishing a unique identity for your business and effectively communicating its value to your target audience. Branding and marketing is an essential part of business. “Take the time to understand your customer and consider how your customer reacts to what you’re Saying,”
Sales to Drive Revenue: Implementing strategies to attract customers and convert them into paying clients.
Managing People, Process & Benefits: Building a strong team, establishing efficient workflows, and offering competitive benefits to attract and retain talent.
Operations & Accounting: Managing the day-to-day activities of your business and accurately tracking your financial performance. Accounting is important when you’re starting a business.Keep your business account separate from your personal account. A lot of small businesses start with the personal credit of the owner to give the starting point.
Technology that Matters: Technology is important for its ability to help all businesses scale to provide repeatable and consistent. Leveraging technology to streamline operations, improve efficiency, and improve customer experience.
Money matters for Small Business Read More »
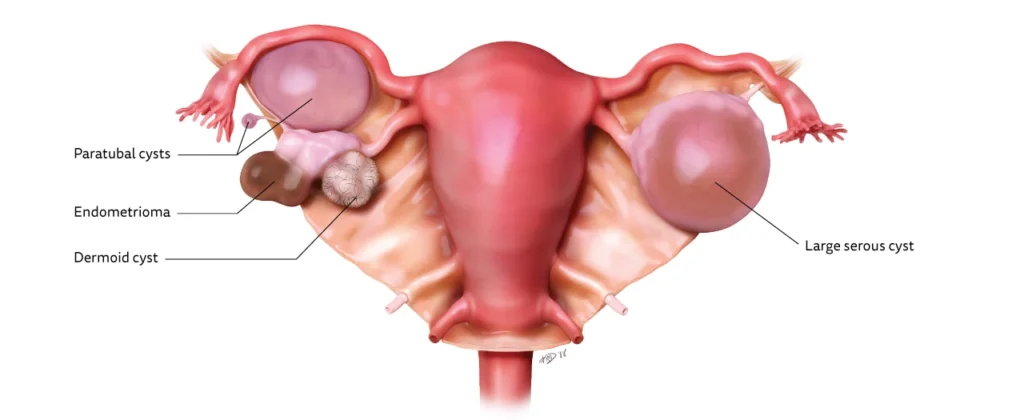
Ovarian cysts are fluid-filled sacs or pockets within or on the surface of an ovary.
An ovarian cyst is a semi-solid or fluid-filled sac within the ovary.
Many women will have them at some point during their lives. Most ovarian cysts present little or no discomfort and are harmless. The majority disappear without treatment within a few months.
Most ovarian cysts occur as part of the normal workings of the ovaries. These cysts are generally harmless and disappear without treatment in a few months. Cysts are caused by abnormal cell growth and aren’t related to the menstrual cycle. They can develop before and after the menopause. Conditions that cause Ovarian Cysts include;
1. Hormonal Imbalances:
Risks Factors include;
1. Medications:
2. Genetics:
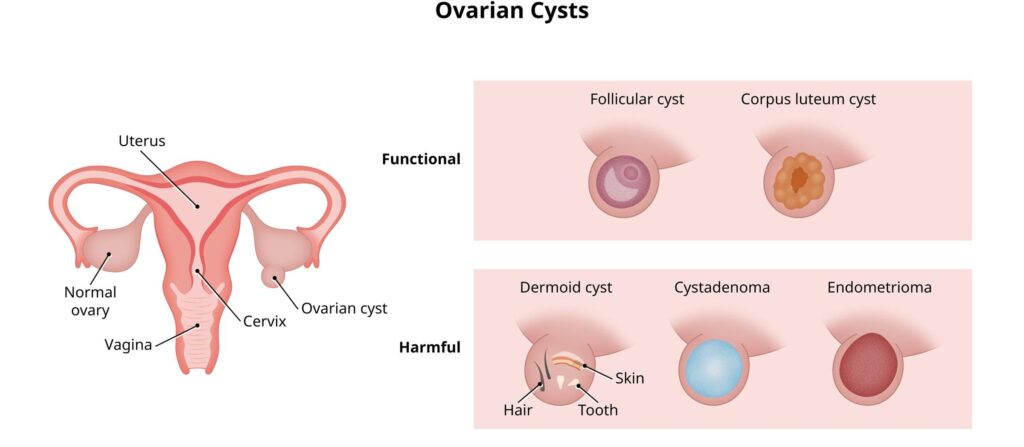
Functional Cysts/Physiological Cysts
Cysts that develop as part of the menstrual cycle and are usually harmless and short-lived; these are the most common type of ovarian cyst.
Cysts that occur due to abnormal cell growth; these are much less common
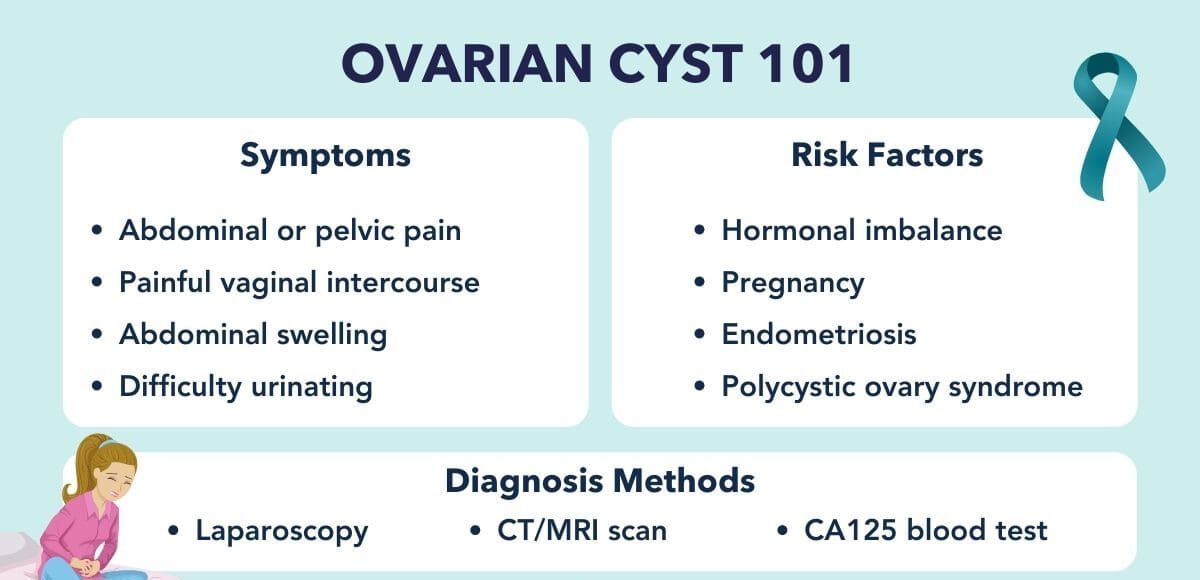
Medical History and Physical Examination:
Imaging Tests:
Blood Tests:
Laparoscopy:
Biopsy:
Management of ovarian cysts depends on various factors such as the type of cyst, its size, symptoms, and the individual’s medical history.
1. Watchful Waiting: In many cases, ovarian cysts resolve on their own without treatment. This approach involves monitoring the cyst through regular check-ups, such as ultrasound scans, to ensure it is not growing or causing any complications.
2. Medications: Hormonal birth control pills may be prescribed to regulate the menstrual cycle and prevent the formation of new cysts. These medications can also help shrink existing functional cysts. They work by suppressing ovulation and reducing the production of ovarian cysts.
3. Surgical Intervention: Surgery may be recommended in the following situations:
4. There are two main surgical approaches:
5. Fertility Preservation: If fertility is a concern, aim to preserve the reproductive organs as much as possible. In some cases, only the cyst is removed, leaving the ovaries intact. However, in certain situations, both ovaries may need to be removed, which can lead to early menopause. In such cases, assisted reproductive techniques may be considered.
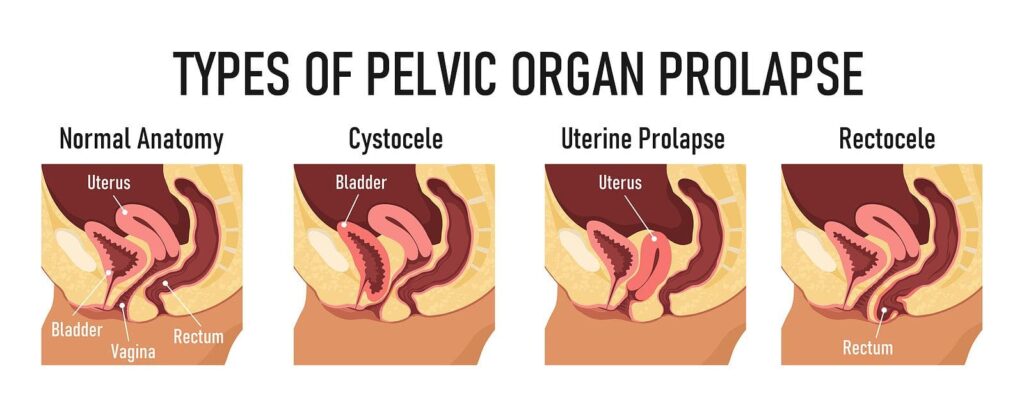
POP occurs when the muscles and ligaments that support the pelvic organs weaken, allowing these organs to bulge or drop into the vagina.
It is divided into three main categories:
1. Anterior Vaginal Wall Prolapse:
Cystocele: This is the most common type of POP. It happens when the bladder bulges into the vagina. It can be graded from 1 to 3 based on the extent of the bulge:
Urethrocele: This occurs when the urethra, the tube that carries urine from the bladder, bulges into the vagina.
2. Apical Prolapse:
Enterocele: This is when a portion of the small intestine bulges into the upper part of the vagina.
Uterine Prolapse: This is a prolapse of the uterus itself into or out of the vagina. It is graded based on how far the cervix (the lower part of the uterus) has descended:
Vaginal Vault Prolapse: This happens when the upper part of the vagina loses its support and sags or drops into the vaginal canal or outside the vagina.
3. Posterior Vaginal Wall Prolapse:
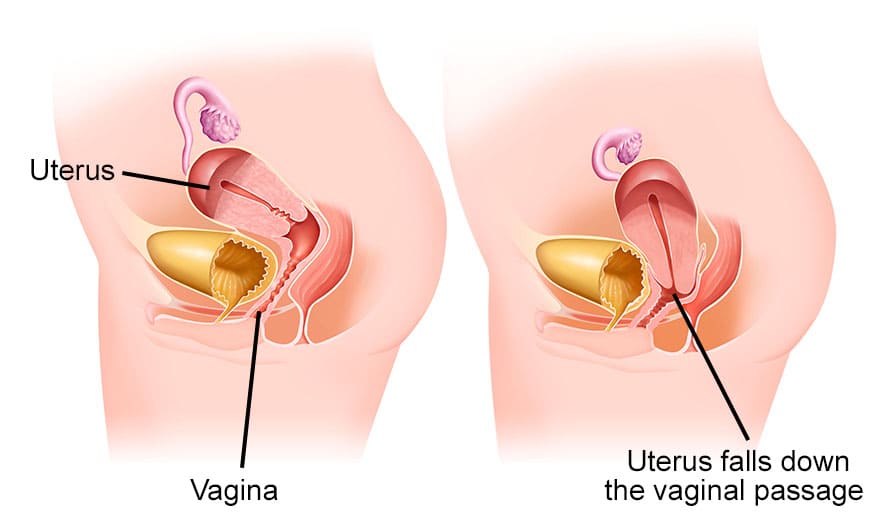
Uterine prolapse occurs when the uterus descends from its normal position into the vaginal canal due to weakened pelvic floor muscles and ligaments.
A uterine prolapse is a condition where the internal supports of the uterus become weak over time and the uterus sags out of position, descends downwards into the vagina.
Uterine prolapse (also called descensus or procidentia) means the uterus has descended from its normal position in the pelvis further down into the vagina.
Uterine prolapse occurs when the pelvic floor muscles and ligaments, which normally support the uterus and other pelvic organs, become weakened or damaged. This allows the uterus to descend into or even protrude from the vagina.
Common causes include pregnancy, childbirth, hormonal changes after menopause, obesity, severe coughing and straining on the toilet.
1. Pregnancy and Childbirth:
2. Age and Menopause:
3. Other Factors:
The pelvic floor muscles and ligaments act as a hammock, supporting the uterus, bladder, and rectum. When these structures are weakened, the uterus can descend into the vagina.
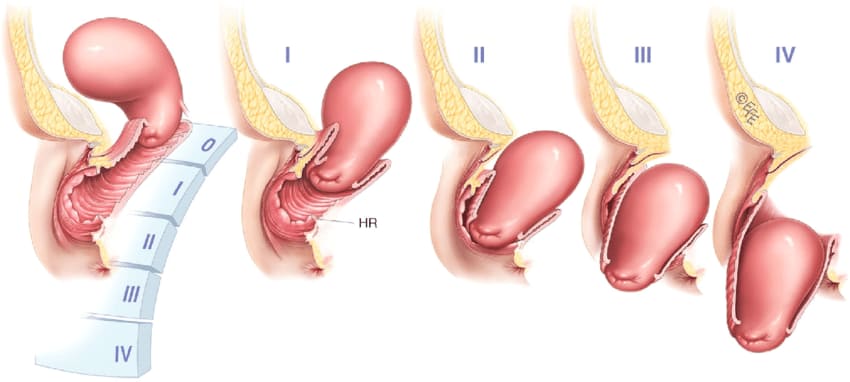
Uterine prolapse is staged based on how far the cervix has descended:
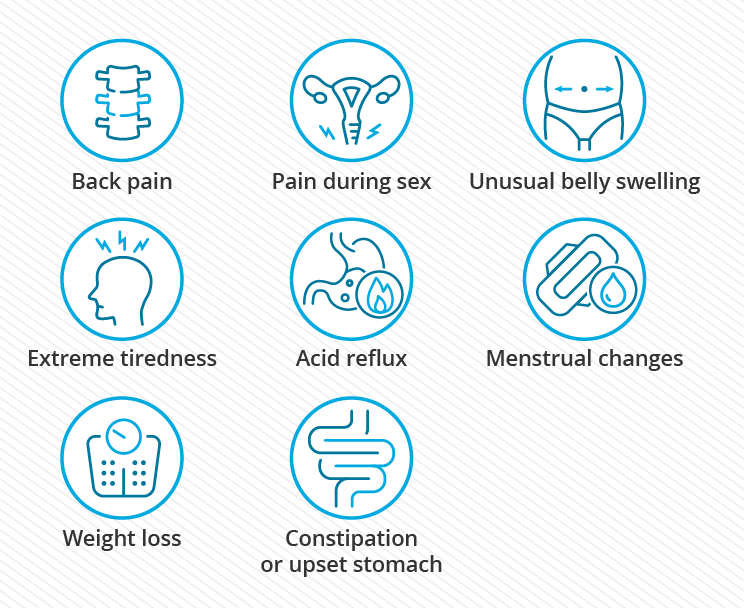
Symptoms of uterine prolapse vary depending on the severity but can include:
History taking: A detailed medical history about symptoms and risk factors.
Physical examination:
Laboratory studies:
The management of uterine prolapse depends on the severity of the prolapse, the patient’s symptoms, and their overall health. It can range from conservative measures to surgical interventions.
Conservative Management:
Definitive Management (Surgery):
Surgery is considered when conservative options fail to provide relief or for severe prolapses.
Cervical prolapse is a type of pelvic organ prolapse where the cervix descends into the vaginal canal, often occurring along with uterine prolapse.
(Remember Cervix can not prolapse without the uterus too)
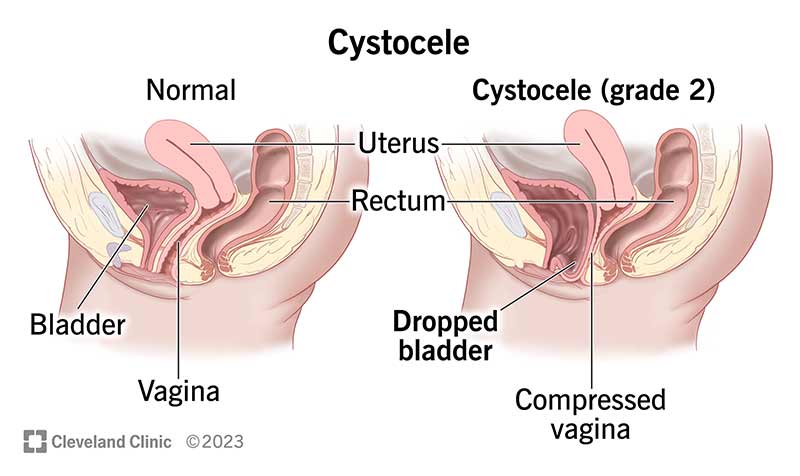
Bladder prolapse, or cystocele, occurs when the bladder bulges into the vaginal wall due to weakened supportive tissues.
When both the bladder prolapse (cystocele) and urethra prolapse (urethrocele) occur together, its called Cystourethrocele.
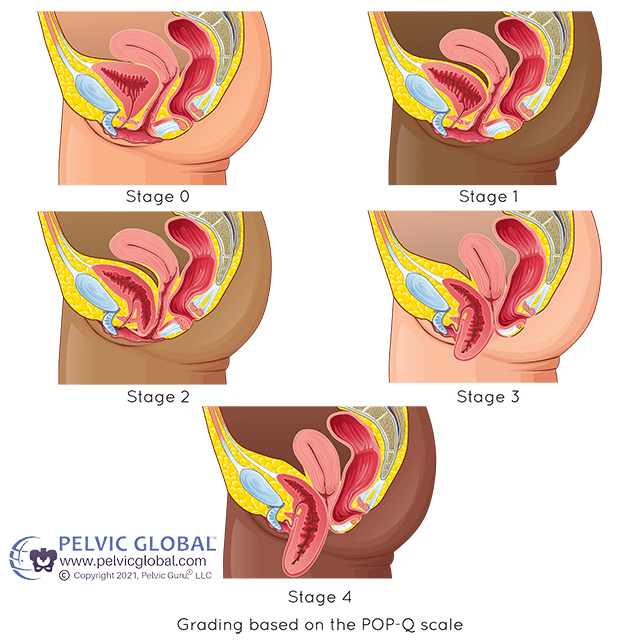
Grade 1 (mild): Only a small portion of the bladder drops into the vagina.
Grade 2 (moderate): The bladder drops enough to be able to reach the opening of the vagina.
Grade 3 (severe): The bladder protrudes from the body through the vaginal opening.
Grade 4 (complete): The entire bladder protrudes completely outside the vagina
Initial Assessment:
Further Diagnostic Tests:
Imaging Tests (May be used to confirm diagnosis and plan treatment):
Evaluating Associated Conditions:
Mild Cases (Grade 1): These often don’t require medical or surgical intervention. Lifestyle changes can help alleviate symptoms:
More Severe Cases (Grades 2-3): If symptoms significantly impact daily life, treatment options include:
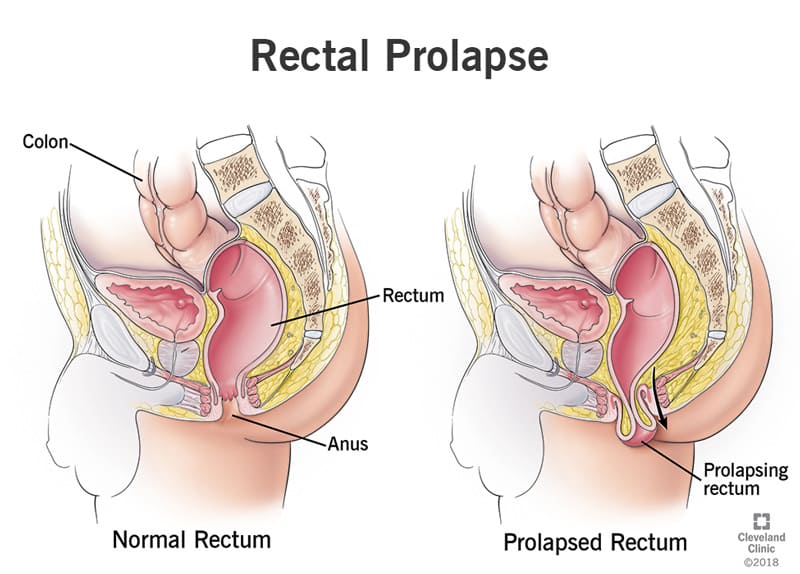
Rectal prolapse occurs when the rectum (the last section of the large intestine) falls from its normal position within the pelvic area and protrudes through the anus.
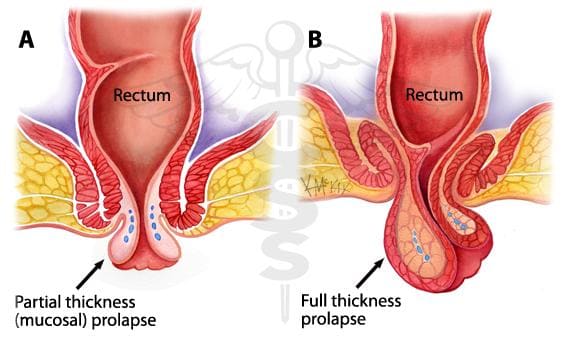
It can involve a mucosal or full-thickness layer of rectal tissue.
Epidemiology:
Rectal prolapse is more common in older adults with a long-term history of constipation or weakened pelvic floor muscles. It is more prevalent in women, especially those over 50 (postmenopausal women), but can also occur in younger individuals and infants.
Pathophysiology:
Mucosal prolapse occurs when the connective tissue attachments of the rectal mucosa are loosened and stretched, allowing the tissue to prolapse through the anus.
Surgical Treatment:
Nonoperative Management:
Non-surgical Management:

Pelvic Organ Prolapse (POP) Read More »
Eye care is characterized as the special attention given to the eyes to prevent complications.
Natural Cleansing:
Eye Cleansing:

Topical medication is the preferred route for treating eye diseases. Eye medications are delivered to:
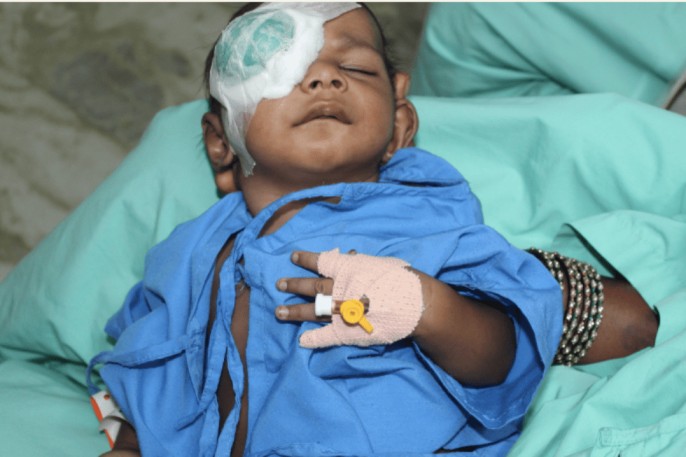
The care involves pre-operative, intra-operative, and post-operative care.
Common conditions requiring surgical intervention include trauma, Cataracts, Foreign body eye, Congenital malformations, Glaucoma, Eye injuries, Astigmatism or strabismus, Sagging of the upper eyelid (ptosis) and detached retina. The ophthalmologist will determine the treatment and procedure, ranging from a simple incision to total removal of the eyeball (enucleation).
Upon arrival at the pediatric surgical ward, the following post-operative care procedures are implemented:
Initial Care and Positioning.
Ongoing Observations:
Welcoming the Child:
Performing Eye Swabbing:
Performing Eye Cleansing:
Instilling Eye Medication:
Applying Eye Padding/Dressing(s)/Shields:
Precautions:
Check the physician’s orders before giving anything by mouth to avoid nausea and vomiting.
Approaching the Patient:
Diversional Activity:
Nursing Care of the Patient with Vision Loss:
Bathing
Care of Your Eye
Activity
Healthy Eating
Medications
When to Seek Help
How to Instill Eye Drops
Care of a child under going eye surgery Read More »
Eye infections occur when bacteria, viruses, fungi, or other microorganisms invade the tissues of the eye or its surrounding structures.
These infections can range from mild to severe and may involve various parts of the eye, including the conjunctiva, cornea, eyelid, or internal ocular structures.
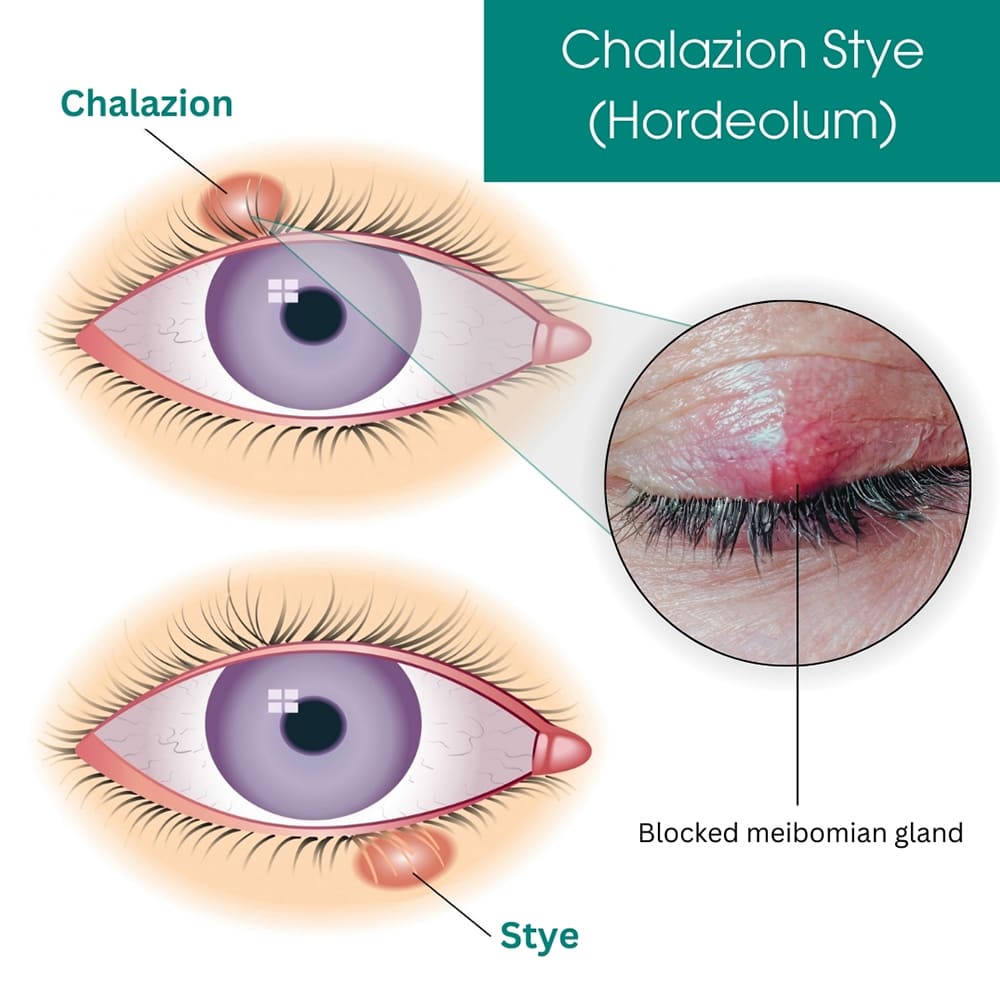
A stye, also known as a hordeolum, is a localized infection of the hair follicle or the oil-producing (sebaceous) or sweat glands in the eyelid.
A stye, or hordeolum, is a localized, painful bacterial infection or inflammation of the glands or hair follicles at the edge of the eyelid.
Commonly caused by Staphylococcus aureus.
It often results from Staphylococcus aureus infection and can occur either externally (on the lid margin) or internally (within the eyelid).
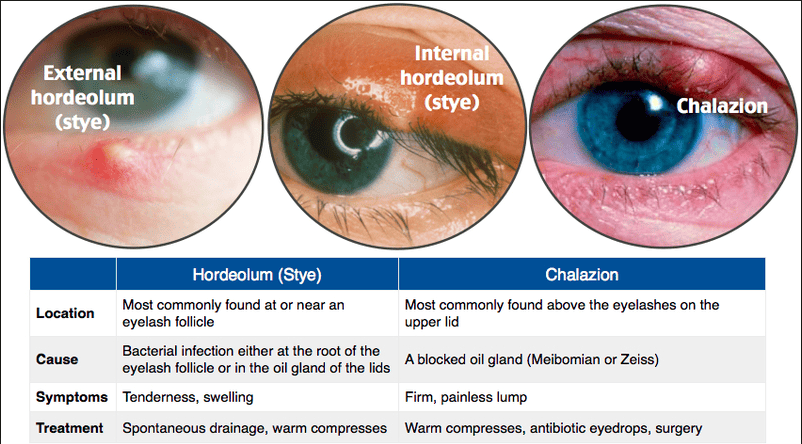
1. Internal Hordeolum: Affects the Meibomian glands, which are sebaceous glands located within the eyelid.
Clinical Characteristics:
2. External Hordeolum: Involves the glands of Zeis (sebaceous glands) or Moll glands (sweat glands) at the base of the eyelash follicle.
Clinical Characteristics:
Early Symptoms:
Progressive Signs:
Advanced Symptoms:
1. General Care
Avoid Rubbing or Touching the Eye:
Warm Compresses:
2. Medications
Antibiotic Eye Ointments:
Analgesics:
3. Eyelash Removal
4. Hygiene Practices
5. Lifestyle Modifications
6. Referral to a Specialist
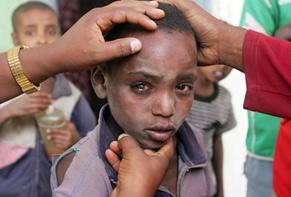
Trachoma is a chronic infection of the outer eye caused by Chlamydia trachomatis, transmitted through direct personal contact, shared towels and cloths, and flies that have come into contact with the eyes or nose of an infected person. It is a common cause of blindness.

Stage I: Trachomatous follicles- follicular (TF). Presence of five or more follicles in the upper tarsal conjunctiva. Follicles are whitish grey or yellow elevations, paler than the surrounding conjunctiva.
Stage II: Trachomatous inflammation – intense (TI). The upper tarsal conjunctiva is red, rough, and thickened. The blood vessels, normally visible, are masked by a diffuse inflammatory infiltration or follicles.
Stage III: Trachomatous scarring (TS). Follicles disappear, leaving scars: scars are white lines, bands, or patches in the tarsal conjunctiva.
Stage IV: Trachomatous trichiasis (TT). Due to multiple scars, the margin of the eyelid turns inwards (entropion); the eyelashes rub the cornea and cause ulcerations and chronic inflammation.
Stage V: Trachomatis corneal opacity (CO). The cornea gradually loses its transparency, leading to visual impairment and blindness.
Community Diagnosis: Essential to establish whether the disease is of public health importance in the community. If so, the SAFE strategy should be the appropriate approach.
The SAFE strategy stands for:
Stages I and II:
Clean eyes and face several times per day.
Antibiotic therapy: The treatment of choice is azithromycin PO:
Failing the above, 1% tetracycline eye ointment: one application 2 times daily for 6 weeks
In children under 6 months or 6 kg: erythromycin PO (20 mg/kg 2 times daily for 14 days)
Stage III: No treatment
Stage IV: Surgical treatment
Stage V: No treatment
Improved Hygiene Practices:
Access to Clean Water and Sanitation:
Environmental Improvement:
Antibiotic Treatment:
Surgical Intervention:
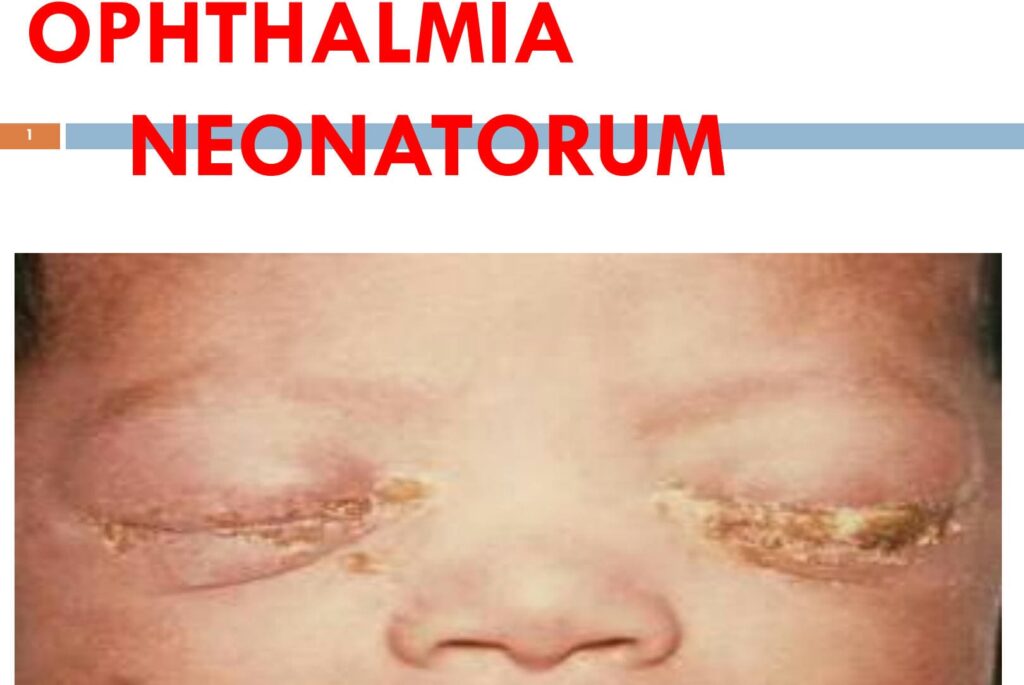
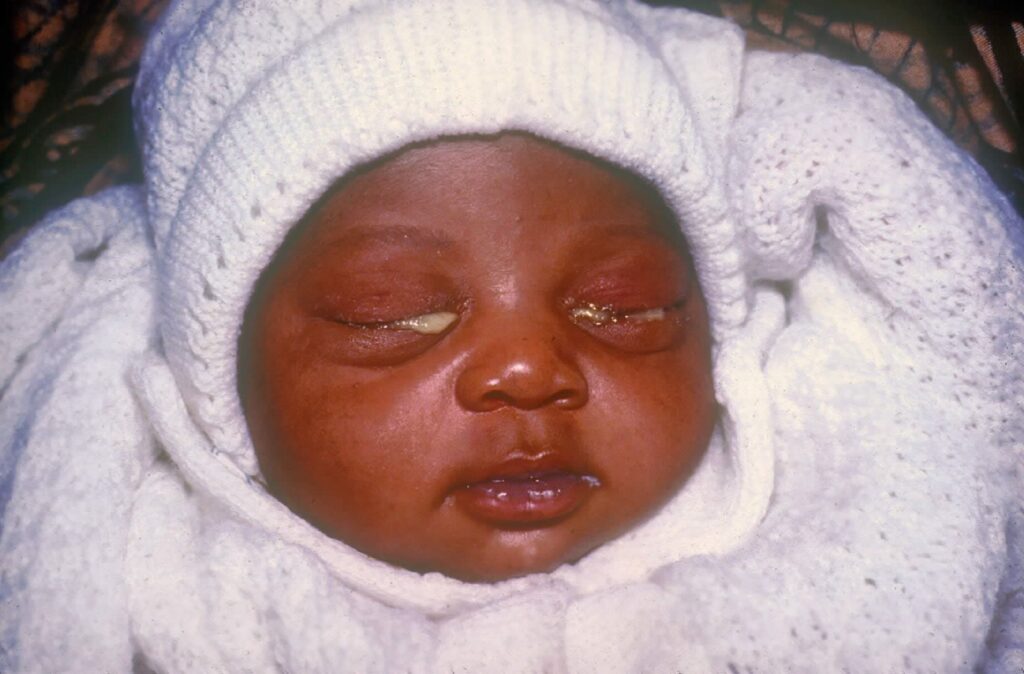
Ophthalmia neonatorum, also known as neonatal conjunctivitis, is any eye infection in the first 28 days of life.
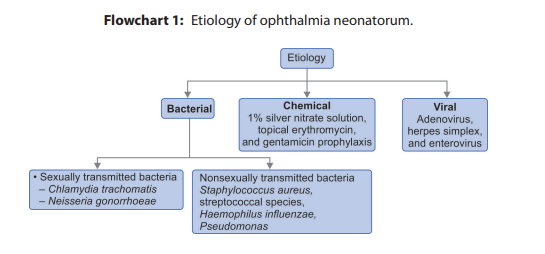
Pathophysiology:
Inflammation of the conjunctiva causes erythema, blood vessel dilation, tearing, and drainage. This reaction tends to be more serious due to reduced tear secretion, decreased immune function, decreased lysozyme activity, and the relative absence of lymphoid tissue of the conjunctiva. Neonate tears also lack immunoglobulin IgA.
The presentation varies depending on the causative agent, but common features include:
Prevention: Prevention strategies target reducing the risk of infection before, during, and after birth.
1. Antenatal (During Pregnancy):
2. Intrapartum (During Labor):
3. Postnatal (After Birth):
Aims of Management:
The primary aims of management are to:
Management in a Maternity Centre (Limited to Mild Cases ONLY – Referral is usually necessary):
Dosage of Diluted Crystalline Penicillin (If Ointments Unavailable – ONLY under direct medical supervision, and ideally as a temporary measure before hospital transfer):
Referral: Refer all suspected cases of ophthalmia neonatorum, especially those with purulent discharge or corneal involvement, to a hospital.
Management in Hospital:
Medical Management: Purulent discharge in the eyes of the newborn baby
→ Take history and examine
1. Rx for the baby:
PLUS:
2. Rx for the mother:
3. Rx for partners:
PLUS:
Educate on compliance:
Incase of specific causative organisms;
Gonococcal Ophthalmia Neonatorum:
Chlamydial Ophthalmia Neonatorum:
Herpes Simplex Ophthalmia Neonatorum:
Nursing Care (Maternity Centre and Hospital):
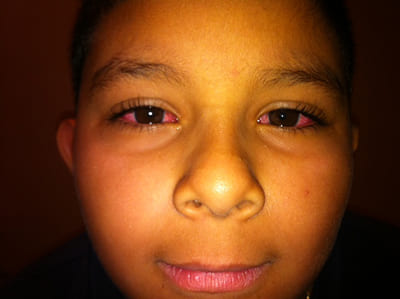
Conjunctivitis is defined as the inflammation of the conjunctival membrane of the eye.
Bacterial:
Viral:
Allergic:
Bacterial:
Viral:
Allergic:
Bacterial:
Viral:
Allergic:
Eye Infections in Children Read More »
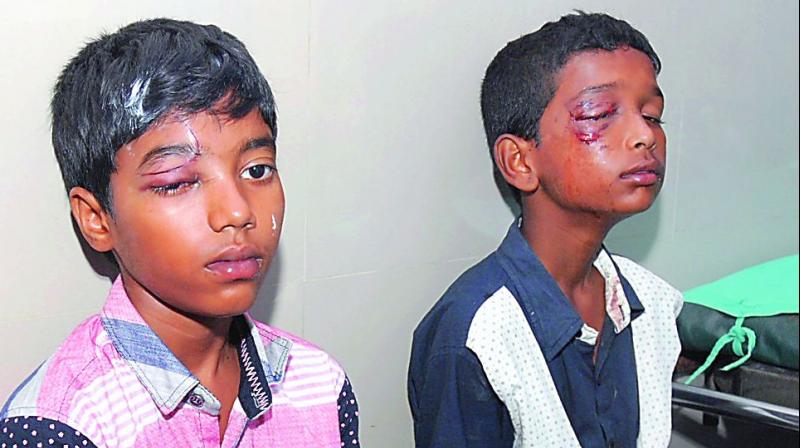
An eye injury refers to any trauma or damage to the eye or its surrounding structures, including the eyelids, conjunctiva, cornea, sclera, iris, lens, retina, or optic nerve.
These injuries may result from mechanical, chemical, or thermal causes, and can range from minor irritations to vision-threatening conditions.
A foreign body is an object in your eye that shouldn’t be there, such as a speck of dust, a wood chip, a metal shaving, an insect or a piece of glass.
Eye injuries are categorized based on the mechanism of injury, the type of trauma, and the specific anatomical location affected.
Type | Description | Examples |
Blunt Trauma | – Impact without penetration to the eye. – Often caused by rounded objects or physical force. | – Sports injuries (e.g., ball, elbow). – Assault (punch). – Airbag deployment in car accidents. |
Penetrating Trauma | – A sharp object pierces the eye, creating an open wound. | – Glass shards. – Nails. – Metallic fragments from tools. |
Chemical Injuries | – Exposure to acids or alkalis, causing chemical burns and tissue damage. | – Cleaning agents. – Industrial chemicals. – Fertilizers or pesticides. |
Thermal Injuries | – Damage caused by excessive heat exposure. | – Explosions. – Hot oil splashes. – Flames or heated objects. |
Radiation Injuries | – Injury due to exposure to ultraviolet (UV) or infrared (IR) rays. | – Sunlight. – Welding arcs. – Tanning lamps. |
Location | Description | Examples of Injuries |
Eyelids | – Protect the eye but are prone to trauma such as lacerations, contusions, and burns. | – Eyelid laceration from sharp objects. – Contusion from blunt force. – Burn injuries. |
Conjunctiva | – The thin membrane covering the white part of the eye and the inside of the eyelids. | – Subconjunctival hemorrhage. – Conjunctival foreign body (dust, sand). |
Cornea | – Transparent, dome-shaped surface responsible for focusing light. | – Corneal abrasion. – Corneal laceration or ulcer. – Foreign body injuries. |
Sclera | – The white, outer covering of the eyeball. | – Scleral lacerations. – Penetrating injuries causing globe rupture. |
Anterior Chamber | – The fluid-filled space between the cornea and iris. | – Hyphema (blood in the anterior chamber). |
Lens | – Focuses light onto the retina; prone to trauma-induced opacity. | – Traumatic cataract formation. |
Retina and Optic Nerve | – Retina is the light-sensitive layer at the back of the eye; the optic nerve transmits signals to the brain. | – Retinal detachment or hemorrhage. – Optic nerve injury (e.g., optic neuropathy). |
Blunt trauma occurs when an object hits the eye with force but does not penetrate. This can lead to:
Penetrating injuries occur when a sharp object pierces the eye. Common examples include injuries from nails, knives, or metal fragments.
Chemical injuries are caused by exposure to irritants like acids or alkalis:
Thermal injuries occur due to contact with hot substances or radiant heat.
Radiation injuries result from prolonged exposure to ultraviolet (UV) or infrared (IR) rays.
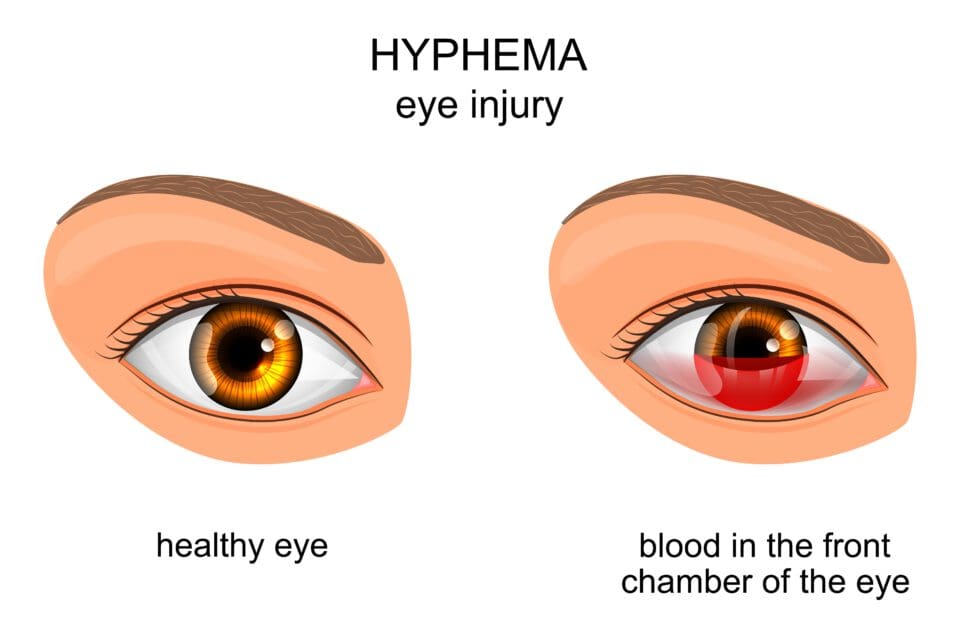
COMMON CONDITIONS ASSOCIATED WITH EYE INJURY AND TRAUMA INCLUDE:
Scratched Eye (Corneal Abrasion): Common causes of corneal abrasions, or scratches to the eye’s surface, include getting poked in the eye or rubbing the eye when a foreign body is present, such as dust or sand. Corneal abrasions are very uncomfortable and cause eye redness and severe sensitivity to light. Scratches can also make eyes susceptible to infection from bacteria or fungi.
Penetrating or Foreign Objects in the Eye: Seek emergency care immediately if a foreign object, like metal or a fish hook, penetrates the eye. Avoid trying to remove the object yourself. Protect the eye with a loosely taped paper cup or eye shield until help arrives.
Caustic Foreign Substance in the Eye (Chemical Burn): Getting unexpectedly splashed or sprayed in the eye by substances such as acids, alkalis, or other harmful chemicals. The basic makeup of the chemical involved can make a lot of difference, such as:
Eye Swelling: Eye swelling and puffy, swollen eyelids can result from being struck in the eye or stung. The best immediate treatment for this type of eye injury is an ice pack.
Subconjunctival Hemorrhages (Eye Bleeding): A subconjunctival hemorrhage involves leakage of blood from one or more breaks in a blood vessel that lies between the white of the eye (sclera) and it’s clear covering (conjunctiva). A subconjunctival hemorrhage is painless and does not cause temporary or permanent vision loss. No treatment is required. Over the course of several weeks, the blood will clear and the eye will return to a normal appearance.
Traumatic Iritis: Traumatic iritis is inflammation of the colored part of the eye that surrounds the pupil (iris) and occurs after an eye injury. Traumatic iritis can be caused by a poke in the eye or a blow to the eye from a blunt object, such as a ball or a hand. Traumatic iritis usually requires treatment. Even with medical treatment, there is a risk of permanent decreased vision.
Hyphemas and Orbital Blowout Fractures: A hyphema is bleeding in the anterior chamber of the eye, the space between the cornea and the iris. Orbital blowout fractures are cracks or breaks in the facial bones surrounding the eye. Hyphemas and blowout fractures are serious eye injuries and medical emergencies.
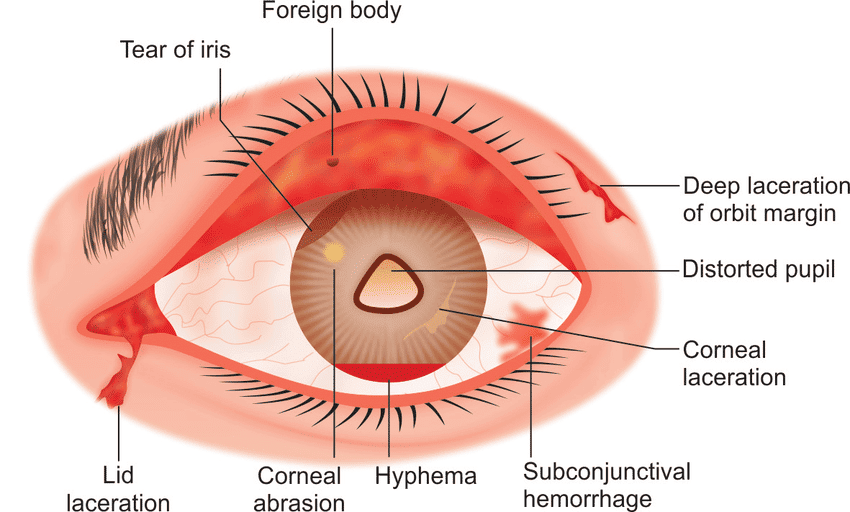
Signs needing emergency care
Management of Eye Injuries
A. Immediate/Emergency Management
Blunt Trauma:
Penetrating Trauma:
Chemical Injuries:
Thermal Injuries:
General Measures:
Medical Management
Topical Medications:
Systemic Medications:
Imaging: CT scan or X-ray for intraocular foreign bodies or orbital fractures.
Surgical Management
Foreign Body Removal:
Corneal Repairs: Suturing for corneal lacerations or perforations.
Treatment for Retinal Detachment: Procedures like pneumatic retinopexy or vitrectomy.
Repair of Ruptured Globe: Requires urgent surgical intervention.
Reconstruction of Eyelids: For severe eyelid lacerations.
Nursing Management
Assessment: Monitor pain levels, vision changes, and signs of infection.
Eye Protection: Cover the injured eye with a sterile shield or dressing.
Pain Management: Administer prescribed analgesics and ensure patient comfort.
Education: Explain the treatment plan and emphasize the importance of follow-up care.
Emotional Support: Provide reassurance to the patient and family, especially in pediatric cases.
Small Cuts, Scratches, or Scrapes Treatment:
Swelling or Bruises with Intact Skin (including a Black Eye) Treatment:
Pain Medicine:
Routine Irritations (sand, dirt, and other foreign bodies on the eye surface):
Embedded Foreign Body (an object penetrates or enters the globe of the eye):
If an object like glass or metal is sticking out of the eye, take the following steps:
Chemical Exposure:
Black Eyes and Blunt Injuries:
A black eye can be a minor injury but might also indicate a significant eye or head trauma.
An in-depth evaluation is necessary to rule out damage to the eye.
For a black eye:
Advice on discharge
Instructions on Medication Use: Proper instillation of eye drops and compliance with prescribed regimen.
Activity Restrictions: Avoid strenuous activities to prevent strain on the injured eye.
Follow-Up Care: Ensure regular visits to the ophthalmologist for monitoring.
Signs to Watch For: Educate the patient about symptoms of complications like worsening pain, vision loss, or redness.
Eye Injuries in Children Read More »
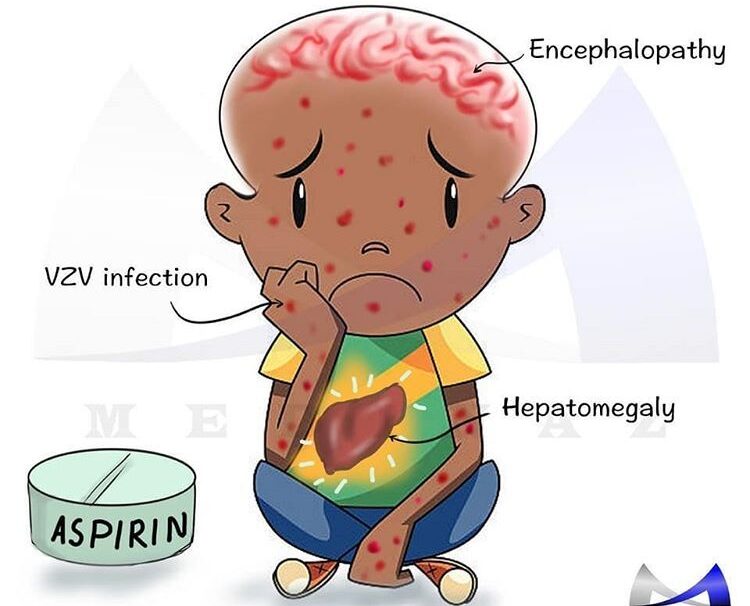
Reye’s syndrome is characterized by acute noninflammatory encephalopathy and fatty degenerative liver failure. I.e It is characterized by swelling in the liver and brain.
Reye’s syndrome commonly affects children recovering from viral infection, most commonly flu or chickenpox.
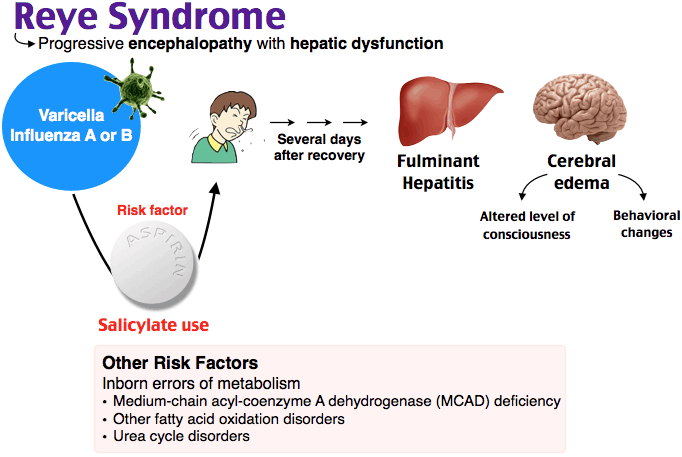

The exact cause of Reye’s syndrome is still unknown, but several factors have been linked to its development.
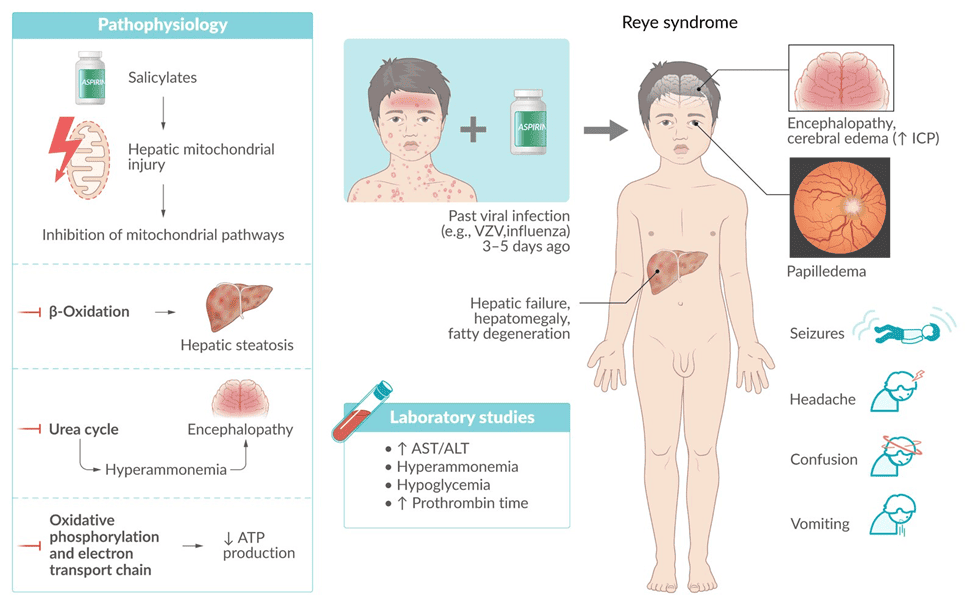
Initial Signs and Symptoms:
For children younger than age 2, the first signs of Reye’s syndrome may include;
For older children and teenagers, early signs and symptoms may include;
Additional Signs and Symptoms:
As the condition progresses, signs and symptoms may become more serious, including;
NB: Reye syndrome should be suspected in any child exhibiting the acute onset of an encephalopathy (without known heavy metal or toxin exposure) and pernicious vomiting.

The stages used in the CDC classification of Reye’s syndrome are as follows:
Stage 0: Alert
Stage 1: Mild Symptoms
Stage 2: Moderate Symptoms
Stage 3: Severe Symptoms
Stage 4: Critical Symptoms
Stage 5: Life-Threatening Symptoms
Stage 6: Unclassifiable
No specific treatment exists for Reye syndrome, and management is primarily focused on providing supportive care based on the stage of the syndrome.
Stage 0-1:
Stage 2:
Stages 3-5:
Urea cycle disorder treatment agents:
Antiemetic agents:
Drugs to avoid
Barbiturates
Nursing Assessment:
Nursing Diagnosis:
Nursing Care Planning and Goals:
Nursing Interventions:
Electrolyte and fluid disturbances:
Increased intracranial pressure (ICP):
Diabetes insipidus (DI):
Syndrome of inappropriate ADH secretion (SIADH):
Hypotension:
Arrhythmias:
Pancreatitis:
Respiratory insufficiency:
Hyperammonemia:
Aspiration pneumonia:
Poor temperature regulation:
Uncal herniation:
Cumulative Exam: https://midwivesrevisionuganda.com/paediatrics-cumulative-test/
A foreign body refers to any object that is not naturally present in a specific area of the body.
Foreign bodies can be objects that are accidentally inserted or lodged in these areas, causing discomfort, obstruction, and potential complications.
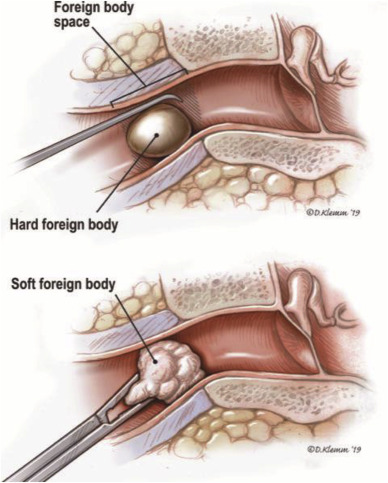
A foreign body in the ear refers to an object that has entered the ear canal and is not supposed to be there.
Most objects that get stuck in the ear canal are placed there by the person themselves. Children who are curious about their bodies and interesting objects, are the group most often having this problem (children aged 9 months to 8 years).
The most common things they put in their ears include Beads, Food (especially beans), Paper, Cotton swabs, Rubber erasers, Small toys, Marbles, Small shells.
Foreign bodies in the ear can be categorized into two main groups: inanimate and animate. Inanimate foreign bodies can further be classified as organic or inorganic.
1. Inanimate Foreign Bodies: Inanimate refers to objects that lack life, consciousness, or the ability to move or grow on their own. Inanimate objects do not possess the characteristics of living organisms, such as metabolism, reproduction, or response to stimuli.
a. Organic: Organic refers to substances that are from living organisms or contain carbon-based compounds
b. Inorganic: Inorganic refers to substances that are not derived from living organisms and do not contain carbon-based compounds. The also include metallic and plastic compounds.
2. Animate Foreign Bodies: Animate refers to objects that are alive, possess life, or exhibit characteristics of living organisms . Animate objects have the ability to move, grow, reproduce, and respond to stimuli.
Less Common
Based on the Object:
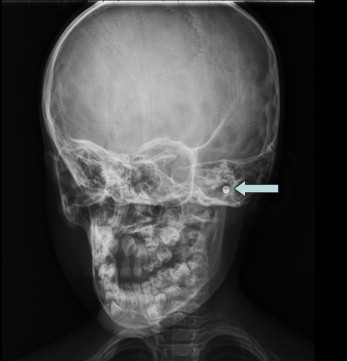
Diagnosis and Investigations of Foreign Bodies in the Ear:
1. Patient History: Obtain a detailed history from the patient or caregiver regarding the nature of the foreign body, duration of symptoms, and any attempts at removal.
2. Physical Examination: Perform a thorough examination of the ear, including inspection of the external ear, otoscopy to visualize the ear canal and tympanic membrane, and assessment of any associated symptoms such as pain, discharge, or hearing loss.
3. Imaging Studies: In some cases, imaging studies may be required to further evaluate the foreign body and its location. The choice of imaging modality depends on the suspected type and location of the foreign body. Common imaging options include:
4. Audiometry: If there is concern about potential damage to the ear or hearing loss, audiometry may be performed to assess the patient’s hearing function.
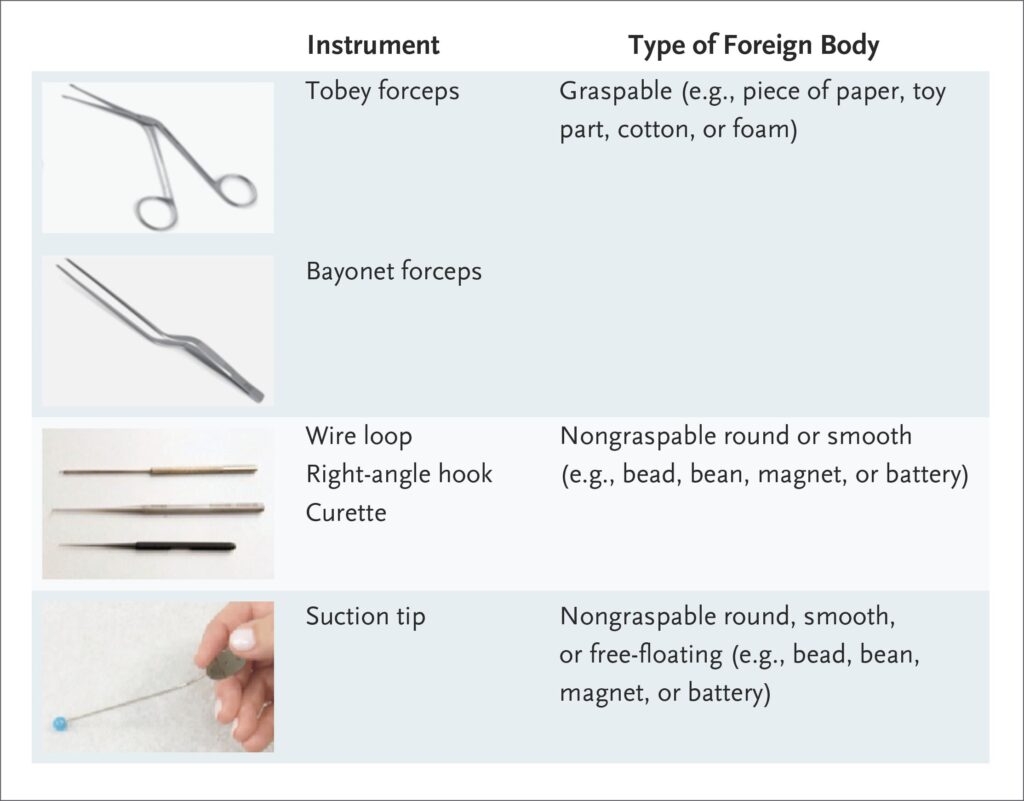
When a patient arrives at the hospital with a foreign body in their ear, we begin by offering a warm welcome and ensuring their comfort. We then proceed with the following steps:
1. Initial Assessment:
2. ENT Specialist Consultation:
3. Treatment Approach:
4. Specific Cases:
5. Post-Removal Care:
6. Urgent Removal Situations:
For smooth round Foreign bodies.
For other Foreign bodies
For insects in the ear
For impacted seeds:
This is accumulation of wax in the external ear that obstructs the external acoustic meatus.
Wax is a normal substance produced in the external ear canal and it can accumulate in it . It is made up of epithelial scales mixed with the secretions from special glands in the skin of the outer ear. Wax in the ear is normal & usually comes out naturally from time to time . In most people, the wax escapes as it is formed but in some it remains in the ear canal forming a wax plug and cause a problem by obstructing it and causing deafness.
Complications:
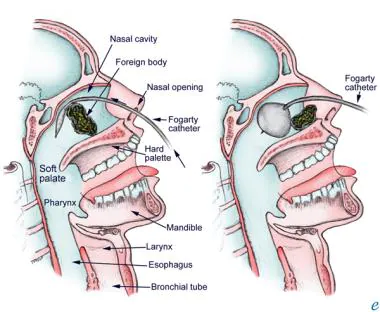
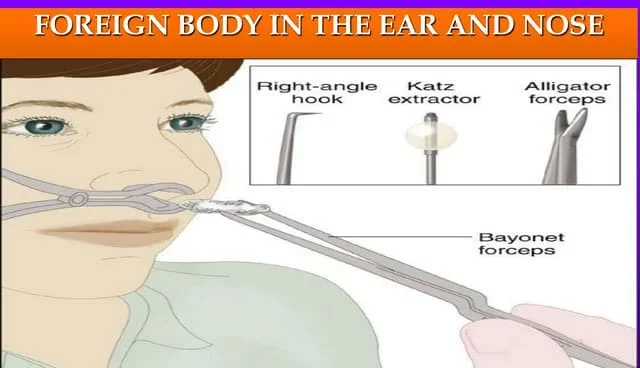
A foreign body in the nose refers to an object that has been inserted into the nasal cavity and is causing discomfort or obstruction.
Foreign bodies in the nasal passages are common, especially in children and mentally retarded adults. They often enter through the anterior nares, but can also come from the mouth or stomach during vomiting or coughing, or be left in the nose during nasal surgery.
Types of Foreign Bodies of the Nose
Clinical Manifestations
Diagnosis
Management
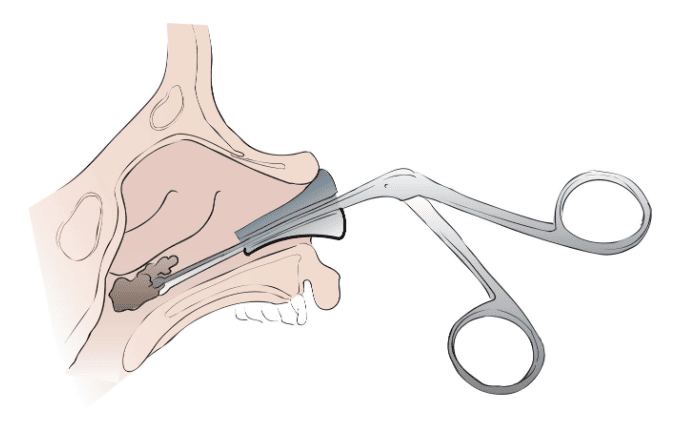
Removal techniques
Before Removal: Reduce swelling: Apply 0.5% phenylephrine (Neo-Synephrine) to shrink the nasal lining and Provide pain relief: Use topical lidocaine to numb the area.
Button batteries must be removed from the nose immediately because of the danger of liquefaction necrosis of the surrounding tissue.
Appropriate infection-control precautions must be taken because the foreign body will likely be expelled against the parent’s cheek and will be covered with mucus and possibly blood.
Removal of foreign bodies from the ear and nose Read More »
Hearing impairment is defined as an impairment in hearing, whether permanent or fluctuating, that adversely affects a person’s ability to hear and understand sounds. It can range from mild to profound.
But let's first see what Hearing means
Hearing starts when sound waves traveling through the air reach the outer ear, also called the pinna. The sound waves then travel through the ear canal to the middle ear.
In the middle ear, the eardrum (a thin tissue layer) vibrates. Three small bones called ossicles amplify these vibrations and carry them to the inner ear.
The inner ear contains the cochlea, a snail-shaped chamber filled with fluid and lined with tiny hair cells. When the vibrations move through the fluid, the outer hair cells amplify them. This amplification allows us to hear soft sounds.
The inner hair cells then translate the vibrations into electrical nerve impulses. These impulses travel along the auditory nerve to the brain, where they are interpreted as sound.
The cochlea is structured so that different areas detect different pitches, like the keys on a piano. From the cochlea, the sound information is transmitted to the cerebrum, where hearing interpretation takes place.
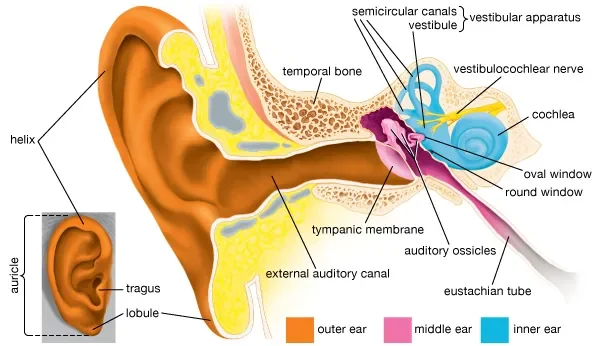
Hearing Impairment:
Hearing impairment occurs when there’s a problem with or damage to one or more parts of the ear.
Deafness:
Hard of Hearing:
Hearing Loss:
Deafened:
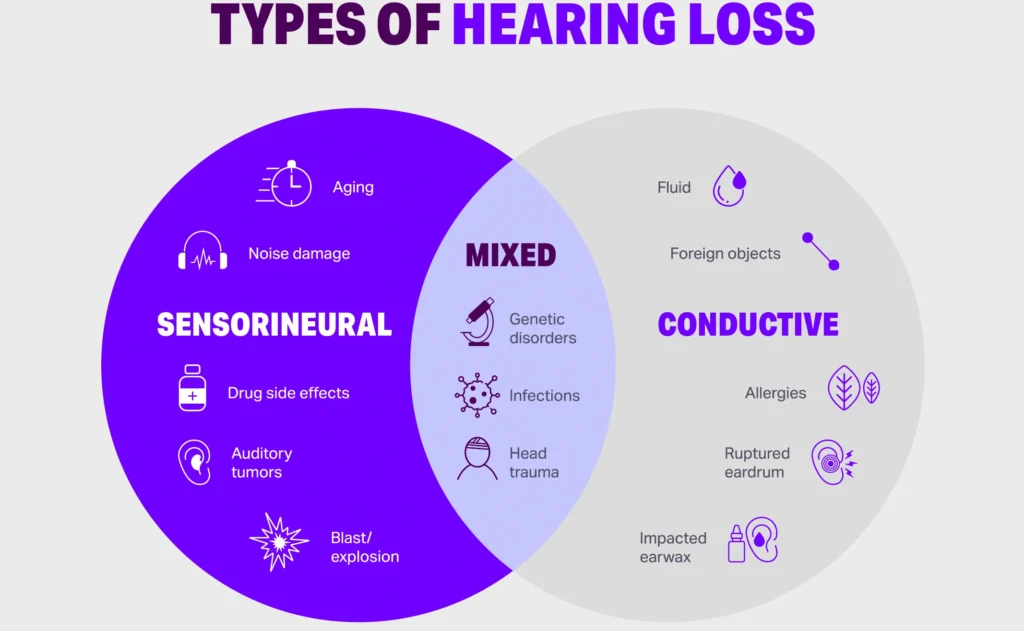
Conductive Hearing Loss: Conductive hearing loss occurs when there is a problem with the outer or middle ear that prevents sound from reaching the inner ear. It can be caused by conditions such as ear infections, blockages in the ear canal, perforated eardrum, or abnormalities in the middle ear bones.
Sensorineural Hearing Loss: Sensorineural hearing loss occurs when there is damage to the inner ear or the auditory nerve pathways that transmit sound signals to the brain. It is the most common type of hearing loss and is often permanent.
Mixed Hearing Loss:
Mixed hearing loss is a combination of sensorineural and conductive hearing loss. It involves both a problem in the outer or middle ear and damage to the inner ear or auditory nerve. This type of hearing loss can occur when someone with pre-existing sensorineural hearing loss develops a conductive hearing loss on top of it.
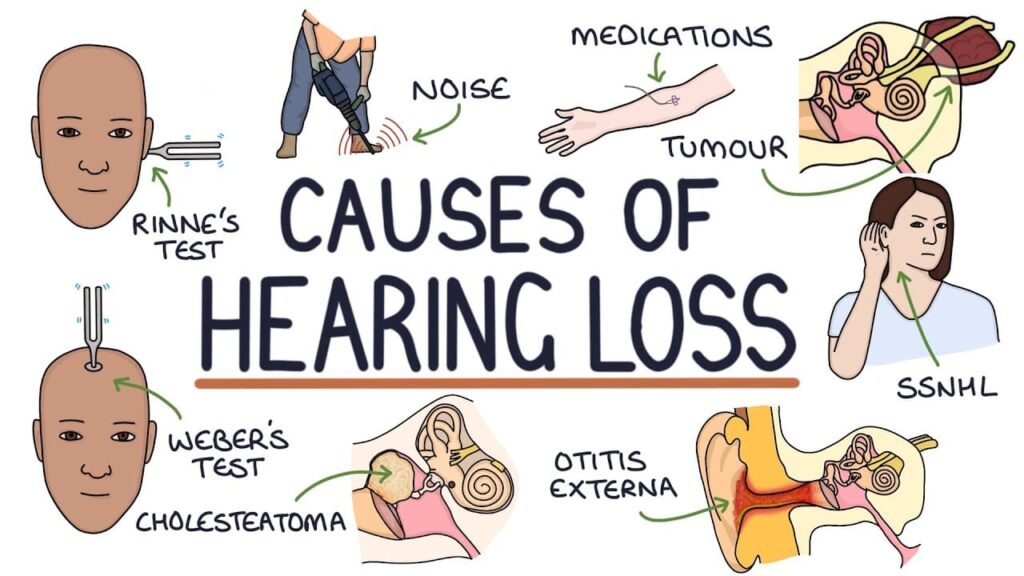
Causes of Hearing Impairment:
11. Infections:
12. Inherited:
13. Congenital Problems: Superior Semicircular Canal Dehiscence: A gap in the bone covering the inner ear can lead to low-frequency conductive hearing loss, autophony, and vertigo.
14. Medications: Ototoxic Medications: Some medications can temporarily or permanently affect hearing. Examples include loop diuretics (furosemide, bumetanide), NSAIDs, and aminoglycosides.
15. Chemicals: Environmental Toxins: Metals (lead) and solvents (toluene) can cause irreversible high-frequency hearing loss by damaging the cochlea and auditory system.
16. Physical Trauma: Head Injury: Damage to the ear or brain centers responsible for processing auditory information can lead to temporary or permanent hearing loss or tinnitus.
17. Sensorineural Hearing Impairment:

Primary Symptoms:
Sensory Symptoms:
Secondary Symptoms:
Other Associated Conditions:
According to age
Infant
Young child
Older child
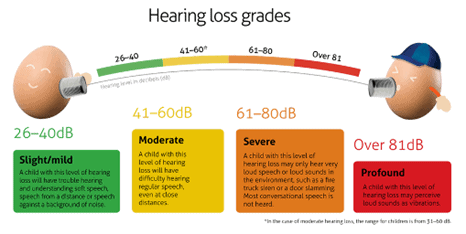
Hearing loss is categorized by type or severity. Furthermore, a hearing loss may exist in only one ear (unilateral) or in both ears (bilateral). Hearing loss can be temporary or permanent, sudden or progressive.
Normal Hearing: Hearing thresholds are within the normal range, typically up to 25 decibels (dB)
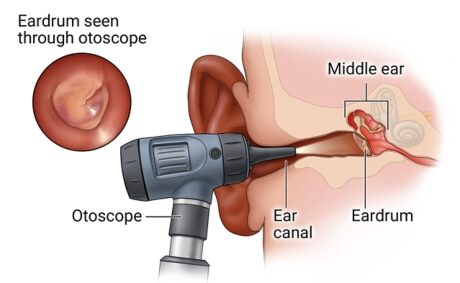
1. History
3. Laboratory testing:
4. Hearing tests:
5. Scans:
MRI and CT scans: These imaging scans can be used to identify the pathology of various causes of hearing loss. They are typically reserved for selected cases where there is a need to further investigate the underlying condition.

The treatment approach depends heavily on the cause, type, and extent of hearing loss.
1. Understanding the Cause:
2. Management Strategies:
a) Assistive Devices:
b) Surgical Interventions:
c) Treatment of Underlying Conditions:
d) Cochlear Implants:
3. Prevention:
4. Living with Hearing Loss:
HEARING IMPAIRMENT Read More »
Javascript not detected. Javascript required for this site to function. Please enable it in your browser settings and refresh this page.