Autonomic Nervous System (ANS)
Autonomic Nervous System (ANS): An Introduction to the Pharmacology
This master guide is designed to make you deeply conversant with:
- The 4 Classes of Autonomic drugs.
- The role of Autonomic drugs in Clinical Practice (Cardiology, Respiratory, Psychiatry, etc.).
- Receptor and Non-receptor mechanisms of ANS drugs.
Note on Adverse Effects (Type A-F) & ADME: While listed in the lecture's opening slide, the provided slides focus exclusively on physiological effects and receptor dynamics. We will provide an emergency overview of Type A-F adverse effects at the end just in case it appears on your exam, but the bulk of this guide will strictly master the core ANS physiology and receptor profiles provided in the slides!
1. The Foundation: Why Autonomic Pharmacology?
Before memorizing drugs, we must understand what we are treating. The nervous system (NS) is the ultimate communication system of the body. It acts as the critical LINK between the BODY and the ENVIRONMENT (both internal, like your sudden drop in blood pressure when you stand up, and external, like a lion chasing you).
If this communication fails, HOMEOSTASIS (the stable, balanced state of the body) is violently disrupted. By understanding Autonomic Pharmacology, we can use drugs to artificially restore this communication and fix homeostasis.
Autonomic pharmacology is highly LOGICAL (if you know the normal physiology, you know the drug's effect) and incredibly CLINICALLY RELEVANT. It applies to:
- Psychiatric Medicine: Treating anxiety (e.g., using beta-blockers for stage fright).
- Respiratory Medicine: Treating asthma and COPD (e.g., inhalers that dilate airways).
- Cardiovascular Medicine: Treating hypertension, heart failure, and arrhythmias.
- GIT Medicine: Treating diarrhea, constipation, and stomach ulcers.
- Genitourinary Medicine: Treating overactive bladder or enlarged prostate issues.
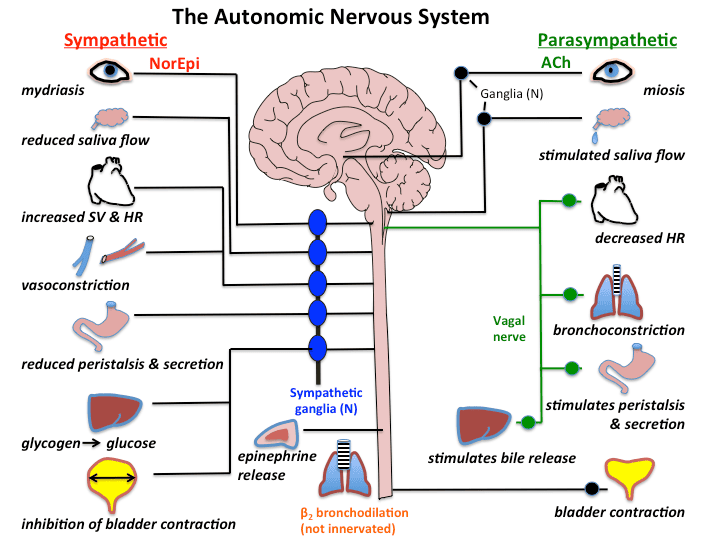
What is the Autonomic Nervous System (ANS)?
The nervous system has two main outputs: Voluntary (Somatic - moving your arm to write a note) and Involuntary (Autonomic). The Autonomic Nervous System (ANS) is simply the "AUTOMATIC" part of the nervous system. It controls visceral organs (the "liquid-like" internal organs: heart, lungs, intestines, blood vessels) without you having to think about it.
The ANS is divided into two competing branches. They are physiological antagonists (they do the exact opposite of each other to keep the body balanced):
- Sympathetic Nervous System (SNS): The "Accelerator." Controls organs during STRESS (Fight, Flight, Fright).
- Parasympathetic Nervous System (PNS): The "Brakes." Controls organs during REST (Rest and Digest / Breed and Feed).
2. The Sympathetic Nervous System: "Fight, Flight, Fright"
The Scenario: You are walking in the bush and suddenly a lion jumps out at you. Your body instantly activates the Sympathetic Nervous System. Every single physiological change that happens next is designed to do one thing: Help you survive by fighting the lion or running away.
The Chemical Messengers (Neurotransmitters)
The sympathetic system communicates using three specific chemicals (Catecholamines). Because these are the messengers, drugs that mimic them are called Sympathomimetics (or Adrenergic drugs), and drugs that block them are called Sympatholytics.
- Noradrenaline (Norepinephrine): The primary neurotransmitter released directly at the nerve endings.
- Dopamine: A precursor and neurotransmitter, heavily involved in the kidneys and brain to maintain perfusion.
- Adrenaline (Epinephrine): This is a hormone, not a neurotransmitter. It is released by the Adrenal Gland directly into the blood. The adrenal gland output is 80% Adrenaline and 20% Noradrenaline. (This massive dump of adrenaline is what gives you that sudden "rush" in your chest when terrified).
Sympathetic System Effects by Organ
(Think deeply: "How does this help me run from the lion?")
| Organ System | Sympathetic Effect | Why? (The Logical Reason) |
|---|---|---|
| Cardiovascular (Heart) | Heart Races: Increased Heart Rate (Chronotropy), increased Force of Contraction (Inotropy), and increased Conduction speed (Dromotropy). | To rapidly pump massive amounts of oxygenated blood to the vital organs and legs for running. Increased force means a higher stroke volume per beat. |
| Cardiovascular (Vessels) | Blood is Diverted: ALL non-essential blood vessels (like those in the skin and gut) CONSTRICT. Blood vessels specifically going to Skeletal Muscles and the Brain DILATE. | You don't need blood in your stomach right now. You need maximum blood (oxygen) in your brain to think fast, and in your muscles to run. (This is why people turn "pale as a ghost" when terrified—skin blood vessels clamp shut!). |
| Respiratory | Bronchial Smooth Muscle RELAXES (Bronchodilation). Bronchial secretions DECREASE. Respiratory rate INCREASES. | Relaxes the airways to open them up as wide as possible. Clears out mucus. This maximizes Oxygen (O2) uptake to fuel the skeletal muscles for sprinting. |
| Gastrointestinal (GIT) | Digestion Shuts Down: Motility DECREASES, Secretions DECREASE (causing Anorexia/lack of appetite), Sphincters TIGHTEN. | Digesting food wastes massive amounts of energy and blood. Constipation and delayed gastric emptying occur to save energy for survival. You won't feel hungry while running for your life. |
| Genitourinary | Urine Output DECREASES: The bladder wall (Detrusor muscle) relaxes, but the exit door (Sphincters/Trigone) TIGHTENS. Renin-Angiotensin System is ACTIVATED. | Stopping to pee while running from a lion is a bad idea. It wastes energy and time. Activating Renin reabsorbs Sodium and Water in the kidneys, raising blood volume and blood pressure to sustain the "fight." |
| Reproductive | Penile Erection INHIBITED. Uterine smooth muscle RELAXES. Genital secretions DECREASE. | Blood is diverted to skeletal muscles. Reproduction is a waste of energy during a life-or-death crisis. (Sympathetic system specifically triggers ejaculation, but inhibits the erection phase). |
| Central Nervous System | Alertness INCREASES (can cause anxiety). Concentration INCREASES. Memory INCREASES. | You need ultimate focus on the threat (the lion) to survive, dodging obstacles instantly. |
| Skin | Sweating INCREASES. Body temperature RISES (due to high metabolism). Body hairs ERECT (Piloerection). | Sweating cools the rapidly overheating engine (your body). Raised hairs attempt to make you look larger and more intimidating to predators. |
| Metabolism (CATABOLIC) | Glucose goes UP: Glycogenolysis & Gluconeogenesis increase. Fat breaks down: Lipolysis increases. Proteins break down. | Catabolism means breaking things down for energy. Your muscles need massive amounts of instant glucose and fatty acids to fuel the sprint, so the liver dumps its sugar reserves into the blood. |
| Exocrine Glands | DECREASE in salivation (causing a dry mouth and difficulty speaking). Decrease in tearing (dry eyes). Decrease in bronchial secretions. | Conserving bodily fluids. (Exam note: Thick, viscous, protein-rich saliva is produced, which makes the mouth feel sticky and dry compared to the watery saliva of the rest state). |
| Ocular (Eyes) | Pupil DILATES (Mydriasis). Accommodation is set for FAR vision. Aqueous humor outflow decreases. Eye secretions reduce. | Dilated pupils let in maximum light to see the predator in the dark. Far vision lets you scan the horizon for an escape route. |
Asthma Attack & Sympathomimetics
The Problem: A patient arrives at the clinic wheezing and struggling to breathe. Their bronchial smooth muscles are tightly constricted (bronchospasm).
The Pharmacological Solution: Based on the table above, the sympathetic nervous system naturally relaxes bronchial muscles. Therefore, we give the patient a Sympathomimetic drug (like Salbutamol/Albuterol). This drug chemically "switches ON" the sympathetic receptors in the lungs, tricking the lungs into a "fight or flight" state. The bronchioles rapidly dilate, allowing the patient to breathe again!
Adverse Effect Logic: Because this drug mimics adrenaline, if too much is absorbed into the blood, it will also hit the heart. What does sympathetic stimulation do to the heart? It makes it race! Therefore, a common side effect of asthma inhalers is tachycardia (fast heart rate), tremors, and palpitations.
Anaphylaxis & The EpiPen
The Problem: A patient eats a peanut and goes into anaphylactic shock. Their blood pressure crashes (severe vasodilation) and their throat swells shut (bronchoconstriction).
The Pharmacological Solution: We inject pure Adrenaline (Epinephrine). Adrenaline hits every sympathetic receptor at once. It forces the blood vessels to clamp shut (restoring blood pressure instantly) and forces the airways to rip open (restoring breathing). It is the ultimate life-saving "fight or flight" override button.
3. The Adrenergic Receptors (Alpha & Beta)
Noradrenaline and Adrenaline don't just magically tell a cell what to do. They must bind to specific "keyholes" on the cell surface called Receptors. The sympathetic system uses Adrenergic Receptors, which are all linked to G-proteins.
There are two main families: Alpha (α) and Beta (β).
Properties & Affinities
- α1 & α2: Have a greater sensitivity and affinity for Noradrenaline.
- β1: Has an equal affinity for both Adrenaline and Noradrenaline.
- β2: Binds exclusively with Adrenaline.
- Mechanisms: Activation of β1 & β2 activates the cAMP pathway. Activation of α1 activates the IP3 / Ca2+ pathway. Activation of α2 actually inhibits cAMP.
Alpha (α) Receptors
General Rule: Alpha 1 is EXCITATORY (it squeezes/contracts things). Alpha 2 is INHIBITORY.
- α1 Location (Excitatory): Think "Constriction and Squeezing".
- Arteries: Causes severe vasoconstriction (raises blood pressure).
- Iris (Pupil): Contracts the radial muscle, causing pupil dilation (Mydriasis).
- Sphincters: Tightens the bladder and GI sphincters to stop flow.
- Skin, Nostrils, Penis: Causes ejaculation, and massive nasal decongestion (shrinks swollen nasal vessels).
- Drug Example: Phenylephrine (an α1 agonist) is used in nasal sprays to clear a stuffy nose by squeezing the vessels shut.
- α2 Location (Inhibitory): Think "The Off Switch".
- Autoreceptors (Pre-synaptic neuron): When activated, they tell the nerve to stop releasing Noradrenaline. It's a negative feedback loop to prevent overstimulation.
- GIT smooth muscles: Relaxes the gut.
- Platelets & Pancreas: Inhibits insulin release.
- Drug Example: Clonidine or Methyldopa (an α2 agonist) tricks the brain into thinking there is too much adrenaline, so the brain shuts down sympathetic output, safely lowering blood pressure (often used in pregnancy).
Beta (β) Receptors
Exam Hack: You have 1 Heart (β1) and 2 Lungs (β2).
- β1 Location (Excitatory):
- HEART (Nodes and muscles): Massively increases Heart Rate (HR), Force of Contraction (FC), and Conduction velocity.
- KIDNEY (Juxtaglomerular apparatus): Triggers the release of Renin, activating the Renin-Angiotensin-Aldosterone system to raise blood pressure.
- β2 Location (Inhibitory/Relaxing):
- ALL Non-Vascular smooth muscles: Relaxes them!
- Bronchial smooth muscles: Bronchodilation (Asthma relief).
- Uterine smooth muscles: Stops premature labor contractions (Tocolysis).
- Urinary bladder smooth muscles (Detrusor): Relaxes to hold more urine.
- GIT (Liver & Pancreas): Stimulates glucose release to fuel muscles.
- Skeletal Muscle Blood Vessels: Causes vasodilation to rush blood to the running muscles.
- β3 Location (Stimulatory):
- Adipocytes (Fat cells): Stimulates lipolysis (fat breakdown for energy).
- Bladder Detrusor Muscle: Enhances relaxation. (Drug Example: Mirabegron is a β3 agonist used to treat overactive bladder by forcing it to relax and hold more urine).
Clinical Scenario: Hypertension & Sympatholytics (Beta-Blockers)
The Problem: A patient has dangerously high blood pressure and a racing heart. Their sympathetic system is overworking the heart.
The Pharmacological Solution: We want to "SWITCH OFF" the sympathetic effect on the heart. We look at our receptors: The heart is driven by β1 receptors. Therefore, we prescribe a Sympatholytic drug specifically called a Beta-1 Blocker (like Atenolol or Metoprolol). This drug sits in the β1 receptor keyhole, blocking adrenaline from binding. The heart rate and force drop, and blood pressure returns to normal!
Contraindication Alert: What if we gave a non-selective beta-blocker (a drug that blocks BOTH β1 and β2, like Propranolol) to a patient who also has Asthma? Blocking β1 fixes the heart, but blocking β2 in the lungs prevents bronchial relaxation, triggering a deadly asthma attack! This is why knowing exact receptor locations is vital.
Clinical Scenario: Benign Prostatic Hyperplasia (BPH)
The Problem: An older man has an enlarged prostate that is squeezing his urethra, making it impossible to urinate. The urinary sphincter is too tight.
The Solution: We know α1 receptors cause sphincters to squeeze shut. So, we give an Alpha-1 Blocker (like Tamsulosin/Flomax). This blocks the α1 receptors in the prostate and bladder neck, causing the smooth muscle to instantly relax, allowing the patient to urinate normally.
4. The Parasympathetic Nervous System: "Rest & Digest"
The Scenario: You successfully escaped the lion. You are now sitting safely on your couch, watching TV, and eating a massive burger. Your body switches to the Parasympathetic Nervous System. Every physiological change is designed to REST, DIGEST, CONSERVE ENERGY, and BREED.
The Chemical Messenger (Neurotransmitter)
The parasympathetic system is incredibly simple compared to the sympathetic. It relies on exactly ONE chemical messenger:
- Acetylcholine (Ach): Released by Cholinergic neurons.
- Drugs that mimic Ach are called Parasympathomimetics (or Cholinergic drugs). Drugs that block it are called Parasympatholytics (or Anticholinergics).
Parasympathetic System Effects by Organ
(Think deeply: "How does this help me rest and digest my food?")
| Organ System | Parasympathetic Effect | Why? (The Logical Reason) |
|---|---|---|
| Cardiovascular (Heart) | Heart Slows Down: Decreased heart rate and conduction. Note: No direct effect on the force of contraction in the ventricles. | You are resting. Pumping hard wastes energy. The vagus nerve puts the brakes on the SA and AV nodes. |
| Cardiovascular (Vessels) | ALL blood vessels DILATE. (Crucial Exam Note: There is NO direct parasympathetic nerve supply to most blood vessels! However, circulating drugs that stimulate M receptors on blood vessels cause the release of EDRF/Nitric Oxide, which causes massive vasodilation). | Lowers blood pressure to a calm, resting state. |
| Respiratory | Bronchial Smooth Muscle CONTRACTS (Bronchoconstriction). Bronchial secretions INCREASE. Respiratory rate DECREASES. | You don't need massive oxygen intake on the couch. Airways narrow to normal resting size to protect the lungs from debris. (Adverse effect of cholinergic drugs: Can cause suffocation/worsen breathing in asthmatics!) |
| Gastrointestinal (GIT) | Digestion Opens for Business! Motility INCREASES, Secretions INCREASE (stomach acid, enzymes), Sphincters LOOSEN. | To rapidly process the burger you just ate, absorb nutrients, and defecate the waste. (Adverse effect of excessive cholinergic drugs: Severe diarrhea and stomach cramps). |
| Genitourinary | Urine Output INCREASES: The bladder wall (Detrusor) CONTRACTS to push urine out. The exit doors (Sphincters/Trigone) RELAX. Renin-Angiotensin has NO EFFECT. | Now is the safe time to dispose of bodily waste without worrying about predators. |
| Reproductive | Penile Erection INCREASED. Uterine smooth muscle CONTRACTS. Genital secretions INCREASE (vaginal lubrication). | "Breed and Feed." Erection is driven by increased blood flow via parasympathetic vasodilation. |
| Central Nervous System | Alertness, Concentration, and Memory are DECREASED. | Allows the brain to REST and transition to sleep. |
| Skin | Sweating INCREASES (specifically common after a heavy meal - "meat sweats"). Body temperature DROPS. | Cooling down to a resting metabolic rate. |
| Metabolism (ANABOLIC) | Glucose, Fat, and Protein ANABOLISM. | Anabolism means building up. The body takes the digested nutrients and stores them as fat and glycogen to conserve energy for the next emergency. |
| Exocrine Glands | INCREASE in salivation. INCREASE in tearing (crying). INCREASE in bronchial secretions. | Copious, watery saliva is required to chew and swallow food efficiently. Tears protect the resting eye. |
| Ocular (Eyes) | Pupil CONSTRICTS (Miosis). Accommodation is set for NEAR vision (reading a book on the couch). Eye secretions INCREASE. | Protects the retina from excess light while resting. Near vision allows for close-up tasks like eating or reading. |
Organophosphate Poisoning & The "DUMBELS" / "SLUDGE" Mnemonics
The Problem: A farmer accidentally sprays himself with toxic agricultural pesticides (organophosphates) or a soldier is exposed to Sarin nerve gas. These chemicals permanently block Acetylcholinesterase, the enzyme that normally destroys Acetylcholine. Suddenly, the patient has a massive, uncontrollable flood of Acetylcholine in his body. His entire Parasympathetic nervous system goes into severe, lethal overdrive.
The Symptoms: Because parasympathetic is "Rest and Digest" to an extreme, he leaks from every orifice. You can remember this via two famous mnemonics:
- DUMBELS: Diarrhea, Urination, Miosis (pinpoint pupils), Bronchospasm/Bradycardia, Emesis (vomiting), Lacrimation (tears), Salivation.
- SLUDGE: Salivation, Lacrimation, Urination, Defecation, GI distress, Emesis.
The Pharmacological Solution: The patient will die of suffocation from massive bronchial secretions and bronchospasm (drowning in their own fluids). You must immediately administer a Parasympatholytic drug (like Atropine). Atropine acts as an impenetrable shield, blocking the Muscarinic receptors from the massive flood of Acetylcholine, "switching off" the lethal parasympathetic response, drying up the lungs, and saving the patient's life.
5. The Cholinergic Receptors (Nicotinic & Muscarinic)
Acetylcholine acts on two completely different families of receptors: Nicotinic (N) and Muscarinic (M). Nicotine and Muscarine are natural plant toxins that helped scientists discover these different "keyholes".
1. Nicotinic (N) Cholinoceptors
These are fast-acting ligand-gated receptors. Binding of Ach to these initiates the opening of Na+ (Sodium) ion channels, causing instant electrical depolarization (firing). Note: Small doses of nicotine stimulate these, but large toxic doses paralyze/inhibit them!
- Nm Receptor (Nicotinic-Muscle): Located on the motor end plate of the Somatic Nervous System (Voluntary movement). Binds Ach to cause skeletal muscle contraction.
Clinical Note 1: Surgical Muscle Relaxants (like Rocuronium or Curare) work by blocking this exact receptor, paralyzing the patient for surgery!
Clinical Note 2: In the autoimmune disease Myasthenia Gravis, the body's immune system destroys these Nm receptors, leading to profound muscle weakness. - Nn Receptor (Nicotinic-Neuron): Located at the Autonomic Ganglia (the relay stations for both Sympathetic AND Parasympathetic nerves) and the Adrenal Medulla. It propagates the nerve impulse down the chain.
2. Muscarinic (M) Cholinoceptors
These are slower, G-protein linked receptors located on the actual visceral target tissues (Heart, GIT, pupil, bladder, etc.). There are 5 subtypes (M1 through M5):
- M1: Located in the GIT and CNS. (Promotes gastric acid secretion. Blocking it with drugs like Scopolamine treats motion sickness/nausea).
- M2: Located in the HEART. (Remember: 2 lungs for β2, but for Muscarinic, M2 is the heart! It slows the heart rate down).
- M3: Located on Exocrine glands (Lacrimal/tears, salivary, bronchial, sweat) causing massive secretions. Also located on Smooth muscles (Bronchial, Urinary Bladder, Uterine) causing contraction. (Drug example: Pilocarpine stimulates M3 in the eye to constrict the pupil and drain fluid in Glaucoma).
- M4 & M5: Located primarily in the CNS.
Cholinoceptors branch into Muscarinic and Nicotinic.
-> Nicotinic: Nn (Autonomic Ganglia, Adrenal Medulla) and Nm (Neuromuscular junction / Somatic).
-> Muscarinic: M1 (CNS/GIT), M2 (Heart), M3 (Exocrine, Bladder, Uterus), M4/M5 (CNS).
6. Crucial Autonomic Rules and Exceptions
1. Dual Innervation
MOST organs in the human body have dual innervation. This means they receive nerve cables from BOTH the Sympathetic and Parasympathetic systems. They act as Reciprocal Physiological Antagonists (one increases the function, the other decreases it to maintain balance). The heart is the perfect example: Sympathetic pushes the accelerator, Parasympathetic pushes the brake.
2. The "Sympathetic ONLY" Exception
Some organs do NOT have dual innervation. They ONLY receive Sympathetic Innervation. These are:
- Most Blood Vessels: (Constricted by sympathetic tone. To dilate them naturally, the body just turns down the sympathetic signal. There is no parasympathetic "reverse" cable for most vessels).
- Sweat Glands: (Crucial for temperature regulation).
- Piloerector Muscles: (The tiny muscles that make body hair stand up).
- Spleen.
3. The "Complementary & Synergistic" Exceptions
While the two systems usually fight each other, there are three major exceptions where they work together or do the same thing:
- Salivary Secretion: BOTH systems increase salivation! (However, the quality is different. Parasympathetic = copious, watery saliva for digestion. Sympathetic = thick, mucous saliva for stress).
- Sweating: BOTH systems can cause sweating. Sympathetic causes stress/heat sweating. Parasympathetic causes post-meal "meat sweats".
- The Penis (Complementary Effects): The two systems work in a beautiful sequence to achieve reproduction.
- Parasympathetic = Points (Produces ERECTION via vasodilation and engorgement).
- Sympathetic = Shoots (Produces EJACULATION and seminal emission).
7. Summary: The 4 Classes of ANS Drugs
Whenever you are given a clinical scenario, you have 4 major pharmacological tools to fix the patient. Think of them as "SWITCH ON" and "SWITCH OFF" buttons for the two systems.
SWITCH ON the Sympathetic system. (Mimic Noradrenaline/Adrenaline).
- Uses: Asthma (open airways - Salbutamol), Anaphylaxis (Epinephrine), Cardiac Arrest (restart heart), Nasal congestion.
SWITCH OFF the Sympathetic system.
- Uses: Hypertension (lower heart rate - Beta Blockers), Anxiety, Angina, Benign Prostatic Hyperplasia (Alpha Blockers).
SWITCH ON the Parasympathetic system. (Mimic Acetylcholine).
- Uses: Glaucoma (constrict pupil to drain fluid - Pilocarpine), Urinary retention (force bladder to contract - Bethanechol).
SWITCH OFF the Parasympathetic system.
- Uses: Organophosphate poisoning (Atropine), Overactive bladder (stop bladder spasms), Pre-surgery (dry up saliva to prevent choking), Motion sickness (Scopolamine).
These drugs achieve these effects by targeting various stages of the neurotransmitter lifecycle, including: Synthesis, Storage, Release, Receptor Recognition (Binding), Reuptake, and Metabolism.
Emergency Exam Supplement: Adverse Drug Effects (ADRs) Types A-F
As noted, this was in the Learning Outcomes slide but omitted from the lecturer's core presentation. If you are tested on it, here is the simplified universal pharmacological standard for ADRs:
- Type A (Augmented): Predictable, dose-related. An exaggeration of the drug's normal action. (e.g., A blood pressure drug causing blood pressure to drop too low, making the patient faint).
- Type B (Bizarre): Unpredictable, NOT dose-related. Usually allergic, immunological, or genetic reactions. (e.g., Anaphylactic shock from Penicillin).
- Type C (Chronic): Occurs only after prolonged, chronic, long-term use. (e.g., Long-term Steroid use causing osteoporosis and adrenal suppression over years).
- Type D (Delayed): Occurs years after the drug was stopped. Often teratogenic (birth defects) or carcinogenic (causes cancer).
- Type E (End of Use): Withdrawal symptoms that occur when a drug is stopped abruptly. (e.g., Rebound severe hypertension if you suddenly stop taking a beta-blocker cold turkey).
- Type F (Failure of Efficacy): Unexpected failure of the therapy, often caused by drug interactions (e.g., taking an antibiotic with antacids prevents absorption, so the antibiotic fails to cure the infection).
Quick Quiz
ANS Drugs Intro Quiz
Pharmacology - mobile-friendly and focused practice.
Privacy: Your details are used only for quiz tracking and certificates.
ANS Drugs Intro Quiz
Pharmacology
Preparing questions...
Choose your answer and keep your streak alive.
Great effort.
Here is your quick performance summary.
Autonomic Nervous System (ANS) Read More »